Brief Background/Significance
Cardiovascular disease (CVD) presents as one of the leading causes of death globally and is a major driver of health loss, disability, and excess costs on the healthcare system. From 1990 to 2019, the cases of CVD increased from 271 million to 523 million, while the deaths increased from 12.1 million to 18.6 million (Roth et al., 2020). In 2021, inadequate physical activity was linked to 0.397 million CVD deaths and 0.686 million overall deaths globally. (Vaduganathan et al., 2022).
Low physical activity is also linked to other risk factors associated with CVD, such as a high body mass index, high plasma glucose levels, high blood pressure, and high LDL cholesterol levels. While the condition is preventable or improvable through various modifiable factors, such as increasing physical activity, the growing incidence of CVD presents a significant issue for the public health system. Although there are many ways people can reduce their CVD risk, physical activity is an essential component that can substantially lower the risk. The problem is that many programs are not delivered in Spanish, which presents a barrier to implementing a physical activity program effectively.
Due to immigration status, the Hispanic and Latino populations of the US have a higher risk of cardiovascular diseases. Undocumented and documented Hispanic immigrants are less likely to obtain treatment for high cholesterol, hypertension, and diabetes when compared to naturalized citizens. Studies have revealed significant undertreatment of Hispanics/Latinos without US citizenship, particularly among undocumented immigrants, despite the crucial role that cardiovascular drugs play in CVD prevention (Guadamuz et al., 2020).
The majority of immigrants in the United States reach middle and late adulthood, a time when the risk of CVD and associated diseases dramatically rises. Recent research reveals that immigrants had higher rates of CVD mortality among Hispanics/Latinos than those who were born in the country, highlighting the significance of maintaining proper care for this population (Guadamuz et al., 2020). Hence, both legal and illegal immigrants have poorer access to health care, such as insurance or a regular doctor, than naturalized citizens have.
Moreover, Hispanics have an increased risk of cardiovascular diseases. Because they are more likely to have high blood pressure, obesity, diabetes mellitus, and ischemic strokes than non-Hispanic whites, Hispanics have increased cardiovascular disease risks (Shaw et al., 2018). In comparison to 66% of non-Hispanic whites, 72% of Hispanics who had a stroke also had high blood pressure.
Obesity affects 75% of males and 72% of women in Mexican Americans who are 20 years of age and older. Diabetes mellitus affects about 30% of adult Hispanics, and nearly a third of Mexican American people 20 years of age and older have CVD (Shaw et al., 2018). Hence, Hispanics have a higher rate of CVD when compared to the non-Hispanic US population.
Language barriers are a significant contributing factor to the higher rates of CVD observed in the Hispanic population. The Brookings Institution notes that due to a lack of insurance, language difficulties, and cultural differences, Hispanics often face poor health outcomes and restricted access to healthcare (Shiro et al., 2022). Moreover, the healthcare profession contains too few Hispanic representatives to provide the availability and quality of care necessary (Shaw et al., 2018). Patient education for the Hispanic community is commonly cited as being hampered by the lack of awareness of Hispanic culture and language. Hence, language differences are one of the reasons for the high CVD rates among the Hispanic population of the US.
Another attribute of the CVD risk among Hispanics is access to healthcare among this demographic. The availability and accessibility of health insurance are key factors in determining access to healthcare services in the United States, since a sizable fraction of the Hispanic population lacks health insurance, and a large portion of them live as undocumented immigrants (Ortega et al., 2020). Hence, the Hispanic population in the US faces higher CVD rates partially because a large portion of them live as undocumented immigrants and thus lack health insurance.
Additionally, a high prevalence of CVD among Hispanics can be attributed to the lack of physical activity among them. According to reports, Americans of Hispanic heritage are the least physically active. The most recent Behavioral Risk Factor Surveillance System data reveal that Hispanic men and women continue to have very high rates of obesity, hypertension, diabetes, and inactivity. Compared to 66% of non-Hispanic white individuals, just 37% of all Hispanic adults had their cholesterol levels examined (Khan et al., 2022).
Additionally, compared to NHW patients, Mexican Americans exhibited a greater age-adjusted incidence of hemorrhagic stroke. The existing disparities in CVD mortality, especially the difference in stroke mortality between non-Hispanic white and Hispanic people, are explained by suboptimal CVD risk factor profiles (Khan et al., 2022). Hence, lack of physical activity is a significant factor in the high CVD rate among Hispanics.
Problem Statement
The population of adults 45 to 55 years old whose primary language is Spanish experiences high risks of CVD compared with other ethnic groups in the US, according to Gomez et al. (2022). The rates of both traditional and non-traditional risks associated with CVD are higher among the Hispanic population (Gomez et al., 2022). Although there are many educational materials available in Spanish, not having an in-person educational session in conjunction with a weekly Spanish-language Zoom session may limit the number of people who engage in physical activity (Javed et al., 2022).
Furthermore, language barriers and implicit bias can lead to miscommunication with health professionals, resulting in misdiagnoses. Evidence-based programs, such as the National Institutes of Health (NIH) Physical Wellness Checklist (PWC) Program, provide tools to enhance physical activity (Figure 1). Providing a Spanish class as part of the PWC program is likely to increase physical activity in adults whose primary language is Spanish.

Organizational Needs
The Project will use the Spanish version of the PWC. The program’s lack of consideration for cultural differences and language barriers can negatively impact physical activity and the quality of health knowledge acquired by participants whose primary language is Spanish. Thus, quality improvement in the form of physical activity exercise recommendations may increase the program’s efficiency in reducing the risks of CVD in the adult population.
Addressing the language barriers will likely improve the population’s awareness of CVD risks and contribute to a more active lifestyle. The Organization sees a large number of patients daily, resulting in inadequate time to educate them on the benefits of exercising. Implementing this program in their primary care office will likely improve patient outcomes.
Purpose & Practice-Based Question
The objective of this Quality Improvement (QI) project is the implementation of the Physical Wellness program within a primary care setting for adults aged 45 to 55 who are at risk for CVD. The project aims to evaluate the program’s effect on participant knowledge, physical activity levels, and willingness to maintain physical activity after the program concludes.
The practice-based question is: What is the impact of a Physical Wellness Program presented in Spanish on the knowledge, physical activity, and post-project exercise commitment of Spanish-speaking adults at risk for CVD?
Impact of Project on Public Health and Health Disparities
The population that speaks Spanish as its first language presents a minority group that often faces barriers to access to health services. Language barriers, cultural differences, and limited financial opportunities contribute to increased risks of CVD in the population and low efficiency of existing preventive measures (Javed et al., 2022).
Providing the necessary information about health issues in an accessible and comprehensible form can increase the population’s awareness about CVD prevention and reduce health disparities in the unequal distribution of health information. The Project will also define ways to improve motivation to participate in physical activity and adopt a healthy lifestyle among adults at risk of CVD who speak Spanish as their primary language, thereby reducing their risk of developing other lifestyle-related diseases, such as obesity, diabetes, and hypertension.
Literature Review and Synthesis
The effectiveness of physical exercise interventions for reducing the risks of CVD is widely explored in the existing body of knowledge. Liang et al. (2021) have demonstrated that implementing an exercise program can enhance an individual’s weight loss, blood pressure, and cholesterol profile, while also reducing cardiovascular risks by regulating inflammation, coagulation, and fibrinolysis. A study by Arija et al. (2017) demonstrates that implementing a nine-month physical activity program can reduce systolic blood pressure, total and LDL cholesterol levels. Two years after the intervention, participants in the program had lower incidences of adverse cardiovascular events and higher adherence to regular physical activity (Arija et al., 2017).
According to Newsom et al. (2002), low adherence to physical activity recommendations among Hispanic groups may be associated with a lack of moderate and vigorous physical activity in their free time. Therefore, educating patients in Spanish in the Physical Wellness Program can provide additional motivation. Furthermore, research conducted by Paydar and Johnson (2020) defined that a higher percentage of Hispanic adults with metabolic syndrome preferred moderate recreational activities over other types of physical activity.
The recommendations in the current Physical Wellness Program primarily focus on making minor adjustments to the individual’s choices to increase their physical activity. Providing the population with additional information about incorporating moderate physical exercises into daily activities, such as jogging or cycling, can enhance the program’s effectiveness by reducing additional CVD risk and promoting daily physical activity.
Conceptual/Theoretical Framework
Jean Watson’s theory addresses the maintenance and restoration of health. The model prioritizes both the prevention of disease and the treatment of existing conditions. According to Watson, providing patient care is the most critical aspect of nursing and is more effective at promoting health than traditional healthcare.
Besides, Watson’s model makes various assumptions, such as caring is comprised of multiple caring variables that contribute to fulfilling a variety of human requirements; good caregiving is beneficial to one’s health and the development of the family. The other assumption is a caring environment, where patients can fulfill their potential while being free to decide what is in their best interest at any particular time (Aghaei et al., 2020).
Watson’s nursing theory is built around four central ideas: person, health, environment/society, and nursing. The first component is Environment/Society, which is the source of the values that dictate how individuals should behave and the objectives they should strive towards. The second component is the person; according to this philosophical perspective, the human being is viewed as a whole and unified entity (Dunn et al., 2020). The significance of a human being transcends and is distinct from that of the sum of their parts.
The third aspect is one’s state of health. The mind, body, and spirit should all be in tune with one another for optimal health. A connection can also be made to health. The component examines the degree to which one’s internal and experienced selves are compatible. The fourth component is nursing, which can be defined as the human science of individuals, their health and illness experiences, and the treatment of these conditions by medical experts. (Dunn et al., 2020).
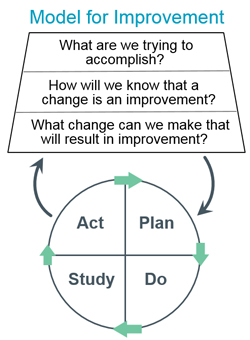
The IHI model for improvement will provide the framework for this QI project, as it is based on the Plan-Do-Study-Act (PDSA) cycle, which is set up into four categories that can be repeated. It helps test a change that has been implemented. (IHI, 2022) The plan is to offer a one-in-person physical activity class, followed by a 1-hour virtual weekly physical activity class coordinated by a DNP student. I plan to observe participants to gain a deeper understanding of the required physical activity levels. I will survey at 4 and 8 weeks to determine if their physical activity levels have increased. The study has not been conducted; therefore, this information has not been gathered.
Goals/Outcomes Measures
- 20 Spanish-speaking adults, 45 to 55 years old with CVD risk, will be recruited in a primary care office for program participation in May.
- 90% of participants will join in person for the first weekly physical activity led by a DNP student.
- 70% will join in a 1-hour virtual weekly physical activity led by the DNP student.
- 70% will increase their physical activity by 5% within 4 weeks of being in the PWC Program.
- 75% of participants will increase physical activity to 150 minutes per week by 8 weeks.
- 50% will have improved knowledge of required physical activity levels to reduce the risk of CVD within 1 month.
- 50% will continue 150 minutes of physical activity after the program is completed.
Project Steps
The participants will be established patients at the primary care site. Participants will be recruited in person. Participants will be cleared to participate in the proposed exercise program by a Primary Care Provider through a physical examination, as well as a cardiologist examination, within the same year. The inclusion criteria for the program are individuals with cardiovascular risk who are over 45 years old and have Spanish as their primary language. All the recruited participants will be asked to participate in the Project and give verbal consent.
The participants’ personal health information will remain confidential for the ethical purpose of protecting their privacy and anonymity. The intervention will begin with one in-person class followed by weekly 1-hour virtual group physical activity classes led by the DNP student, which will also provide participants with information on the importance of physical activity for health. The physical activity will focus on moderate aerobic activities that can be practiced in recreational settings, as well as teaching participants to set specific physical activity goals, such as taking the stairs instead of the elevator.
The participants will be asked to complete a Likert Scale questionnaire to assess how often they exercise and for how long. The Likert questionnaire will be administered on the first day of the program, at the 4-week mark, and at the 8-week mark. The International Physical Activity Questionnaire will be used to measure participants’ physical activity levels and to educate them on moderate to high-intensity exercise. The acquired information will be kept in a password-encrypted computer.
Data Analysis
The test to be applied in the Project will be the Wilcoxon signed rank test. This study will evaluate the relationship between exercise before, during, and after implementing the PWC. The dependent variable is the implementation of the Checklist, and the independent variable is the duration of exercise. The data gathered will be used to show the benefits of implementing the PWC in Spanish. It will also show the specific types of physical activity preferred by adults at risk of CVD. The information will provide the basis for recommendations regarding the required time for regular physical activity and its intensity for patients with CVD risk.
Disseminated Findings
Project results can be disseminated through a PowerPoint presentation or a poster presented at an office meeting. Publication of project results will be available in English and Spanish on the Florida Nurse Association’s website, which will disseminate the Project and its findings to the nursing community at both regional and local levels. Spanish nursing websites in Spanish-speaking countries can also be explored for a publication venue. I can also present the findings in a faculty meeting and explain to nursing students the importance of educating their patients about a healthy and active lifestyle. The Project will be made in English and Spanish.
Cost Benefit
Participants will be provided with refreshments and healthy snacks during the first week of the program. Each participant will also receive a 10-dollar Publix gift card upon program completion. The Project is estimated to cost $400 for handouts, flyers, gift cards, healthy snacks, and refreshments.
Results/Findings
There were 8 participants in this quality improvement project, which was conducted over an 8-week timeframe. At the 4-week mark, out of the 8 participants, 4 were exercising twice a week, 2 were working out once a week, and 2 were exercising 4 times a week. At the end of the study, one participant continued to exercise. None of the participants had exercised before the start of the Project. Based on these findings, the Project’s goals were partially met.
- Goal 1. Not met. While it was forecast that the Project would have 20 participants, only 8 were recruited.
- Goal 2. Met. All of the participants joined offline for the first weekly physical activity.
- Goal 3. Met. 75% (6 out of 8) joined in a 1-hour online weekly physical activity.
- Goal 4. Met. 87% (7 out of 8) increased their physical activity by at least 5% within 4 weeks of being in the program.
- Goal 5. Met. 50% (4 out of 8) successfully reached the target of 150 minutes of physical activity per week within the 8 weeks.
- Goal 6. Met. 50% (4 out of 8) reported on greater awareness of demanded physical activity levels to reduce CVD risk within 1 month.
- Goal 7. Not met. 12% (1 out of 8) of the participants proceeded with 150 minutes of physical activity after the end of the program.
Key Facilitators of Success and Barriers Encountered
The student has encountered some barriers and facilitators of success while working on the program. The participants were motivated by bonuses provided to them (refreshments, healthy snacks, and Publix gift cards), reporting that it was one of the main reasons why they participated. However, with a study sample of less than 50% of what was predicted (8 to 20 participants), the study has only partially met its goals. Hence, the key facilitator of success was the cost-benefit system, while the biggest barrier was the small sample size.
Unintended Consequences
The cost-benefit analysis has underestimated the amount of funds required for handouts. The participants required more refreshments during the first week of the program than was estimated, leading to the initial budget of $400 growing to $450. The reason for this is that the participants did not exercise before the start of the program, and thus started to experience fatigue earlier and required more water.
Project Evaluation
The course of the Project can be evaluated both formatively and summatively. In terms of formative evaluation, due to the smaller sample of participants, adjustments were needed for the course of the project. With a smaller sample, the team was able to communicate with the participants more personally, which led to a higher retention rate and the achievement of the majority of the Project’s goals.
In terms of summative evaluation, while the study sample was smaller, the required goals were met for the sample that was worked with. The team has met the learning objectives, as the primary goals of the Project (5 out of 7) were met. Hence, the team had to be more personal with the participants due to the smaller study sample and managed to meet most of the required goals regardless of this.
Recommendations
In the future, the Project can be repeated with adjustments to recruitment and budgeting. Firstly, the team will need to recruit participants from a larger sample to increase the number of participants for the Project. Secondly, the team needs to allocate a higher budget for refreshments, as most participants are expected to experience fatigue due to a sedentary lifestyle. Thus, the recruitment demographic and the budget for refreshments must be higher.
Conclusion
Despite the small sample size and the overall objectives being missed, the project successfully met the goals set for its participants. The program achieved a moderate degree of success in encouraging an active lifestyle among Spanish-speaking adults aged 45-55 with CVD risk, as demonstrated by half of the participants reporting improved physical activity knowledge and one person continuing to exercise after the program ended.
References
Aghaei, M. H., Vanaki, Z., & Mohammadi, E. (2020). Watson’s human caring theory-based palliative care: A discussion paper. International Journal of Cancer Management, 13(6).
Arija, V., Villalobos, F., Pedret, R., Vinuesa, A., Timón, M., Basora, T.,… & Basora, J. (2017). Effectiveness of a physical activity program on cardiovascular disease risk in adult primary health-care users: the “Pas-a-Pas” community intervention trial. BMC Public Health, 17.
Dunn, K. S., & Robinson-Lane, S. G. (2020). A philosophical analysis of spiritual coping. Advances in Nursing Science, 43(3), 239–250.
Gomez, S., Blumer, V., & Rodriguez, F. (2022). Unique cardiovascular disease risk factors in Hispanic individuals. Current Cardiovascular Risk Reports, 16(7), 51.
Guadamuz, J. S., Durazo-Arvizu, R. A., Daviglus, M. L., Perreira, K. M., Calip, G. S., Nutescu, E. A., Nutescu, E. A., Gallo, L. C., Castaneda, S. F., Gonzalez, F., & Qato, D. M. (2020). Immigration Status and Disparities in the Treatment of Cardiovascular Disease Risk Factors in the Hispanic Community Health Study/Study of Latinos (Visit 2, 2014-2017). American Journal of Public Health, 110(9).
Institute for Healthcare Improvement. (2022). Science of improvement: Testing changes. In Institute for Healthcare Improvement.
Javed, Z., Haisum Maqsood, M., Yahya, T., Amin, Z., Acquah, I., Valero-Elizondo, J., Andrieni, J., Dubey, P., Jackson, R. K., Daffin, M. A., Cainzos-Achirica, M., Hyder, A. A., & Nasir, K. (2022). Race, racism, and cardiovascular health: Applying a social determinants of health framework to racial/ethnic disparities in cardiovascular disease. Circulation: Cardiovascular Quality and Outcomes, 15(1), 72–86.
Khan, S. U., Lone, A. N., Yedlapati, S. H., Dani, S. S., Young, M. T., Khan, M. Z., Watson, K. E., Parwani, P., Rodriguez, F., Cainzos‐Achirica, M., & Michos, E. D. (2022). Cardiovascular disease behavioral risk factors among Latinos by citizenship and documentation status. Journal of the American Heart Association, 11(7), 1–12.
Liang, G., Huang, X., Hirsch, J., Mehmi, S., Fonda, H., Chan, K.,… & Nguyen, P. K. (2021). Modest gains after an 8-week exercise program correlate with reductions in non-traditional markers of cardiovascular risk. Frontiers in Cardiovascular Medicine, 8.
Newsom, J. T., Denning, E. C., Elman, M. R., Botoseneanu, A., Allore, H. G., Nagel, C. L., Dorr, D. A., & Quiñones, A. R. (2022). Physical activity as a mediator between race/ethnicity and changes in multimorbidity. The Journals of Gerontology. Series B, Psychological Sciences and Social Sciences, 77(8), 1529–1538.
Ortega, A. N., Pintor, J. K., Langellier, B. A., Bustamante, A. V., Young, M. T., Prelip, M. L., Alberto, C. K., & Wallace, S. P. (2020). Cardiovascular disease behavioral risk factors among Latinos by citizenship and documentation status. BMC Public Health, 20, 1–9.
Paydar, M., & Johnson, A. A. (2020). Dietary intake, physical activity and metabolic syndrome in African Americans, Hispanics and Whites. Journal of the National Medical Association, 112(2), 215–224.
Roth, G. A., Mensah, G. A., Johnson, C. O., Addolorato, G., Ammirati, E., Baddour, L. M.,… & GBD-NHLBI-JACC Global Burden of Cardiovascular Diseases Writing Group. (2020). Global burden of cardiovascular diseases and risk factors, 1990–2019: update from the GBD 2019 study. Journal of the American College of Cardiology, 76(25), 2982–3021.
Shaw, P. M., Chandra, V., Escobar, G. A., Robbins, N., Rowe, V., & Mascata, R. (2018). Controversies and evidence for cardiovascular disease in the diverse Hispanic population. Journal of Vascular Surgery, 67(3), 960–969.
Shiro, A. G., & Reeves, R. V. (2022). Latinos often lack access to healthcare and have poor health outcomes. here’s how we can change that. Brookings.
U.S. Department of Health and Human Services. (n.d.). Physical activity guidelines, get active. National Heart Lung and Blood Institute.
Vaduganathan, M., Mensah, G. A., Turco, J. V., Fuster, V., & Roth, G. A. (2022). The global burden of cardiovascular diseases and risk: A compass for future health. Journal of the American College of Cardiology, 80(25), 2361–2371.