Introduction
The primary focus of the current literature review is on the effectiveness of end-of-life palliative care (PC), with a particular emphasis on patients’ perceptions of this care. Based on Collins et al. (2018), which identified three main key statements, four additional relevant sources were found. These include Collins et al. (2021), Ekberg et al. (2019), Farabelli et al. (2020), and Reigada et al. (2020). When discussing various aspects of palliative care, the selected articles support the key ideas presented in the primary source. All the materials contribute to uncovering an understanding of the challenges and opportunities for quality end-of-life care and emphasize the importance of reducing the stereotypical notion of PC.
Search Strategy
Appropriate resources and guidelines were used in creating the search strategy. The search tool included the USC Library (n.d.), Google Scholar, and PubMed sources. The help tools and citation prompts (Library help, n.d.; APA Style, n.d.) were undoubtedly useful. Keywords from Collins et al.’s (2018) discussion topics were used to match search results, including palliative care, death euphemism, dying, end-of-life communications, and combinations of these elements. Filters were included to provide searches in English and in the publication period from 2019 to 2023. Relevant topic filters were also used, especially “Communication” and “Palliative Care.”
Findings
This literature review has selected four articles that are most relevant to aspects of communication in palliative care and patients’ perceptions of these services. While not all articles discuss the same key points, they are relevant to the overall discussion of palliative care and interactions with nursing staff at the end of life, and demonstrate agreement with the points outlined in the main article (Collins et al., 2018). This phenomenological study aimed to gain an understanding of patients’ attitudes and reactions to palliative care messages, to identify patterns and biases.
Thus, three key themes for discussion were identified, which are reflected in a multitude of parallel sources cited as confirmed facts (Brooks et al., 2020; Kremling et al., 2022). Among these themes are reluctance to talk about death, association of PC with death, and aversion to PC because of this perception (Table 1). Relevant ideas are highlighted in the table and by the interpretation of other sources.
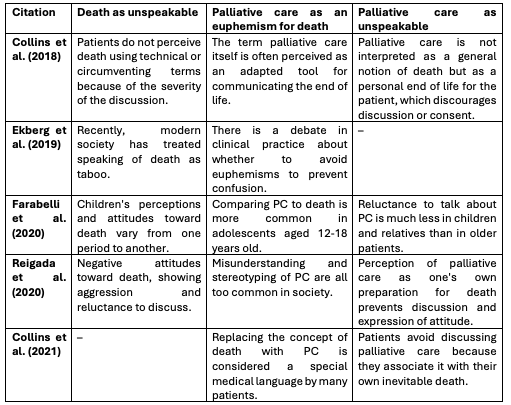
Palliative Care Communication
To justify the correctness of the selection of the other articles, a brief description of them and their relation to the topic should be given. For example, the article by Ekberg et al. (2019) also focuses on palliative care communication, examining the use of implicit or ambiguous terms by patients when discussing it. She additionally emphasizes the difficulties and necessary caution that must be exercised when communicating with severely ill patients, in parallel with the importance of showing understanding and consistency in such conversations.
Pediatric Specifics
Additional factors in the discussion are the focus on pediatric settings and the perception of PC as unspeakable by young patients or relatives (Ekberg et al., 2019; Schuelke et al., 2021). The study’s results confirm not only the key themes chosen but also provide suggestions for improving patient perceptions and nurses’ communication skills in these situations.
An equally important issue related to the negative interpretation of PC is the opinion and understanding of the situation by relatives of terminally ill patients. Farabelli et al. (2020) discuss psychosocial and family support as essential in their work, while emphasizing the validity of Collins et al.’s (2018) findings.
Like the previous one, this work highlights pediatric cases of palliative care and emphasizes the dependence of attitudes toward it on patients’ personal perceptions of death. Moreover, it highlights the roles of social workers and nurses as significant in addressing patients’ social, emotional, and existential problems. Ten basic tactics in communication are highlighted to increase the effectiveness of their work with people and to provide comprehensive care not only to patients but also to their families.
Patient Perception of Palliative Care
The third supplemental article is chosen because of its relevance to reviewing patients’ experiences. Reigada et al. (2020) believe that personal perception determines whether one views palliative care as a treatment or not. Using a meta-synthesis, the authors evaluate perceptions of communication in a given end-of-life setting and identify honest, empathetic, and appropriate communication by nursing staff as the primary tool for building trust.
Moreover, like other researchers, the authors emphasize the importance of promoting patient-centered care and reducing anxiety as crucial factors in the care context (Reigada et al., 2020; Palliative Care Australia, n.d.). Thus, this support for the main ideas is present in the generalized analysis of patient response to PC, confirming the existence of the problem.
The fourth article is the least related to the discussion of the emphasized points of the main one, but likewise correlates with them. This article was also written by Collins and Philip, only with different co-authors (Collins et al., 2021). It is a newer interpretation of the authors’ primary ideas, but alongside the consideration of public PC and its impact on healthcare outcomes, one of the main problems remains the issue of perception.
The association of such medical care with death, complete with an aversion to death, exacerbates the outcomes of consent decisions (Kuosmanen et al., 2021). Moreover, increased efforts by medical staff to destigmatize the concept are necessary, and usually, such efforts are insufficient (Olsson et al., 2021; Gonella et al., 2019). In some situations, medical professionals quite officially use PC as a euphemism for imminent death, which is an unacceptable aggravation.
Discussion
This section examines three key discussion points in the context of a critical appraisal of selected and supporting sources. Identified in the Collins et al. (2018) study, these three points are discussed in turn and are important details of contemporary palliative care. By engaging with the relevant literature, patients’ general attitudes toward nursing care at the end of life are determined and complemented by the propriety of adhering to national standards or other guidelines.
Death as Unspeakable
This issue is raised because of the complexity of a person’s perception of approaching death, which does not contribute to motivation and coping with the disease. Collins et al. (2018; 2021) highlight patients’ use of ambiguous language or technical terms in an attempt to avoid emotionally complex terminology.
Undoubtedly, the existence of such a factor cannot be denied, and more often than not, significant deterioration of health is accompanied by severe psychological problems – depression, frustration, and instability (Tang et al., 2021). Thus, in today’s society, talking about death outside the hospital room has become taboo (Ekberg et al., 2019). It is most likely due to a historically substantial increase in life expectancy and quality of life, as well as a decrease in people’s daily encounters with death, which was common in underdeveloped medicine.
Different attitudes to death are also noted in people of different generations. Each stage of adulthood is typically associated with distinct levels of emotionality and perceptions of the dying process (Farabelli et al., 2020). Researchers have listed observable features, and the greatest fear of death in the awareness of its inevitability is experienced by older patients (Omori et al., 2022). Moreover, negative emotions may include normal reactions that include anger, displays of aggression, denial, and reluctance to discuss (Reigada et al., 2020). Thus, the general social view of aversion to death is shaped by human culture, and news about terminal illnesses may not be positive for anyone, regardless of the situation.
Additionally, attention must be paid to the effectiveness of communication, which is vital in overcoming the barriers of inexpressibility. Competent, open, and empathetic dialogue can create a safe space for patients to express their concerns and fears, and to receive all necessary information about palliative care. Active listening and response validation techniques should be employed in a manner that respects the patient’s pace and willingness to communicate (Registered Nurse Standards for Practice, n.d.). This fact is further emphasized by the national standards for palliative care, which stipulate that creating a supportive environment for patients and their relatives is a prerequisite.
PC – Euphemism for Death
Such associativity is a logical extension of the previous thesis and requires a significant level of effort and revision of the medical system to minimize this stereotype. Many patients perceive PC as an adapted tool to discuss imminent death without using frightening and taboo words (Collins et al., 2018; Habeck-Fardy, 2021). That said, even specially prepared wards with designated areas for care for these patients are considered by many to be places of death instead of places of life, which they are not. Care is calculated to improve people’s condition, and positive outcomes exist (Ryan et al., 2020).
Moreover, there is an ongoing debate about completely banning the use of the concept of PC solely in a negative sense, even in intra-collaborative communication (Ekberg et al., 2019). Support for such an initiative could be considered mandatory because patients could witness such a thing, which would only increase associativity. In this regard, one can confirm the authors’ truthful expression.
Comparing care to death is also often not possible in understanding child patients or younger relatives of patients. Such euphemisms and stereotypes are more likely to be used by adults, as noted by Farabelli et al. (2020). At the same time, medical terminology does not imply a direct reference to death by medical personnel, which contributes to this occurrence of prejudice.
Reigada et al. (2020) note that such misinterpretations of the PC purpose are common in society. For the same reason, many patients believe that the term is indeed an official substitute for the concept of death (Collins et al., 2021). In this situation, all of the authors are correct, and further work should be done among nursing staff to reduce the incorrect use of the concepts.
Palliative Care as Unspeakable
Corresponding to the first two statements, the third is their logical continuation. It can be considered a result of prejudice, and it is crucial to assess the root causes identified above to eliminate this problem. The importance lies in perceiving the PC offers as a personal death sentence and failing to receive needed treatment because of the refusal (Collins et al., 2018; Collins et al., 2021).
The problem can often be seen in cases of ill children when their relatives deny them a chance and medical care because of personal bias and stereotypical thinking (Farabelli et al., 2020). At the same time, the danger that such a situation can pose to society should not be overlooked – denying the possibility of death cannot stop the inevitable, just as all things should be called by their proper names. Preparing for death, as some perceive, palliative care is, if not an attempt to save, prolong or cure, then at least to provide relief in situations of physical and emotional suffering.
For the same reason, education and awareness-raising are crucial for changing one’s attitudes about the purpose and meaning of PC, which is highlighted and emphasized in the standards in parallel to the obligatory initiation of discussion of such care in the early stages of the disease to prepare and ensure timely consent and access (Registered nurse standards for practice, n.d.). Patient-centered care and psychosocial support are also crucial in addressing the causes of this misperception of care, as highlighted by researchers (Ryan et al., 2020). Thus, along with other key issues, there is one major discussion about the incorrect association of PC with death, which only brings problems.
Conclusion
In summary, this literature review has addressed the three key communication issues related to palliative care at the end of life, as articulated at the beginning of this paper. These issues bring to the forefront the cultural and social barriers surrounding discussions of PC and death, defining misconceptions and unfounded fears. By applying effective communication strategies, fostering open dialogue, and dispelling misconceptions, a better understanding of PC can be achieved, facilitating and enhancing the quality of professional profiles.
References
APA Style Main Page. (n.d.). American Psychological Association.
Brooks, J. V., Poague, C., Formagini, T., Sinclair, C. T., & Nelson-Brantley, H. V. (2020). The role of a symptom assessment tool in shaping patient-physician communication in palliative care. Journal of Pain and Symptom Management, 59(1), 30–38.
Collins, A., Brown, J. E. H., Mills, J., & Philip, J. (2021). The impact of public health palliative care interventions on health system outcomes: A systematic review. Palliative Medicine, 35(3), 473–485.
Collins, A., McLachlan, S.-A., & Philip, J. (2018). Communication about palliative care: A phenomenological study exploring patient views and responses to its discussion. Palliative Medicine, 32(1), 133–142.
Ekberg, S., Danby, S., Rendle-Short, J., Herbert, A., Bradford, N. K., & Yates, P. (2019). Discussing death: Making end of life implicit or explicit in paediatric palliative care consultations. Patient Education and Counseling, 102(2), 198–206.
Farabelli, J. P., Kimberly, S. M., Altilio, T., Otis-Green, S., Dale, H., Dombrowski, D., Kieffer, J. R., Leff, V., Schott, J. L., Strouth, A., & Jones, C. A. (2020). Top ten tips palliative care clinicians should know about psychosocial and family support. Journal of Palliative Medicine, 23(2), 280–286.
Gonella, S., Campagna, S., Basso, I., De Marinis, M. G., & Di Giulio, P. (2019). Mechanisms by which end-of-life communication influences palliative-oriented care in nursing homes: A scoping review. Patient Education and Counseling, 102(12), 2134–2144.
Habeck-Fardy, A. (2021). Passing on death: An audit of the terminology utilized in discharge summaries for deceased patients. Death Studies, 45(6), 413–419.
Kremling, A., Bausewein, C., Klein, C., Schildmann, E., Ostgathe, C., Ziegler, K., & Schildmann, J. (2022). Intentional sedation as a means to ease suffering: A systematically constructed terminology for sedation in palliative care. Journal of Palliative Medicine, 25(5), 793–796.
Kuosmanen, L., Hupli, M., Ahtiluoto, S., & Haavisto, E. (2021). Patient participation in shared decision-making in palliative care – an integrative review. Journal of Clinical Nursing, 30(23–24), 3415–3428.
Library help. (n.d.). USC Australia.
Olsson, M. M., Windsor, C., Chambers, S., & Green, T. L. (2021). A scoping review of end-of-life communication in international palliative care guidelines for acute care settings. Journal of Pain and Symptom Management, 62(2), 425-437.e2.
Omori, M., Jayasuriya, J., Scherer, S., Dow, B., Vaughan, M., & Savvas, S. (2022). The language of dying: Communication about end-of-life in residential aged care. Death Studies, 46(3), 684–694.
Palliative care Australia. (n.d.). PCA.
Registered nurse standards for practice. (n.d.). Nursing and Midwivery Board AU.
Reigada, C., Arantzamendi, M., & Centeno, C. (2020). Palliative care in its own discourse: a focused ethnography of professional messaging in palliative care. BMC Palliative Care, 19(1), 88.
Ryan, S., Wong, J., Chow, R., & Zimmermann, C. (2020). Evolving definitions of palliative care: Upstream migration or confusion? Current Treatment Options in Oncology, 21(3), 20.
Schuelke, T., Crawford, C., Kentor, R., Eppelheimer, H., Chipriano, C., Springmeyer, K., Shukraft, A., & Hill, M. (2021). Current grief support in Pediatric Palliative Care. Children (Basel, Switzerland), 8(4), 278.
Tang, M. L., Goh, H. S., Zhang, H., & Lee, C. N. (2021). An exploratory study on death anxiety and its impact on community palliative nurses in Singapore. Journal of Hospice and Palliative Nursing: JHPN: The Official Journal of the Hospice and Palliative Nurses Association, 23(5), 469–477.
USC Library. (n.d.). Guides: Find information – Journals.