Background
Generic name: Clozapine.
Brand names: Clozaril, FazaClo, Versacloz, Clopine, CloZAPine Synthon, Denzapine, Zaponex.

According to the FDA (2023), indications for taking Clozapine are:
- treatment of schizophrenia in patients who do not demonstrate positive dynamics when using other medications;
- reducing the risks of suicidal and self-harming behavior associated with schizophrenia and other psychotic disorders.
Drug Classification
The drug is an atypical antipsychotic, which determines the key differences in its use. Advantages:
- fewer side effects;
- targeting negative symptoms;
- lack of pronounced inhibitory effect;
- no effect on the production of sex hormones;
- complex effect on dopamine and serotonin levels;
- potential to treat severe cases of schizophrenia (Gammon et al., 2021).
Mechanism of Action
Clozapine affects neuronal readaptation by modulating neurotransmitters, including dopamine and serotonin. Less dopamine-like formula prevents extrapyramidal side effects (Gammon et al., 2021). Similar to the serotonin receptor, the chemical composition helps balance neurotransmitters in the patient’s brain and reduce symptoms of schizophrenia. It significantly improves symptoms within 14 days of starting treatment.
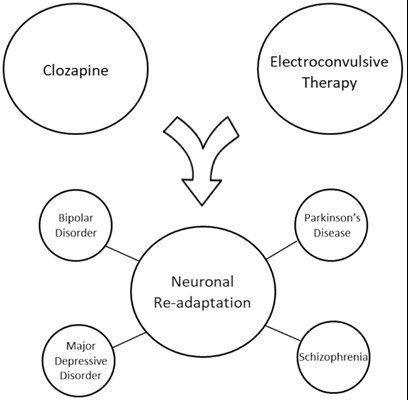
Pharmacokinetics and Pharmacodynamics
The pharmacokinetics of Clozapine share similarities with SSRIs.
- Absorption. After oral administration, Clozapine is absorbed at a rate of 90-95% (de Leon et al., 2020).
- Distribution. When taking the drug 2 times a day, the maximum concentration in the blood is achieved on average after 2.1 hours (Clozapine, n.d.).
- Metabolism. According to Edinoff et al. (2021), “clozapine is extensively metabolized by the hepatic cytochrome P450 (CYP) system” (p. 459).
- Removal. The half-life of the drug takes from 6 to 26 hours.
Note: Possible disruption of drug absorption with age and in cases of kidney and liver diseases.
Complex pharmacodynamics due to simultaneous interactions with dopamine, serotonin, and other neurotransmitters.
- Blocking action on dopamine receptors.
- Antiserotonergic properties.
- Antipsychotic and sedative effects.
Dosing
Initial dose. 12.5 mg orally once or twice a day (Sinha, 2023, para. 33).
Maintenance dose. May increase total daily dose in increments of 25 mg to 50 mg per day to a target dose of 300 mg to 450 mg per day (Sinha, 2023, para. 34).
The medication is taken orally. Dosing can be changed for specific populations, and consider taking other medications, including:
- CYP inhibitors;
- CYP inducers;
- Drugs for kidney and liver failure treatment (Clozapine, n.d.).
Specific Populations
- Children and Adolescents. The use of the drug is not recommended due to the specific nature of its effects and the lack of sufficient evidence.
- Elderly. Initial dosing is 12.5 mg orally once a day, with the possibility of increasing the dosage, provided there are no metabolic disturbances.
- Pregnant. Use is possible at a minimum dosage, provided the potential benefits of the intervention outweigh the associated risks for both the mother and fetus. It is not recommended to take the drug in the third trimester due to increased risks “for extrapyramidal and/or withdrawal symptoms following delivery” (Clozapine, n.d., para. 25).
- Individuals with Suicidal Behavior. Clozapine is indicated to reduce the risk of recurrent suicidal behavior.
Half-Life and Side Effects
A drug’s half-life is the period during which the drug is partially eliminated from the body, and its amount is halved. The half-life of the drug is approximately 12 hours (Edinoff et al., 2021). Its importance lies in the following:
- Avoiding the accumulation of the drug in the body.
- Establishing dosage and frequency of administration.
- Development of individual treatment regimens.
- Preventing side effects.
Common side effects include:
- dizziness
- headaches
- nausea
- constipation
- weight gain
- blurred vision
- fever
- increased sweating
- insomnia
- hypotension
- sedation/somnolence
- tachycardia.
Adverse reactions:
- seizures
- liver problems
- cough
- trouble breathing
- dry mouth
- hypertension
- rigidity
- confusion
- urinary abnormalities
- rash
- diabetes mellitus
- cardiomyopathy
- myocarditis
- paralytic ileus
- dyslipidemia.
Contraindications
Contraindications for Clozapine include (Sinha, 2023, para. 12):
- heart problems, high blood pressure;
- a seizure, head injury, or brain tumor;
- diabetes, or risk factors such as being overweight;
- high cholesterol or triglycerides;
- liver or kidney disease;
- glaucoma;
- smoking.
Clozapine is contraindicated when used with some other drugs, such as (Clozapine, n.d., para. 12):
- amisulpride
- dronedarone
- eliglustat
- fezolinetant
- irinotecan
- irinotecan liposomal
- nirmatrelvir
- nirmatrelvir/ritonavir
- saquinavir
- thioridazine.
Searching for alternatives is recommended when using:
- asenapine;
- bupropion;
- clarithromycin;
- dopamine;
- hydrocodone;
- lithium;
- rifampin;
- trazodone;
- zidovudine and other medications.
Overdose
Maximum dosing is 90 mg daily. Overdose may cause:
- severe sedation;
- delirium;
- cardiovascular effects;
- seizures.
Diagnostics and Labs Monitoring
- Regular CBC should be performed to monitor white blood cell levels (Correll et al., 2022).
- Cardiovascular monitoring with an electrocardiogram (Correll et al., 2022).
- Monitoring of the functioning of the kidneys and liver.
- Regular general physical examination to identify side effects and make changes to the treatment plan.
Considerations
Comorbidities. Special cases concern the prescription and dosage of Clozapine for patients with cardiovascular disease, liver and kidney disorders, and populations at increased risk of diabetes.
Legal and Ethical. Prescribing Clozapine requires patient education about the risks and consequences of the intervention, as well as ongoing monitoring to prevent deterioration in physiological parameters.
Pertinent Patient Education. Patients should be informed of the potential risks and early signs of serious side effects.
References
Clozapine (Rx). (n.d.). Medscape.
Correll, C. U., Agid, O., Crespo-Facorro, B., de Bartolomeis, A., Fagiolini, A., Seppälä, N., & Howes, O. D. (2022). A guideline and checklist for initiating and managing clozapine treatment in patients with treatment-resistant schizophrenia. CNS Drugs, 36(7), 659–679.
de Leon, J., Ruan, C. J., Schoretsanitis, G., & De Las Cuevas, C. (2020). A rational use of clozapine based on adverse drug reactions, pharmacokinetics, and clinical pharmacopsychology. Psychotherapy and Psychosomatics, 89(4), 200–214.
Edinoff, A. N., Fort, J. M., Woo, J. J., Causey, C. D., Burroughs, C. R., Cornett, E. M., Kaye, A. M., & Kaye, A. D. (2021). Selective serotonin reuptake inhibitors and clozapine: Clinically relevant interactions and considerations. Neurology International, 13(3), 445–463.
FDA. (2023). Information on Clozapine. US Food & Drug Administration.
Flanagan, R. J., Lally, J., Gee, S., Lyon, R., & Every-Palmer, S. (2020). Clozapine in the treatment of refractory schizophrenia: a practical guide for healthcare professionals. British Medical Bulletin, 135(1), 73–89.
Gammon, D., Cheng, C., Volkovinskaia, A., Baker, G. B., & Dursun, S. M. (2021). Clozapine: Why is it so uniquely effective in the treatment of a range of neuropsychiatric disorders? Biomolecules, 11(7), 1030–1048.
Hallare, J., & Gerriets, V. (2023). Half-life. National Library of Medicine.
Sinha, S. (2023). Clozapine. Drugs.