Introduction
Pressure ulcers are disruptions to the skin tissue caused by prolonged pressure on a particular area. However, the ulcers can be prevented through interventions that significantly lower the risks of developing bed sores. This paper aims to determine whether an effective repositioning schedule implemented in a healthcare setting can reduce the risk of bed sores and the subsequent medical problems associated with the condition in geriatric patients.
Significance of Practice Problem
While pressure ulcers are preventable, current circumstances portray the condition as a significant challenge to the well-being of the general population and the costs and resources hospitals allocate to mitigate the issue. According to researchers, 60,000 people die from complications related to bed sores in the US yearly (Khojastehfar et al., 2020). Moreover, pressure ulcers are associated with high medical costs and a low quality of life.
Another aspect that highlights the topic’s significance is that patients with skin tissue disruptions experience longer hospital stays (Ojeda Méndez et al., 2020). As a result, the practice problem has been identified as significant, and interventions are necessary to address the aforementioned limitations.
PICOT
The following PICOT question will be addressed: Are geriatric patients (P) who are put on a 3-hour repositioning schedule (I) less prone to developing pressure ulcers (O) compared to patients who are not put on a turning schedule (C) during a 6-week intervention? Geriatric patients with mobility issues will be the demographic examined during the research. The intention is to determine whether a nursing intervention consisting of implementing a repositioning schedule every 3 hours addresses the risk of developing bed sores compared to the lack of a schedule.
Search Strategy
The keywords applied to search relevant studies on the topic are “bed sores prevention”, “pressure ulcer repositioning schedule,” and “pressure ulcer intervention”. The platform used for the research is Google Scholar, and articles published within the last five years have been selected. As a result, five primary studies were selected.
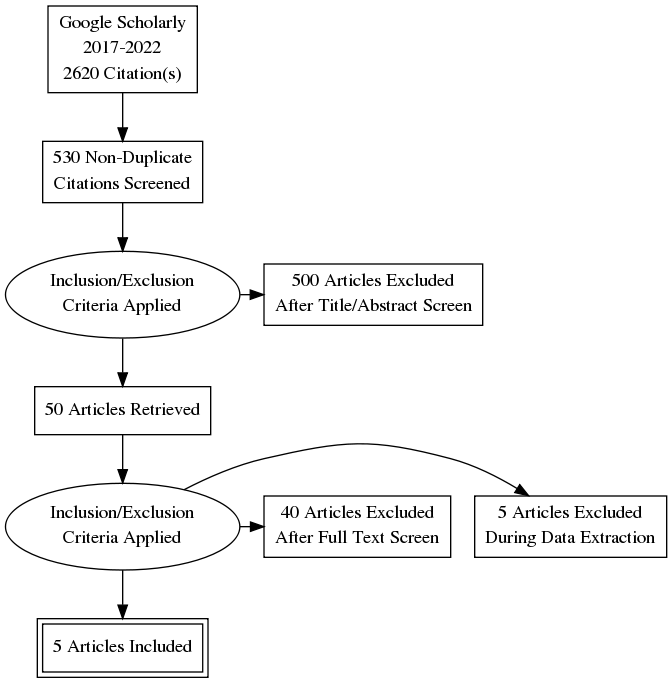
Research Overview
The primary research selected for the current analysis presents various findings that correlate with the research question. Lavallée et al. (2018) conducted a study showing that nurses’ lack of knowledge regarding the frequency of repositioning patients is a factor that maximizes the occurrence of bed sores. Alhammadi and Ogale (2020) attested that teaching healthcare providers to implement preventive measures for bed sores, including frequent patient turning, minimizes the risk of pressure ulcers. Hessels et al. (2019) concluded that pressure ulcers occur partly due to nurses’ failure to adhere to a 2-hour turning schedule implemented in healthcare settings.
Moreover, Ebi et al. (2019) found a correlation between bed sores and the lack of adherence to a schedule in which pressure on the skin tissue is frequently assessed. Bereded et al. (2018) conducted a study that demonstrated that changing the patient’s position significantly reduces the occurrence of bed sores. The primary research on the topic suggested that repositioning could be addressed through a turning schedule, which aligns with the PICOT question applied to the current research.
Conclusion
Pressure ulcer prevention is complex and requires frequent contact with the patient and attendance. However, since the condition is preventable and correlates with multiple risks, it is essential to minimize potential limitations. The proposed intervention, namely, implementing a schedule of repositioning geriatric patients with mobility issues once every three hours, can significantly improve the rate of bed sore occurrence. This will subsequently address multiple problems, including the high cost of treatment, a lowered quality of life, infections, and discomfort.
References
Alhammadi, H. M. A., & Ogale, R. J. (2020). Effectiveness of home caregivers teaching program on prevention of decubitus ulcer in bed ridden elderly patients. International Journal of Nursing December 2020, 7(2), 69–79.
Bereded, D. T., Salih, M. H., & Abebe, A. E. (2018). Prevalence and risk factors of pressure ulcer in hospitalized adult patients; a single-center study from Ethiopia. BMC Research Notes, 11(1).
Ebi, W. E., Hirko, G. F., & Mijena, D. A. (2019). Nurses’ knowledge to pressure ulcer prevention in public hospitals in Wollega: A cross-sectional study design. BMC Nursing, 18(1).
Hessels, A. J., Paliwal, M., Weaver, S. H., Siddiqui, D., & Wurmser, T. A. (2019). Impact of patient safety culture on missed nursing care and adverse patient events. Journal of Nursing Care Quality, 34(4), 287–294.
Khojastehfar, S., Najafi Ghezeljeh, T., & Haghani, S. (2020). Factors related to knowledge, attitude, and practice of nurses in intensive care unit in the area of pressure ulcer prevention: A multicenter study. Journal of Tissue Viability, 29(2), 76–81.
Lavallée, J. F., Gray, T. A., Dumville, J., & Cullum, N. (2018). Barriers and facilitators to preventing pressure ulcers in nursing home residents: A qualitative analysis informed by the theoretical domains framework. International Journal of Nursing Studies, 82, 79–89.
Ojeda Méndez, C. A., Palomino Pacichana, D. S., BejaranoBarragán, L., Ocampo-Chaparro, J. M., & Reyes-Ortiz, C. A. (2020). Factors associated with prolonged hospital stay in an acute geriatric unit. Acta Médica Colombiana, 46(1).