Introduction
- Importance of skin-to-skin contact.
- Supported by international organizations.
- Contributes to the infant’s thermoregulation.
- Reduces the risk of jaundice.
- Reduces stress at birth.
- Favors successful breastfeeding.
The issue of early skin-to skin contact between a mother and an infant is a popular topic for discussion in contemporary medical science. According to the World Health Organization and the United Nations International Children’s Emergency Fund, skin-to-skin contact (SSC) between mothers and newborns should be established as soon as possible after the child is born (Stevens, Schmied, Burns, & Dahlen, 2014). SSC can be defined as “placing a naked infant onto the bare chest of the mother” (Stevens et al., 2014, p. 456). Application of this technique within one hour after birth is considered to have benefits for a baby including maintenance of the infant’s thermoregulation and stimulation of breastfeeding (Stevens et al., 2014).
Description of the Ace Star Change Model
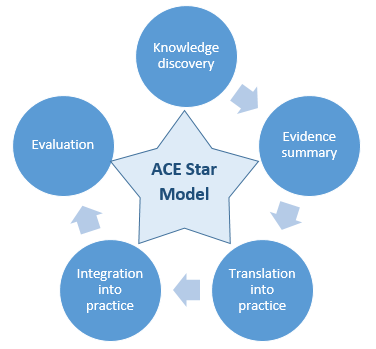
One of the models for change that can be applied in evidence-based practice is the ACE Star Model, also known as the model of knowledge transformation, developed by Kathleen Stevens (White & Dudley-Brown, 2012). It comprises all aspects necessary for the successful change implementation. The model includes five stages: knowledge discovery, evidence summary, translation into practice, integration into practice, and evaluation (White & Dudley-Brown, 2012).
During knowledge discovery stage, the existing information regarding the change problem is investigated. During evidence summary stage, the evidence that proofs of the problem significance are discovered. Translation onto practice stage presupposes the definition of ways that help to apply evidence to practice while integration into practice includes practical steps of change implementation. Finally, the evaluation of the activities is provided to assess its efficiency and make alterations in case of necessity.
Practice Issue
- Infants placed in radiant warmer after delivery.
- lack of education on the benefits of SSC.
- necessity of discovering the effect of early SSC.
The practice issue identified for this change project is that babies are frequently placed in a radiant warmer after delivery and then assessed, weighed, foot-printed and medicated, then wrapped in a blanket and given to the mother without skin-to-skin contact. This happens due to a lack of knowledge concerning the benefits of SSC. The significant question for evidence-based practice to answer during the change project implementation is: What is the effect of skin-to-skin contact within the first 10 minutes to one hour of birth? On a broader range in the field of health care, the issue of early SSC can be meaningful in problems involving nutrition and the related problem of obesity.
Scope of the Problem
- Breastfeeding 56.6% more successful in case of early SSC (Aghdas, Talat, & Sepideh, 2014).
- Early SSC to achieve thermal control (Nimbalkar et al. (2014).
- Reduction of hypothermia incidence (Nimbalkar et al., 2014).
It is a wide-spread practice applied in about a half of all deliveries to place healthy newborns in radiant warmers after delivery instead of immediately placing them on their mother’s chest, promoting skin-to-skin contact for thermoregulation and stimulation of breastfeeding. Thus, early separation is a problem, because lack of SSC can negatively influence thermoregulation and the future duration of breastfeeding. To contribute to the solution of the early newborn separation problem and enhance the SSC practice, it is necessary to implement education interventions on the benefits of SSC in promoting breastfeeding.
Team/Stakeholders
- team leader.
- gynecologist.
- obstetrician-gynecologist.
- pediatrician.
- charge nurse.
- a nurse.
- visiting nurse.
Every stakeholder has certain responsibilities in a team. The leader of the team will guide the project. A gynecologist will take care of the pregnant women before and after delivery. An obstetrician-gynecologist will be in charge of the delivery process. A pediatrician will provide assessment of the newborn babies and give recommendations on care. A charge nurse will control and organize care for women and their newborns, and a nurse will provide care for women and infants with a focus on successful breastfeeding. A visiting nurse will help to assess the organization of breastfeeding and the babies’ condition after they are discharged. Every member of the team will contribute to a valid assessment of the impact of early SSC on successful breastfeeding.
Evidence to Support Need for Change
- SSC after normal delivery.
- SSC after caesarean section.
- SSC contributes to thermoregulation.
Moore, Bergman, Anderson, & Medley (2016) conducted a systematic review of impacts that early SSC has on mothers and their healthy newborn infants. Stevens et al. (2014) reviewed the literature on the implementation of immediate or early SSC after caesarean section and concluded that SSC can be implemented in case of caesarean surgery. Beiranvand et al. (2014) also provided evidence of the effects of SSC after caesarean delivery on temperature and success of breastfeeding.
Research by Aghdas et al. (2014) contributed to evidence supporting the influence of immediate and continuous mother–infant SSC on the self-efficiency of breastfeeding by primiparous women. Further evidence supporting the significance of early SSC after normal delivery for incidence of hypothermia in neonates is suggested by Nimbalkar et al. (2014).
- SSC favorable for breastfeeding initiation (Beiranvand et al., 2014).
- Increase in breastfeeding duration (Moore et al., 2016).
- SSC reduces newborn stress (Stevens et al., 2014).
- Contribution to infant physiological stability.
- Maternal-infant bonding (Moore et al., 2016).
It was discovered that that early SSC positively influences breastfeeding initiation and contributes to the increase in breastfeeding duration. Early SSC is also useful for infant physiological stability within the first hours after birth. Apart from physiological effects, psychological impacts of SSC are also present. For example, Stevens et al. (2014) found proofs that SSC reduces newborn stress and Moor et al. (2016) believe that SSC positively influences the development of connection between a mother and a newborn. Thus, the existing evidence provided by research support the importance of early or immediate SSC between a mother and an infant.
Recommendations for Change
- SSC recommended immediately after birth for healthy babies at term.
- SSC necessary for baby’s temperature regulation.
- Routine procedures without interrupting SSC.
- Facilitation of continuous SSC through the first breastfeeding.
- Involvement of other caregivers in case the mother’s condition does not allow SSC.
- Mothers’ education about the health benefits of breastfeeding.
- Encouragement of rooming-in.
- Support of feeding on cue demand.
- Exclusive breastfeeding for the first six months.
After the discovery of evidence, some recommendations for the implementation of SSC can be provided. First of all, it is recommended to apply SSC for mothers and infants immediately after birth both in the case of vaginal and caesarean delivery of healthy babies. Even in case of mother’s bad condition, other caregivers can be involved. Still, the primary recommendation is the efficient mother’s education regarding the necessity of early SSC and its role in baby’s health maintenance and successful breastfeeding.
Action Plan

Action plan includes five major steps. It includes the presentation of project objectives to the stakeholders. Educational part of the project comprises two steps, nursing training and improvement of practical skills appropriate for the organization of early SSC and further successful breastfeeding, and patient education, including informing women of the importance of immediate SSC for breastfeeding and an infant’s wellbeing and teaching them foundations of baby care and breastfeeding.
They are followed by the implementation itself after which the assessment of the project efficiency will be conducted. The evaluation plan will include a survey-based research of breastfeeding organizational success and quantitative research on infants’ outcomes based on medical records. The evaluation of breastfeeding success can be executed at least after six months after birth.
Timeline for the Plan
- Preparation and presentation: 1 week.
- Nursing education: 2-3 weeks.
- Patient education: 1 week.
- Implementation: 4 weeks.
- Evaluation: 1 week.
- Evaluation of breastfeeding success: 6 months after project implementation.
The timeline for plan implementation is two months. During this period, the project will be prepared and presented. From two to three weeks of nursing education concerning the organization of early SSC including both theoretical knowledge and practical skills will be followed by patient education that will last for a week. The project will be implemented during four weeks. The evaluation will be provided within a week after the project implementation. Finally, the success of breastfeeding among the participants of the project will be assessed after six months since 6-month period is considered successful for breastfeeding.
The Nurse’s Role and Responsibility in the Pilot Program
- Control and organization of care.
- Provision of SSC after the delivery.
- Facilitation of SSC in the operating room.
- Provision of patient education on the importance of SSC.
- Focus on successful breastfeeding.
- Assessment of breastfeeding organization.
A professional nurse can contribute to the issues related to SSC both in hospital settings and after the discharge. First of all, nurse’s role is in facilitating early SSC of a mother and a newborn child both in case of normal delivery and caesarean section. One of the key responsibilities of a nurse is the organization of patient education to provide future mothers with information concerning the significance of SSC and its impact on breastfeeding success and general baby’s health. A visiting nurse is responsible for evaluation of breastfeeding organization at home after mothers and infants are discharged from the hospital.
Procedure
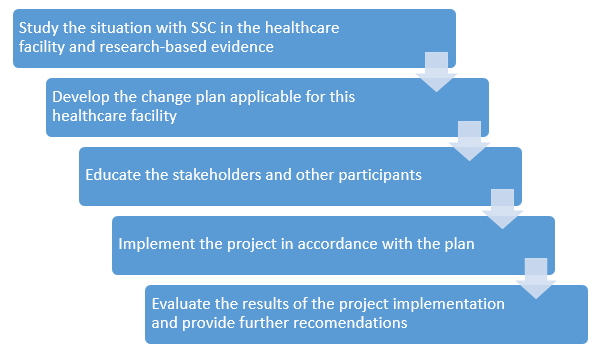
The procedure should begin with the examination of researches related to the problem and how this problem is treated within the healthcare facility that will be the basis for the change project. After that, a careful planning is necessary to include all important aspects. Education part is significant because it prepares all participants for the implementation of the project. The implementation itself is followed by the evaluation of the results which includes further recommendations that will help to preserve the positive change.
Resources Available to the Staff
- WHO recommendations.
- Nursing literature.
- Researchers on the problem of SSC.
- Materials of conferences about breastfeeding.
- Experience of healthcare professionals.
Staff of healthcare facilities should be guided by the recommendations of WHO. For example, Guidelines on Maternal, Newborn, Child and Adolescent Health approved by the WHO Guidelines Review Committee can be a useful resource for planning interventions concerning promotion and protection of newborn health including the issue of early SSC. Other resources for the staff involved in the process of care include nursing literature for theoretical knowledge and research materials to learn about the practical aspects of SSC problem.
Also, materials of conferences and workshops about SSC and breastfeeding can contribute to sharing knowledge on the problem. Finally, experience exchange with other healthcare professionals can contribute to better understanding of practical issues of SSC and its effects.
Disseminating Findings
- Internal;
- Among the colleagues.
- External;
- Outside the organization.
The results of the research preceding the project and the findings obtained during the implementation of the change project can be disseminated to make them available to other interested people. They can be disseminated both internally, among colleagues within the healthcare facility, and externally, outside the organization. For internal distribution of project results, the presentation of the project findings can be used. Presentations can be organized for the interested staff members to inform them on the findings and stimulate their further application. Distributing the findings externally can involve publishing in specialized journals and presenting at conferences or workshops dedicated to the issue of breastfeeding and related problems.
Implications for Further Change Process
- Patient education programs.
- Nursing education plans.
- Inclusion of project ideas on regular basis.
The findings of the project can be applied for further change process. First of all, they can be included as a component in nursing and patient education on a regular basis. To ensure the permanent character of the project’s implementation, both nursing and patient education interventions should be provided on a regular basis to make them aware of the significance of early SSC. Constant education interventions will contribute to a more successful application of SSC and, as a result, better patient outcomes among women and newborn children.
Summary
- Contribution of the change model to the solution of SSC problem.
- Negative character of early separation.
- Positive impacts of early SSC.
- Significance for baby’s health.
- Positive contribution to breastfeeding organization.
- Implications for nursing practice and education.
Generally speaking, the suggested change model contributes to a solution to the identified problem of implementing SSC immediately after birth. One of the major aspects of the problem is the negative impact of an early separation of a mother and her infant compared to immediate SSC. The change model provides the discovery of knowledge, summary of evidence proving the importance of early or immediate SSC and its positive influence, ideas for translation into practice, a plan for integration into practice, and ideas for evaluation of the project.
References
Aghdas, K., Talat, K., & Sepideh, B. (2014). Effect of immediate and continuous mother–infant skin-to-skin contact on breastfeeding self-efficacy of primiparous women: A randomised control trial. Women and Birth, 27(1), 37-40. Web.
Beiranvand, S., Valizadeh, F., Hosseinabadi, R., & Pournia, Y. (2014). The effects of skin-to-skin contact on temperature and breastfeeding successfulness in full-term newborns after cesarean delivery. International Journal of Pediatrics, 2014. Web.
Moore, E., Bergman, N., Anderson, G., & Medley, N. (2016). Early skin-to-skin contact for mothers and their healthy newborn infants. Cochrane Database of Systematic Reviews. Web.
Nimbalkar, S., Patel, V., Patel, D., Nimbalkar, A., Sethi, A., & Phatak, A. (2014). Effect of early skin-to-skin contact following normal delivery on incidence of hypothermia in neonates more than 1800 g: randomized control trial. Journal of Perinatology, 34(5), 364-368. Web.
Stevens, J., Schmied, V., Burns, E., & Dahlen, H. (2014). Immediate or early skin-to-skin contact after a Caesarean section: a review of the literature. Maternal & Child Nutrition, 10(4), 456-473. Web.
White, K.M., & Dudley-Brown, S. (2012). Translation of evidence into nursing and health care practice. New York, NY: Springer Publishing Company.