Normal Pathophysiology of Gastric Acid Stimulation and Production
The healthy functioning of the gastrointestinal tract is crucial for the human body since it ensures digestion, absorption, and assimilation of all the necessary components of nutrition, without which other processes cannot run successfully. When the tract acts normally, food is ingested into the mouth cavity for moistening and mechanical processing; then, it is forwarded along its length with the help of peristaltic movements of the muscles into the stomach and small intestine. There, enzymes are secreted to break carbohydrates, proteins, and fats into basic nutrients that are absorbed across the epithelium of the small intestine (McCance & Huether, 2015).
Gastric acid, secreted by parietal cells in the stomach, is needed to create the optimal pH for pepsin and gastric lipase, thereby assisting food digestion. Normally, gastrin output begins even before food intake and can be caused by the thought, sight, or smell of it.
G-cells (found in the distal one-third of the stomach) that secret gastrin gets stimulated further when protein arrives there (McCance & Huether, 2015). As a result, histamine is released from enterochromaffin-like cells, which stimulates parietal cells. Then, the secretion of acid occurs. Antral D cells react to the drop in pH by releasing somatostatin that causes the so-called negative feedback control (inhibition of gastrin release) (Waldum, Hauso, & Fossmark, 2014).
The output of acid begins at birth and reaches its maximum level at the age of 2. The decline begins in elderly individuals; nevertheless, the process normally continues throughout the entire life.
Changes of Gastric Acid Stimulation and Production with GERD, PUD, and Gastritis Disorders
Gastroesophageal Reflux Disease or GERD (a stomach disorder typically referred to as heartburn) is a widespread condition that appears as a result of acid reflux. Hydrochloric acid produced by the stomach causes the secretion of gastric acid by the gastric gland. As it has already been mentioned, digestive enzymes it contains are required to split molecules. When too much acid is released, it irritates the stomach; as a result, some people can experience acid reflux to the esophagus, causing the so-called heartburn (Orlando, 2016). Therefore, gastric acid is the major triggering factor of GERD. It has been proven by research that excessive production of it can be stopped by changes introduced to the diet and lifestyle (McCance & Huether, 2015).
Peptic Ulcer Disease (PUD) is the condition occurring as a result of the disturbed mucosal integrity in the stomach, which is caused by the local inflammation. As a result, a defined mucosal defect appears, which can be either chronic or acute (depending on the pathophysiology). The condition can be caused by anti-inflammatory drugs, excessive secretion of acid, or transferable ulcers (Ali, 2013). The major contributor, however, is the massive output of gastric acid, which typically happens to patients who have increased parietal cells and suffer from hypersecretion owing to this.
Gastritis is erosion, inflammation, or irritation of the stomach lining that is also connected with gastric acid secretion. The disorder can appear suddenly or develop gradually. In the majority of cases, it is affected by some factors that hinder mucosal defenses (e.g. secretion of insulin and gastric acid, epidermal growth, etc.) (McCance & Huether, 2015). The condition of the patient may get aggravated by any change of gastric secretion.
The Impact of Gender on GERD, PUD, and Gastritis
Although GERD has been extensively studied by many scholars, there is no clear difference found in its manifestations in male and female patients. Research devoted to peculiarities of GERD in women (who experienced heartburn, chest pain, and regurgitation) has revealed small margin results; however, it was discovered that the symptoms experienced by female patients were more frequent and severe (McCance & Huether, 2015).
The same is true about PUD as the disorder is more frequently observed in women. This can be explained by the fact that they have lower immunity to mucosa protection since they secret less hormonal gastric acid. On the contrary, gastritis is more widespread in men as they typically consume more alcohol, which irritates the stomach (McCance & Huether, 2015). In women, this condition usually appears due to the abuse of anti-inflammatory drugs and aspirin.
Diagnosis and Treatment
If the symptoms of any of the three diseases occur in women, they should immediately undertake examination and take dietary precautionary measures. For diagnosing PUD, both men and women can make use of acid-blocking pills to identify whether they relieve the symptoms. If the ulcers are severe, surgery may be required. In lighter cases, medications, a balanced diet, and lifestyle changes are the most common treatment options (McCance & Huether, 2015). Gastritis can be diagnosed via physical examination (taking into consideration genetics), endoscopy, or biopsy. It is usually accompanied by nausea, epigastric pain, burning pain, vomiting, and difficulty eating. In some cases, an upper endoscopy, blood test, and stool test can also be recommended as a part of diagnostics. Antibiotics, vitamin B12 shots, and antacids are used to treat the condition (Waldum et al., 2014).
Mind Map: Gastritis
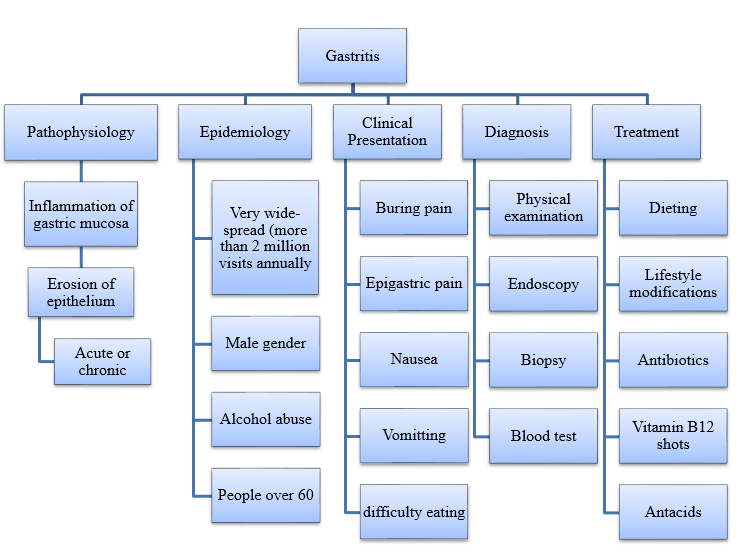
References
Ali, M. Z. (2013). Peptic ulcer disease. KYAMC Journal, 3(2), 270-272.
McCance, K. L., & Huether, S. E. (2015). Pathophysiology-e-book: The biologic basis for disease in adults and children. Amsterdam, Netherlands: Elsevier Health Sciences.
Orlando, R. C. (2016). Gastroesophageal reflux disease. Boca Raton, FL: CRC Press.
Waldum, H. L., Hauso, Ø., & Fossmark, R. (2014). The regulation of gastric acid secretion–Clinical perspectives. Acta Physiologica, 210(2), 239-256.