Introduction
Photographs in the past were regarded as a reliable way of keeping memories. Most people took photos for autobiographical purposes intended to serve as a memory and communication. For example, photographs were used as a reminder of how life was in the past. Photography has since moved on from a reserve of family memories into other fields. According to Maître (2017, p.1), this change began forty years ago when solid digital sensors replaced analog silver films. The introduction of solid digital sensors meant led to the development of point-and-shoot cameras that fits in a pocket. Then they were introduced into mobile phones and tablets, leading to the revolution of the photographic industry (Maître, 2017, p.1). Maître (2017, p.5) noted that compact cameras were the first digital cameras introduced in the 1980s.
Compact cameras comprised of a fixed lens, retractable focal length, and the viewing was done through a screen. These cameras could comfortably fit into a pocket. However, most cameras in modern society consist of internal and removable memory, visualization and modification screens, image stabilization elements, filters and lenses, and shutters, focus, and light measurement mechanisms (Maître, 2017, p.309). These advancements facilitated the integration of photography into the medical sector. This paper analyzes improvements of digital cameras in the healthcare industry, focusing on the field of dermatology.
Medical practitioners use photography for a variety of reasons while treating patients. In 1840, Alfred Donne photographed sections of bones, teeth, cells from body fluids, and cellular debris in what is the first recorded case of medical photography (Harting et al., 2015, p.401). Since then, advances in cameras have increased the application of photography in medical specialties, such as dermatology, radiology, pathology, and psychiatry.
The photographs are a great way to document patients’ history and are used to track the progression over time accurately. For instance, dermatologists use magnification and non-polarized light to view skin lesions, which helps in improving diagnostic capability (Harting et al., 2015, p.402; Michelangeli, 2019, p.7). High-quality images provided by digital photography are useful in the medical sector because doctors use them to track disease progression and educate patients.
Dermatology is a visual-based field because it involves the collection of photography and imaging for diagnosis and tracking the effectiveness of the medicine. According to Michelangeli (2019), doctors used to sketch or paint illustrations of skin diseases before the invention of photography. Therefore, the introduction of black and white photography in the mid-nineteenth century helped the doctors to capture images and hand color the areas with lesions after live observation. The introduction of digital and high-quality imaging systems further helped dermatologists in analyzing patients’ skin conditions.
Challenge
Several experiments have been conducted to evaluate the effectiveness of imaging and photography in dermatology. A study by Milam and Leger (2018) study included a total of 157 dermatologists, examined their habits and opinions. These researchers used SurveyMonkey questionnaires to gather answers from dermatologists in the United States. Of the total 153 participants who responded, 61.8% of the dermatologists indicated they use medical photography daily, whereas 21.7% reported they use imaging almost with every patient (Milam and Leger, 2018, p.5). The experts said varied opinions and habits on medical photography.
Milam and Leger (2018) noted the diverse use of photography in dermatology. 87.5% of the participants used photography to document biopsy sites, 60.0% in research and publications, 72.4% in teaching, 54.6% to liaise with dermatopathologists and care providers, and 82.9% to track disease progression. A total of 70 participants (46%) admitted that they used smartphones to take the images. 77.1% of those used smartphones, whereas only 42.9% admitted to using secure electronic medical record applications. Further, 75.7% of participants indicated they obtained consent for photographs from their participants to take the pictures.
Additionally, 74.5% reported that doctors received electronic or hard copies of photos from the patients, whereas only 47.4% confirmed using secure messaging systems. Milam and Leger (2018) study assessed privacy issues when collecting photographs and images from the patients. The privacy issues include consent, safety standards, and other liability concerns that occur when using patients’ photography.
Solutions
Necessary security measures should be put in place to safeguard pictures captured by dermatologists because they often contain personally identifiable information. A study conducted by Abbott et al. (2018) examined Australian dermatologists and dermatology trainees in their natural practices relating to clinical smartphone use. The study used an anonymous 24-question survey in the SurveyMonkey platform where the dermatologists were required to state their reasons for capture, transmission, and storage of clinical images. The survey also analyzed whether consent was obtained, awareness of current guidelines, and work policy as well as reliance on smartphones.
Results
In total, 105 dermatologists and dermatology trainees across Australia participated in the study. The results show that 97% of the respondents carried their smartphones with them at work. The majority of the participants indicated they sent or received images on their smartphones or emails regularly. Further, dermatologists stated they captured images of the patients mainly for obtaining advice from colleagues (60%), while 55% gathered images with the aim of monitoring patient progress (Abbott et al., 2018, p.102). Others captured images for education purposes (38%), communication with caregivers (34%), research (12%), and backup if dedicated cameras were to fail (8%). The main reasons for receiving or sending images were advice on diagnosis (90%), recommended treatment (85%), general counsel (32%), education (17%), and monitoring rural patients (5%). Most respondents used email (85%), 70% used text, and 7% used special applications for clinical photography (Abbott et al., 2018, p.103).
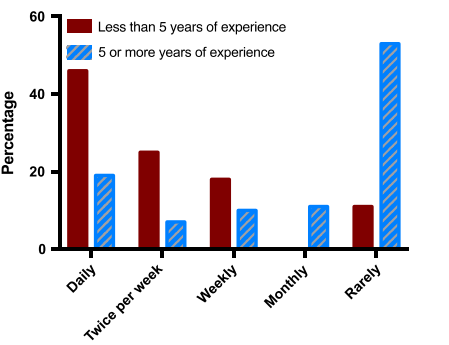
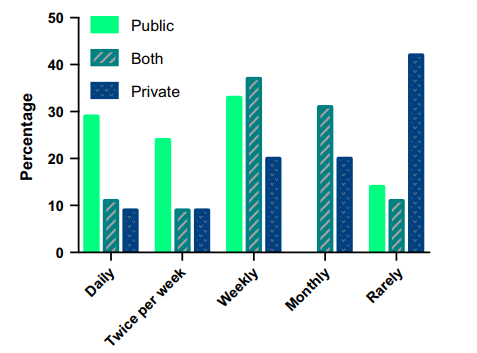
The study shows that consent was obtained when taking photographs, but not for documenting the images. Additionally, only 2% got written consent, while 30% sought verbal permission and recorded it as part of clinical documents. Further, 46% of the participants obtained verbal consent and did not document it in the patients’ records (Abbott et al., 2018, p.104). Also, research indicated 22% of the participants reported being aware of the workplace guidelines concerning the use of smartphones in clinical photography. Other respondents (34%) reported awareness of formal workplace procedures for using patients’ photos on smartphones.
Only a few people had read the guidelines on clinical photographs and the use of personal images, and 65% of the participants indicated the need for further education on taking, transmitting, and documenting clinical pictures on smartphones.
Evaluation
Evidence collected from the research studies shows that images collected by dermatologists are essential in improving service delivery. Abbott et al. (2018, p.105) noted that high-quality photos add value to clinical consultations, especially when the images accurately capture the color, texture, and depth of the skin lesions. However, there are considerable risks associated with the use of digital images in photography, especially when specialists fail to comply with the written technology-based guidelines. Therefore, dermatologists have moral and legal obligations to ensure photography captured supplements communication and services delivery without compromising the privacy of the patients. Specialists should also focus on obtaining written consent from the patients for specific purposes (Ashique et al., 2015, p.3). For instance, doctors should emphasize when the images are to be recorded and shared with other caregivers.
Without proper privacy guidelines, the adoption of digital technology in healthcare might create more problems than advantages they offer. Therefore, many organizations have focused on creating guidelines and policies for safeguarding information. For instance, the Health Insurance Portability and Accountability Act (HIPAA) was enacted to ensure the privacy and protection of medical records (Nettrour et al., 2019, p.2). As a result, any individually identifiable information is protected under HIPAA, including the images taken by dermatologists.
The communication mechanisms noted in the two studies do not meet the clinical guidelines and standards. The use of smartphones to text or email images exposes the data to potential attacks because they do not meet encryption standards. Nettrour et al. (2019, p.3) noted that even under the circumstances that the smartphones have encryption standards, images should not be texted, they can easily be intercepted. The authors recommended the use of electronic medical transmission systems because they are designed to store and share personally identifiable information securely. These systems also comply with HIPAA rules, such as performing data backup services and changing passwords regularly to ensure security. Dermatologists and medical professionals should seek written consent when they want to take, store, or share patients’ information.
Reference List
Abbott, L.M., Magnusson, R.S., Gibbs, E. and Smith, S.D. (2018) ‘Smartphone use in dermatology for clinical photography and consultation: current practice and the law’, Australasian Journal of Dermatology, 59(2), pp.101-107. Web.
Ashique, K.T., Kaliyadan, F. and Aurangabadkar, S.J. (2015) ‘Clinical photography in dermatology using smartphones: an overview’, Indian dermatology online journal, 6(3), p.158-163. Web.
Harting, M.T., DeWees, J.M., Vela, K.M. and Khirallah, R.T. (2015) ‘Medical photography: current technology, evolving issues and legal perspectives’, International journal of clinical practice, 69(4), pp.401-409. Web.
Maître, H. (2017) From photon to pixel: the digital camera handbook. John Wiley & Sons.
Michelangeli, F. (2019) ‘Imaging the unimaginable: medical imaging in the realm of photography’, Clinics in dermatology, 37(1), pp.38-46. Web.
Milam, E.C. and Leger, M.C. (2018) ‘Use of medical photography among dermatologists: a nationwide online survey study’, Journal of the European Academy of Dermatology and Venereology, 32(10), pp.1804-1809. Web.
Nettrour, J.F., Burch, M.B. and Bal, B.S. (2019) ‘Patients, pictures, and privacy: managing clinical photographs in the smartphone era’, Arthroplasty Today, 5(1), pp.57-60. Web.