Introduction
- Reflection on Covid-19 incident;
- Using Gibbs’ reflective cycle;
- It has six stages;
- Description, feelings, evaluation, analysis, and conclusion;
- Sixth stage – plan of action.
This presentation is a critical reflection on a Covid-19 incident that I have experienced during my nursing practice using Gibbs’ reflective cycle. This cycle has six stages (1) including description (of the experience), feelings (about the experience), evaluation (of the both good and bad of the experience), analysis (to make sense of an occurrence), conclusions (learning points), and action plan (changes that could be done in the future). As shown in this presentation, Gibbs’ reflective cycle offers an elaborate framework to examine experiences.

Scenario
- I am a wound specialist;
- Effects of Covid-19;
- Referred to Covid-19 patient;
- Battling fear;
- Torn between my job and fear;
- Scared of contracting Covid-19.
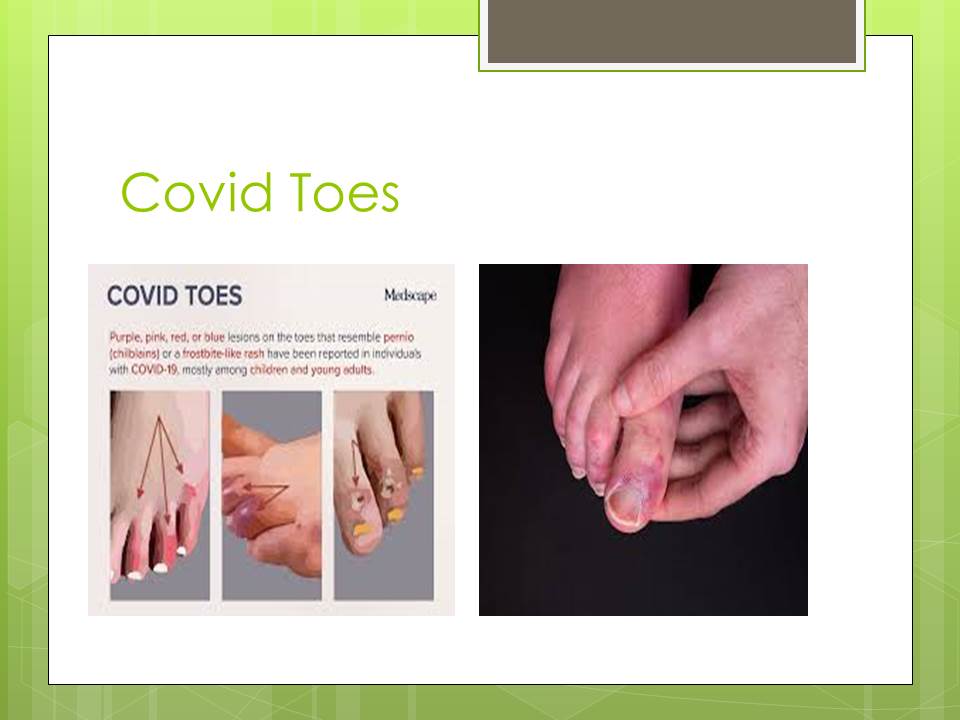
My daily routine involves seeing patients with different types of wounds like pressure ulcers, diabetic ulcers and other types in my daily clinic. The hospital atmosphere where I work is always tense and anxiety, most of the time, fills the air due to Covid-19. One morning while I was checking my system for new referral notification, I found a referral for one of my colleagues and friend who was admitted with Covid-19 and referred to me to check his toes discoloration, which is now being called “Covid toe”. I spent a few minutes silent in front of my desk as my brain stopped working and my heart rate increased. I was torn between seeing this patient do my job as doing before and at the same time, I was anxious that I might acquire the disease.

Scenario: Continuation
- I decided to see patient;
- Put on my PPE;
- Informs patient about my visit;
- He becomes agitated;
- Calms him down soothingly;
- Examines and dresses Covid toe.
I finally put my PPE mask on and entered his room. However, the patient was in distress and the moment I explained to him what I needed to do, he started shouting and yelling. I managed to calm him down by speaking softly and soothingly assuring him that all will be well because he was in good hands of competent care professionals. After calming down, I assessed his toes and conducted ankle-brachial index diagnosis to assess the complexity of the vascularity of lower extremity before dressing the wound. Being next to the patient, I experienced incredible stress, although I was fully protected by the PPE mask and his assignment nurse supported me, and she was calm. I was highly stressed, my hands were shaking, and I was sweating all over.

Covid Toes
Covid-19 Protective Gear
This is how I was dressed when entering the patient’s room.

Description
- Received referral from a friend;
- Had to examine “Covid toes”;
- Patient becomes agitated;
- Applies effective communication;
- Calms down the patient;
- Performs wound care protocols.
I received a referral to attend to a patient friend who had been diagnosed with Covid-19, specifically to check his toes, which had started to undergo discoloration – a condition termed as “Covid toes”. In the room, we were two of us – his assignment nurse and I, and the moment I started explaining to the patient that I had come to examine his “Covid toes”, he became restless and within no time, he started yelling and shouting. I had to think quickly and act appropriately by applying what I had studied in theory about handling a restless patient. Effective communication plays a central role in calming down such patients (2). Therefore, I talked to the patient softly and soothingly. The assignment nurse remained calm throughout this incident.

Description: Continuation
- Thought of normal nurse-patient interaction
- Situation escalates
- Patient becomes agitated.
- Acceptable outcome
- Conducted ankle-brachial index diagnosis
- Dressed the wound
- Mission accomplished.
I was in the patient’s room specifically to examine his “Covid toes”. In my mind, I would enter the room, have the normal nurse-patient interaction, examine, dress his wounds and get out of the place. However, the patient’s restlessness and yelling interrupted my plan. Nevertheless, the outcome of the situation was acceptable. After calming the patient I assessed his toes and conducted an ankle-brachial index diagnosis to assess the complexity of the vascularity of lower extremity before dressing the wound.

Feelings
- Very tensed;
- Dealing with Covid-19 patient;
- Calming down the patient;
- Shaking and sweating.
The entire period, during the situation, I was tensed. The thought that I was dealing with a Covid-19 patient was chilling. Despite being fully covered and protected using a PPE mask, I felt vulnerable as if I would catch the disease anytime. Additionally, there was the issue of the patient being restless, yelling, and ordering us to leave him alone. Before the situation, I was already tensed and stressed. With reports (3, 4) of nurses and other care professionals being infected and some dying, it was expected that I would be stressed and scared. After the situation, I was relieved that I had calmed the patient, examined and dressed his wounds and gotten out of the room. I was shaking and sweating throughout this incident.

Feelings: Continuation
- Assignment nurse scared, but calm;
- I lacked composure;
- I contributed positively and negatively;
- Unnecessary tension and fears.
I think the assignment nurse, who was present at the time, was also feeling scared, especially given that I was shaking and sweating. I think other care providers are also concerned about handling Covid-19 cases. During the situation, my mind focused on ensuring that I stayed safe without being exposed in any way and calming down the patient so that I could accomplish my objective of wound examination and dressing. In retrospect, I think my fear of Covid-19 made the situation unnecessarily worse.

Evaluation
- Both good and bad aspects;
- Courage to attend Covid-19 patient;
- Applied theoretical knowledge;
- Calmed the patient;
- Lack of composure;
- Contributed negatively.
I gathered the courage to attend a Covid-19 patient, which was a good thing. Second, I applied my theoretical knowledge to calm down the patient before I successfully examined and dressed his wounds, which is part of what went well. However, I was freaking out during the situation. I think my lack of composure contributed negatively to the situation. However, at the same time, my experience in calming down the patient contributed positively to the situation. I think the assignment nurse contributed positively to the entire experience.

Discussion
- I remained focused;
- Remembered primary role of nursing;
- Unnecessary, but founded fears;
- I am human first;
- Acted rationally and practically;
- Most care providers are scared.
I think one of the reasons why things went well was the fact that I remained focused on my objective. Despite being scared of handling the patient, deep down I knew that as a nurse, my primary task is to provide care to the vulnerable and those in need of my services (5). This understanding helped me to overcome my fears and examine the patient’s wounds. On the other hand, I believe the reason why my interaction with the client did not go well was due to my fears concerning Covid-19. From my experience, I believe that I acted rationally and practically to accomplish my objectives. From the available literature, I understand that, just like myself, most care providers are scared of Covid-19 (6).

Conclusions
- Very informative experience;
- Scared for my life;
- Balanced nursing practice approach;
- Importance of effective communication;
- Patient calmed down;
- Achieved my objectives.
This experience has been more enlightening and informative than any other that I have had during my nursing career. First, I now understand what it means to be scared of my life when in line of my duty. I have always believed that my patients’ wellbeing comes first and I should not think twice when making a decision concerning whether to help a patient. However, I now acknowledge that I am a human being with fears, and this allows me to approach my nursing practice more pragmatically for the wellbeing of both the patients and myself. Second, I now understand the important role of effective communication in nursing practice (7). When I resorted to soothing talk, the patient calmed down and I was in a position to accomplish my objectives.

Conclusions: Continuation
- Situation could be more positive;
- If I remained calm;
- Develop skills on composure;
- De-escalation skills;
- Meditation for my calmness.
This situation could have been more positive for everyone involved if I had not freaked out when interacting with the patient. Therefore, I need to develop some skills to help me to remain composed when dealing with stressing scenarios. First, I need to learn de-escalation skills (8) as an effective way of calming down agitated patients. Second, I will learn how to apply meditation during my practice. For instance, in this case, I could have used meditation (9) to calm myself down and reduce my shaking, together with sweating. This way, I could have been more confident and assuring to the patient and the assignment nurse. Ultimately, the experience would have been better, even with the patient becoming agitated.

Action Plan
- Would remain calm and composed;
- Register for online class;
- On mediation in nursing;
- Apply skills learned;
- Be conscious of my environment.
If I had to do the same thing again, I would remain calm and composed throughout the situation. I was fully protected through my PPE mask and other protective gear, and thus there was no reason for being scared. As such, to develop the needed skills, I will register for an online class about effective mediation in nursing practice. This way, I will gain the requisite knowledge on how to calm myself down even when the surrounding circumstances are adverse. Addition, I will practice how to meditate daily because I believe that with enough practice, I will perfect my skills. Finally, to make sure that I act differently next time, I will always be conscious of my environment and act appropriately without unwarranted fears.

Reference List
Gibbs G. Learning by doing: a guide to teaching and learning methods. Oxford: Further Education Unit; 1988.
Dithole KS, Thupayagale-Tshweneagae G, Akpor OA, Moleki MM. Communication skills intervention: promoting effective communication between nurses and mechanically ventilated patients. BMC Nurs. 2017;16(1): 1-6.
Jewett C, Bailey M, Renwick D, Kaiser Health News. Nearly 600 US health care workers have died of COVID-19: the tally includes hospital janitors, administrators and nursing home workers. ABC News [Internet]. 2020.
Marsh S, McIntyre, N. Six in 10 UK health workers killed by Covid-19 are BAME. The Guardian [Internet]. 202o.
Flinter M, Hsu C, Cromp D, Ladden MD, Wagner EH. Registered nurses in primary care: emerging new roles and contributions to team-based care in high-performing practices. Jour. Ambul. Car. Mngt. 2017;40(4): 287-296.
Deying Hu, Yue Ko, Wengang Li, Qiuying Ha, Zhang X, Zhu LX, et al. Frontline nurses’ burnout, anxiety, depression, and fear statuses and their associated factors during the COVID-19 outbreak in Wuhan, China: a large-scale cross-sectional study. EClin.Med [Internet]. 2020.
Norouzinia R, Aghabarari M, Shiri M, Karimi M, Samami E. Communication barriers perceived by nurses and patients. Glob. Jour. Heal. Sci. 2016;8(6): 65-74.
Appold K. De-escalation training prepares hospitalists to calm agitated patients. Hospt [Internet]. 2015.
van der Riet P, Levett-Jones T, Aquino-Russell C. The effectiveness of mindfulness meditation for nurses and nursing students: an integrated literature review. Nurs. Edu. Tod. 2018;65: 201-211.
Syrek R. Trending clinical topic: Covid toes. Medscape [Internet]. 2020.