Introduction
In the early 19th century, families were expected to support their relatives because there was a severe lack of structured assistance. Basic housing and medical services were available. This is where the development of modern healthcare and social services started. As it oversees both health and social care in the UK, the Department of Health is responsible for developing the overall strategy and vision for organizing service delivery at both local and national levels.
Evidence serves as the foundation for decision-making in health and social care services, and practices are guided by policy. In addition to understanding reflective practices in the delivery of healthcare and analyzing theoretical concepts related to evidence-based practice, this essay will discuss the history of current health and social care services, their organization and provision in the UK, and their structure and delivery.
Chronological Development of the Current Health and Social Care Services
In the UK, health and social care services have existed since the 19th century. Families were expected to support their family members during this time because structured assistance was scarce, as Bönker & Wollmann (2019) discuss. The elders were cared for by their families, and those without immediate or extended family were admitted to workhouses, where basic housing and medical care were provided. According to research by Palmer & Dwyer (2020), charities were founded to help those in need, and improvements were made in the second half of the 20th century through charitable interventions.
According to Maclean et al. (2021), significant events in the 20th century—including the National Health Service (NHS) implementation in 1948, welfare spending increases in the 1950s and 1960s, and the adoption of a market approach to service provision in the 1970s and 1980s—shaped the development of health and social care services. The responsibility for providing social care for adults with learning disabilities has been transferred from Primary Care Trusts to Local Authorities in the twenty-first century.
Over the years, there have been significant changes in how services and their delivery are monitored. For instance, Foundation Hospital self-monitoring is mentioned by Maclean et al. (2021) (monitoring is the process of gathering data on current procedures and results). Other important organizations, such as the National Institute for Health and Care Excellence (NICE), the National Clinical Assessment Authority (NCA), and Local Delivery Plans (to name a few), also monitor and evaluate service provision and delivery. It is envisioned that self-monitoring will prevail and that value-based service and care delivery will become the standard.
Several important pieces of legislation have influenced the development of health and social care services in the UK. The NHS Long Term Plan, The Care Standards Act 2010, The Equality Act 2010, Every Child Matters, The Mental Health Act 2007, Safeguarding Policy – Protection of Vulnerable Adults, The Care Standards Act 2000, The Children Act 1989, The Data Protection Act 1998, and 2018 are a few of these. The Care Act of 2014, the Race Relations Act of 1976, as amended in 2001, the Mental Health Act of 1983 and 2007, the NHS and Community Care Act of 1990, and the General Data Protection Regulation (GDPR) (Hughes & McGuire, 2022). As demonstrated by Fisher et al. (2022), these pieces of legislation aim to ensure that the needs of communities and service users are met, that services are safe and suitable for their intended use, and that services are accountable both financially and in terms of quality assurance. It is crucial to stay up to date on any changes, as these laws and policies are constantly evolving.
Organization and Provision of Care Services
Care services encompass a broad range of support offered to individuals who require assistance with daily living tasks due to illness, disability, or advanced age (World Health Organization [WHO], 2022). Governmental organizations and bodies frequently regulate and finance the delivery of care services. The Department of Health and Social Care, a central government agency, is responsible for organizing and providing care services in the UK (Tennison et al., 2021). For the delivery and provision of health and social care services, they are responsible for creating an overall strategy and vision. Government policies and regulations set the financial and regulatory framework for the delivery of care services.
For various age groups and needs, there are numerous types of care services available. According to Lozano et al. (2020), the different types of care services include hospital care, doctor’s office care, maternity care, speech therapy, dental care, eye care, health promotion, mental health care, and complementary care. There are also community services such as hospice care, nursing homes, and daycare facilities for children and adults.
Services for social assistance include foster care and adoption, child protection, residential care, child and family support, and counseling. There are also other childcare options, including childminders, nurseries, crèches, playgroups, family centers, toy libraries, parent-and-toddler groups, and after-school/holiday clubs (Bull et al., 2020). Plans for special education and training are also available. Additionally, private hospitals and shop mobility services are available.
Ensuring services are of high quality and meet the needs of service users is one of the major challenges in providing care services. This calls for thorough resource planning, coordination, and monitoring in addition to ongoing service monitoring and evaluation (Nyashanu et al., 2020). Ensuring that everyone who needs care services can access them, regardless of background or situation, is another challenge. This calls for a commitment to diversity and equality, as well as a readiness to adapt services to meet the needs of various groups.
Evaluation of Reflective Practices Relating to How Care is Delivered
Reflective practice is a method that helps healthcare professionals learn from their mistakes and develop their skills. It entails critically evaluating what you have done and considering how you might proceed differently in the future(Dahlberg & Dahlberg, 2020). Reflective practice can help healthcare professionals identify areas for growth and acquire new skills.
Healthcare professionals must use reflective practice as a vital tool to continue developing their abilities and knowledge in health and social care (Sicora, 2017). It entails examining one’s actions and decisions, reflecting on them, and participating in peer development initiatives. Better patient outcomes and a higher standard of care can be achieved through reflective practice, which enables healthcare professionals to critically assess their work and pinpoint areas for development (Bassot, 2023). In the continuously changing field of healthcare, it is added that it fosters ongoing education and professional development.
However, putting reflective practice into practice can present several difficulties. Finding time for reflective practice is one of the biggest obstacles, as care providers often have busy schedules. A supportive environment that promotes and supports reflective practice is necessary, as are resources like training and supervision, and coworkers who are willing to participate in reflective practice with you (Dahlberg & Dahlberg, 2020). The nature of the job itself may also pose difficulties, such as handling emotionally taxing situations or resolving complex ethical dilemmas.
Several strategies can be used to ensure reflective practice is effectively incorporated into healthcare provision. According to a 2022 study by Barr and Dowding, regularly holding reflective sessions, promoting open communication, offering training and support, and including reflective practice in performance evaluations can all contribute to making reflective practice an essential component of healthcare delivery. According to Barrett et al. (2020), teams and individuals can improve patient outcomes and have a more satisfying, rewarding professional experience by prioritizing reflective practice.
Analysis of Theoretical Concepts Related to Evidence-Based Practice
Evidence-based practice is the use of the best available data to guide decisions regarding the care of specific people or populations. This decision-making process is used in health and social care. First-hand experience, professional opinion, and research studies are just a few examples of the types of sources from which this proof may be deduced (Aveyard & Sharp, 2017). The evidence-based practice aims to improve the quality of care delivered to both individuals and populations by ensuring that decisions are based on the best available evidence (Shayan et al., 2019). It involves analyzing and synthesizing evidence critically before using it to inform decision-making in a given situation.
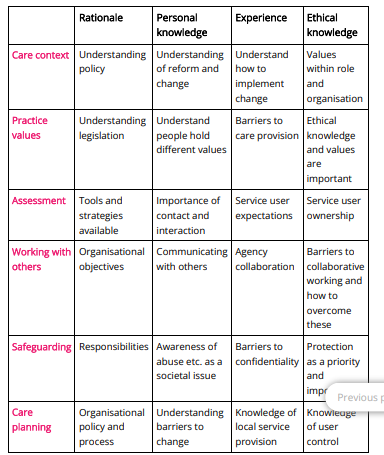
Theoretical concepts include, as stated by Dryden-Palmer et al. (2020), personal knowledge and experience, ethical knowledge, understanding of policy and reform, understanding of legislation, assessment tools and strategies, working with others, safeguarding responsibilities, care planning, and knowledge of local service provision, as shown in Table 1 above.
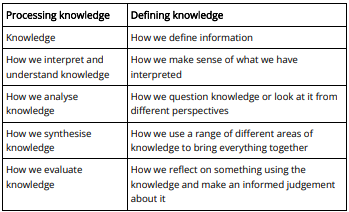
Using Bloom’s Hierarchy (or Taxonomy) (1965), it is easy to understand the process of acquiring knowledge in different ways (Bloom & Krathwohl, 2020). In other words, we ask ourselves, ‘How do we know what we know?’ and then ‘How can we apply what we know?’ In addition to knowledge, we apply skills that help disseminate theoretical knowledge in a practical manner.
EBP in healthcare and social care is supported by a variety of theories. The Stetler Model is one of the most widely applied theories. Nilsen (2020) asserts that this model offers a framework for integrating EBP into clinical practice. There are five steps in the process: preparation, validation, comparison, decision-making, and application.
The Diffusion of Innovations Theory is another theory that backs EBP. According to this theory, new concepts and innovations spread among a population. The adoption process is broken down into five stages: information, persuasion, decision-making, implementation, and confirmation.
Conclusion
It is crucial to keep up with any updates or changes since laws and policies governing the development of health care and service care are ever-changing. The Department of Health and Social Care, a central government department, has the mandate of planning and delivering care services in the UK. Several strategies should be used to ensure the efficient implementation of reflective practice in the provision of healthcare. Different types of healthcare professionals and stakeholders use evidence-based practice, which integrates the best research evidence, clinical expertise, and patient values to inform care-related decisions and improve outcomes.
References
Aveyard, H., & Sharp, P. (2017). EBOOK: A Beginners Guide to Evidence-Based Practice in Health and Social Care. McGraw-Hill Education (UK).
Barr, J., & Dowding, L. (2022). Leadership in health care. Sage.
Barrett, A., Kajamaa, A., & Johnston, J. (2020). How to… be reflexive when conducting qualitative research. The clinical teacher, 17(1), 9-12.
Bassot, B. (2023). The reflective practice guide: An interdisciplinary approach to critical reflection. Taylor & Francis.
Bloom, B. S., & Krathwohl, D. R. (2020). Taxonomy of educational objectives: The classification of educational goals. Book 1, Cognitive domain. Longman.
Bönker, F., & Wollmann, H. (2019). The rise and fall of a social service regime: Marketisation of German social services in historical perspective. In Comparing public sector reform in Britain and Germany (pp. 327-350). Routledge.
Bull, F. C., Al-Ansari, S. S., Biddle, S., Borodulin, K., Buman, M. P., Cardon, G.,… & Willumsen, J. F. (2020). World Health Organization 2020 guidelines on physical activity and sedentary behavior. British Journal of Sports Medicine, 54(24), 1451-1462.
Dahlberg, H., & Dahlberg, K. (2020). Open and reflective lifeworld research: A third way. Qualitative Inquiry, 26(5), 458-464.
Dryden-Palmer, K. D., Parshuram, C. S., & Berta, W. B. (2020). Context, complexity, and process in the implementation of evidence-based innovation: a realist informed review. BMC health services research, 20(1), 1-15.
Fisher, R., Allen, L., Malhotra, A. M., & Alderwick, H. (2022). Tackling the inverse care law.
Hughes, D., & McGuire, A. (2022). Legislating for health: the changing nature of regulation in the NHS. In Quality and Regulation in Health Care (pp. 89-111). Routledge.
Lozano, R., Fullman, N., Mumford, J. E., Knight, M., Barthelemy, C. M., Abbafati, C.,… & Cárdenas, R. (2020). Measuring universal health coverage based on an index of effective coverage of health services in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. The Lancet, 396(10258), 1250-1284.
Maclean, M., Harvey, C., Yang, R., & Mueller, F. (2021). Elite philanthropy in the United States and United Kingdom in the new age of inequalities. International journal of management reviews, 23(3), 330-352.
Nilsen, P. (2020). Overview of theories, models, and frameworks in implementation science. In Handbook on Implementation Science (pp. 8-31). Edward Elgar Publishing.
Nyashanu, M., Pfende, F., & Ekpenyong, M. (2020). Exploring the challenges faced by frontline workers in health and social care amid the COVID-19 pandemic: experiences of frontline workers in the English Midlands region, UK. Journal of Interprofessional Care, 34(5), 655-661.
Palmer, C., & Dwyer, Z. (2020). Good running? The rise of fitness philanthropy and sports-based charity events. Leisure Sciences, 42(5-6), 609-623.
Shayan, S. J., Kiwanuka, F., & Nakaye, Z. (2019). Barriers associated with evidence‐based practice among nurses in low‐and middle‐income countries: A systematic review. Worldviews on Evidence‐Based Nursing, 16(1), 12-20.
Sicora, A. (2017). Reflective practice, risk and mistakes in social work. Journal of Social Work Practice, 31(4), 491-502.
Tennison, I., Roschnik, S., Ashby, B., Boyd, R., Hamilton, I., Oreszczyn, T.,… & Eckelman, M. J. (2021). Health care’s response to climate change: a carbon footprint assessment of the NHS in England. The Lancet Planetary Health, 5(2), e84-e92.
World Health Organization. (2022). Rebuilding for sustainability and resilience: strengthening the integrated delivery of long-term care in the European Region (No. WHO/EURO: 2022-5330-45095-64318). World Health Organization. Regional Office for Europe.