Advantages of Breastfeeding
- Benefits for child’s health (Clark & Bungum 2003):
- Development of greater resistance to infectious diseases in breastfed children.
- Development of stronger immune systems in breastfed children.
- Low rates of chronic diseases (e.g. leukaemia, diabetes, asthma) in breastfed children.
- Benefits for mother’s health (Buckley & Charles 2006):
- Lower risk of breast cancer.
- Decreased risk of mastitis.
- Lower risk of development of type 2 diabetes.
- Economic Benefits (Clark & Bungum 2003):
- Families spend less (or no money) on ABM (artificial baby milk).
- Countries spend less on health care services as the rates of some diseases decrease.
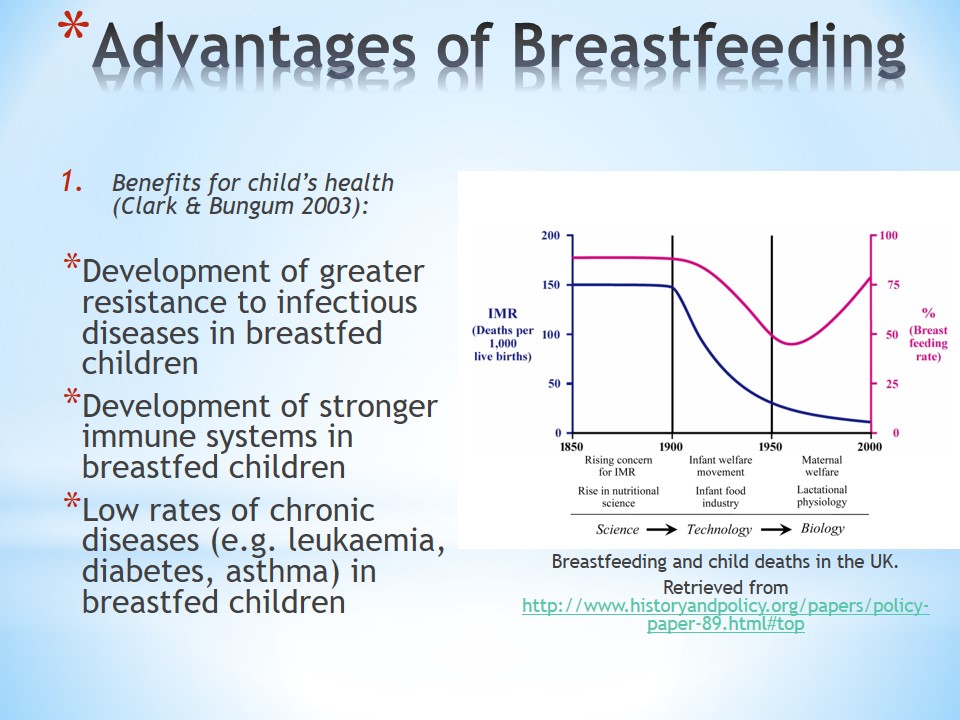


Disadvantages of Breastfeeding
There are quite a few disadvantages of breastfeeding:
- Transmission of diseases (Giugliani 2004):
- *Such diseases as HIV can be transmitted during breastfeeding.
- *Infectious diseases can also be transmitted from mother to child during breastfeeding.
- Possible negative effects of breastfeeding:
- Such disease as mastitis and such inconvenience as damage to nipples is sometimes associated with breastfeeding.


Addressing the disadvantages
Notably, the disadvantages mentioned above may be avoided:
- Infected mothers can resort to a wet-nurse or ABM.
- The use of correct breastfeeding strategies prevent new mothers from developing a variety of diseases and disorders.

Reference List
Buckley, KM & Charles, GE 2006, ‘Benefits and challenges of transitioning preterm infants to at-breast feedings’, International Breastfeeding Journal 1.13, pp. 1-7.
Clark, SGJ & Bungum, TJ 2003, ‘ The benefits of breastfeeding: an introduction for health educators’, Californian Journal of Health Promotion 1.3, pp. 158-163.
Giugliani, ERJ 2006, ‘Common problems during lactation and their management’, Journal de Pediatria 80.5, pp. 147-154.