Introduction
Acute Myocardial Infarction (AMI) is a deadly medical emergency that has claimed the lives of many citizens in the UK. According to the British Heart Foundation (2022) statistics, approximately 7.6 million people are affected by coronary heart disease, with 168,000 mortality cases reported annually.
Blockage of the heart’s arteries deprives the muscles of oxygen and nutrients, causing AMI (Saleh and Ambrose, 2018). This factor results from the death of cells, which can lead to a heart attack (Alun and Murphy, 2019). The common presenting symptoms include chest pressure, sweating, nausea, shortness of breath, and joint pains (Ojha and Dhamoon, 2021). Therefore, this paper addresses the nursing care and management of a patient with AMI by following the case of Jamie to assess the efficacy of the interventions used and provides recommendations for future nursing care.
Current Health Status
Apart from the symptoms, the patient was alert and responsive to all questions. On the other hand, he appeared weak and uncomfortable talking about marital and employment status issues. His blood pressure was 140/80mmHg, with a pulse of 92 beats per minute (Chioncel et al., 2020). The body temperature was 38°C above optimal (Pamukçu, 2019). The vital signs necessitated an emergency response, considering that the attack was in its acute stages.
Nursing Evaluation
Jamie is a 65-year-old male divorcee with three adult children. Jamie has a medical history of hypertension, diabetes, and anemia. The patient’s primary complaints included chest pain on the left side lasting over 24 hours, persistent nausea for two days, sweating, shortness of breath with any physical activity, and sometimes occurring without cause. Jamie also reported that he has been vomiting for the past two days and feeling lethargic.
The patient’s past medical history indicated that he was diagnosed with anemia and had undergone a blood transfusion of about four pints. He was also diagnosed with type II diabetes 10 months ago. This health history indicates that the client could have had a heart attack, and this necessitated an Emergency.
Family History
The patient’s family history is that the Parents suffered from cardiac issues, including a fatal stroke and heart attack. His mother succumbed to a heart arrhythmia at age 68, while his father died of myocardial infarction after ongoing colon cancer treatment at 72 years of age. Jamie’s social history includes his recent divorce two years ago, which contributed to a sedentary lifestyle due to a lack of motivation to exercise. He is a retired military officer who was active in his role. Currently, the patient weighs 89 kg and is an active smoker. Additionally, he drinks alcohol on special occasions, which has contributed to many complications.
Assessment of Findings
The pathophysiology of MI is complex and involves some interconnected processes. It begins with an initial insult, such as plaque rupture in a coronary artery that causes the blockage of blood flow to the heart muscle (Curtis et al., 2021). This lack of oxygen to the heart muscle leads to an energy crisis, causing an excessive release of calcium ions into the cell, which damages the cell membrane and leads to cell death (Rossello, Lobo-Gonzalez, and Ibanez, 2019). In addition, the lack of oxygen causes an increase in the production of free radicals within the cell, leading to further damage to the cell membrane and ultimately cell death.
The death of the cells in the affected area of the heart muscle leads to inflammation, which can cause further damage to the muscle and weaken the heart’s ability to pump blood. Additionally, the damaged muscle can form scar tissue, which is less effective than healthy muscle tissue at pumping blood (Rossello, Lobo-Gonzalez, and Ibanez, 2019). As a result, the heart muscle becomes weaker and less able to pump as much blood as before (Chadwick et al., 2019). An insufficient oxygen supply results in fatigue, sweating, joint pain, shortness of breath, and nausea.
Critical Analysis of Prioritized Nursing Care Interventions
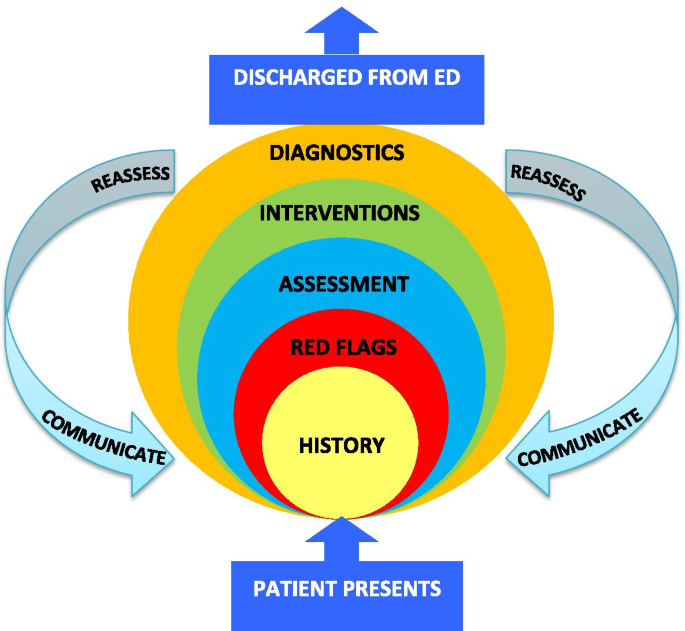
The nursing framework used in this emergency was the structured framework. This model employs a systematic approach that follows a methodological system, enabling nurses to provide comprehensive care for patients with high-risk diseases (Aranda Hernandez et al., 2023). The steps described in Figure 1 illustrate the nursing roles in each of the crucial stages of successful recovery, such as taking the patient’s information and medical history immediately after they arrive at the hospital, and the information is to be disseminated among authorized individuals to facilitate care (Goedemans, Bax, and Delgado, 2020). The second phase is identifying potential threats, whereby the nurse must ensure that any life-threatening conditions, such as loss of consciousness, are addressed by immediate referral to the ER or other integrative medical approach.

Physicians play an integral role in facilitating the nurse’s responsibility, as they can prescribe the necessary medications and care after diagnosis to ensure the patient receives adequate treatment. For instance, administering the IV line was the nurse’s responsibility alongside other roles, such as administering aspirin and pain medications (Aranda Hernandez et al., 2023). The final step is the provision of aftercare services, which include communicating with the patient to elaborate on their progress and provide recommendations on the best lifestyle habits.
Prioritized Nursing Care Interventions
Jamie was admitted to the hospital at 18:00 with an acute myocardial infarction (MI). Jamie first presented to the Emergency Department (ED) with chest pain, nausea, diaphoresis, profuse sweating, and vomiting (Konijnenberg et al., 2020). Upon arrival, the necessary clinical information and tests were conducted, and then the ED team initiated a 12-lead ECG.
This test revealed ST elevations in V1-4 and ST depressions in leads II, III, and aVF. These findings were highly suggestive of an AMI (Aranda Hernandez et al., 2023). At about 18:30, Jamie was given 180 mg of aspirin, clopidogrel, and a sublingual nitroglycerin tablet to relieve the pain (Kloner, 2021). He was then transferred to the coronary care unit (CCU) for further management.
The patient was admitted to the CCU at around 20:00 and was put on oxygen via nasal cannula. An intravenous (IV) line was placed for fluid resuscitation and administration of medications. His vital signs were monitored continuously, and a 12-lead Electrocardiographic (ECG) analysis was done, which showed ST elevation in leads V1, V2, and V3, consistent with an ST elevation myocardial infarction (STEMI), confirming the previous diagnosis. Jamie was immediately started on aspirin and clopidogrel orally.
He was also given a sublingual nitroglycerin for chest pain relief, and a heparin infusion was started (Aranda Hernandez et al., 2023). The ECG was repeated and showed resolution of ST-segment elevation in leads V1, V2, and V3, refuting all doubt of error (Maroules et al., 2022). He was then monitored for improvement and reaction to the medication for the next critical hours.
The next day, Jamie was moved to the cardiac catheterization laboratory (CCL), where an angiogram was done. The angiogram revealed an occlusion of the left anterior descending (LAD) artery (Chioncel et al., 2020). A percutaneous coronary intervention (PCI) was performed, and the LAD artery was stented (Kadesjö et al., 2019). The nurses closely monitored his vital signs, and an echocardiogram was done to assess his left ventricular function (Mughal and Sastry, 2022). Results showed an ejection fraction of 0.50 and evidence of acute myocardial infarction.
His ECG revealed ST-segment elevation in leads II, III, and aVF. Jamie was admitted to the coronary care unit and started on an intravenous (IV) infusion of nitroglycerin and morphine for pain relief. His heart rate and blood pressure were continually monitored (Musher, Abers, and Corrales-Medina, 2019). An echocardiogram was repeated on the second day and showed an ejection fraction of 29%, indicating moderate to severe left ventricular dysfunction (Mafham et al., 2020).
His fluid balance was maintained with IV fluids, and his electrolytes were monitored closely. Nurses administered the prescribed medications within the first hour, including the pain relievers. Jamie was monitored for complications for three hours after all the medical interventions were completed and throughout his stay in the ER. Therefore, the care provided at this stage was error-free, and no omissions were noted after the patient was transferred to the recovery unit.
Despite the systematic approach used, numerous errors were identified in the system, including poor communication, which delayed processes. Inadequate communication with the patient’s primary care physician or cardiologist resulted in improper management of medications, inadequate use of follow-up imaging studies, and limited access to laboratory results (Shah, Puri, and Kalra, 2019). These errors delayed processes, as the team had to wait longer for them to be completed (Konijnenberg et al., 2020).
For instance, after the patient left the ER, a complete summary of health was still unavailable; this was integral in the psychoeducation of the patient and their family. This delay resulted in a general description of the client’s progress, which should not have been the case. Therefore, the care provided to Jamie was moderately excellent; however, there is still room for improvement, particularly in record-keeping, communication, and collaboration among clinical experts.
Factors That Impacted the Type of Care
The patient was subjected to a 12-lead ECG, which is integral in diagnosing a myocardial infarction, considering that it determines the cardiac rhythm of a patient to determine the severity of their attack. The ECG was necessary for proper diagnosis, considering the patient was still conscious and without cardiac arrest (Shah, Puri, and Kalra, 2019). Another necessary intervention was the administration of pain medication and blood thinners (Mechanic et al., 2021). Aspirin is vital since it helps avoid blood clots, which are an integral trigger for a heart attack. This drug was administered as soon as the patient arrived, which was integral considering that it prevented clotting and reduced the risk of hemorrhagic stroke.
The patient was also given heparin in the coronary care unit, considering they had a history of diabetes and smoking. The reason is that heparin reduces complications in AMI, especially in patients with high cholesterol due to high-risk factors contributed by the underlying issues (Maroules et al., 2022). During this time, nurses were on high alert due to the constant monitoring needed.
Afterward, the patient underwent a coronary angiogram procedure, which is necessary for acute heart attacks, since it enabled the experts to identify any blockages in the heart that triggered the disease (Mughal and Sastry, 2022). The scan revealed that his left ventricle had a defect due to a lack of sufficient blood flow, and this necessitated a revascularization. This systematic approach indicated a carefully choreographed care system.
Main Learning Points and Recommendations
My learning points are influenced by the HIRAD nursing framework, which provides a guideline for effective nursing management. First, nurses should understand how to spot the signs of an AMI. Symptoms may include fatigue, sweating, nausea, and shortness of breath. When a nurse notices a change in these symptoms, she should notify the doctor immediately (Ortíz-Barrios and Alfaro-Saíz, 2020). Furthermore, the nurse must be aware of risk factors for myocardial infarction, such as hypertension, diabetes, and tobacco use.
There is a need for nurses to be well-versed in the many MI treatments currently in use. Medicines like ACE inhibitors, beta-blockers, and anticoagulants fall within this category (Curtis et al., 2021). Moreover, changes in nutrition, exercise, and stress management can reduce the likelihood of a heart attack. Additionally, nurses should be able to instruct patients on recognizing the warning signs of a heart attack and what to do in the event of a heart attack emergency.
Conclusion
Nursing care for myocardial infarction patients is essential for successful recovery and prevention of further health complications. Nurses play an important role in monitoring, diagnosing, and treating patients, as well as providing education and support to patients and their families. To provide the best possible care, nurses must stay up to date on current evidence-based practices and research, while also being aware of their patients’ unique needs. Myocardial infarction patients need a comprehensive nursing care plan that includes diet and lifestyle modifications, medications, regular monitoring of vital signs, and physical activity.
Reference List
Alun, J. and Murphy, B. (2019). Loneliness, social isolation and cardiovascular risk. British Journal of Cardiac Nursing, 14(10), pp.1–8.
Aranda Hernandez, A., Bonizzi, P., Peeters, R. and Karel, J. (2023). Continuous monitoring of acute myocardial infarction with a 3-Lead ECG system. Biomedical Signal Processing and Control, 79, p.104041.
British Heart Foundation (2022). Heart and Circulatory Diseases (Cardiovascular Disease; CVD). British Heart Foundation, England: UK Factsheet, p.21.
Chadwick, J., Davatyan, K., Subramanian and Priya, J. (2019). Epidemiology of Myocardial Infarction. In: B. Pamukçu, ed., Myocardial Infarction. Intechopen, p.138.
Chioncel, O., Parissis, J., Mebazaa, A., Thiele, H., Desch, S., Bauersachs, J., Harjola, V., Antohi, E., Arrigo, M., Gal, T.B., Celutkiene, J., Collins, S.P., DeBacker, D., Iliescu, V.A., Jankowska, E., Jaarsma, T., Keramida, K., Lainscak, M., Lund, L.H. and Lyon, A.R. (2020). Epidemiology, pathophysiology and contemporary management of cardiogenic shock – a position statement from the Heart Failure Association of the European Society of Cardiology. European Journal of Heart Failure, 22(8).
Curtis, K., Sivabalan, P., Bedford, D.S., Considine, J., D’Amato, A., Shepherd, N., Fry, M., Munroe, B. and Shaban, R.Z. (2021). Implementation of a structured emergency nursing framework results in significant cost benefit. BMC Health Services Research, 21(1).
Goedemans, L., Bax, J.J. and Delgado, V. (2020). COPD and acute myocardial infarction. European Respiratory Review, 29(156).
Kadesjö, E., Roos, A., Siddiqui, A., Desta, L., Lundbäck, M. and Holzmann, M.J. (2019). Acute versus chronic myocardial injury and long-term outcomes. Heart, 105(24), pp.1905–1912.
Konijnenberg, L.S.F., Damman, P., Duncker, D.J., Kloner, R.A., Nijveldt, R., van Geuns, R.-J.M., Berry, C., Riksen, N.P., Escaned, J. and van Royen, N. (2020). Pathophysiology and diagnosis of coronary microvascular dysfunction in ST-elevation myocardial infarction. Cardiovascular Research, [online] 116(4), pp.787–805.
Kloner, R.A. (2021) Treating acute myocardial infarctions with anti-inflammatory agents. Journal of Cardiovascular Pharmacology and Therapeutics, 26(6), pp.736-738.
Mechanic, O.J., Gavin, M., Grossman, S.A. and Ziegler, K., 2021. Acute myocardial infarction.
Maroules, C.D., Rybicki, F.J., Ghoshhajra, B.B., Batlle, J.C., Branch, K., Chinnaiyan, K., Hamilton-Craig, C., Hoffmann, U., Litt, H., Meyersohn, N., Shaw, L.J., Villines, T.C. and Cury, R.C. (2022). 2022 use of coronary computed tomographic angiography for patients presenting with acute chest pain to the emergency department: An expert consensus document of the Society of cardiovascular computed tomography (SCCT). Journal of Cardiovascular Computed Tomography.
Mafham, M.M., Spata, E., Goldacre, R., Gair, D., Curnow, P., Bray, M., Hollings, S., Roebuck, C., Gale, C.P., Mamas, M.A., Deanfield, J.E., Belder, M.A. de, Luescher, T.F., Denwood, T., Landray, M.J., Emberson, J.R., Collins, R., Morris, E.J.A., Casadei, B. and Baigent, C. (2020). COVID-19 pandemic and admission rates for and management of acute coronary syndromes in England. The Lancet, 396(10248), pp.381–389.
Mughal, L.H. and Sastry, S. (2022). Advances in the treatment of ST Elevation Myocardial Infarction in the UK. JRSM Cardiovascular Disease, 11, p.204800402210755.
Musher, D.M., Abers, M.S. and Corrales-Medina, V.F. (2019). Acute Infection and Myocardial Infarction. New England Journal of Medicine, 380(2), pp.171–176.
Ojha, N. and Dhamoon, A.S. (2019). Myocardial infarction. Nih.gov.
Ortíz -Barrios, M.A. and Alfaro-Saíz, J.-J. (2020). Methodological Approaches to Support Process Improvement in Emergency Departments: A Systematic Review. International Journal of Environmental Research and Public Health, 17(8).
Rossello, X., Lobo-Gonzalez, M. and Ibanez, B. (2019). Editor’s Choice- Pathophysiology and therapy of myocardial ischaemia/reperfusion syndrome. European Heart Journal: Acute Cardiovascular Care, 8(5), pp.443–456.
Saleh, M. and Ambrose, J.A. (2018). Understanding myocardial infarction. F1000Research, 7(1), p.1378.
Shah, A.H., Puri, R. and Kalra, A. (2019). Management of cardiogenic shock complicating acute myocardial infarction: A review. Clinical Cardiology, 42(4).