Public health problems affect groups of people in different thresholds, including neighborhood communities and people within a state. Public health nursing field has a role to play in the management of such problems. The field concentrates on the health wellness of populations, as opposed to focusing on health outcomes for individual groups. Mental illness is one of such problems. Although all population segments are vulnerable to mental illness, this paper restricts its discussion on the link between homeless people in the United States and mental illness. Homelessness is a significant problem that affects people’s health in different proportions in various parts of the world. Due to their socio-economic status, homeless people in the US are vulnerable to health problems, including mental illness, compared to people drawn from high socio-economic status.
In other words, many homeless persons tend to belong to low socio-economic families (Johnson & Haigh, 2012). Ensuring good mental health for such persons calls for the creation of a means of accessing quality health care for all people within a nation. However, mentally ill people experience problems of accessing such care, especially those who are homeless due to lack of financial resources or the presence of physical barriers. Hence, there is a need to establish elaborate policies for addressing the problem of mental illness among homeless people in all regions in the US. This paper establishes a plan of policies for addressing the public health problems of mentally ill homeless people. However, it first offers a description of the problem statistically and in terms of how it relates to the goals of Healthy People 2020. It then provides an in-depth analysis of the problem before proposing potential policy interventions.
Description of the Identified Problem
People experience the problem of homelessness when they do not have places to live in with peace, dignity, and good security. People who are considered homelessness include those who sleep in vehicles, those living with their friends in temporary shelters, refugees, and those who live in houses that do not have tenure security. The nature of the problem of homelessness depends on the adopted definition. Indeed, all persons who cannot access regular, enough, and fixed residence are legislatively considered homeless in the United States. They also include people who sleep in private or public places that were not designated for occupation by people during their design. All persons who live in temporary accommodation facilities awaiting institutionalization are also considered homeless in the US.
Pearson and Linz (2011) establish a link between mental health and homelessness, arguing that people who experience mental illnesses and lack of psychosocial support face a high risk of homelessness. They claim that by linking all persons with mental illness to legal services, substance abuse, and housing, medical practitioners help in preventing the problem of mental illness among homeless Americans. Pearson and Linz’s (2011) arguments indicate that resolving the problem of homelessness can help to alleviate or minimize the public health problem of mental illness. However, a further argument on this possibility requires an understanding of the statistics concerning the prevalence of homelessness and mental illness in the US.
Statistics
Statistical findings derived from the Annual Homeless Assessment Report (AHAR) to Congress (2016) show that about 23,000 persons sleep in emergency accommodations every night. Important to note is that these figures are exclusive of persons termed in England as ‘hidden’ homeless persons. The term covers persons, single people, or families, which live with other relatives or friends. Consequently, it sounds plausible to infer that the problem of homelessness is not only a key public health challenge in developing nations but also in the developed ones such as the US.
In a social study, acquiring 100% accurate data is incredibly challenging. Hence, the available data is only based on estimates. The approximations are mainly based on national averages. However, community estimates may considerably vary with respect to local geographies. However, the Annual Homeless Assessment Report (AHAR) to Congress (2016) provides the most accurate statistics on the state of homelessness in the US. It issues an annual homeless assessment report to the US Congress. The data shows that almost 550,000 US citizens were homeless as of January 2016 (The Annual Homeless Assessment Report (AHAR) to Congress, 2016). The other source entails counts of homeless and sheltered persons in the course of the year as extracted from community samples. Such data is extracted from HMIS of the communities. Therefore, the data shown in Figure 1 below is based on a close comparison of the information from the national and community statistics.
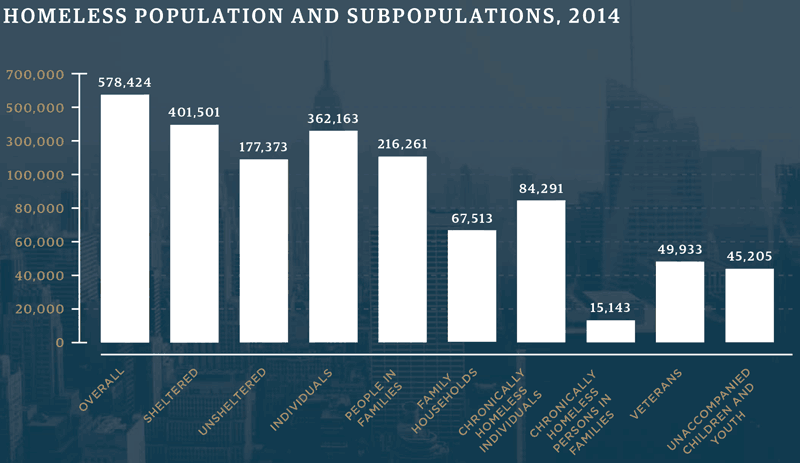
Statistical findings of homeless people in the US vary according to familial composition, marital status, ethnicity, substance abuse, education levels, mental health, and employment status among other demographic characteristics such as geography and duration. NAMI (2017) paints a dismaying picture of mental illness preference rates in the United States. The organization notes that about 43.8 million or 18.5% of Americans report cases of mental illness every year. About 9.8 million of such people have serious mental illnesses, which impair with their life activities (NAMI, 2017). Indeed, the organization continues to inform that in about 20.2 million people in the US experiencing disorders associated with substance abuse, half of them have the problem of mental illness. In terms of social statistics in line with the primary interest to the current paper, NAMI (2017) posits, “An estimated 26% of homeless adults staying in shelters live with serious mental illness and an estimated 46% live with severe mental illness and/or substance use disorders” (para.8). This segment forms the focus of discussion in the subsequent sections of the paper.
Relevance of the Problem
Nations measure their population’s health. For example, Healthy People 2020 assesses the general health of the population of the United States of America. It monitors life expectancy of the US citizens compared to other nations in an international context, healthy lives expectancy, YPLL (years of potential life lost), and the prevalence of unremitting ailments among other indicators (Healthy People 2020, 2013, para.2). To this extent, the problem of mental illness relates to the goal of Healthy People 2020. By managing it through interventions that seek to address risk factors such as homelessness, it becomes possible to achieve the desired outcomes, for instance, the reduction of YPLL. A reduced problem of mental illness increases the number of productive years lived, since the public health problem affects people’s capacity to execute their daily activities more productively.
The problem of mental illness and homelessness is not only important in the context of the United States, but also in the global domain. In support of this assertion, Mental Health Network (2012) estimates that about 100 million people encounter challenges of being homeless after finding themselves living in vehicles, shelters, and parks (p. 1). This observation shows that on the global scale, the challenge of homelessness has critical effects on the quality of life lived. Its implications on public health are also an issue that attracts global public health interest. Such global interest has led to the initiation and successful completion of studies on emergency medical care facilities, shelters, and even life in the streets. Such studies are aimed at determining the traits of homeless populations, including their health conditions. Such effort establishes the need for the participation of public health nurses in providing solutions to mental illness in the US. This role stems from the need to understand the best care interventions relevant to particular traits of homeless people.
Researchers such as Cockersell (2011) indicate that many people from varied backgrounds, for instance, elderly, needy persons, children, youths, and immigrants among other classes of people, have tendencies of becoming homeless in the event that they are unable to meet their daily needs. These scholarly findings are astounding since they reveal the issue of homelessness as a key indicator of people’s health status. Indeed, homelessness directly correlates with chronic illnesses such as respiratory infections, heart failure, cardiovascular ailments, and physical health challenges, including accidents (Mental Health Network, 2012). Additionally, mental health challenges have also been found to be a key trait of persons living in the streets where one the groups of persons here is classified as homeless (Cockersell, 2011).
In the contest of Minnesota, the problem is relevant. Indeed, data from “Mental illness linked to homeless in Minnesota” (2016) reveals, “60% of homeless adults in Minnesota report having a serious mental illness while 51 percent have a chronic health condition” (para.1). This finding indicates a high prevalence of mental illness among homeless adults in Minnesota compared to any other health condition such as asthma, diabetes, or hypertension. Recognition of the prevalence of mental illness among homeless people has prompted the development and implementation of various public health projects to address the problem.
Public Health Projects
Hospitalization and the treatment of mental illness affect the wider community in terms of care costs, accessibility to care providers, and the cost of insurance. Since public nursing is concerned about health conditions that affect communities, it suggests that public nursing has a role to play in overcoming or in the management of mental illness among homeless people in Minnesota. Public health nurses can work in collaboration with state agencies to provide evidence-based care to people placed on housing programs as one of the initiatives to counter homelessness, which is a major risk factor for mental illness in Minnesota. One of such programs entails Healthy People 2020, which aims at increasing the health outcomes of all people living the United States. At the state level, the state of Minnesota’s Department of Health has a clear goal of improving and ensuring wellness and positive health outcomes for all citizens, including homeless mentally ill people.
In dealing with the challenges of homelessness, Healthy People 2020 targets increasing accessibility to quality healthcare for homeless people living with mental illness. Its target is 41% by 2020 (Healthy People 2020, 2016, p.229). This target was based on 2006 baseline study in which 37% of the target population accessed healthcare. The objective uses 10% improvement. Healthy People 2020 has endeavored to achieve this objective, although hindrances such as new cases of mentally ill people becoming homelessness persist. However, by 2020, this objective is achievable or may even be surpassed.
Different federal and state policies have been established to deal with homelessness. For example, the state of New York’s policies, for instance, Permanent Supportive Housing and Housing First, have proven very effective in ending homelessness. In addition, the US has federal housing programs that include federal housing assistance. Two major programs under this category are housing vultures and public housing schemes. The programs have proven effective in providing stable housing to the homeless population segments in the US. However, there remain scholarly differences in the debate concerning the effectiveness of the programs, especially in addressing the problem of mental illness associated with homelessness.
One of the greatest initiatives by the US is to eliminate inequalities in the accessibility of quality mental health care through advocating for affordable care to all people, despite their demographic differences. For example, the US Affordable Care Act purposes to guarantee equal accessibility of quality health care among all US citizens, irrespective of their racial backgrounds or their nature of disabilities. Obamacare Facts (2012) posits, “Obamacare ensures that sick people cannot be dropped from insurance, they cannot be denied health care for any pre-existing conditions, and that women cannot be charged more than men by insurance companies” (para.5). This effort guarantees no discrimination among all citizens of the United States with respect to their accessibility to quality healthcare. Therefore, through the policy initiative, homeless Americans who are facing challenges in accessing quality mental health care because of their low socio-economic status stand to gain immensely. The lingering question revolves around the effectiveness of the programs in addressing homelessness in the effort to guarantee positive health outcomes and wellness. The next section addresses this question coupled with the role of public health nurses in implementing the programs.
Analysis of the Problem
The problem description section indicated that in different states, including Minnesota, homelessness is an incredible risk factor to mental illness. Therefore, by putting in place programs for addressing the problem, public health nurses can work in collaboration with such program implementers in the delivery of mental illness care to foster positive mental health outcomes in homeless communities. However, before considering the effectiveness of homeless intervention programs, it is important to address the anatomy of the problem of homelessness using the web of causation as the epidemiological model.
Web of Causation
As shown in Appendix 1, homelessness can result from structural causes such as poverty, lack of sufficient supply of affordable housing and unemployment challenges that continue to ruin many nations around the globe (Hafetz, 2009). Other causes include public and social policy problems, for instance, community and public housing policies, education, and expenditure without negating taxation policies. Health challenges associated with homelessness also include ill health, the fragmentation of families, intellectual disability, domestic violence, and alcohol or drugs dependency-associated problems such as mental illness among others. Department for Communities and Local Government (2012) reveals how poor health can cause poverty and hence homelessness. For instance, poor health can have impacts on an individual’s ability to engage in productive employment or education, which is an important aspect in the alleviation of poverty. Poor health can also cause people to sacrifice necessities, including housing, to meet various medical care and treatment costs. From the paradigm of public health in general, poverty has immense negative impacts.
Approaches to Address Homelessness and Mental Illness and their Effectiveness
An understanding of various causations of homelessness underlines the need to develop and implement effective programs aimed at reducing the problem by proactively addressing its related health risks such as mental illness. Indeed, the question of the effectiveness of the programs for reducing homelessness, including housing schemes, has been the subject of research in the United States and elsewhere across the world. Castellow, Kloos, and Townley (2015) report that the experiences of homelessness coupled with the time spent while living as a destitute person have a bearing on the victim’s psychological distress, incidences of use of alcohol and substance abuse, and a decreased probability of recovery from mental illness. The study indicated that homelessness was a factor that contributed to psychological vulnerability to experiencing negative mental health. Consequently, housing programs can help in the alleviation of homelessness-associated traumatic experiences that lead to poor mental health outcomes.
Benston (2015) conducted a systematic review study with the objective of analyzing the best available research in the United States concerning permanent supportive housing programs for homeless individuals with mental illness and the effect of the programs on housing status and mental health. The research identified a weakness where studies have failed to analyze the effects of permanent housing as an important input to mental illness and homelessness. For example, for the 14 reviewed articles, only three reported using a housing fidelity assessment tool to test whether the housing intervention was in line with the established theoretical standards. Besides, the conceptions and implementation of housing varied widely across studies, thus threatening internal and external validity. The researchers concluded that existing gaps in studies on permanent housing program coupled with housing suggested the inability of the research to help in informing housing policy programs to guarantee best outcomes in the alleviation of the problem together with its associated risks such as mental illness.
Vet et al. (2013) conducted a systematic review of the effectiveness of case management for homeless people. They reviewed literature on standard case management (SCM), intensive case management (ICM), assertive community treatment (ACT), and critical time intervention (CTI) for homeless adults. The study found little evidence concerning the effectiveness of ICM. However, the researchers concluded that SCM helped to improve housing stability, reduce substance abuse, and/or eliminate barriers to employment associated with substance use. They also found ACT as having the capacity to improve housing stability. It was also cost-effective for mentally ill persons. Consistent with these findings on the effectiveness of homelessness programs, Page, Petrovich, and Kang (2012) reckon that destitute persons would benefit from inclusion in CMHC social support networks, psychosocial rehabilitation programs, and assistance with re-connecting with natural support systems, some of which may have been terminated throughout the course of the individuals.
Mental Health and Homelessness Reduction Plan
Studies have been conducted in different nations around the globe to unveil various health problems that are associated with homelessness. Indeed, mental health is one of the most significant problems. Mental Health Network (2012) posits that more than 70 percent of all persons in the US who seek homelessness services experience mental health challenges. About 64 percent of these groups of people have problems associated with excessive consumption of substances. Hence, the abuse of substances is a major contributing factor to poor mental health. Hence, it is a major driver of the mental public heath challenge facing many nations.
Mental Health Network (2012) also reveals a myriad of causes of homelessness, although it singles out mental health as one of the major contributing factors. For persons having mental health problems, once an individual becomes homeless, chances are that the psychological health issue may become worse. Consequently, any mental health and homelessness reduction plan should also address the underlying implication of homelessness that leads to poor mental health. The plan is developed to be implemented in Minnesota in the US. Consider a scenario where Morgan and Joyce are homeless and mentally ill citizens living in Minnesota. The two are also involved in drug and substance abuse, owing to lack of attention and guidance from a knowledgeable person or relative concerning the underlying dangers of drug consumption. Mike and Joe are public nurses who are tasked with addressing the issues faced by Morgan and Joyce.
Primary goal
Reduce progression to serious mental illness between Morgan, Joyce, and other similar people living in Hennepin County, Minnesota by 7% by the end of 2018.
Objective 1: Reducing Substance Abuse
Reducing substance abuse requires Mike and Joe to design and implement an appropriate intervention program. Intervention programs are developed in accordance with the appropriate epidemiological, social, and environmental assessments concerning Morgan and Joyce. Epidemiological assessment takes analytical and descriptive forms (Needle et al., 2011). In Hennepin County, Minnesota, Mike and Joe can develop and implement “You Can Quit Substance Abuse Program” alongside housing programs developed by the state agencies. The programs will deploy a descriptive approach to epidemiology. Descriptive epidemiology entails the assessment of the occurrence of health challenges in the context of time, place, and a specific group of people. The “You Can Quit Substance Abuse Program” will focus on 18 and above-year-old people in Hennepin County, Minnesota. Through social and environmental assessments, it becomes possible for the public nurses to develop health-related problem intervention program to solve specific health problems affecting the communities. In the context of the “You Can Quit Substance Abuse Program”, the focus will be on the quality of life among homeless mentally ill people in target geographical region.
Objective 2: Increasing Accessibility to Mental Healthcare
Increasing accessibility to mental health care calls for Mike and Joe to proactively advocate for inclusive care delivery. For example, public health nursing fraternity can call an action to ensure “no health without mental health”, especially among the venerable groups such as the homeless. Such policy can help in the establishment of guidelines for improving the general population’s mental health by guaranteeing accessibility to quality psychological care by all Minnesota people (Shelley, Ghinwa, Ray, & Fridkin, 2015). This way, Mike and Joe will steer the development of holistic approaches to addressing the problem of inequality among mentally ill by asserting that quality mental health care by all people entails every Minnesota citizen’s business. Under such policy framework, prevention is the preferred approach to addressing the prevalence of mental health illnesses among the homeless population segments. It suggests the need to address the underlying risk factors of homelessness. Through the initiative, by 2018, it will be possible to have achieved true parity in terms of the access to evidence-based medical treatment for mental illnesses for all homeless people living in Minnesota, including Morgan and Joyce.
Objective 3: Participating in Mental Health Leadership
Mike and Joe will participate in healthcare leadership. Working in this capacity, nurses have the responsibility of developing and implementing various evidence-based health care programs while at the same time participating in resolving sophisticated healthcare-related issues. Advanced roles of public health nurses involve providing directions on policies, developing standards, and evaluating the outcomes of health promotion and care management initiatives. Consistent with this objective, as Patterson and Nochajski (2010) argue, the public health nurses will engage in the development of a health promotion program or any other mechanism for addressing any challenging health risk factor. These initiatives precede the improvement of the strategies and procedures for evaluating its effectiveness in terms of resolving mental health challenges among homeless people in Hennepin County, Minnesota such as Morgan and Joyce.
Summary and Conclusion
Homelessness is a major challenge facing nations, including those in the developed world, for instance, the US. The paper argued that homelessness forms an incredible issue in public health discourses since it is associated with health problems, including mental illness, behavioral problems such as alcoholism, crime and substance abuse, and chronic ailments. Nevertheless, amid these problems, many states such as Minnesota have statistics indicating high rates of persons living under conditions that pose threat to their lives. Such conditions include sleeping in rough places, in vehicles, squats, and even in temporary and poorly hygienic forms of accommodation. Faced with the problem of homelessness and mental illness, public health nursing has the responsibility of enacting programs that can be implemented alongside state agency-initiated housing programs. This way, public health nurses participate in improving health outcomes in homeless communities living with mental illness.
References
Benston, E. (2015). Housing programs for homeless individuals with mental illness: Effects on housing and mental health outcomes. Psychiatric Services, 66(8), 806-816.
Castellow, J., Kloos, B., & Townley, G. (2015). Previous homelessness as a risk factor for recovery from serious mental illnesses. Community Mental Health Journal, 51(6), 674-84.
Cockersell, N. (2011). Homelessness and mental health: Adding clinical mental health interventions to existing social ones can greatly enhance positive outcomes. Journal of Public Mental Health, 10(2), 9–98.
Department for Communities and Local Government. (2012). Rough sleeping statistics England – Autumn 2011 experimental statistics. London, England: Department for Communities and Local Government.
Hafetz, J. (2009). Homeless legal advocacy: New challenges and directions for the future. Fordham Urban Law Journal, 12(5), 1222-1229.
Healthy People 2020. (2013). Objective topic areas and page numbers. Web.
Healthy People 2020. (2016). General health status. Web.
Johnson, R., & Haigh, R. (2012). Social psychiatry and social policy for the twenty-first century – new concepts for new needs: The ‘psychologically informed environment. Mental Health and Social Inclusion, 14(4), 30–35.
Mental Health Network. (2012). Mental health and homelessness: Planning and delivering mental health services for homeless people. Web.
Mental illness linked to homeless in Minnesota. (2016). Web.
NAMI. (2017). Mental health by the numbers: Prevalence of mental illness.Web.
National Alliance to End Homelessness. (2015). The state of homelessness in America. Web.
Needle, J., Petchey, P., Benson, J., Scriven, A., Lawrenson, J., & Hilari, K. (2011). The role of allied health professionals in health promotion. London, England: NIHR Service Delivery and Organization Program.
Obamacare Facts. (2012).Facts on Obama health care plan. Web.
Page, J., Petrovich, J., & Kang, S. (2012). Characteristics of homeless adults with serious mental illnesses served by three street-level federally funded homelessness programs. Community Mental Health Journal, 486(1), 699-704.
Patterson, A., & Nochajski, H. (2010). Using the stages of change model to help clients through the 12-steps of alcoholics anonymous. Journal of Social Work Practice in the Addictions, 10(2), 224-227.
Pearson, S., & Linz, S. (2011). Linking homelessness with mental illness. Perspectives in Psychiatric Care, 47(4), 165-166.
Shelley, M., Ghinwa, D., Ray, S., & Fridkin, S. (2015). Evaluating and improving surveillance of infections associated with health care, United States. Emerging Infectious Diseases, 21(9), 1537-1542.
The Annual Homeless Assessment Report (AHAR) to Congress. (2016). Point-in-time estimates of homelessness. Web.
Vet, R., van Luijtelaar, M., Brilleslijper-Kater, S., Vanderplasschen, W., Beijersbergen, M., & Wolf, J. (2013). Effectiveness of case management for homeless persons: A systematic review. American Journal of Public Health, 103(10), 13-26.