Abstract
This study was designed to investigate the effectiveness and implications of using evidence-based practices in modern nursing, a domain in which EBP is increasingly popular. To guide the research and meet its objectives, the researcher first developed a PICOT question. The researcher considered a systematic review to be the most appropriate method for answering the question above. Data were collected from specific scholarly journals to help understand the concept of EBP, how nurses apply it, the challenges faced, and its implications.
The study revealed that the concept has a positive impact on nurses’ performance. When they use EBP, they have the opportunity to learn about the latest best practices in nursing. They get to acquire new knowledge that regularly improves their performance.
However, the study also revealed that the main challenge nurses face in implementing EBP is a lack of relevant materials. It is not possible to apply this concept if there are no materials that can facilitate the problem. It also emerged that when policies are developed requiring nurses to use this concept, compliance increases significantly. The researcher concluded that although EBP has a significant positive impact on nurses’ performance, its effectiveness depends directly on the support nurses receive from other relevant stakeholders.
Introduction
Background
The concept of evidence-based practice (EBP) is increasingly popular in nursing. Li, Cao, and Zhu (2019, p. 1) define it as “using the best available evidence for decision-making and providing efficient and effective care for patients on a scientific basis.” When caring for patients, nurses are often expected to make decisions that may have different implications for their clients. Such decisions may also affect how a doctor handles the patient, especially if the nurse’s action contradicts the doctor’s instructions and a corrective measure becomes necessary. Ellis (2022) explains that EBP provides clear guidelines for nurses to follow, offering a standardized approach to decision-making and patient care. It eliminates situations in which nurses’ actions and decisions become unpredictable and unguided.
Modern nursing practice has undergone significant changes from its past form. According to Gallagher-Ford et al. (2020), nurses are increasingly faced with critical decisions that may have lasting implications for their patients’ health. Traditionally, nurses were expected to strictly follow doctors’ instructions. They lacked the latitude to make decisions, even when a patient’s life was in danger, and they had no way to help. However, the rigid environment in which nurses were expected to receive instructions with very limited decision-making capacity is slowly changing (Craig & Dowding, 2019; Bankanie et al., 2021). Currently, nurses often collaborate with doctors on patient care strategies.
EBP is rapidly becoming popular as a concept that nurses have to embrace in their practice. University of St. Augustine for Health Sciences (2020, para. 2) explains that “It is a method by which practitioners across the healthcare professions review and assess the most current, highest-quality research to inform their delivery of care.” It has become necessary for nurses to base their actions and decisions on scientific evidence. Stannard (2019) argues that nurses can only justify their decisions and actions when supported by scientific evidence. In this study, the researcher seeks to investigate the effectiveness and implications of modern evidence-based practices in nursing.
Justification/Rationale for the Review
Importance of the Topic
Assessing the implications and effectiveness of evidence-based practice is crucial because it helps determine the relevance of this concept in modern nursing practice and its practical application. It may be easy to develop a theoretical concept, hoping that it will be widely accepted and practiced.
However, sometimes reality may differ from the perception the author of the theory or concept had. The use of EBP offers numerous benefits to nurses, their patients, and doctors, but the challenge is that most nurses rarely use it (Boswell & Cannon, 2023; Happell et al., 2019). This study will not only explain the effectiveness of EBP but also discuss how well it is practiced and what can be done to enhance its popularity among nurses.
Reasons Why the Study Is Needed
This study is necessary because it addresses a significant issue in modern nursing practice. Studies have suggested that EBP use enhances nurses’ efficiency and effectiveness (Schmidt, 2021). The problem is that the number of those who embrace this practice is significantly low. It indicates a significant weakness in the promotion and implementation of this concept. The study will address how these weaknesses can be addressed.
Critical Debate
The implications and effectiveness of EBP in modern nursing practice have sparked a critical debate among various scholars. At the same time, Godshall (2020), Grove and Cipher (2019), and Kim, Mallory, and Valerio (2022) contend that EBP is gaining wide acceptance among nurses. Melnyk and Fineout-Overholt (2019) and Houser (2023) note that there is a problem with its actual implementation. The number of nurses who regularly use this concept in their daily practice is significantly low (White, Terhaar, and Dudley-Brown, 2019; Heinen et al., 2019). This suggests a need for further training for nurses and for the popularization of this concept.
Statistics and Links to Higher Policy
The researcher considered it necessary to review statistics on the application of evidence-based practice among nurses. As shown in Figure 1, most nurses do not apply this concept in their practice. The statistics show that EBPs, such as asking questions in PICO format, acquiring the best evidence, appraising the literature, applying them in clinical practice, and assessing outcomes, are often performed once a month by fewer than 50% of nurses. Those who never engage in any of these activities make up as much as 35% of nurses. Less than 8% do them daily, but not on all patients.
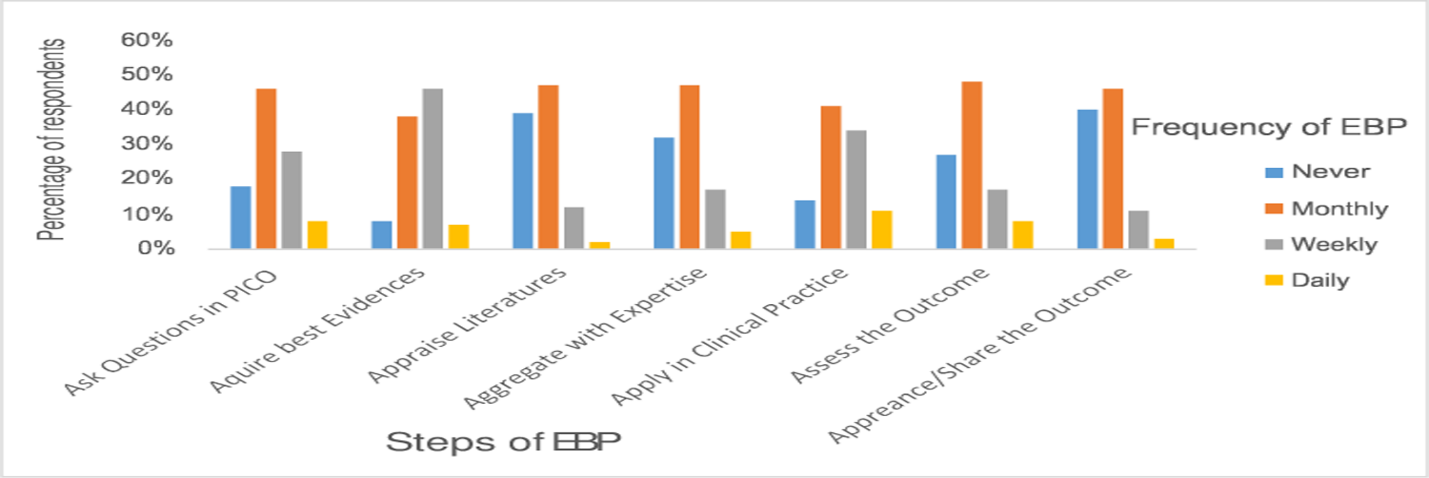
The researcher also assessed the frequency with which nurses use various sources of information to guide their practice. As shown in the figure below, approximately 2% of participating nurses consistently use printed materials for information, a concerning trend. The most commonly used resources are policy guidelines (approximately 25%) and information from colleagues (around 10%).
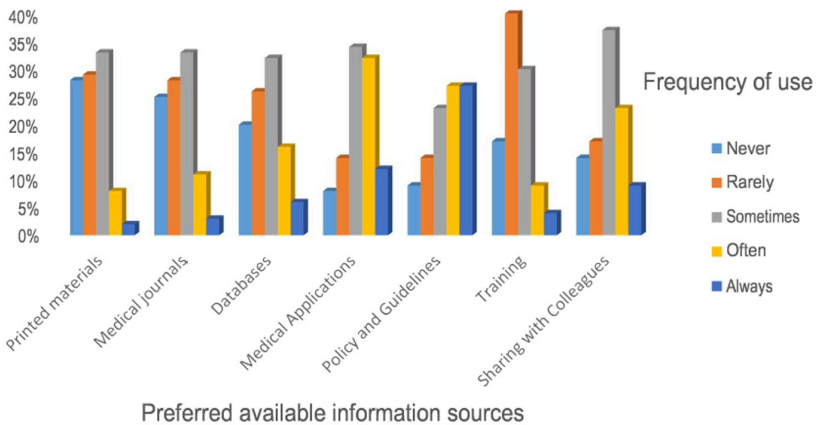
This indicates that when there are no policy requirements, these nurses may lack the incentive to apply EBP in their practices. This means that the Department of Health (DH), the National Institute for Health and Care Excellence (NICE), the World Health Organization (WHO), and the Nursing and Midwifery Council have a significant role to play in defining policy guidelines and ensuring their implementation.
Evidence That Prompted the Research Question in Relation to Nursing Practice
It is necessary to link this study to evidence that made it necessary to conduct the research in relation to nursing practice. A study by Dang et al. (2021) indicated that the concept of evidence-based practice is gaining increasing popularity in the field of nursing; however, its actual implementation is a major concern. The study reveals that most nurses who claim to apply this concept do not fully understand how to implement it (Gray-Miceli et al., 2021; Bumby, 2020). The study revealed a significant gap: those responsible for implementing the practice often lack a clear understanding of the concept.
Key Issues Standing Out
During a preliminary literature review, several key issues emerge regarding the implications and effectiveness of modern evidence-based nursing practices. One key issue that emerged is the lack of specific standards for what constitutes evidence-based practice in nursing, as noted by Lunden et al. (2020). This means that the actions taken by one nurse may differ from those of another, even when they face the same situation and both claim to use evidence-based practice.
Another issue that emerged is the nurses’ willingness to abandon popular practices and embrace evidence-based practice (Kim et al., 2019; Combrinck, Wyk, and Mogale, 2022). There are cases where nurses claim to use evidence-based practice when it suits them, while in practice they still employ some traditional methods.
Aim and Objectives
This study aims to determine the implications and effectiveness of evidence-based practices in modern nursing practice. The following are the objectives of this research:
- To determine the implications of evidence-based practices in modern nursing practice.
- To assess the effectiveness of EBP in modern nursing practice.
- To decide how widespread EBPs are within contemporary nursing.
Research Question
After defining the aim and objectives of the study, it was necessary to develop specific questions to facilitate data collection and analysis. The following is the PICO (population, intervention, comparison, outcomes) question that will be answered using a systematic review.
Among nurse practitioners (P), what are the implications and effectiveness of evidence-based practice (I) on enhancing the performance (C) compared to no intervention (O)?
The researcher will answer the question above by conducting a systematic literature review, followed by a discussion of the results. The use of secondary sources was considered adequate because this field of knowledge has attracted a significant number of scholars over the years. It was possible to fully rely on these published sources to achieve the study’s aims and objectives.
Methodology
Systematic vs. Literature Reviews and Their Benefits
It is essential to understand the literature on systematic reviews and literature reviews, including their benefits. According to Katowa et al. (2021), the primary goal of a systematic review is to answer a focused clinical question and eliminate bias. In contrast, the goal of a literature review is to provide an overview or summary of a given topic.
The question in a systematic review is clearly defined and often guided by the PICO framework, whereas a question in a literature review can be either a specific question or a general topic (Rivera & Fitzpatrick, 2021; Petrovic, Hack, and Perry, 2020). While a literature review can be based on a single source or database, a systematic review is more comprehensive and would require multiple databases.
Both systematic and literature reviews have benefits in a given study. A literature review provides an overview of the topic, enabling readers to understand what other scholars have discovered in a given field of study. It also makes it possible to identify potential knowledge gaps that require further investigation. On the other hand, systematic reviews enable the answer to a specific clinical question using a wide range of secondary sources (Tanner & Stanislo, 2022; Norful et al., 2022). It offers a more comprehensive approach to assessing a specific clinical question.
Reasons for the Use of a Systematic Literature Review
In this study, the researcher chose to utilize secondary data sources to answer the research questions and achieve the study’s aims and objectives. A straightforward literature review was considered less appropriate, and a systematic literature review was deemed more appropriate. Unlike literature reviews, which tend to be broad and descriptive, this study focused on a specific, targeted question, which can be achieved only through a systematic literature review (McCrae & Purssell, 2020; Patole, 2021).
This method is also known for its completeness and ability to minimize bias in a study (Jolley, 2020; Bidewell et al., 2020). A systematic literature review was also prioritized because it involves using numerous databases to facilitate a comprehensive search for evidence, unlike a literature review, which can rely on only one database or even a single source.
A systematic review was considered more reliable in this study because it employs specific parameters in a clinical study, which in this case take the form of PICO. This means that such an investigation must clearly define the population under investigation, which in this case is nursing practitioners, and the intervention, which is the use of evidence-based practices (Tworek, 2019). The study must also explain the alternative to the intervention, which in this case would be failing to use EBP, and the outcome, which refers to the benefits of using the intervention to the targeted population or their clients.
Inclusion and Exclusion Criteria and Why They Were Chosen
Evidence-based practice has attracted the attention of many scholars over the years, and as a result, numerous publications have been published on this topic. It was necessary to select sources that specifically address the issue under investigation in the best way possible. As such, an inclusion/exclusion criterion for selecting the sources had to be developed. Table 1 outlines the criteria used to identify sources utilized in this study.
Table 1: Inclusion and Exclusion Criteria
The criteria selected for the table below were chosen to ensure that the sources addressed the PICO question, were recent enough to capture new developments in this field, and were accessible for this review. The criteria also enabled the researcher to use only reliable sources published by individuals with experience and academic authority in this field.
Type of Research Targeted
The researcher’s decision to use a PICO question meant that quantitative studies would be the most ideal for the systematic review. Tucker et al. (2022) explain that PICO questions are often answered more effectively through quantitative studies because they enable the establishment of relationships among variables. However, this comprehensive systematic review also needed to incorporate randomized controlled trials (RCTs), qualitative studies, and mixed-methods research, provided they directly addressed the research question.
Literature Search Strategy
The researcher targeted specific databases to obtain the information needed for the study. The main databases from which most of the sources in this study were obtained include PubMed, Medline, EBSCO, Embase, Cochrane Library, Web of Science, and HMIC. Google Scholar was another important database where additional sources were obtained (Haber et al., 2020). The keywords and phrases used in searching for the material were evidence-based practice, implications, effectiveness, and modern nursing practice, as shown in Table 2 below. The researcher also typed the entire title of this research to help locate the sources.
Table 2: Key Words/Phrases
The initial number of sources before filtering was 715. The inclusion and exclusion criteria were then used to filter the sources to 100, as shown in the PRISMA flow diagram in Figure 3. The study targeted nurses who use EBP in their practice, rather than patients. The figure below shows the filtering process and the number of studies at each stage.
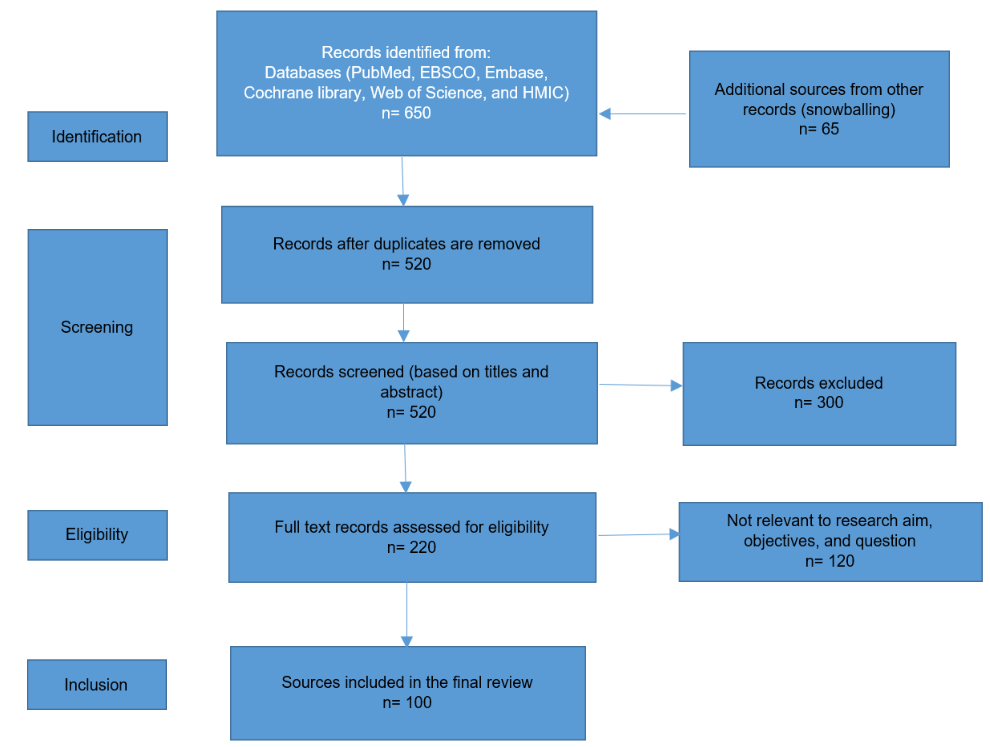
Literature Review and Results
Critique of the Research Studies
In this systematic review, the researcher identified 7 articles for critique. When critiquing the articles, the researcher intends to use the Critical Appraisal Skills Programme (CASP) Tools to achieve this goal. CASP was considered appropriate because it is a simple yet effective tool for assessing the validity and accuracy of an article’s presentation of information on a given issue. The researcher intends to critique each article separately to determine whether they accurately address their aims and are relevant to this study. Table 3 identifies the chosen articles, the guiding questions used, the number of participants, the methods employed, and the results presented based on the analysis conducted.
Table 3: Table of Results of the Articles
Critical Appraisal Skills Program Tools
It is necessary to critically appraise the seven articles shown in the table above. The researcher utilized the CASP tool to critically evaluate the articles. This tool focuses on determining the validity of the study, its results, and the report’s applicability in a local context.
Chen et al. (2020) Article
The validity of this study can be assessed by examining the sampling method, the participants, the methodology, the report of bias, and its reliability. The researcher defined clear inclusion/exclusion criteria to ensure that those included had specific knowledge that enabled them to respond to the research questions. A simple random sampling method was then employed to select participants, aiming to avoid bias in the participant selection process, as suggested by Tucker et al. (2021). A total of 1,166 nurse managers were included in the study. The researcher then used descriptive statistics and one-way ANOVA (t-tests) to analyze the participants’ data.
The study results indicate that a manager’s total Quick-EBP-VIK score is determined by their educational background, their professional title (which denotes EBP training), and the organization’s EBP culture and readiness. It means that nurses with greater knowledge of EBP are more likely to practice it than those with limited knowledge, an argument supported by Yoo et al.’s (2019) study. It also emphasizes the need to create a culture that supports the implementation of new concepts within an organization.
The results of this study will help inform local nurse manager actions in the country. Nurse Managers should recognize their critical role in promoting EBP among nurse practitioners under their supervision (Billings and Halstead, 2019; Hopp & Rittenmeyer, 2020). As leaders, they must recognize that they play a crucial role in fostering an environment that encourages their subordinates to experiment with new strategies (D’Souza et al., 2021). They need to make systems and resources available that enable nurses at their institutions to implement EBP in their daily activities.
Wakibi et al. (2021) Article
Assessing the validity of this source begins with defining its methodology: a systematic review that utilized a convergent qualitative synthesis method. This study was based on 250 secondary sources, selected using specific inclusion and exclusion criteria to ensure only trustworthy materials were included in the research. The criteria also enabled the elimination of all potential sources of bias in the study, thereby enhancing its reliability.
The study demonstrates that well-designed educational strategies enhance students’ knowledge and skills in EBNP. It means that nurses’ ability to apply evidence-based practice depends on their education. When they undergo thorough training and are assisted in understanding how to apply the concept, they can easily integrate it into their practice (Hung et al., 2019; Valentine, Sekula, and Lynch, 2020). The study emphasizes the need to redefine educational strategies to prioritize the tool.
Findings from this study can be applied locally, particularly to redefine the education system. The study shows that one significant barrier to the successful implementation of EBP is inadequate training among nurses. When nurses are adequately equipped with the relevant knowledge during their college education, they can easily apply it in their practice (Boswell et al., 2020). This means that educational authorities and policymakers should consider empowering nurses during their college years by redefining the curriculum.
Gómez-Salgado et al. (2023) Article
The validity of this study depends on the sampling of participants. The authors employed a stratified sampling method to select 755 nursing students, who subsequently participated in the study. They made an effort to ensure that all forms of bias are eliminated in the study, especially when selecting the participants and identifying secondary data sources. The chosen method for their research was a multicenter cross-sectional observational study. The steps these scholars took to enhance the study’s validity also made the outcome more reliable.
Findings suggest that nursing degree students are more likely to apply EBP concepts upon graduation if they demonstrate intermediate to high proficiency in EBP knowledge, skills, and attitudes, along with a strong sense of work commitment. The study shows that students with high knowledge of the EBP concept tend to practice it when they become registered nurses. The foundation of the attitude towards EBP is often developed while a student is in college (Jeanette & Pappas, 2020). As such, educators are responsible for ensuring that the principles of this concept are instilled in learners at the earliest possible stage.
The results will help promote the use of EBP locally among nurses nationwide. The study has identified college as the point at which nurses should be exposed to EBP. They should understand this concept and its principles, its significance, and the desirable application method (Raynolds et al., 2021). Local education stakeholders play a crucial role in ensuring that nursing students are exposed to sufficient, relevant information on evidence-based practice and its application.
Alqahtani et al. (2020) Article
The authors of this article were keen to enhance the study’s validity, which explains why they chose staff nurses, as they had the relevant knowledge about the issue being investigated. They used convenience sampling to select 277 staff nurses. However, this method has been criticized for sometimes failing to provide an accurate representation of the total population (Beanlands et al., 2019; Drummond et al., 2019). This may render the study’s outcome questionable. However, analysis of the sample used shows that it effectively represented the entire population and eliminated bias in the participant selection process. The researcher chose a cross-sectional correlational design as the preferred method for the project.
The results show that the nurses in the study felt a need to improve their theoretical knowledge and practical skills to actively participate in the process. They felt that although information about the benefits of EBP is widespread, knowledge of how to use it is limited. Nurses can’t apply a concept that they barely understand (Jamie et al., 2020; Collins et al., 2021). Without proper training, it is almost impossible for them to use it in their practice.
The results presented in this article will be beneficial in the local context. Although the sampling method was criticized as being less desirable, the findings indicate that the primary challenge in implementing EBP is limited knowledge among nurses. This issue has been identified in various jurisdictions worldwide (Coleman, 2019). This means that nurses need to be trained to equip them with the necessary knowledge to implement this concept effectively.
Shamsaee et al. (2021) Article
The article used convenience sampling to identify 79 nursing students for the study. Convenience sampling is often considered less ideal when assessing study validity. The article also faces criticism for using a relatively small sample to represent the entire population (Larsen et al., 2019). To enhance reliability, the researcher increased the number of secondary sources used in the study. They also made an effort to avoid bias when identifying the participants for the study.
The results of this study indicate that virtual education significantly affects the information-seeking skills and knowledge of nursing students. As Marlaine, Peggy, and Leslie (2022) reaffirm, virtual platforms provide additional avenues for nursing students to learn concepts such as evidence-based practice. In a world where technology plays a critical role in learning, colleges should leverage these platforms to equip learners with emerging skills, such as EBP. It requires the support of the management of learning institutions and other relevant stakeholders to make the necessary resources available to achieve these objectives.
The results presented in this article are particularly relevant in the local context. It highlights the importance of virtual platforms in promoting learning and enhancing information literacy among nursing students. It serves as a reminder to stakeholders that they need to invest in virtual education by providing the necessary infrastructure and support.
Rudman, A. et al. (2020) Article
The study’s validity assessment indicates that the researchers employed random sampling to select 2,474 registered nurses as participants. This sampling approach was vital to ensuring bias was eliminated in participant selection. An observational longitudinal study (unpaired t-tests) was the chosen method for the study. There were no reports of bias, as the approach of selecting participants effectively eliminated the issue. It meant the sample reliably represented the entire study population.
The study’s results show that registered nurses with specialist education and greater experience report a greater extent of EBP application, as do registered nurses who work in home care settings and outpatient settings. The study shows that nurses with specialized education and experience have a greater capacity to apply this concept. Factors such as the workplace setting and the facilities available to the nurse also influence the frequency of EBP adoption (Machaly et al., 2020; Grønkjær et al., 2023). Creating an enabling environment is crucial in enabling nurses to use this tool in their practice.
The results will be particularly helpful in the local context, as they outline the necessary steps to ensure nurses comply with EBP in their practice. Policymakers are reminded that they can define how often EBP can be used by making relevant resources available to nurses. Enabling them to gain the necessary workplace experience is also encouraged.
Al-Lenjawi, B. et al. (2022) Article
To assess the validity of this article, the researcher focused on determining various factors. It was evident that the researcher used convenience sampling to select 278 nurses as participants. This sampling method has a weakness in that it cannot reduce bias in a study (Ruggiri et al., 2019; Cacchione, 2020). The authors used a quantitative cross-sectional design to select participants for the study. They made an effort to enhance reliability by using a high number of secondary sources.
The results indicate that the major organizational barriers include a lack of time, limited support from colleagues during the implementation of research evidence, limited empowerment of nurses to change practice, and limited access to relevant research articles. These barriers make it challenging for nurses to adopt EBP in their practice (Tucker et al., 2019; Li, Cao, & Zhu, 2019). The study also indicated that there is limited goodwill among those in positions of power to eliminate these barriers. It is seen as an additional cost and as a factor that can lower nurses’ overall performance.
Results will help locally by focusing on and identifying barriers to implementing EBP and finding solutions. Management of local healthcare institutions plays a significant role in promoting the use of EBP in nursing practice. They should understand and appreciate the significance of EBP to eliminate these barriers (Green & Lori, 2019; Campbell et al., 2020). They must empower nurses not only through regular education but also by providing the necessary materials.
Results and Findings
Findings from the analysis indicate that the application of EBP in contemporary nursing practice has significant implications for nurse performance. The study shows that when nurses use EBP, they are less likely to make mistakes that could harm their patients’ health. This tool also enables them to learn new concepts and best practices that can improve their performance (Beckett et al., 2021; Azumah, Chandler, and Puntil, 2022). They get to apply the knowledge that is regularly published about nursing.
Gray and Grove (2020) and Younas and Quennell (2019) believe that it would make them better leaders. The challenge identified in the analysis is that the number of people using this concept is significantly low. For the few who use it, findings reveal that they use it only once a month or once a week at best. Those who use it at least once a day are less than 5% of the entire population (Veldhuizen et al., 2021; Taylor et al., 2021). This suggests that more efforts are needed to promote its use.
It became apparent that there is a need for close connection and coordination between nurses and administrators. For instance, one of the major themes that emerged was the need for policy relating to the use of EBP. It was evident that nurses tend to use the concept more often when their institutions have policies requiring it (Behrens & Langer, 2022; Kim, 2022). However, the researcher observed that if such policies are developed without involving nurses, they may fail to be implemented. Another theme was the ease of accessibility of the articles nurses need to refer to (Zhou et al., 2021; Ackley et al., 2020). When these materials are lacking, it becomes almost impossible to embrace the policy.
The systematic review indicates that EBP can be effectively implemented when goodwill exists among all relevant stakeholders. The researcher observed that nurses alone cannot effectively implement EBP unless they are properly trained and equipped with the relevant resources. This view aligns with the findings of numerous scholars, including Evans (2023) and Sutton (2021), who argue that this concept will be fully entrenched in nursing practice only if all stakeholders are actively involved.
The element that appears to be missing from the review is the role of patients (Shi, 2021; Tatli & Jette, 2022). It is unclear whether patients play a role in nurses’ ability to use EBP. The researcher’s overall assessment of the evidence presented is that EBP has positive implications for nursing practice; however, its effectiveness depends on nurses’ training and the availability of the materials necessary for its implementation. The evidence aligns with the topic’s primary subject matter, as it directly addresses the original research question.
Recommendations and Implications for Nursing
Summary of the Findings in Relation to the Research Question
Findings from the systematic review indicate that evidence-based practice directly affects nurses’ effectiveness in the modern nursing environment. The analysis indicates that EBP use fosters an environment in which nurses have clear guidelines for undertaking specific responsibilities. In many cases, these nurses face situations where they must make critical decisions while caring for a patient, especially in emergencies. In the absence of a physician, they may be the only option to save a patient’s life (Spencer, 2020; Jette, 2019). However, there is also the risk that when they make a mistake, their actions may worsen the patient’s condition and even cost them their life.
The use of EBP provides nurses with clear guidelines for addressing cases they encounter in healthcare institutions. Before deciding on how to care for a patient, healthcare professionals are expected to utilize existing evidence (Mitchell, 2020; Martijn, 2022). This step is designed to prevent them from taking actions that may worsen a patient’s condition. Kitson et al. (2021) and Skela-Savic et al. (2020) suggest that when uncertainties arise, nurses can rely on EBP to inform their actions and decisions.
Key Findings
The systematic review conducted has reaffirmed the importance of evidence-based practice in modern nursing. The findings reveal three main components of EBP, as shown in Figure 4. The first component is the utilization of the best external evidence. Labrague et al. (2019) explain that before taking a major action or decision, a nurse practitioner should use existing scientific evidence, a position supported by Steele and Monroe (2020). They are encouraged to avoid making decisions solely based on their views and perception of the condition. Instead, they need to ensure that their actions are supported by existing scientific evidence.

The second component involves drawing on individual clinical practice. Nurses are trained caregivers who possess the skills and expertise to make informed decisions about patient care (Dearholt et al., 2021; Gradone & Staffileno, 2019). They are required to draw on their clinical expertise whenever they are providing care to their patients. Although they are encouraged to utilize the best external evidence, they must rely on their individual clinical expertise to apply the knowledge gained from these sources (Cusack et al., 2019; Shayan, Kiwanuka, and Nakaye, 2019). Whenever they realize that external evidence contradicts their individual clinical expertise, they should seek the opinion of other experts to avoid costly mistakes that may harm the patient.
The third component is to consider the patient’s values and expectations. Nurses are required to understand and respect the rights of patients under their care. Values of one patient may be significantly different from those of another patient (Qin et al., 2020; Mathieson, Grande, and Luker, 2018). For instance, Christian beliefs differ in many ways from those of Muslims. A Muslim male may insist that only a male nurse can offer them the nursing care that they need based on their Islamic values. A nurse is expected to respect such values and assist the patient accordingly.
Findings reveal that although EBP has gained popularity among nurses worldwide, its practice remains uncommon. Data show that those who strictly follow this concept in their daily practice are fewer than 5% of nurses. The majority noted that they would follow the guidelines every month (Cardoso et al., 2021). The only way to ensure that the concept is widely practiced is to introduce policies that compel nurses to incorporate it into their practice. Findings of this study effectively answered the research question.
Implications for Nursing Practice and Recommendations
The findings of this study strongly suggest that nurses need to adopt evidence-based practice in their modern nursing practices. It is evident that nurses are aware of this concept and understand its significance. However, its application is not widespread among nurses as would be expected (McNett et al., 2021). Lack of strict regulatory policies, reluctance to embrace change, and the ease of using current methods are among the challenges to the effective implementation of EBP (Ramukumba & Amouri, 2019; Weberg & Davidson, 2021). Currently, nurses utilize EBP when deemed necessary. There are no established mechanisms to determine whether nurses effectively apply the concept. The following are the recommendations for nursing/practice that should be considered based on findings made:
- The DH, NICE, and WHO should develop guidelines to help assess whether nurses are using evidence-based practice in their daily work.
- There is a need to have policy guidelines and regulatory policies that would compel nurses to embrace EBP in their daily practice.
- Regular training for nurses is necessary to help them understand how to apply this concept as technology continues to evolve.
- Materials needed by nurses as external evidence to support their decisions and actions should be readily available in both print and electronic sources.
There is also a need for future scholars to consider the following in their quest to expand knowledge in this field:
- To investigate why the majority of nurses in both developed and developing nations do not prioritize EBP in their daily practice.
- To identify policies that can be developed both at the national and organizational levels to promote compliance.
- To investigate the best ways that relevant scientific evidence can be made easily accessible to nurses.
More research is needed to address some of the concerns raised by nurses who argue that implementing EBP in their daily practices is time-consuming and sometimes unnecessary. The researcher believes that further inquiry is necessary in this area of research to address the emerging knowledge gaps, as noted by Chien (2019) and Webb (2020). Both quantitative and qualitative research types will be necessary to address the issues identified above.
Limitations
It is essential to acknowledge the limitations encountered during the conduct of this study. One thing the researcher would do differently if there were a possibility of conducting this research again would be to rely more on primary data. This project relied heavily on secondary data available. However, primary data would have enabled the researcher to get the views of the nurses directly. The high speed at which technology is changing means that a publication made as recently as two years ago may already be outdated.
For instance, AI technologies have made significant progress over the past two years, redefining how knowledge is stored and shared (Kane & Linsley, 2022). How nurses felt that information should be available to them five years ago may not be the same way they want to access the same information today. As such, collecting primary data is the most effective way to gather the most recent information. This is a major limitation in doing this type of review. It limits the ability to obtain the most recent information on the issue being investigated.
The researcher made an effort to avoid any bias when collecting the articles. However, it is necessary to admit that priority was given to articles that were easily and freely available in the various databases explained above. It meant that articles that required expensive subscriptions to access their databases were excluded. Time was also an issue, which meant that the ease of access to the articles was prioritized. However, the quality of the materials used was prioritized over their accessibility. The databases mentioned in the methodology section were reliable in providing quality articles on this topic of interest.
Conclusion
It was revealed that the main implication of EBP in modern nursing practice is that it enhances efficiency. It significantly reduces errors among nurses and enables them to understand the current best practices. It allows nurses to conduct regular research and to understand emerging trends and practices in their field. Those who employ EBP are more likely to be innovative in their practice and more capable of utilizing modern tools and practices than those who do not.
The effectiveness of EBP application was determined to depend on several factors. The first factor that was identified was the level of training among the nurses. The study showed that nurses who have undergone thorough training on the concept and understand how it should be applied tend to use it more frequently than those with limited or no knowledge about it. Training of the nurses also helps them to appreciate the significance of EBP in their nursing practice. It was also revealed that the availability of the resources needed to apply the concept in practice was critical.
Nurses can only base their decisions and practice on scientific evidence if they are provided with relevant journal articles and other materials to support their work. The materials should be easily accessible and presented in a way that makes it easy to access the needed information. It also emerged that having policies promoting the use of EBP among nurses can enhance its application. When nurses realize that applying this concept is a requirement, they will be compelled to learn how to do so.
Recommendations for Nursing Practice
The outcome of this study has shown that EBP in modern nursing practice helps improve nurses’ performance. However, it was also evident that its implementation has faced various challenges. The following recommendations can help in addressing the identified challenges:
- Nurses should be adequately trained to ensure they understand the significance of EBP and how to apply it in their practice.
- Nurse managers should ensure that nurses have the resources that they need to effectively implement EBP.
- Administrations of various hospitals should enact policies that would force nurses to use EBP in their practice.
Recommendations for Research
There is a need for future scholars to explore this topic further to expand the field of knowledge. They should identify existing knowledge gaps and conduct studies to address them. The following are some of the recommended areas that still need further investigation:
- Future scholars should investigate the role that patients can play to encourage nurses to regularly use EBP in their practice.
- Future scholars should investigate why some nurses who already understand the significance of EBP and how to use it fail to apply it in their practice.
- There is a need to investigate how positive peer pressure among nurses can be used to encourage them to embrace EBP in their practice.
It is essential to note that a specific factor influenced the research process. A research article was published about the growing awareness of evidence-based practice in the country. The article reported that, although awareness of the concept was growing, its application was still significantly less common among nurses. The article outlined the numerous benefits that EBP offers, particularly in enhancing the efficiency of nurses. It explained that it is the best way for nurses to rapidly learn about the industry’s best practices and emerging technologies. The encounter motivated the researcher to conduct this study. It was necessary to understand the significance of EBP and the factors that can limit and encourage its application.
This field of study still requires further investigation to understand the various issues that have emerged in this study. One of the critical areas that would need further investigation is the role of patients in encouraging nurses to use EBP in their practice. Patients form the most important part of stakeholders in the healthcare system, and their views and input are often ignored when developing new concepts. There is a general feeling that patients will always accept any new practice that has direct benefits. However, sometimes it becomes necessary to involve them in the activity when developing new concepts. In this case, it would be interesting to investigate the role they can play in encouraging nurses to use EBP. Scholars should also investigate the role that emerging technologies play in facilitating the use of EBP in modern nursing practice.
Reference List
Ackley, J. et al. (2020) Nursing diagnosis handbook: an evidence-based guide to planning care. 12th edn. New York: Elsevier.
Al-Lenjawi, B. et al. (2022) ‘Evidence-based practice among critical care nurse’s/midwives in Qatar’, Open Journal of Nursing, 12(1), pp. 42-59.
Alqahtani, N. et al. (2020) ‘Nurses’ evidence-based practice knowledge, attitudes and implementation: a cross-sectional study’, Journal of Clinical Nursing, 29(2), pp. 274-283.
Azumah, D., Chandler, K. and Puntil, D. (2022) ‘Practice and the professional doctorate: a diffractive re-reading’, Journal of Further and Higher Education, 4(1), pp. 1-8.
Bankanie, V. et al. (2021) ‘Assessment of knowledge and compliance to evidence-based guidelines for VAP prevention among ICU nurses in Tanzania’, BMC Nursing, 20(209), pp. 1-13.
Beanlands, H. et al. (2019) ‘Decreasing stress and supporting emotional well-being among senior nursing students: a pilot test of an evidence-based intervention’, Nurse Education Today, 76(1), pp. 222-227.
Beckett, C. et al. (2021) ‘An integrative review of team nursing and delegation: implications for nurse staffing during COVID-19’, Sigma, 18(4), pp. 251-260.
Behrens, J. and Langer, G. (2022) Evidence based nursing and caring. Bern: Hogrefe.
Bidewell, J. et al. (2020) Understanding research methods for evidence-based practice in health. 2nd edn. Hoboken: Wiley.
Billings, M. and Halstead, J. (2019) Teaching in nursing e-book: a guide for faculty. 6th edn. London: Saunders.
Boswell, C. and Cannon, S. (2023) Introduction to nursing research: incorporating evidence-based practice. 6th edn. Jones & Bartlett Learning.
Boswell, C. et al. (2020) ‘Self-efficacy: changing the tide of evidence-based practice’, Sigma, 17(2), pp. 129-135.
Bumby, J. (2020) ‘Evidence-based interventions for retention of nursing students: a review of the literature’, Nurse Educator, 45(6), pp. 312-315.
Cacchione, P. (2020) ‘Innovative care models across settings: providing nursing care to older adults’, Geriatric Nursing, 41(1), pp. 16-20.
Campbell, L. et al. (2020) ‘Quad council coalition community/public health nursing competencies: building consensus through collaboration’, Public Health Nursing, 37(1), pp. 96-112.
Cardoso, D. et al. (2021) ‘Nursing educators’ and undergraduate nursing students’ beliefs and perceptions on evidence-based practice, evidence implementation, organizational readiness and culture: an exploratory cross-sectional study’, Nurse Education in Practice, 54(1), pp. 1-12.
Chen, L. et al. (2020) ‘Value, knowledge and implementation on evidence-based practice among nurse managers in China: A regional cross-sectional survey’, Journal of Nursing Management, 28(1), pp. 139-147.
Chien, L. (2019) ‘Evidence-based practice and nursing research’, Journal of Nursing Research, 27(4), p. 29.
Coleman, D. (2019) ‘Evidence based nursing practice: the challenges of health care and cultural diversity’, Journal of Hospital Librarianship, 19(4), pp. 330-338.
Collins, T. et al. (2021) ‘British association of critical care nurses: evidence-based consensus paper for oral care within adult critical care units’, Nursing in Critical Care, 26(4), pp. 224-233.
Combrinck, Y., Wyk, N. and Mogale, R. (2022) ‘Preserving nurses’ professional dignity: Six evidence-based strategies’, International Nursing Review, 69(1), pp. 106-113.
Craig, J. and Dowding, D. (eds.) (2019) Evidence-based practice in nursing. 4th edn. Amsterdam: Elsevier.
Cusack, L. et al. (2019) ‘Re-engaging concepts of professionalism to inform regulatory practices in nursing’, Journal of Nursing Regulation, 10(3), pp. 21-27.
D’Souza, P. et al. (2021) ‘Effectiveness of an evidence-based practice training program for nurse educators: a cluster-randomized controlled trial’, Sigma, 18(4), pp. 261-271.
Dang, D. et al. (2021) Johns Hopkins evidence-based practice for nurses and healthcare professionals: model and guidelines. 4th edn. Indianapolis: Sigma Theta Tau International.
Dearholt, S. et al. (2021) Johns Hopkins evidence-based practice for nurses and healthcare professionals. New York: Sigma Theta Tau International.
Degu, A. et al. (2022) ‘Evidence-based practice and its associated factors among point-of-care nurses working at the teaching and specialized hospitals of Northwest Ethiopia: a concurrent study’, PLoS ONE, 17(5), pp. 1-18.
Drummond, S. et al. (2019) ‘Partial thromboplastin time, implantable port, coagulation panel, venipuncture, blood draw’, Clinical Journal of Oncology Nursing, 23(4), pp.431-433.
Ellis, P. (2022) Evidence-based practice in nursing. London: SAGE Publications.
Evans, D. (2023) Making sense of evidence-based practice for nursing: an introduction to quantitative and qualitative research and systematic reviews. London: Routledge.
Gallagher-Ford, L. et al. (2020) ‘The effects of an intensive evidence-based practice educational and skills building program on EBP competency and attributes’, Sigma, 17(1), pp. 71-81.
Godshall, M. (2020) Fast facts for evidence-based practice in nursing. 3rd edn. New York: Springer Publishing Company LLC.
Gómez-Salgado, J. et al. (2023) ‘Commitment, perception and evidence-based practice training in Spanish nursing students: A multi-centre cross-sectional study’, Journal of Clinical Nursing, 32(6), pp. 715-725.
Gradone, L. and Staffileno, B. (2019) ‘Integration of evidence-based practice at an Academic Medical Center’, Medsurg Nursing, 28(1), pp. 53-58.
Gray, J. and Grove, S. (2020) Burns and grove’s the practice of nursing research: appraisal, synthesis, and generation of evidence. London: Elsevier Health Sciences.
Gray-Miceli, D. et al. (2021) ‘A framework for delivering nursing care to older adults with COVID-19 in nursing homes’, Public Health Nursing, 38(4), pp. 610-626.
Green, C. and Lori, J. (2019) ‘Should nursing be considered a STEM profession’, Nursing Forum, 55(2), pp. 205-210.
Grønkjær, M. et al. (2023) ‘Establishing and leading a cross-institutional partnership to integrate fundamentals of care into clinical practice, nursing education and research’, Journal of Advanced Nursing, 79(3), pp. 951-960.
Grove, S. and Cipher, J. (2019) Statistics for nursing research: a workbook for evidence-based practice. 3rd edn. New York: Elsevier.
Haber, J. et al. (2020) Nursing and midwifery research: methods and appraisal for evidence-based practice. Melbourne: Elsevier Health Sciences.
Happell, B. et al. (2019) ‘Developing an evidence-based specialist nursing role to improve the physical health care of people with mental illness’, Issues in Mental Health Nursing, 40(10), pp. 832-838.
Heinen, M. et al. (2019) ‘An integrative review of leadership competencies and attributes in advanced nursing practice’, Journal of Advanced Nursing, 75(11), pp. 2378-2392.
Hopp, L. and Rittenmeyer, L. (2020) Introduction to evidence-based practice: a practical guide for nursing. London: F.A. Davis.
Houser, J. (2023) Nursing research: reading using and creating evidence. 5th edn. Burlington: Jones & Bartlett Learning.
Hung, H. et al. (2019) ‘Evidence-based practice curriculum development for undergraduate nursing students: the preliminary results of an action research study in Taiwan’, Journal of Nursing Research, 27(4), pp. 30-31.
Jamie, M. et al. (2020) ‘The effect of an evidence-based practice education and mentoring program on increasing knowledge, practice, and attitudes toward evidence-based practice in a rural critical access hospital’, Journal of Nursing Administration, 50(5), pp. 281-286.
Jeanette, E. and Pappas, S. (2020) ‘The value of nursing research’, Journal of Nursing Administration, 50(5), pp. 243-244.
Jette, E. (2019) ‘The curse of bureaucratisation or the blessings of professionalisation? Nurses’ engaged adoption of quality management in hybrid managerial positions’, Scandinavian Journal of Management, 35(3), pp. 2-8.
Jolley, J. (2020) Introducing research and evidence-based practice for nursing and healthcare professionals. London: Taylor & Francis Group.
Kane, R. and Linsley, P. (2022) Evidence-based practice for nurses and allied health professionals. London: SAGE Publications.
Katowa, P. et al. (2021) ‘Implementing evidence-based practice nursing using the PDSA model: process, lessons and implications’, International Journal of Africa Nursing Sciences, 14(1), pp. 5-12.
Kim, J. et al. (2019) ‘Performance and influencing factors of evidence-based pressure ulcer care among acute care hospital nurses’, Sigma, 16(1), pp. 29-35.
Kim, M., Mallory, C. and Valerio, D. (2022) Statistics for evidence-based practice in nursing. 3rd edn. Burlington: Jones & Bartlett Learning.
Kim, T. (2022) ‘Patient safety as a global health priority’, Cardiovascular Therapy and Prevention, 21(10), pp. 3-9.
Kitson, A. et al. (2021) ‘How nursing leaders promote evidence-based practice implementation at point-of-care: a four-country exploratory study’, Journal of Advanced Nursing, 77(5), pp. 2447-2457.
Labrague, L. et al. (2019) ‘A multicountry study on nursing students’ self-perceived competence and barriers to evidence-based practice’, Worldviews on Evidence-Based Nursing, 16(3), pp. 236-246.
Larsen, C. et al. (2019) ‘Methods for teaching evidence-based practice: a scoping review’, BMC Medical Education, 19(259), pp. 2-9.
Li, S., Cao, M., and Zhu, X. (2019) ‘Evidence-based practice: knowledge, attitudes, implementation, facilitators, and barriers among community nurses-systematic review’, Medicine, 98(39), pp. 1-9.
Lunden, A. et al. (2020) ‘Readiness and leadership in evidence-based practice and knowledge management: a cross-sectional survey of nurses’ perceptions’, Nordic Journal of Nursing Research, 41(4), pp. 187-196.
Machaly, E. et al. (2020) ‘Effect of implementing evidence-based nursing guidelines on nurses’ performance about care provided for children undergoing hemodialysis’, Journal of Nursing and Health Science, 9(3), pp. 21-28.
Marlaine, C., Peggy, L. and Leslie, N. (2022) ‘Knowledge for nursing practice: beyond evidence alone’, Research and Theory for Nursing Practice, 35(1), pp. 3-9.
Martijn, F. (2022) ‘The rise of the partisan nurse and the challenge of moving beyond an impasse in the (re)organization of Dutch nursing work’, Journal of Professions and Organization, 9(2), pp. 20-37.
Mathieson, A., Grande, G. and Luker, K. (2018) ‘Strategies, facilitators and barriers to implementation of evidence-based practice in community nursing: a systematic mixedstudies review and qualitative synthesis’, Primary Health Care Research & Development, 20(6), pp. 1-11.
McCrae, N. and Purssell, E. (2020) How to perform a systematic literature review: a guide for healthcare researchers, practitioners and students. Berlin: Springer International Publishing.
McNett, M. et al. (2021) ‘Advancing evidence-based practice through implementation science: critical contributions of Doctor of Nursing practice- and Doctor of Philosophy-prepared nurses’, Worldviews on Evidence-Based Nursing, 18(2), pp. 93-101.
Melnyk, M. and Fineout-Overholt, E. (2019) Evidence-based practice in nursing & healthcare: a guide to best practice. 4th edn. Philadelphia: Wolters Kluwer.
Mitchell, P. (2020) ‘Nursing science and health policy: Opportunities in the year of the nurse and the midwife’, International Nursing Review, 67(1), pp. 1-3.
Norful, A. et al. (2022) ‘Nursing perspectives about the critical gaps in public health emergency response during the COVID-19 pandemic’, Sigma, 55(1), pp. 22-28.
Patole, S. (2021) Principles and practice of systematic reviews and meta-analysis. Berlin: Springer International Publishing.
Petrovic, K., Hack, R. and Perry, B. (2020) ‘Establishing meaningful learning in online nursing post-conferences: a literature review’, Nurse Educator, 45(5), pp. 283-287.
Qin, X. et al. (2020) ‘Integrating the best evidence into nursing of venous thromboembolism in ICU patients using the ‘i-PARIHS framework’’, Plos One, 6(1), pp. 1-16.
Ramukumba, M. and Amouri, S. (2019) ‘The implementation of evidence-based practice in a United Arab Emirates Hospital’, Africa Journal of Nursing and Midwifery, 21(1), pp. 4-14.
Raynolds, S. et al. (2021) ‘Results of the chlorhexidine gluconate bathing implementation intervention to improve evidence-based nursing practices for prevention of central line associated bloodstream infections study: A stepped wedge cluster randomized trial’, Implementation Science, 16(45), pp. 3-9.
Rivera, R. and Fitzpatrick, J. (2021) The peace model evidence-based practice guide for clinical nurses. Hoboken: Sigma Theta Tau International.
Rudman, A. et al. (2020) ‘Registered nurses’ evidence-based practice revisited: a longitudinal study in mid-career’, Sigma, 17(5), pp. 348-355.
Ruggiri, J. et al. (2019) ‘Implementing post-discharge 48-hour scripted call for patients with heart failure: an evidence-based practice quality improvement project’, Medsurg Nursing, 28(3), pp. 183-187.
Schmidt, A. (2021) Evidence-based practice for nurses: appraisal and application of research. Hoboken: Jones & Bartlett Learning.
Shamsaee, M. et al. (2021) ‘Assessing the effect of virtual education on information literacy competency for evidence-based practice among the undergraduate nursing students’, BMC Medical Informatics and Decision Making, 21(48), pp. 8-12.
Shayan, J., Kiwanuka, F. and Nakaye, Z. (2019) ‘Barriers associated with evidence-based practice among nurses in low- and middle-income countries: a systematic review’, Worldviews on Evidence-Based Nursing, 16(1), pp. 12-20.
Shi, Y. (2021) ‘An assessment of the reliability and validity of the Chinese version of the reporting of clinical adverse events scale for nursing interns: a cross-cultural adaptation of scales and online investigation’, Nurse Education in Practice, 57(24), pp. 1-11.
Skela-Savic, B. et al. (2020) ‘Teaching evidence-based practice (EBP) in nursing curricula in six European countries- a descriptive study’, Nurse Education Today, 94(1), pp. 1-7.
Spencer, T. (2020) ‘Improving diversity of the nursing workforce through evidence-based strategies’, Journal of Nursing Education, 59(7), pp. 363-364.
Stannard, D. (2019) ‘A practical definition of evidence-based practice for nursing’, Journal of Perianesthesia Nursing, 34(5), pp. 1080-1084.
Steele, B. and Monroe, H. (2020) Christian ethics and nursing practice. New York: Cascade Books.
Sutton, N. (2021) Evidence based practice nurse: Amazon digital services LLC. London: KDP Print.
Tanner, A. and Stanislo, K. (2022) ‘School nursing research and research implementation priorities’, Impact Factor, 38(6), pp. 3-8.
Tatli, A. and Jette, E. (2022) ‘Knowledge legitimacy battles in nursing, quality in care and nursing professionalization’, Journal of Professions and Organization, 1(3), pp. 1-16.
Taylor, S., et al. (2021) ‘The effect of sensory discrimination training on sensorimotor performance in individuals with central neurological conditions: a systematic review’, British Journal of Occupational Therapy, 1(1), pp. 1-13.
Tucker, S. et al. (2019) ‘Patient, nurse, and organizational factors that influence evidence-based fall prevention for hospitalized oncology patients: an exploratory study’, Sigma, 16(2), pp. 111-120.
Tucker, S. et al. (2021) ‘Implementation science: application of evidence-based practice models to improve healthcare quality’, Sigma, 18(2), pp. 76-84.
Tucker, J. et al. (2022) Evidence-based practice in action: comprehensive strategies, tools, and tips from University of Iowa Hospitals & Clinics. Hoboken: Sigma Theta Tau International.
Tworek, B. (2019) ‘Examining the impact of knowledge translation interventions on uptake of evidence-based practices by care aides in continuing care’, Sigma, 16(1), pp. 21-28.
University of St. Augustine for Health Sciences. (2020) The role of evidence-based practice in nursing.
Valentine, J., Sekula, K. and Lynch, V. (2020) ‘Evolution of forensic nursing theory: introduction of the constructed theory of forensic nursing care: a middle-range theory’, Journal of Forensic Nursing, 16(4), pp. 188-198.
Veldhuizen, J. et al. (2021) ‘Evidence-based interventions and nurse-sensitive outcomes in district nursing care: a systematic review’, International Journal of Nursing Studies Advances, 3(1), pp. 3-9.
Wakibi, S. et al. (2021) ‘Teaching evidence-based nursing practice: a systematic review and convergent qualitative synthesis’, Journal of Professional Nursing, 37(1), pp. 135-148.
Webb, L (2020) Communication skills in nursing practice. London: SAGE Publications.
Weberg, D. and Davidson, S. (2021) Leadership for evidence-based innovation in nursing and health professions. 2nd edn. Burlington: Jones & Bartlett Learning.
White, K., Terhaar, F. and Dudley-Brown, S. (eds.) (2019) Translation of evidence into nursing and health care. London: Springer Publishing.
Yoo, J. et al. (2019) ‘Clinical nurses’ beliefs, knowledge, organizational readiness and level of implementation of evidence-based practice: the first step to creating an evidence-based practice culture’, Plos ONE, 3(1), pp. 4-16.
Younas, A. and Quennell, S. (2019) ‘Usefulness of nursing theory-guided practice: an integrative review’, Scandinavian Journal of Caring Sciences, 33(3), pp. 540-555.
Zhou, Y. et al. (2021) ‘Application of evidence-based nursing in patients with acute myocardial infarction complicated with heart failure’, American Journal of Translational Research, 13(5), pp. 5641-5646.