Signs and Symptoms According to the DSM-5-TR
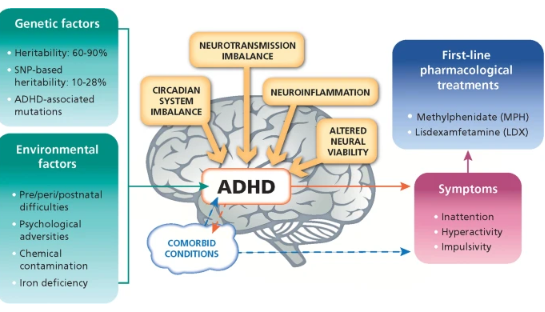
ADHD individuals are unable to concentrate; they get quickly upset and act on impulse. As seen in Figure 1, the disorder’s symptoms are classified as three types of behavioral problems: inattention, hyperactivity, and impulsivity (Kuiper et al., 2021). Based on the DSM-5-TR criteria for the condition, an individual should have six or more signs of inattention for children up to age 16, or five manifestations for adolescents and adults (Koutsoklenis & Honkasilta, 2023).
Some of the classical prodromes include an individual failing to give close attention to details or making careless mistakes, having trouble concentrating on tasks, and not listening when spoken to directly (Gomez et al., 2023). Moreover, the client may seem reluctant to follow commands, does not complete assigned duties, is easily distracted, forgetful, and struggles to engage in activities that require thinking, as shown in Figure 1.

DSM-5-TR criteria dictate that the client should exhibit six or more signs of hyperactivity-impulsivity for children up to age 16, or exhibit five or more signs for adolescents. Symptoms of hyperactivity-impulsivity should be present for at least 6 months to a level that is disruptive to an individual’s personal development (Ahuja & Shazlee, 2021). Some of the classical prodromes of hyperactivity-impulsivity include the patient frequently fidgeting with or tapping their hands and leaving their seat in situations where seating is expected. Other signs include running about in circumstances where they should not, and being unable to participate in leisure activities. Moreover, the patient may talk excessively, blurt out an answer before the question is completed, have trouble waiting for their turn, and intrude on others during conversations.
Differential Diagnoses
ADHD symptoms are likely to overlap with those manifested in other conditions, such as emotional and behavioral disorders, developmental diseases, psychosocial factors, developmental variations, and other medical problems. Clinical signs of anxiety include inability to concentrate, restlessness, hyperactive behaviors, and impulsive reactions (Brooker et al., 2020). Patients with anxiety can have trouble sitting still and are less likely to control fidgeting. All of these symptoms resemble those identified in ADHD. Comparatively, it may lead to challenges in memory, organization problems that hinder concentration, disorientation, and absent-mindedness.
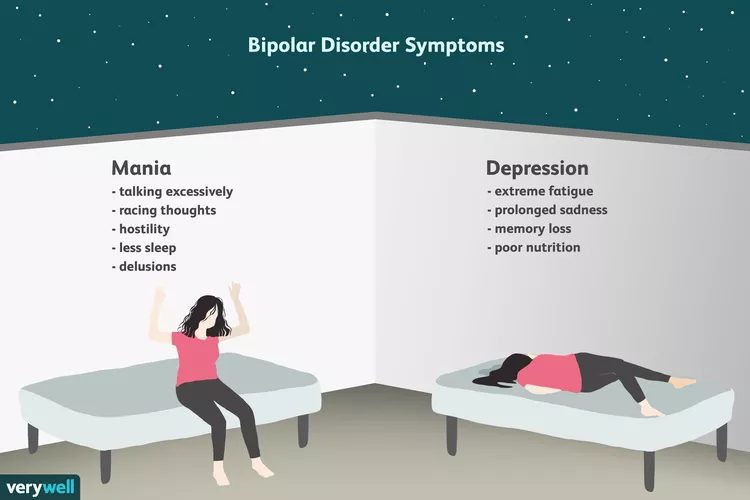
Bipolar disorder can be manifested clinically with such symptoms as intense excitement, hurried thoughts, hyperactivity, impulsive behavior, and excessive talking, as evidenced in Figure 2. This can be confused with those present in ADHD patients. Obsessive-compulsive disorder presents with attention and concentration problems, which might appear among ADHD clients (Magro et al., 2021). ADHD can be associated with the risk of substance abuse, and hence, an individual misusing alcohol might present with conduct problems that are likely to mimic the condition. Some of these may include excessive talking, moodiness, problematic work situations, restlessness, and irritability.
Common ADHD symptoms of attention difficulties, impulsivity, and irritability may arise due to certain conditions like thyroid diseases, allergies, and iron deficiency anemia. Similarly, individuals with learning disabilities might present with issues organizing, processing, remembering, and attention, which are classical manifestations of ADHD (Drigas et al., 2021). Autistic children have prodromes such as hyperactivity, overexcitement, and impulsivity in stimulating environments, which are common in ADHD. Therefore, all these conditions can co-occur with ADHD; thus, proper assessments should be performed to collect and integrate specific information.
Incidence
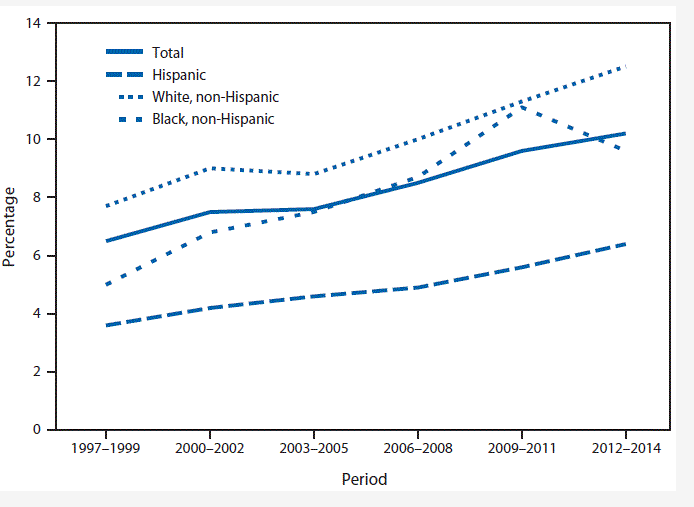
ADHD is among the most commonly diagnosed childhood disorders in America. Ilic and Ilic (2022) study that ADHD is likely to affect 6% of children worldwide, with 1-20% being school-going age. Shrestha et al. (2020) argue that the 2016-2017 National Survey of Children’s Health indicated that more than 5.3 million children in the United States were diagnosed with ADHD, which accounts for 8.8% of the population aged 3-17. The survey showed that the figures had increased by 23% compared to 2003. Statistics indicate that about 2.9 million individuals aged 12-17 have a current ADHD diagnosis, as evident in Figure 3 (CHADD, 2023). These findings reflect a concerning trend for the condition, which has been increasing over the past decade.
Development and Course
Manifestations of ADHD are apparent during childhood. While the exact reason for ADHD is unclear, some elements may exacerbate this condition. For example, environmental and hereditary causes, as well as neuromissive disorders, contribute to this illness, as illustrated in Figure 4. Faldu et al. (2021) argue that exposure to environmental toxins, such as mercury and lead, is implicated in the development of ADHD. Moreover, being a blood relative of ADHD patients, premature birth, and having maternal drug abuse increase the likelihood of developing the condition.
Prognosis
Individuals might not outgrow ADHD, but some might learn to manage their symptoms. They might not meet the criteria for ADHD when they become adults. The disease has no cure, but treatment has been shown to decrease symptoms (Cortese, 2020). For others, the condition might affect their functioning throughout their life. According to Krull and Chan (2019), early identification and management of the condition are essential for improving adult outcomes. Adults with ADHD had a higher chance of having accidents, while children were likely to get injured.
Considerations
While attention deficit disorder is becoming more common, there is an unequal distribution of under- and over-treatment among people of color. Culture and race affect an individual’s perception of ADHD. According to Kappi and Martel (2021), aspects of cultural values, such as parental efficacy and chance, can be linked to the notion that ADHD-related conduct can resolve on its own. Culturally based perspectives can hinder decision-making since children cannot consent to treatment. Parents who believe that ADHD symptoms can resolve on their own might fail to consent to treatment for their children due to age, thus resulting in worsening of symptoms. Clinicians should be aware of and manage their biases, since cultural stereotypes can contribute to the deterioration of the condition.
Treatment
Pharmacological
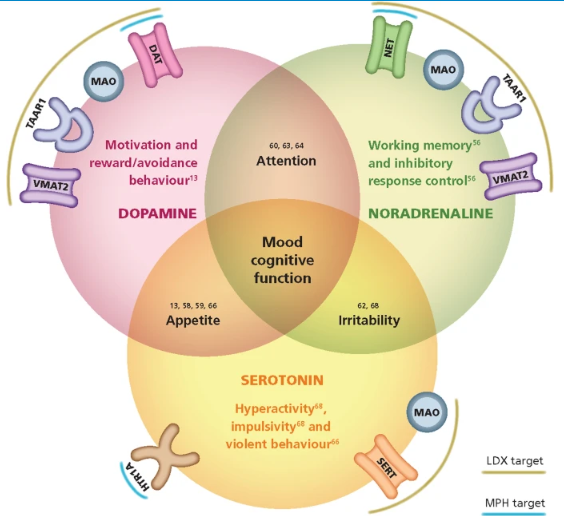
ADHD medications might include nonstimulants such as atomoxetine and stimulants such as Methylphenidate, as evident in Figure 4. According to Cortese (2020), stimulants help manage ADHD and thus should be considered among the first. Rice (2019) argues that Methylphenidate prevents noradrenaline and dopamine uptake in the terminal by blocking the dopamine transporter, as presented in Figure 5.
Common adverse effects of these medications include trouble sleeping, lack of appetite, moodiness, elevated blood pressure, agitation, tension, stomach aches, and headaches. However, Cortese (2020) noted that stimulant use in children with ADHD resulted in reduced vertical growth by 1 cm per year. The side effects occur during the first few days of initiating therapy or taking high doses and might disappear on their own.
Nonpharmacological
Literature supports the nonpharmacological management of ADHD, indicating its effectiveness. Psychosocial treatment for the condition involves behavioral management, training interventions, and physiological treatments. According to Cortese (2020), behavioral interventions are based on adjusting conduct contingencies so that youngsters can increase desired behaviors and limit undesirable ones. Caregivers can be taught how to identify problematic conduct in their children and rebuke unwanted behaviors through nonphysical means, such as rewarding good habits through praise.
In some cases, children with ADHD may qualify to receive special education. In such circumstances, individualized training programs can be tailored to the client and monitored closely. According to Cortese (2020), peer-based interventions, such as social interaction through sharing, peer-mediated interventions, and peer proximity strategies, can improve children’s social skill integration. Psychotherapy interventions, such as cognitive behavior therapy, focus on the youth’s habits and offer training on positive thinking and coping strategies.
Diagnostics and Labs
ADHD, like many conditions, might improve with early interventions. This necessitates testing and evaluation through an empirically validated approach. Currently, there is no laboratory-based test for confirming an ADHD diagnosis. However, initial diagnostic laboratory tests, including liver function tests, serum thyroid function tests, and electrolyte levels, help verify this diagnosis and aid in management. In addition to the DSM-5-TR criteria mentioned, several conditions should be met for one to be diagnosed with ADHD (Kuiper et al., 2021).
The patient should exhibit several symptoms of inattention or hyperactivity-impulsivity that were present before the age of 12. The signs presented should have been present in two or more settings, such as at work, school, with friends, at home, or with relatives. The clinician should ascertain that there is evidence that the prodrome presented interferes with and reduces the client’s quality of school, social, or work functioning. Moreover, the clinician should ascertain that the clinical manifestations do not happen only during schizophrenia or other psychotic disorders. The signs presented should not be better explained by other mental conditions such as anxiety, mood, personality, or dissociative disorders.
Comorbidities
Despite medication prescriptions and administration paired with behavior therapy, some individuals might continue to experience significant symptoms. Conditions such as depression, learning impairments, oppositional defiant disorder (ODD), language problems, anxiety, obsessive-compulsive disorder, and tics might be comorbid with ADHD. According to Koneti (2022), ODD is a common comorbidity for ADHD, and therapists should distinguish between the two conditions. Failure to acknowledge these comorbidities might limit the client’s functional improvement.
Legal and Ethical Considerations
The ethical dilemma of non-maleficence/ beneficence vs fairness may arise when working with people with ADHD. The tutor might order the student not to come back to school before getting drugs. Likewise, hyperactive impulsivity could cause victims to seek legal charges against the convict (Freckelton, 2019). Clinicians should strive to moderate conflicting beliefs and the law to achieve positive outcomes for children. For instance, if the school requires a child to undergo a medical examination for admission, the therapist could contact the school to inform them.
Pertinent Patient Education Considerations
Patient education on ADHD is essential in the management of the condition. The clinician should provide information on the disease, common symptoms, neurological mechanisms, and associated conditions such as anxiety. The therapist should educate the client on how to recognize and remove elements that contribute to impulsivity and inattention. Moreover, the client should be informed of the expected clinical course and intervention strategies, including the associated benefits and risks. The therapist should review how ADHD can affect the patient’s social skills, learning, family life, and behavior. The clinician should offer other ways of learning management through advocacy groups.
References
Ahmed, A. (2022). ADHD: What is the disorder and how is it treated? PlanStreet.
Ahuja, N. & Shazlee, J. (2021). Attention deficit hyperactive disorder: A weakness or a superpower. Journal of Medical and Pharmaceutical Innovation, 8(43s), 31-33.
Brooker, R. J., Moore, M. N., Van Hulle, C. A., Beekman, C. R., Begnoche, J. P., Lemery-Chalfant, K., & Goldsmith, H. H. (2020). Attentional control explains covariation between symptoms of attention-deficit/hyperactivity disorder and anxiety during adolescence. Journal of Research on Adolescence, 30(1), 126-141.
CHADD. (2023). The general prevalence of ADHD.
Cortese, S. (2020). Pharmacologic treatment of attention deficit–hyperactivity disorder. New England Journal of Medicine, 383(11), 1050-1056.
Drigas, A., Mitsea, E., & Skianis, C. (2021). Virtual reality and metacognition training techniques for learning disabilities. Sustainability, 14(16), 10170.
Faldu, K. G., Patel, S. S., & Shah, J. S. (2021). Celastrus paniculatus oil ameliorates synaptic plasticity in a rat model of attention deficit hyperactivity disorder. Asian Pacific Journal of Tropical Biomedicine, 11(3), 105-114.
Freckelton, I. (2019). Attention deficit hyperactivity disorder (ADHD) and the criminal law. Psychiatry, Psychology and Law, 26(6), 817-840.
Gomez, R., Chen, W., & Houghton, S. (2023). Differences between DSM-5-TR and ICD-11 revisions of attention-deficit/hyperactivity disorder: A commentary on implications and opportunities. World Journal of Psychiatry, 13(5), 138-143.
Ilic, I., & Ilic, M. (2022). Global incidence of attention deficit/hyperactivity disorder among children. Biology and Life Sciences Forum, 19(1), 6.
Kappi, A., & Martel, M. (2021). Parental barriers in seeking mental health services for attention deficit hyperactivity disorder in children: Systematic review. Journal of Attention Disorders, 26(3), 408-425.
Koneti, A. (2022). Assessing the effectiveness of the summer treatment program as a behavioral intervention therapy for children with autism and ADHD [CMC Senior Thesis, Claremont McKenna College]. Scholarship@Claremont.
Koutsoklenis, A., & Honkasilta, J. (2023). ADHD in the DSM-5-TR: What has changed and what has not. Frontiers in Psychiatry, 13, 1064141.
Krull, K. R. & Chan, E. (2019). Attention deficit hyperactivity disorder in children and adolescents: Overview of treatment and prognosis. MediLib.
Kuiper, K., Swaab, H., & Tartaglia, N. (2021). Early developmental impact of sex chromosome trisomies on attention deficit-hyperactivity disorder symptomology in young children. American Journal of Medical Genetics Part A, 185(12), 3664-3674.
Magro, M., Scala, M., & Michetti, R. (2021). Adult ADHD vs obsessive-compulsive disorder in the DSM-V Era: A case report between challenging differentiation and comorbidity. International Journal of Psychiatry Research, 4(6), 1-4.
Marcia, P. (2022). Most common symptoms of bipolar disorder. Verywell Mind.
Quintero, J., Gutiérrez-Casares, J. R., & Álamo, C. (2022). Molecular characterisation of the mechanism of action of stimulant drugs Lisdexamfetamine and methylphenidate on ADHD neurobiology: A review. Neurology and Therapy, 11(4), 1489-1517.
Rice, C. D. (2019). Behavioral and Biochemical Studies of Novel Allosteric Modulators of the Dopamine Transporter with Therapeutic Potential. Drexel University.
Saline, S., & Mencher, J. (2022). When children with ADHD explore gender identity: A guide for parents. ADDitude.
Sherry, C. (2020). What is ADHD? Verywell Health.
Shrestha, M., Lautenschleger, J., & Soares, N. (2020). Non-pharmacologic management of attention-deficit/hyperactivity disorder in children and adolescents: A review. Translational Pediatrics, 9(Suppl 1), S114.