Executive Summary
Mental health is an integral part and the most critical component of health, and it can contribute to inequality within biased or discriminatory systems of healthcare. The primary features of mental health care include a robust nervous system and a balanced mind, body, and spirit (Kilbourne et al., 2018). Mental illness inequality has been a problem for many societies for centuries and has only become more pronounced in recent years.
The Covid-19 pandemic only exacerbated the issue, leaving many people struggling to cope with psychological issues such as fear, loneliness, and isolation (Kwong et al., 2020). According to Campion et al. (2020), the pandemic caused a significant increase in mental health issues, with anxiety and depression being the most common. This was especially prominent among vulnerable groups such as those with pre-existing mental health conditions, young people, and minority communities.
The mental health inequalities in the country have also been compounded by the economic downturn caused by the pandemic. The main reason is that many people, including the mentally ill, lost their jobs or had their incomes significantly reduced (Masters et al., 2020). This has led to increased poverty and inequality, particularly impacting minority communities, people from low-income households, and those living in rural areas (Gilbody et al., 2019). The stigma surrounding mental health issues, especially among minorities, further exacerbates the issue and makes it even harder to access care (Spoorthy et al., 2020). Many of these populations attribute the decreased access to mental health care to a lack of insurance coverage, inability to pay for services, and limited access to mental health providers in rural areas.
The pandemic also caused significant disruption to mental health services, with many services being suspended or scaled back. This disruption created a shortage of mental health professionals, especially nurses, making it difficult for those needing mental health care (Vindegaard and Eriksen Benros, 2020). Thus, mental illness inequality refers to the unequal distribution of mental health resources and services among different populations. This can include disparities in access to treatment, quality of care, and outcomes for people with mental illness based on factors such as race, ethnicity, socioeconomic status, and geographic location.
Population and Demographics
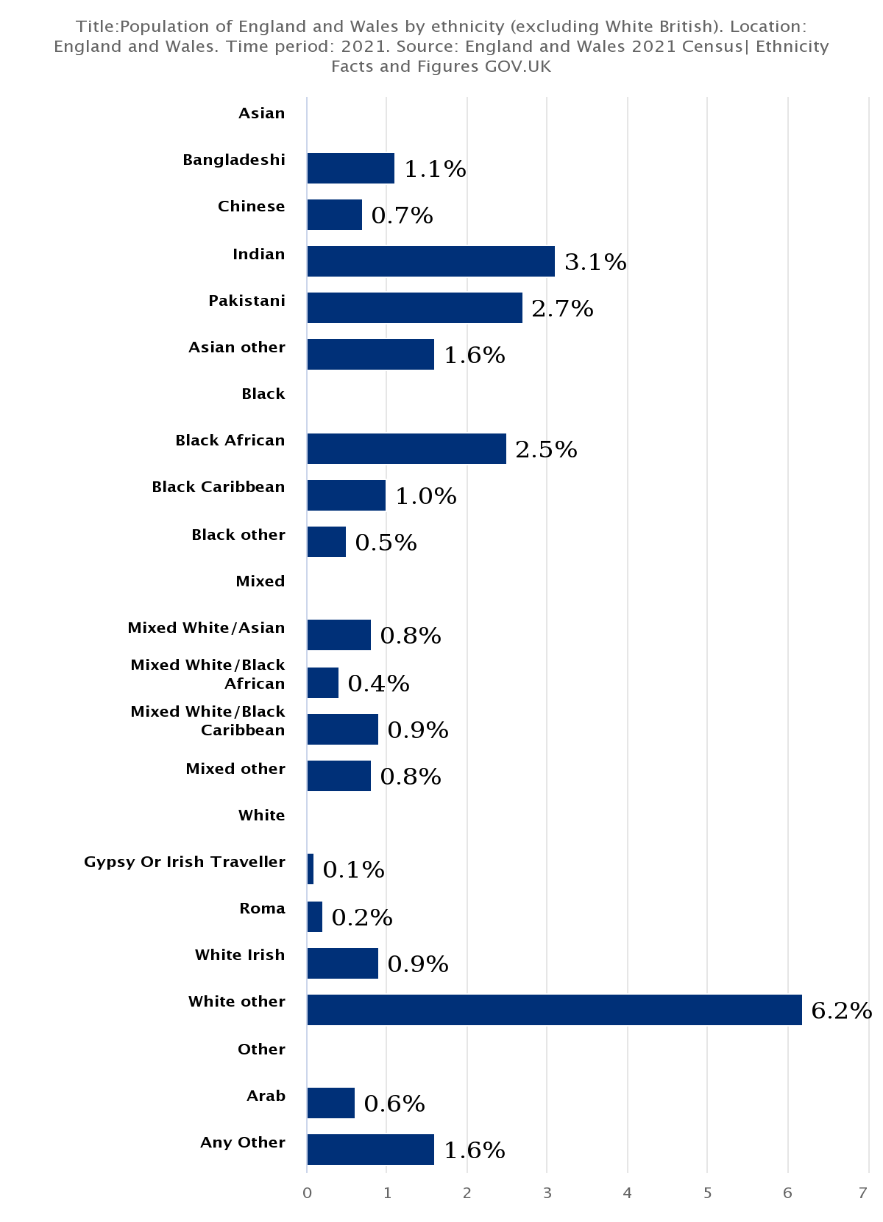
The minority ethnic populations in the UK represent a diverse range of backgrounds, cultures, and religions. According to the 2021 Census, minority ethnic populations made up 18.3% of the total population in England and Wales, with the largest minority being the Asian/Asian British (9.3%). This is followed by the Black/Black British (4.0%) and other mixed and minority groups, which constitute 2.9% and 2.1%, respectively (Office for National Statistics, 2022).
Figure 1 illustrates the population of England and Wales, highlighting the proportion of minority ethnic groups. Research by Hackett et al. (2020) has shown that minorities in the UK are at increased risk of poorer health outcomes and inequalities compared to the majority population. This is due to various factors, such as unequal access to healthcare services, cultural and language barriers, poverty, and discrimination.
To understand why mental illness inequality is more prevalent in certain areas or within certain demographics, it is vital to critically analyze the core factors, contributors, and determinants. The Social Determinants of Health (SDH) refer to the conditions in which people are born, grow, live, work, and age, and which shape the health of populations (Islam, 2019). According to Dahlgren and Whitehead’s Ecological Systems Model, health and well-being are determined by individual and contextual factors (Dahlgren and Whitehead, 2021).
The model suggests that the SDH is multi-level, with the influence of individual factors, such as lifestyle and behavior, being mediated by contextual factors, including economic, social, and environmental influences. For example, minority ethnic groups are more likely to live in areas with poor housing, inadequate sanitation, and high levels of air pollution. This can lead to several health issues, including respiratory and skin conditions.
The social environment also impacts the health of minority ethnic groups and people from low-income households. These populations are more likely to experience discrimination and marginalization, which can lead to higher stress levels and mental health issues. They tend to experience a lack of social support networks, which can further exacerbate their health issues. Additionally, minority ethnic groups may be subject to cultural and language barriers and discriminatory policies, making accessing resources even more difficult (Kilbourne et al., 2018). By analyzing the Dahlgren and Whitehead model, it is possible to gain a better understanding of the factors that contribute to health disparities among minority ethnic groups and those from low-income households in the United Kingdom.
Public Health Issue
Impact
Mental illness inequality is a problem for society because it perpetuates disparities in mental health outcomes and limits the potential of individuals and communities. According to MHFA England’s (2020) epidemiological data estimates, one in four adults in the UK will experience a mental illness in any given year. In the UK, mental illness disproportionately affects those from less affluent backgrounds, with research showing that people living in deprived areas are more likely to experience mental health inequalities (MHFA England, 2020).
Those from minority ethnic backgrounds are also more likely to experience mental health inequalities due to the racism and discrimination they often face. This is large because these individuals are often exposed to higher stressors, such as poverty, homelessness, and unemployment, and face greater barriers to accessing appropriate mental health services. Thus, mental illness and inequality in the UK have a serious and wide-reaching impact on individuals and populations. Individuals who have a mental illness can experience various issues, including depression, anxiety, insomnia, substance abuse, and suicidal thoughts. On a population level, mental illness can lead to a wide range of social and economic problems, including increased poverty, homelessness, and crime.
Changeability
The health needs and determinant factors of mental health inequality can be changed through a combination of policy, programmatic- and individual-level interventions. To be effective and sustainable, these interventions must address the underlying social determinants of health that contribute to mental health inequality, such as poverty, discrimination, and lack of access to education and employment opportunities (Kilbourne et al., 2018).
This can be achieved through a range of measures, including increased access to mental health services, expanded employment opportunities, provision of educational opportunities, and advocacy for social and political change. These measures can not only help to reduce the prevalence of mental illness but also reduce inequality. To ensure that these changes are sustainable, it is crucial to focus on long-term solutions that are monitored and evaluated over time. These solutions may include providing access to education, creating economic opportunities, and advocating for social and political reforms.
Acceptability
To achieve the maximum impact when tackling mental illness and inequality, a set of changes must be made to address the underlying causes of mental illness and inequality. The changes must be based on a thorough understanding of how mental illness and inequality are created and perpetuated, and must consider the various impacted stakeholders and the resources available to address these issues. Some of these changes include:
- Increase access to mental health care services, especially for those in marginalized communities.
- Enhance public awareness and understanding of mental health issues through targeted public education campaigns.
- Enhance the quality of mental health services, regardless of their background or financial situation.
- Increase research into mental illness to improve our understanding of mental illness and develop better treatments.
- Develop better systems of care: Mental health services need to be integrated into a comprehensive system of care that provides support to individuals with mental illness.
- Strengthen the mental health parity law to ensure that mental health care is treated like physical health care.
Resource Feasibility
Despite increasing awareness of mental illness and inequality in the UK, there are still not enough resources available to make the necessary changes. The government has increased spending on mental health services in recent years; however, demand for these services continues to outpace available resources. A recent report by the Mental Health Foundation (2020) estimated that the economic impact of mental illness costs the UK economy £105 billion a year, with a further £34.9 billion in lost productivity.
The report also highlighted the cost of mental health services, with NHS expenditure on mental health services in England rising from £9.9 billion in 2015/16 to £12.2 billion in 2018/19. Additionally, there are still significant gaps in access to mental health services, especially in more deprived areas. While the UK government has made commitments to combat inequality, there is still much work to be done to ensure that everyone has equal access to opportunities.
Policies and Strategies
The UK government has recognized the importance of addressing mental health and inequality issues. The NHS has developed a range of policies, strategies, and guidelines to help address and change these issues (NHS, 2022). These are primarily NHS initiatives aimed at ensuring the health and well-being of citizens and promoting social inclusion. These policies and strategies are linked to the national government authority policy, and they include:
- Mental Health Strategy 2020-2025. This strategy outlines the government’s plan to enhance mental health services and reduce inequalities in England. It contains a detailed action plan to ensure that mental health services can meet the needs of those who require them.
- Mental Health Equality Delivery System. This system outlines the government’s commitment to reducing inequalities in mental health services and ensuring that everyone has access to quality mental health care. The system encompasses specific initiatives, including increasing access to mental health services for individuals from diverse backgrounds, enhancing the quality and safety of mental health services, and bolstering the mental health workforce.
- Mental Health Act 1983. This Act outlines the legal rights of individuals with mental health issues, including their entitlement to treatment and support (NHS, 2022). The Act also protects the rights of people with mental health problems and ensures that their rights are respected.
- Mental Health Taskforce. This Taskforce was established in 2015 to ensure the effective implementation of the government’s mental health strategy (NHS, 2015). The Taskforce guides efforts to reduce inequalities in mental health services, as well as strategies to enhance access to mental health care.
- Health and Social Care Act 2012. This Act provides for improved access to mental health services, with an emphasis on promoting early intervention and prevention (Glover-Thomas, 2013).
The Intervention Designed to Change Health Outcomes
The Campaign: Audience and Correlations
The UK has seen a rise in mental illness and inequality in recent years, leading to the development of various campaigns aimed at tackling these issues. One such campaign is “Every Mind Matters (EMM),” launched by Public Health England in partnership with the NHS. The campaign is designed to raise awareness of mental health issues while providing practical guidance and tips to help people take control of their mental well-being.
Thus, its intended audience is people with mental illnesses who regularly experience inequality. The campaign’s objectives and intentions correlate with the identified demographic data. The campaign utilizes a variety of media channels to reach its target audiences, including websites, social media, radio, television, print media, and public events (NHS, 2021). It is based on the idea that mental health is just as important as physical health and that everyone can take simple steps to improve their mental well-being.
The Transtheoretical Model of Change
The Transtheoretical Model of Change (TMC) provides a framework for understanding the process of behavior change and how individuals progress from one stage to the next. It was developed and designed by Prochaska and DiClemente in 1983. According to the model, behavior change involves a sequence of five stages: pre-contemplation, contemplation, preparation, action, and maintenance (LaMorte, 2019). The TMC has been successfully used to describe and explain the process of behavior change in a variety of contexts. Figure 2 highlights the stages of the Transtheoretical Model of Change.
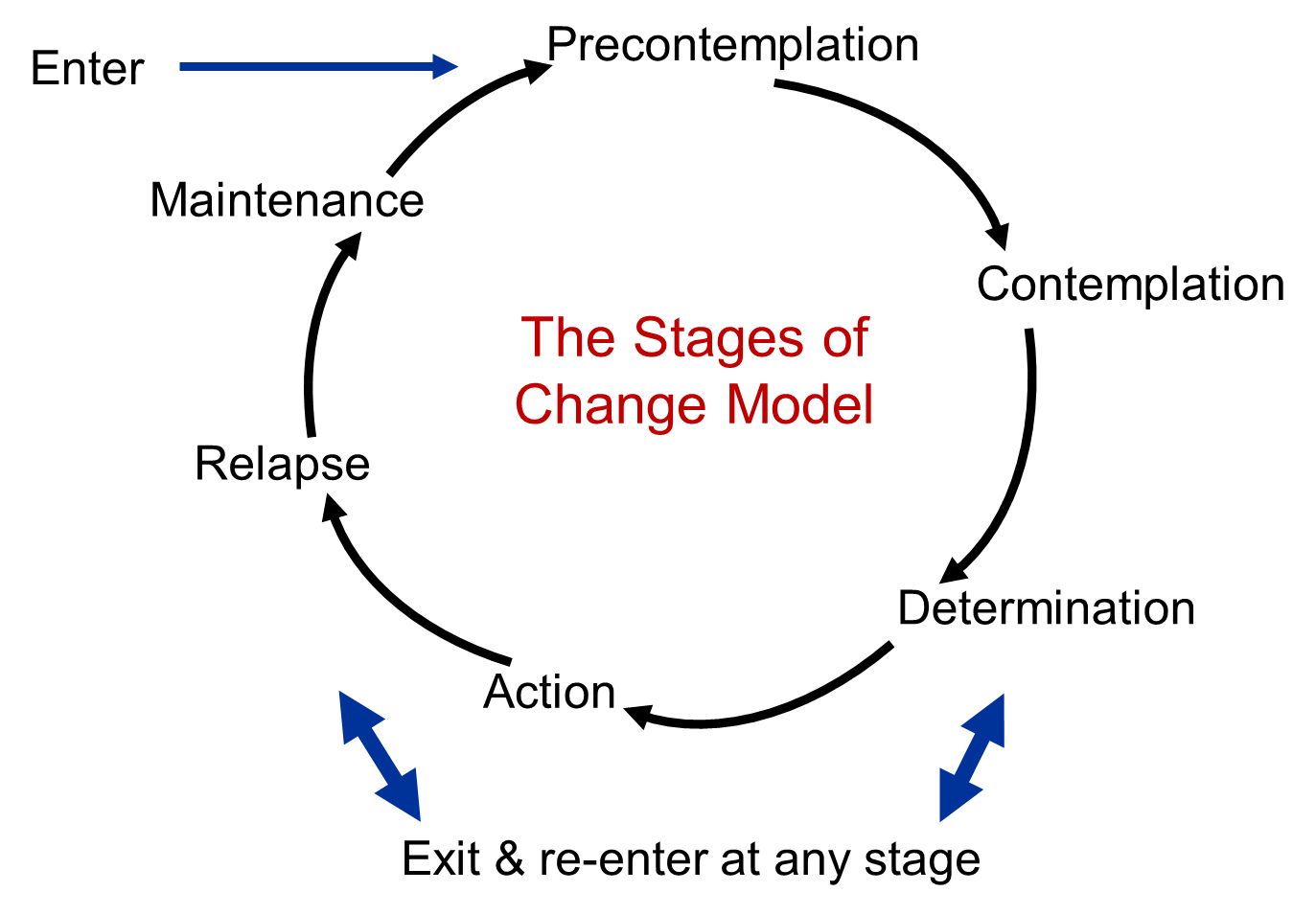
The EMM campaign, run by the NHS in the UK, is an example of how the TMC can be applied to a mental health equality campaign. According to the NHS (2021), the campaign encourages people to take action to look after their mental health and to seek support when needed. The campaign utilizes the TMC to guide individuals through the stages of behavioral change, from pre-contemplation (when people are unaware of the need for change) to action (when people take steps to care for their mental health).
At the precontemplation stage, individuals may be unaware of the need to change and thus be unaware of the EMM. The campaign uses awareness-raising tactics to encourage people to recognize the need for change. This includes providing information about common mental health issues and the benefits of taking action to look after one’s mental health. Contemplation is the next stage, where individuals become aware of the need to change but have not yet committed to making the change. At this stage, the campaign offers guidance and support to help individuals reflect on their thoughts and feelings about taking action to care for their mental health.
In the preparation stage, individuals are ready to take action but may require additional support to take the first steps. Here, the campaign encourages people to plan for change by setting realistic goals and making achievable action plans (Worthington, 2021). This includes guiding, making lifestyle changes, and seeking professional help. In this stage, individuals begin to implement their plans and make changes to their lifestyles.
The action stage follows the preparation stage. Here, the campaign provides ongoing support to help people take action in their mental health care. This includes providing tips and techniques for managing stress, enhancing sleep quality, and increasing physical activity. Maintenance is the stage where individuals are committed to their behavior change and need to find ways to sustain it. At the maintenance stage, the campaign encourages people to continue their good work by staying connected with support networks and seeking help when needed.
The locus of control theory suggests that individuals have either an internal or external locus of control; that is, they either view themselves as being in control of their own lives or view their lives as being subject to forces beyond their control (Reknes et al. 2019). The EMM encourages individuals to take ownership of their mental health and well-being, making it a priority in their lives.
By taking control of their mental health, individuals assume responsibility for their own well-being, which aligns with the internal locus of control theory. This is in contrast to an external locus of control, which suggests that an individual’s mental health is determined by external factors beyond their control (Zangeneh and Al-Krenawi, 2019). By highlighting the importance of taking ownership of one’s mental health, the campaign supports an internal locus of control and encourages individuals to take control of their own well-being.
Compare and Contrast
The EMM is a public mental health campaign developed by Public Health England, the National Health Service (NHS), and the Mental Health Foundation. The evidence base that informed the design and construction of EMM includes research conducted by the Mental Health Foundation, which found that many people lack the necessary information and support to manage their mental health and well-being, and often feel unprepared to do so (Zangeneh and Al-Krenawi, 2019). It was designed to help people take action to look after their mental health and well-being and to provide advice and support to those struggling with their mental health.
The campaign is similar to other mental health campaigns, such as the Heads Together initiative. It was launched by The Royal Foundation of the Duke and Duchess of Cambridge and The Duke and Duchess of Sussex in 2016 (Heads Together, 2018). The Heads Together campaign aimed to end the stigma surrounding mental health and provide people with access to the support they need. Both campaigns offer access to resources, including information leaflets, to help individuals better understand and manage their mental health. However, EMM focuses on providing a more holistic approach to mental health and well-being.
Conclusion
In conclusion, mental illness inequality affects people from all walks of life, hence affecting the state of a nation. Therefore, several considerations have to be put in place to assess the effect of mental health disorders. The considerations include changeability, acceptability, impact, and resource feasibility. The main drive behind such considerations is the broad margin of demographics when mental health issues are considered.
After considering these factors, the next major steps are the placement and implementation of policies and strategies to curb the spread of mental health conditions. The initiatives placed by the United Kingdom include mental health campaigns, strategies, and crisis care concordant. The implementations occur through various individuals, such as Prochaska and DiClemente, utilizing the Transtheoretical Model of Change and campaigns like Every Mind Matters. The combined efforts ensure the effective implementation of mental health strategies, leading to an improvement in the nation’s mental health state.
Recommendations
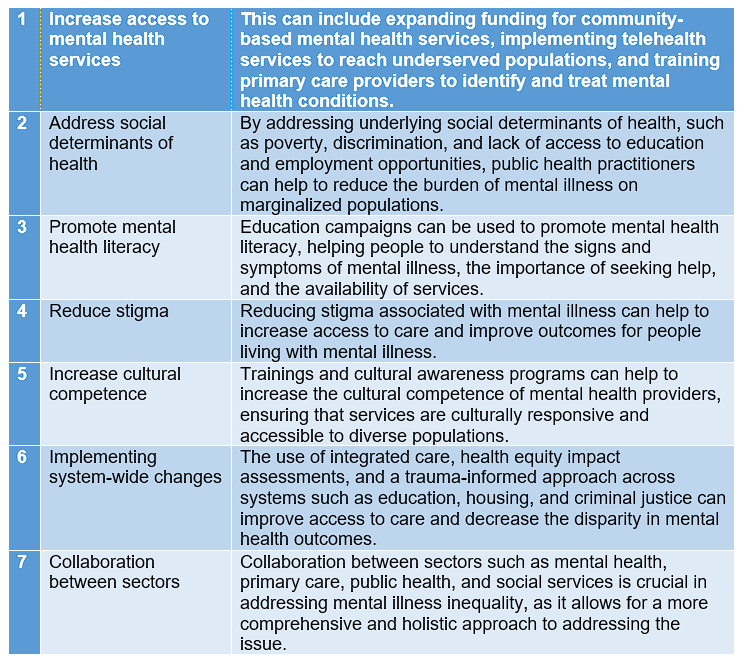
Addressing mental illness inequality requires public health efforts to both increase access to mental health services and resolve relevant social determinants of health. It is additionally critical to focus on promoting mental health literacy, reducing stigma, increasing cultural competence, implementing system-wide changes, and collaboration between sectors.
Some examples of interventions include expanding funding for community-based mental health services, implementing telehealth services, training primary care providers, conducting education campaigns, offering cultural awareness programs, integrating care, and conducting health equity impact assessments. It’s important to note that addressing mental illness inequality is a complex and ongoing process that requires a multifaceted approach and collaboration between sectors. Public health practitioners should work with community-based organizations, policymakers, and other stakeholders to develop and implement effective interventions. Figure 3 below provides a summary of all key recommendations.
Reference List
Campion, J. et al. (2020) ‘Addressing the public mental health challenge of COVID-19’, The Lancet Psychiatry, 7(8), pp. 657–659.
Dahlgren, G., and Whitehead, M. (2021) ‘The Dahlgren-Whitehead model of health determinants: 30 years on and still chasing rainbows’, Public Health, 199(1), pp. 20–24.
Gilbody, S. et al. (2019) ‘Smoking cessation for people with severe mental illness (scimitar+): A pragmatic randomised controlled trial’, The Lancet Psychiatry, 6(5), pp. 379–390.
Glover-Thomas, N. (2013) ‘The Health and Social Care Act 2012’, Medical Law International, 13(4), pp. 279–297.
Hackett, R. A. et al. (2020) ‘Racial discrimination and health: a prospective study of ethnic minorities in the United Kingdom’, BMC Public Health, 20(1), pp. 1-7.
Heads Together. (2018) Heads together | join the conversation | mental health.
Islam, M. M. (2019) ‘Social determinants of health and related inequalities: confusion and implications’, Frontiers in Public Health, 7, pp. 1-11.
Kilbourne, A. M. et al. (2018) ‘Measuring and improving the quality of mental health care: a global perspective’, World Psychiatry, 17(1), pp. 30–38.
Kwong, A. S. F. et al. (2020) ‘Mental health before and during the COVID-19 pandemic in two longitudinal UK population cohorts’, The British Journal of Psychiatry, 218(6), pp. 1–10.
LaMorte, W. (2019) The transtheoretical model (stages of change).
MHFA England. (2020) Mental health statistics.
NHS. (2015) NHS England» Mental Health Taskforce.
NHS. (2021) Every Mind Matters.
NHS. (2022) Mental Health Act.
Office for National Statistics. (2018) Population of England and Wales.
Office for National Statistics. (2022) Ethnic group, England and Wales – Office for National Statistics.
Reknes, I. et al. (2019) ‘Locus of control moderates the relationship between exposure to bullying behaviors and psychological strain’, Frontiers in Psychology, 10, pp. 1323-1325.
Vindegaard, N., and Eriksen Benros, M. (2020) ‘COVID-19 pandemic and mental health consequences: systematic review of the current evidence’, Brain, Behavior, and Immunity, 89(4), pp. 531-542.
Worthington, A. K. (2021) Transtheoretical Model.
Zangeneh, M., and Al-Krenawi, A. (2019) Culture, diversity and mental health – enhancing clinical practice. Heidelberg: Springer.