The effective management of healthcare programs unswervingly relates to the quality of health outcomes. The escalating demand for improved healthcare services at a subsidized cost is triggered by the Medicare program, which favors even the financially unstable. Therefore, this calls on the health managers to improvise the innovative techniques and action plans. The implementation and integration of technology-driven change initiatives across the health sector have since shown to support the effort of the health administrators in achieving these aims. The electronic health record (EHR) system, for instance, has proved a great deal of harmonized operations for the health service organizations as they tackle the challenge of managing the information system in their respective organizations. This has been reached through improving the interactivity between physicians and patients, and their health system giving out transformational facilities like scheduling appointments, medication refills, and patient progress monitoring (Schwalbe et al., 2017). However, the evolving healthcare landscape and the new regulatory framework require consistent system upgrades that provide an optimal solution to the current concerns while creating new grounds for the care providers.
This paper underpins three essential considerations and healthcare tools that healthcare managers need in order to develop new strategic directions that are vital for the execution of health services in their respective organizations. Specifically, the budget and the Gantt chart will be discussed in the framework of quality HIT improvement ingenuities within the health environment. Moreover, a work breakdown structure will be outlined to methodically examine the range of activities needed in completing the electronic health record upgrade activity.
The key elements the administrator should consider tracking the necessary resources for the project
The healthcare managers need to consider various crucial elements to track the resources required for the upgrade activity. Attention to crucial features of the system software forms the primary element to consider in this project. A survey conducted by software advice revealed that most organizations dealing in the health sector are dissatisfied with the current electronic health record system because the required systems lack functionality and the applicable features to the specific practice (Meredith et al., 2017). The significance of the functionality is what makes the managers suggest the specific feature that the health practitioners should consider when selecting or upgrading EHR systems. For instance, managers examine the presence of the necessary features that provide the functionality needed for the system to meet its intended purpose.
The software ease of use
On the other hand, ease of use of the software needed is also a crucial consideration when upgrading the EHR system. Most software system upgrades come with complications. For instance, most software comes with technical interfaces that only require technical knowledge to operate. This, therefore, makes ease of use a focal point for the administrators before any purchase is made. In fact, over the last five years, eases of use have been the top complaint list and concern for software upgrades (Meredith et al., 2017). This clearly shows the technicality involved in tracking the appropriate resources for system soft wares. As a manager choosing a software system with a clean and easy-to-navigate user interface is the best approach.
Hardware compatibility and system match
Consequently, testing the hardware compatibility is key to successfully upgrading the EHR systems. Electronic systems can sometimes be highly complex, and when performing an upgrade system, the current hardware must be examined for its compatibility (Project Management Institute, 2017). In some cases, the software might not work with the already existing hardware. This would require the necessary update on the hardware to guarantee the required compatibility. Furthermore, choosing the systems that match EHR to the practice is imperative to consider in this project plan (Coker Group, 2018). The fact remains that the market for the system software has grown exponentially and that many vendors are offering various services on different platforms. Thus, calling on the managers to choose the software imperatively.
EHR Management Tools
The estimated budget, Gantt chart, and work breakdown structure are among the suitable project management tools that best suit this project. They address the challenge of managing the various qualities of an EHR project, such as the scope of the project initiative (Carstens et al., 2019). Moreover, they outline the resources needed to complete a project and how these resources are allocated to each process. Thus, they form practical apparatus to use in this project as shown in the Gantt chart and budget below.
Gantt chart
The chart is an essential tool for this scenario since it shows the task schedule over time. This will allow the healthcare administrator to narrow the activities to specific days and highlight the interdependency of the tasks, as indicated below.

As a health administrator and a project planner, I will use the Gantt chart to visualize the entire project and see how each task is connected to another. Keep all the members together on the same page, and know which tasks are complete and which are not complete, consequently knowing who is working and who is not working. The Gantt chart through the project timeline will allow me to give more accurate status reports to the stakeholders. The task dependencies highlighted in the Gantt chart help keep tasks connected, making it easier to delegate tasks to other team members and adjust the timeline without negatively affecting the overall project (Penn State, 2020). For instance, in this electronic health record upgrade case, the Gantt chart indicates that the project timeline is 10 moths. This will act as my guide in ensuring the systematic flow of the project activities. For instance, the chart shows that cost benefit analysis cannot be done before completing the upgrade test. This is crucial in proper planning and allocation of resources according to their priorities.
Budget
A budget entails estimating the revenue and cost involved in a given project over a specified period. This makes it necessary for the administrator to use it in this case scenario. It will help the administrator in various ways, as detailed below.
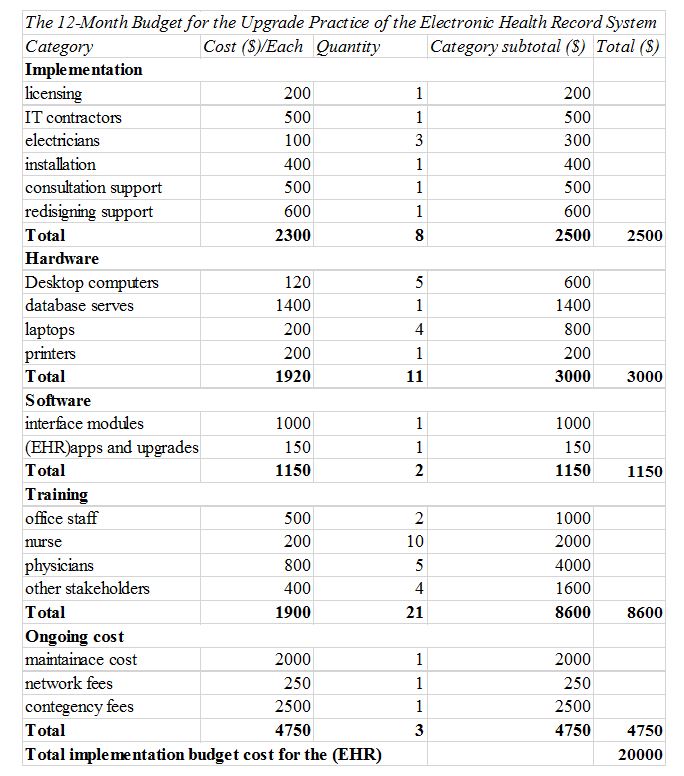
On the other hand, I will use the budget to formulate the activities and understand the priorities while figuring out how the available resources can be used, and which areas need to be evaluated. For instance, in this project, I will consider allocating a higher amount of $7000 to the training of all the stakeholders. At the same, I will reevaluate the hardware components. For instance, if the existing hardware components are compatible with the new software, the hardware part will be reduced to $800 and leave the laptops since they are crucial for the project completion. Lastly, I will use the budget to determine the project areas that require much attention. For instance, in this case, most attention and resource allocation will go to the training, followed by implementation, Hardware, and finally, the software.
Work breakdown structure
Constructing a work breakdown structure (WBS) is crucial for the health administrator to get the project off the ground. The Project Management Institute (2017) states that WBS is “a deliverable hierarchical decomposition of the work to be executed by the project team to accomplish the project objectives and create the required deliverables.” The WBS outlines everything that needs to be done in the project using a chart, thus making it a vital tool to use in this scenario.
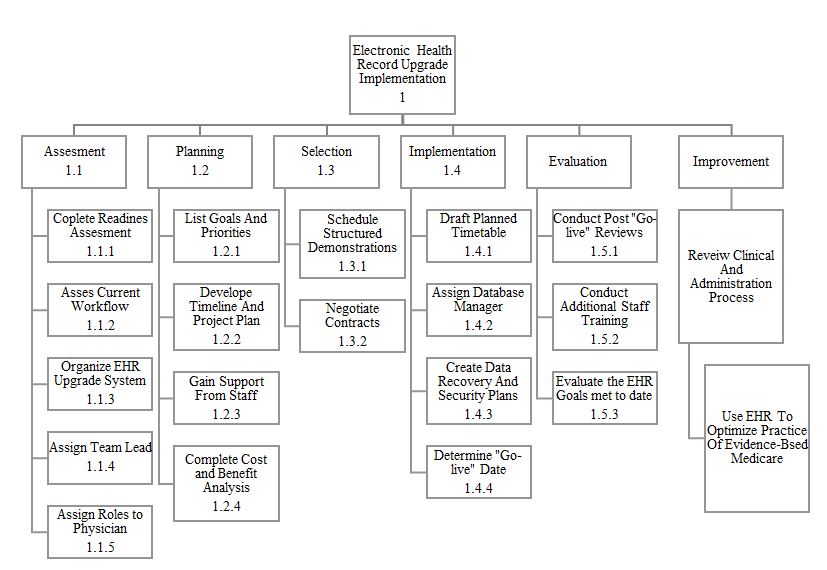
Considering the work breakdown structure (WBS), I will break down the activities in a tree structure view according to their order of performance into deliverables and tasks. I picked the tree structure because it presents a pictorial view that is easy to understand and follow. Similarly, it is the most popular work breakdown structure that most people are familiar with, hence vital in creating ease of work breakdown. This is important in guiding the entire team through all the tasks in line with the project scope. Additionally, the breakdown structure will enable the team to understand where each task fits in the project plan. For instance, the project stakeholders will understand that the staff training is in the evaluation phase while developing the EHR timeline implementation is in the planning section. Using the work breakdown structure eases the channel of communication and makes it more efficient, especially between the members of the team and the administrators (Schwalbe et al., 2017). Arranging and ranking the project deliverables in the order of their completion, in a tree structure, helps harmonize the cooperation of the project members and the stakeholders, thus leading to the effective completion of project activities.
References
Carstens, D. S., & Richardson, G. L. (2019). Project management tools and techniques: A practical guide. CRC Press.
Coker Group. (2018). Vendor Selection and Negotiating EHR Vendor Contracts. Web.
Meredith, J. R., Shafer, S. M., & Mantel Jr, S. J. (2017). Project management: a strategic managerial approach. John Wiley & Sons.
Penn State. (2020). Gantt Charts for Time Management. Web.
Project Management Institute. (2017). A guide to the project management body of knowledge. Newtown Square, PA: Project Management Institute.
Schwalbe, K., & Furlong, D. (2017). Healthcare Project Management: With a Brief Guide to Microsoft Project Professional 2016. Schwalbe Publishing.