Abstract
Autism is a serious disorder that has the potential to disrupt the success of people living with it. This report shall set out to explore various aspects regarding this disorder. To this end, an overview of the symptoms, causes, diagnosis and treatment shall be offered. This shall aim at expanding our understanding regarding this disorder so as to enable us to be better prepared to handle it whenever the need arises.
Introduction
Autism has been noted to be among the most prevalent childhood psychiatric disorder. Kuder (2003) denotes that in the USA, an estimated 2.1% of the population aged between 8 and 17 is affected by autism in its various forms.
Autism is manifested by varied behavior but it is chiefly characterized by inability to communicate, lingual deficits, lack of a sustained attention, low level of activity, temper tantrums, sleep disturbance, aggression inadequate motor control and other non-compliant behavior. These behaviors are detrimental to the social and educational endeavors of the people involved.
Biological and genetic aspects of autism Spectrum Disorders
Autism spectrum is a medical term that is used to describe children and adults who experience difficulties in motor coordination, socializing, communicating (verbal and non-verbal) and language acquisition (Tager-Flusberg, Paul and Lord, 2005). The authors describe autism as a neurological disorder that stems from the brain’s inability to carryout some functions normally.
The causes of Autism as well as the reasons why it affects lingual and communication skills are not entirely known though there is a close linkage between Autism and genetics.
Studies indicate that Autism Spectrum Disorder (ASD) is inherited between family members. A study conducted by the American Psychiatric Association (2000) indicated that there is a 3-6% chance of getting autism amongst siblings.
However, Korvatska et al (2002) state that the difficulty experienced by scientists in pinpointing the genetic aspects of autism emanates from the lack of extended family histories. In most cases, autistic individual become more detached socially that they rarely marry or have children. As such, finding a family that has detailed genetic information regarding autism is difficult.
On a brighter note, twins have been used to explore the genetics behind autism (Beaudet, 2007). One study indicated an 82% likelihood of an autistic identical twin having the same disorder. This is in contrast to the 10% likelihood indicated by results from fraternal twins. More sophisticated studies have in the recent past concluded that 90% of autism related behavioral phenotypes are as a result of inherited genes (Happé & Ronald, 2008). This shows that there is a strong relationship between autism and genes.
Biologically, the root cause of autism has been difficult due to relative inability to access and study the brain systematically. However, technological innovations and advancements such as MRIs, CT scans and SPECT have made it possible to study the structure and functionality of the brain.
As a result, specialists have been able to deduce that majority of the brain’s structures play a pivotal role in the development of ASD. According to NIMH (2009, p. 1) they include but are not limited to “the cerebellum, cerebral cortex, limbic system, corpus callosum, basal ganglia, and brain stem”.
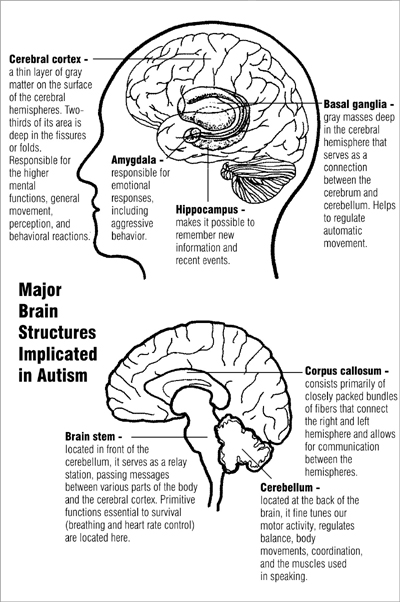
Similarly, other studies indicate that various neurotransmitters such as serotonin and epinephrine have a strong link to autism. The diagram below shows the biological basis of Autism Spectrum Disorder. It shows various structures of the brain and explains the functions that each play. Various symptoms of ASD are as a result of the structures’ inability to carry out their normal function.
A diagram showing brain structures linked to ASD
ASD Etiology
As mentioned earlier, the causes of ASD are not well known. However, researches conducted in this regard indicate that genetic, nutritional and environmental factors play a pivotal role in the development of the disorders. Results from numerous studies indicate that genetic factors predominate.
Others indicate that certain foods, infectious diseases, plastic and metallic extracts could cause autism. Similarly, smoking, alcohol, illicit drugs and some (mercury-based) childhood vaccines have also been attributed to causing autism. However, none of these causes are conclusive and more research needs to be conducted. This is to mean that the theory of causation regarding autism is not complete as yet.
Prevalence of ASD
The most recent survey conducted by center of disease control (CDC) indicated that autism rates have increased significantly over the past three decades. In most cases, studies indicate that autism is most prevalent among children. According to Rutter (2005), boys are four times more likely to be autistic than their female counterparts.
In addition, the author states that the symptoms of autism exhibit themselves from childbirth until three years of age. Parents are the most likely to discover these symptoms. As a result, they should ensure that they have their children checked at the onset of various abnormal behaviors.
Rutter (2005) asserts that the prevalence of autism disorder has been facilitated by ignorance and assumptions made by caretakers. In some cases, parents assume that their children are ‘slow and that they will develop as they grow up. However, this approach has proven to be costly since autism can best be handled as soon as it is detected.
Delaying makes it difficult to come up with remedies and coping mechanisms for both parents and the individuals having autism disorders. The main symptoms of this disorder include communication (verbal and non-verbal) difficulties, inability to develop and maintain relations with other people, abnormal lingual patterns and repetitive behaviors. Whenever any of these symptoms are discovered, it is highly recommended that medical or psychiatric assistance be sought.
Diagnosis of ASD
An early diagnosis of ASD is important since it enables the people involved to come up with effective interventions before its too late. Recent studies show that intensive interventions administered in a control environment for a minimum of two years during preschool leads to behavioral and social improvements among children with ASD.
Clinicians base their diagnosis depending on the behavioral traits exhibited by a child. For a diagnosis to be made, NIMH (2009) asserts that at least one of the symptoms associated with ASD must be present. This means that a patient must have abnormal patterns of communication, socialization and restrictive behaviors.
In most cases, the diagnosis is made through a two-stage process. The first stage is “a developmental screening normally conducted during the routine childhood check-ups, while the second one involves a more comprehensive behavioral analysis by a team of experts (NIMH, 2009, p. 1).” Below are the stages that are followed to diagnose ASD.
Screening
The American Psychiatric Association (2000) recommends that every parent should ensure that a developmental screening test is carried out for his/her child during the “well child” check-up. The author contends that screening plays a pivotal role in the early identification of ASD symptoms.
Due to its importance, there are various screening instruments that have been developed to facilitate the diagnosis process. They include but are not limited to Checklist of Autism in Toddlers (CHAT) and its modified version; M-CHAT. Similarly, the Screening Tool for Autism in Two-Year-Olds (STAT) as well as the Social Communication Questionnaire (SCQ) have proven to be effective in diagnosing ASD in children aged between two years old and above four years old respectively.
According to Tadevosyan-Leyfer et al (2003), questionnaires given to parents provide important information during the diagnosis process. As such, some instruments rely on such responses while others depend on these responses as well as observations made by the caregiver. However, these screening instruments are not as effective as they should be when it comes to identifying mild ASD or Asperger syndrome. As a result, other screening instruments such as the Autism Spectrum Screening Questionnaire (ASSQ) and the Childhood Asperger Syndrome Test (CAST) among others have been developed so as to diagnose these forms of ASD (NIMH, 2009).
Comprehensive Diagnostic Evaluation
This is the second stage of diagnosis and it relies on the skills of a team of different experts such as psychologists, psychiatrists, neurologists, and therapists among others. This evaluation entails a comprehensive analysis of neural, genetic, cognitive and language testing in order to conclude whether a patient is suffering from autism or other behavioral disorders.
Some of the instruments used at this stage include: Autism Diagnosis Interview-Revised (ADI-R), which is a structured interview designed to test a child’s “communication, social interaction, restrictive behaviors and age-of-onset symptoms, and the Autism Diagnosis Observation Scheduling (ADOS-G), which is designed to identify abnormal, missing or delayed communication and social behaviors (NIMH, 2009, p. 1).”
The teams of experts that conduct this diagnosis determine the strengths and weaknesses of the child and recommend various treatment options that should be undertaken.
Treatment of ASD
According to Freitag (2007) there is no one-shoe-fits-all approach to treating ASD. However, specialists in this area seem to agree on the fact that early interventions are of great importance. Arguably, the best treatment is one that considers the interests of the patient, allows the patient to learn in accordance to his/her ability and causes no harm to the overall well being of the patient. With this in mind, there are specialized programs and treatments that have proven to be effective against ASD symptoms.
For starters, Applied Behavioral Analysis (ABA) is among the most used intervention in treating ASD (SAMHSA, 2011). Similarly, there are dietary and medical interventions that help suppress unwanted behaviors among autistic children (NIMH, 2009). In regard to learning, there are specialized educational programs that seek to enhance the socio-communicative, cognitive and language skills of autistic students.
Conclusion
It can be articulated from this report that Autism is a problem that needs to be focused on. With proper understanding as to what the condition entails, parents and practitioners are better armed to assist patients overcome the weaknesses brought about by the condition and therefore achieve successful lives.
From this study, it can be authoritatively stated that early diagnosis and treatment of Autism spectrum is necessary to increase the chances of success in learning for the child suffering from this disease. Whereas Autism is not curable, it can be managed so as to ensure that it is not disruptive to the life of the individual during his/her future endeavors.
References
American Psychiatric Association. (2000). Diagnostic and statistical manual of mental disorders: DSM-IV-TR (fourth edition, text revision). Washington DC: American Psychiatric Association.
Beaudet, A. L. (2007). Autism: highly heritable but not inherited. Nat Med, 13(5): 534–6.
Freitag, C. M. (2007). The genetics of autistic disorders and its clinical relevance: a review of the literature. Mol Psychiatry. 12(1): 2–22.
Happé, F., & Ronald, A. (2008). The ‘fractionable autism triad’: a review of evidence from behavioral, genetic, cognitive and neural research. Neuropsychol Rev, 18(4): 287–304.
Korvatska, E et al. (2002). Genetic and immunologic considerations in autism. Neurobiology of Disease, 9: 107-125.
Kuder, S. (2003). Teaching Students with Language and Communication Disabilities. USA: Allyn and Bacon.
NIMH. (2009) Autism Spectrum Disorders (Pervasive Developmental Disorders). Web.
Rutter, M. (2005). Incidence of autism spectrum disorders: changes over time and their meaning. Acta Paediatr. 94(1): 2–15.
SAMHSA. (2011). Autism Spectrum Disorders. Web.
Tadevosyan-Leyfer, O et al. (2003). A principal components analysis of the autism diagnostic interview-revised. Journal of the American Academy of Child and Adolescent Psychiatry, 42(7): 864-872.
Tager-Flusberg, H., & Lord, C. (2005). Language and Communication in Autism. Web.