Background
The proposed process for improving the operating room involves ensuring cleanliness, efficient resource utilization, and minimizing waiting times. First, the main factors affecting efficiency should be identified and noted. A systematic approach to data collection is used to analyze events, their causes, and their impact on the department’s performance. Due to the involvement of all staff and a focus on employee responsibility, the process is feasible. Improved coordination between employees ensures efficient execution of all operations.
Key Factors Contributing to Hospital and Operating Room Efficiency
Hospital efficiency plays a significant role in improving patient and employee satisfaction. Factors such as ensuring cleanliness, reducing wait times, and utilizing resources efficiently are key to achieving hospital efficiency. Additionally, ensuring the hospital’s efficiency protects patients from the risks of negative experiences and health deterioration. Ensuring cleanliness in the operating room plays a crucial role in patient safety, which in turn affects patient satisfaction.
Certain high-touch surfaces should be cleaned more frequently, and the compliance with cleaning requirements should be higher (Feusner et al., 2023). Cleanliness in the operating room protects patients from potential infections that could lead to complications or even death. In addition, maintaining a high standard of cleanliness enables the institution to establish a strong reputation that distinguishes it from others in a positive manner. Reducing the processing time of requests will increase the flow of patients and reduce their waiting time.
The use of machine learning and optimization will minimize delays (Fairley et al., 2018). Due to specialized equipment, medical staffing, sterilization factors, and other issues, the operating room is a major cost center throughout the hospital. By managing operating room cost planning more effectively, positive changes can be made to improve hospital efficiency (Fairley et al., 2018). Therefore, the process of improving hospital efficiency is important and consists of integral factors of ensuring cleanliness, optimizing processes, and rational use of resources.
Minimizing waiting times, rational use of resources, and cleanliness in the operating room are key aspects to ensuring hospital efficiency. Cleanliness in the operating room protects patients from infections and complications (Feusner et al., 2023). This helps to avoid prolonging treatment time and increasing the cost of additional medical services. The rational use of resources encompasses financial planning, calculating time for procedures, setting staff schedules, and other related activities (D. J. Lee et al., 2019). This aspect helps ensure the quality of work without increasing, and sometimes even reducing, costs.
Minimizing waiting time enables the efficient use of time, ultimately leading to the satisfaction of both staff and patients. The work schedule provides staff with the opportunity to plan and manage time and patients, to reduce the time spent in queues. This will also have a financial impact, as effective time planning will allow you to see more patients and perform higher-quality surgeries. Therefore, these factors are the most suitable for improving hospital efficiency because they are fundamental and lead to practical changes.
Benefits and Challenges of Implementation
The benefits of implementing this process include improved customer experience, increased productivity, and financial sustainability. Reduced waiting time in queues, high-quality procedures, and adherence to cleanliness standards leave patients with only pleasant emotions. Hospital productivity is achieved by minimizing expectations and applying process optimization and machine learning methods (Fairley et al., 2018). Rational allocation of resources, reduced costs for serviced equipment, energy consumption, and so on, allows for predicting the hospital’s expenses and income, which ensures financial stability.
Negative aspects, such as the need for training, changes in workflow, and additional costs, are also available. New approaches often require changes, which can lead to resistance from staff or disagreements about new practices. Training on new changes is necessary for staff to understand and ensure quality (D. J. Lee et al., 2019). This may include the development of training programs, workshops, and other methods, which require additional resources in the form of mentors and finances. Although the changes implemented in the future will lead to lower costs in the initial stages, they will also incur additional costs, which can be a negative aspect. Investments are needed in additional means for disinfecting operating rooms, staff retraining, and updated equipment.
The process of improving efficiency is a lengthy and multi-stage process. First, it is necessary to analyze the current situation in the hospital, taking into account the initial state of affairs and identifying opportunities for improvement. Cleanliness standards should be set and followed in the future. Attention should be paid to ensuring cleanliness throughout the operating room, both in the center and on the periphery. The next step is to develop processes for optimization and mechanization. For example, a model that incorporates machine learning and integer programming helps determine the sequence of surgical procedures in a short time, reducing costs and improving staff and patient satisfaction (Fairley et al., 2018).
The last stages will include monitoring of the implemented changes, reporting, and communication with patients. Data from the initial stage should be compared with actual results and goals. Reporting should be conducted at all levels of staff to ensure open communication and a clear understanding of the implementation’s effectiveness. Communication with patients will help to understand their feedback and satisfaction with the changes implemented. This will help to update the process to ensure patient comfort and satisfaction.
Implementation Strategy, Timeline, Costs, and Evaluation
The implementation timeline can vary and be modified during the process, but in general terms, it typically includes four main stages and takes from six months to a year to complete. The analysis and planning stage will take one to two months. It will involve assessing the current state of the hospital, identifying key performance indicators and key goals for optimization, and selecting a team of staff to lead the implementation process (D. J. Lee et al., 2019).
Both the second and third stages are expected to last one to two months each. These phases will encompass the implementation phase, followed by the necessary correction process. The last stage of monitoring and updates can continue throughout all stages and after implementation, as it ensures that the quality of results is assessed, and strategies are adjusted based on the monitoring data.
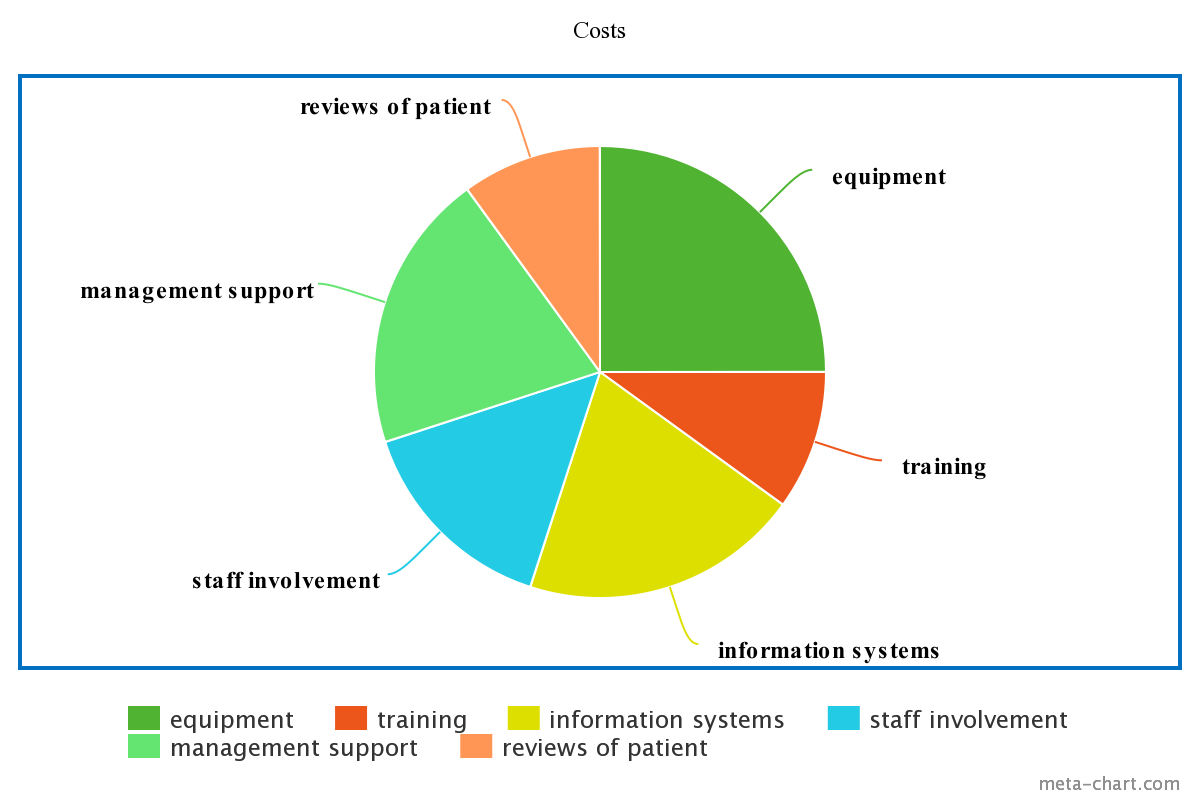
The cost of implementing the changes can be up to $200,000, but once implemented, it will pay for itself within the time of implementation and bring profit in the form of financial stability for the hospital, patient satisfaction, and efficient use of resources. Monetary resources include the cost of equipment, information systems, and training. Equipment will minimize waiting times and improve the quality of cleanliness, and costs up to $100,000.
Information systems include process optimization software, data monitoring and analysis systems, and can cost between $20,000 and $40,000 (Fairley et al., 2018). Training can cost anywhere from $0, in the case of self-study, to $20,000, in the case of implementing workshops, inviting experts, and other similar expenses. Management buy-in, staff involvement, and patient support are essential non-informational resources.
The success of the proposed change will be evaluated by comparing the initial data at the analysis stage with the actual results after the process is implemented. This data will include aspects such as staff and patient satisfaction, efficient allocation of resources, waiting times in queues, and incidence of infection (D. J. Lee et al., 2019). Information technology will allow you to continuously measure and receive daily reports with this data. In the case of reducing waiting time, the frequency of infection, instead of increasing the efficiency of resource allocation and improving staff satisfaction, the implementation of this idea will be successful.
References
Fairley, M., Scheinker, D., & Brandeau, M. L. (2018). Improving the efficiency of the operating room environment with an optimization and machine learning model. In Health Care Management Science (Vol. 22, Issue 10). Springer Science+Business Media.
Feusner, B., Alderman, S. M., & Heishman, C. (2023). Equipment and surface location in operating rooms and potential impact on terminal clean effectiveness. American Journal of Infection Control, 51(7), S21.
Lee, D. J., Ding, J., & Guzzo, T. J. (2019). Improving operating room efficiency. Current Urology Reports, 20(6).