Introduction
The growing problems in emergency department (ED) boarding are endemic due to increased acute care demand and stagnant hospital capacity. In this case, an ED plays a significant role as an access point for comprehensive patient diagnostics and treatment, which may be lacking in a fragmented healthcare system. When EDs are overcrowded and patients experience long wait times, they often leave before receiving a clinical evaluation, a phenomenon known as left without being seen (LWBS). This leads to deferred or delayed care for severe medical conditions and may increase the risk of adverse events.
Positive predictors of patients leaving without clinical evaluation include low acuity, male gender, and high annual visit volume (Sheraton et al., 2020). Conversely, factors such as private insurance or Medicare, older age, weekend visits, and higher income suggest a lower probability of a patient leaving without being seen. The significance of this project lies in its potential to improve ED throughput, reduce the percentage of LWBS, and improve patient health outcomes.
Problem Diagnosis
The ED has experienced an increase in long wait times and the number of LWBS patients. This is regarded as a serious issue for patients and healthcare facilities. In this scenario, patients are compelled to delay or defer their clinical diagnosis and treatment, which can contribute to adverse outcomes. Further investigation into the factors contributing to long wait times and LWBS can help identify the root cause of the problem. The primary sources of this issue may be varied and are presented in the flowchart below.
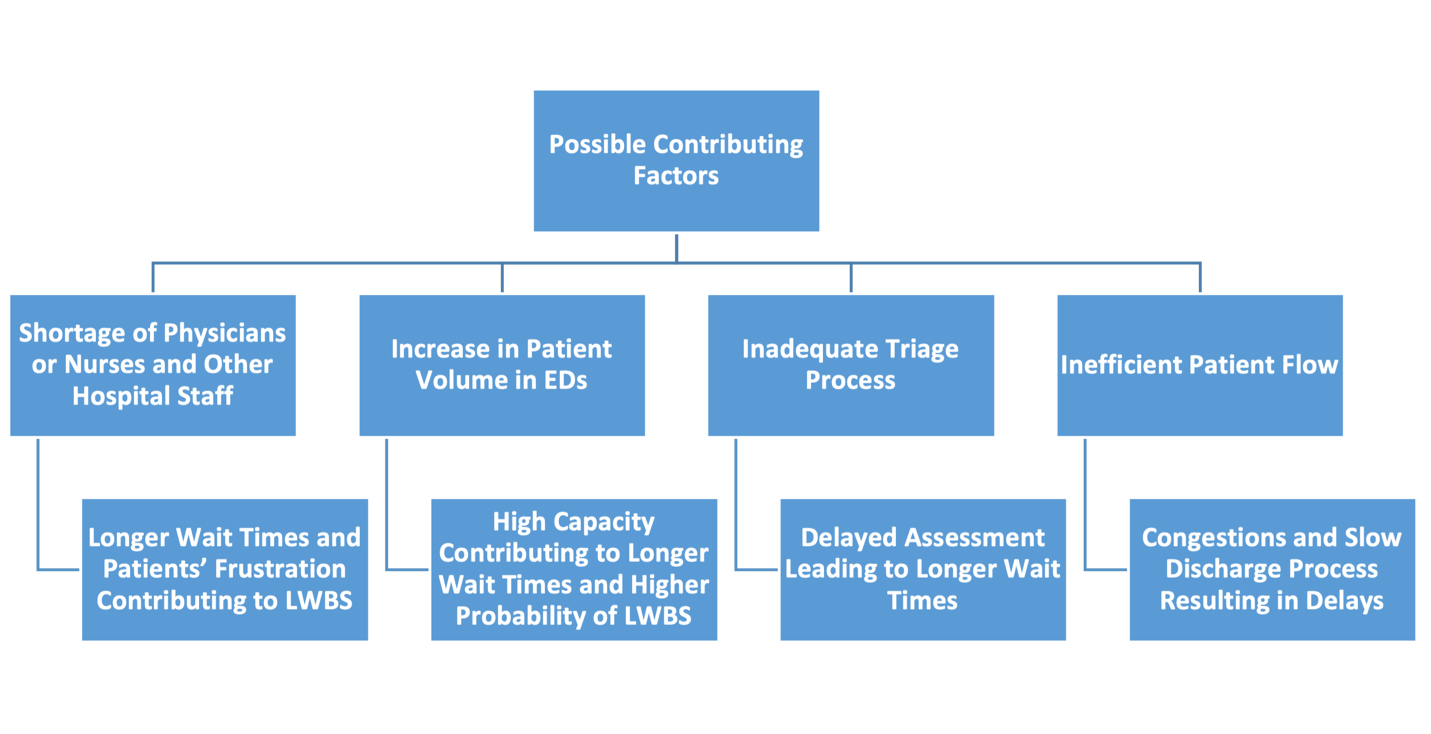
The diagram illustrates the potential contributing factors that can lead to longer wait times and an increase in LWBS cases in the ED, including a shortage of healthcare practitioners and support staff at the hospital. Additionally, high traffic at the facility can overwhelm the department’s capacity to attend to all patients, contributing to the current problem. Similarly, clients at the facility may not be triaged appropriately, and their condition may not be assessed promptly. Lastly, inefficiencies in patient flow can result in slow discharge times, congestion, and delayed patient care.
Statement of the Problem
Waiting times for emergency and elective procedures have been shown to predict satisfaction among service users. In emergency cases, delays in receiving appropriate treatment may also cause an increase in LWBS rates and even lead to serious health problems and avoidable mortality. A World Health Organization (WHO) report shows that hospital patients’ wait times worldwide range from 30 minutes to 2 hours (2018). This issue adversely affects patients’ readiness to return to the hospital for treatment and, consequently, decreases the utilization of health services (Biya et al., 2022).
Longer waiting time is a primary factor contributing to increased LWBS patients and causing dissatisfaction among service users. In addition, the hospital’s bottom line is affected indirectly through reimbursement penalties resulting from lower satisfaction scores and directly through reduced revenues from missed care delivery opportunities (Sheraton et al., 2020). This problem also harms employee morale as healthcare workers feel frustrated and overworked when patients experience lengthy delays in receiving care (McCormick et al., 2019). Therefore, this can lead to lower job satisfaction and increased burnout, thereby affecting the quality of care provided to patients.
A Quality Improvement Model
Six Sigma is the quality improvement (QI) method selected to reduce long wait times and associated LWBS rates. This data-driven approach utilizes statistics to measure and reduce variability, thereby eliminating inconsistency. The tool is represented by DMAIC, which stands for Define, Measure, Analyze, Improve, and Control, or the five phases of the model (Chen et al., 2020). In this case, the definition entails identifying the problem and setting the project’s goals.
The second step entails collecting data to measure ED wait times, LWBS rates, patient satisfaction, and staff morale. The analysis is conducted in the third phase to identify the root causes of the long ED wait times and develop potential solutions. In the fourth level, the solutions are implemented to improve ED throughput. The final stage involves a monitoring process to ensure the improvements are sustained and that the variations that cause long wait times and high LWBS rates are reduced.
By using the DMAIC framework, the administrative processes contributing to long wait times and high LWBS rates can be evaluated to improve overall hospital service. The tool can map out and assess whether the lack of staff engagement, inadequate staffing levels, or the triage process are the main contributors to the long wait times. Additionally, process improvement can be performed to determine whether the duration required to complete specific procedures, such as obtaining laboratory results, exacerbates the problem.
When the Six Sigma process improvement model is applied, the investigative team can determine whether ineffective interdepartmental communication or inadequate staffing complicates the ED admission process. Suppose patients are forced to wait for long hours before they are seen or attended to by physicians. In this case, the hospital boarding process will be redesigned into a single-piece flow, incorporating a timestamp for each step to resolve existing variability. This will enable all stakeholders to track the status of the admission process and alert relevant personnel when delays exceed a predetermined threshold, thereby helping to reduce the number of LWBS patients.
Best Practices That Can Be Implemented
Standardizing the triage process can ensure patients do not wait long for medical assessment and treatment. Multiple patients may present within short time frames, and others may have health problems that have outcomes directly related to the timeliness of treatment, such as myocardial infarction and stroke. In this context, patient safety in the ED is linked to the triage system.
Applying a standardized triage process will ensure that the facility outlines the steps for prioritizing patients based on their symptoms and conditions. The strategy can be supported with triage tools, such as the Emergency Severity Index (ESI), to help nurses quickly and accurately assess patients’ acuity levels and prioritize care (Burgess et al., 2019). In addition, ongoing training can ensure that nurses maintain their skills and stay up to date on new practices. Such measures can guarantee consistency in care delivery and improve healthcare outcomes and patient satisfaction. The triage process may incorporate guidelines for clinical assessment, including vital signs, symptoms, medical records, and protocols for identifying and responding to emergency cases. Enforcing acceptable triage practices is essential in reducing variation in care service delivery, minimizing errors, and improving patient safety.
Establishing a centralized communication system can also increase stakeholder coordination and regular huddles to discuss patient care plans. Similarly, it is essential to communicate with patients clearly and empathetically, ensuring they understand their conditions, receive information about wait times and what to expect during their care, and have their concerns addressed (Burgess et al., 2019). These practices can foster trust between patients and healthcare providers, ensuring that service users are informed and feel involved in their care. This can reduce patient anxiety and significantly improve patient satisfaction.
The hospital can also streamline registration by reducing non-value-added activities, such as documentation and redundant data entry. Similarly, it is essential to increase staffing during peak hours to meet demand by establishing a rotation among team members to share the workload. This can reduce burnout and ensure continuous service delivery even when staff members are on vacation.
How to Measure and Analyze the Results
The result will be tracked and monitored through metrics such as ED wait time, LWBS rate, patient satisfaction scores, and employee morale scores. In this regard, the ED wait time can be measured by analyzing the impact of the hospital’s efforts to reduce the number of LWBS patients against the established targets and determining if the process improvement has achieved the desired impact. If the LWBS rate was 10% before and 5% after the process, this would demonstrate increased effectiveness in reducing the number of patients who leave the ED without receiving care (see Figure 2).
How to Evaluate the Effectiveness of Improvement
The effectiveness of the improvement may be evaluated by comparing the pre- and post-implementation data. The former may include collecting data across all four areas identified by establishing a baseline study. Primary sources of information on LWBS rates before the project’s start may include medical records and patient satisfaction surveys. Suppose the hospital initiates Six Sigma to reduce long wait times in the ED and finds that, before the initiative, the average ED wait time is 2 hours. After the improvement process, the average duration decreases to 1 hour and 30 minutes. This would indicate that the strategy is successful. In this case, statistical charts may be used to identify trends or changes in wait times (see Figure 3).
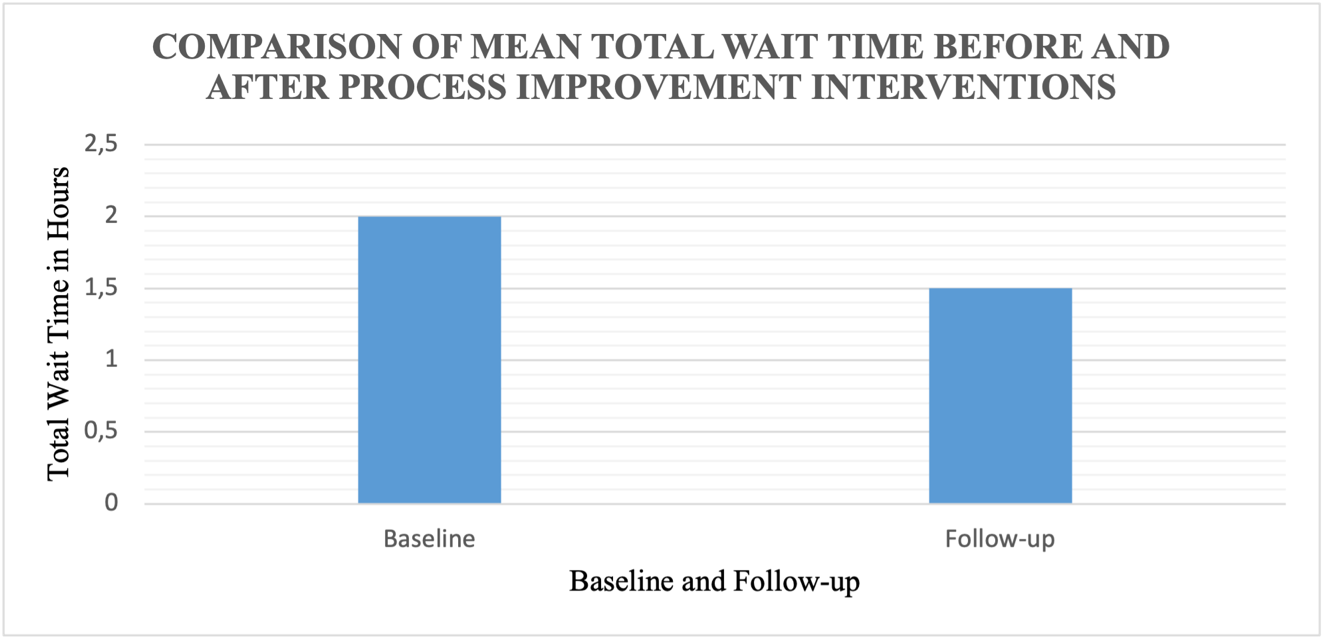
The graph illustrates the mean total wait time before and after implementing the DMAIC framework. One bar represents the mean wait time at baseline, while the other represents the mean wait time after the improvement intervention was initiated. Additionally, patient satisfaction and employee morale levels can be evaluated using a Likert scale before and after the process, where patients can provide feedback through a score of 1 to 5. Establishing a baseline for these two metrics is crucial before the project starts. This can be in the form of a survey, interviews, questionnaires, or other methods of data collection, and repeating the activities a few months after initiating the process to capture changes in the service users’ responses and feelings regarding waiting times.
Conclusion
Longer ED wait times are problematic for the hospital and service users. This issue can delay or defer treatment, leading to serious health complications and preventable deaths. Additionally, it can result in high LWBS rates and adversely affect the patient’s readiness to seek appropriate care, reducing health service utilization.
LWBS patients are often dissatisfied, which may directly impact the hospital’s profitability due to increased missed opportunities in delivering care. The problem can also damage employee morale because they may feel frustrated and overworked. However, implementing the Six Sigma methodology can help the service provider to identify the root cause of the problem and develop solutions to improve the process.
References
Biya, M., Gezahagn, M., Birhanu, B., Yitbarek, K., Getachew, N., & Beyene, W. (2022). Waiting time and its associated factors in patients presenting to outpatient departments at public hospitals of Jimma Zone, southwest Ethiopia. BMC Health Services Research, 22(1), 107.
Burgess, L., Kynoch, K., & Hines, S. (2019). Implementing best practice into the emergency department triage process. International Journal of Evidence-Based Healthcare, 17(1), 27–35.
Chen, Y., VanderLaan, P. A., & Heher, Y. K. (2020). Using the model for improvement and plan‐do‐study‐act to effect smart change and advance quality. Cancer Cytopathology, 129(1), 9–14.
McCormick, C. L., Hervey, W. M., Monahan, C., Gibson, C. A., Winn, J. L., & Catalano, G. (2019). Improved patient outcomes and reduced wait times: Transforming a VA outpatient substance use disorder program. Federal Practitioner, 36(7), 332–338.
Sheraton, M., Gooch, C., & Kashyap, R. (2020). Patients leaving without being seen from the emergency department: A prediction model using machine learning on a nationwide database. Journal of the American College of Emergency Physicians Open, 1(6), 1684–1690.
World Health Organization. (2018). Delivering quality health services: A global imperative for universal health coverage.