Introduction
Healthcare informatics plays a critical role in capturing data that can be used to improve care practices. In a healthcare setting, data is intensive because it involves working with people, and information on their ailments, payments, background, and more is required. It is important to mention that health informatics is an interdisciplinary study that focuses on the design, development, and application of technology in healthcare delivery, management, and planning. Length of stay (LOS) is an opportunity for informatics to utilize methods, such as defining success and flexibility, to implement new systems in healthcare, along with collaborative practice theory and teamwork skills.
Opportunity for Tracking Care Improvement
Tracking in healthcare involves monitoring a patient’s progress throughout hospitalization. A rational opportunity for tracking care improvement is when a facility adopts a data-driven approach to assess length of stay (LOS) to improve care coordination in intensive care units (ICUs) (Zangmo & Khwannimit, 2022). Tracking this matter is one way to coordinate and effectively provide healthcare services, as there is an expectation from the staff regarding the same.
To effectively track LOS for ICU patients, key information must be captured. For example, the patient’s name, admission date, conditions, progress, and discharge date can be recorded under this perspective (Hu et al., 2022). In this case, hospitals may obtain average LOS and use a predictive model to plan for their systemic healthcare delivery issues. Figure 1 shows an example of the calculation of LOS.
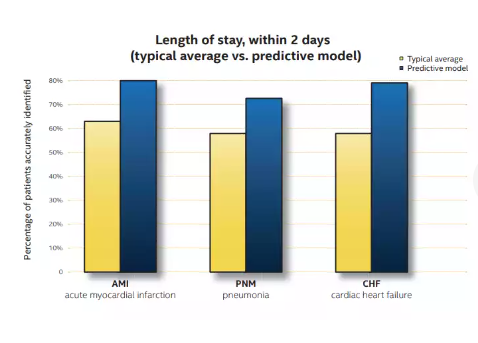
Patient-centered healthcare is a crucial aspect of improved care. Health informatics plays a crucial role in facilitating the integration of advanced technology and required information to develop a conceptual framework that can be applied in a care setting (Trivedi et al., 2021). Through health informatics, doctors and nurses can use electronic health records (EHRs) to coordinate care and share information in collaborative, joint practice within the medical delivery of services. In that case, it will be possible to ensure the quality of treatment and management of patients’ conditions in a care facility (McGonigle & Mastrian, 2018). Health informatics helps clinicians communicate and use available resources to interact, ensuring an exemplary care experience for patient satisfaction.
Required project management strategies include defining success, understanding risk, establishing a central communication tool, and fostering flexibility and adaptability. For example, Intel and Cloudera are popular integrated systems that create artificial intelligence (AI) dimensions, which can be used to predict discharge dates and times of admission, thereby measuring success (Jain et al., 2022). Therefore, these systems require personnel who can effectively configure settings and operate them to obtain data that helps determine the length of hospital stay, ensuring flexibility. In this matter, informatics guides a facility on specific occasions when medical wards are at full occupancy, using the methodologies shown in Figure 2.
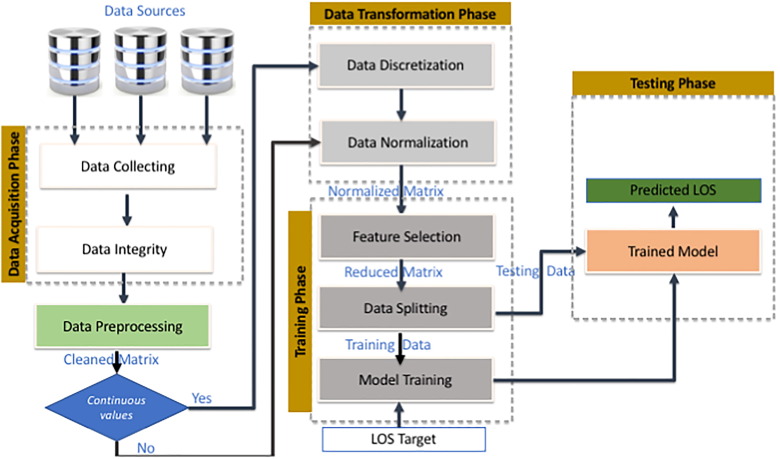
Systems and Staff Members Needed in Design and Implementation
As depicted in previous paragraphs, Intel and Cloudera are the most commonly used systems accounting for LOS in ICU and other care facility settings. The medical team to be included must be able to accurately decide and manage these systems. Hence, the staff required in this case comprises nursing informatics who have specialized in the Internet of Things (IoT) from a medical perspective (Blitz, 2021). While using these systems, the EHR must be patient-specific, including the capture of sensitive data that may be key to determining the appropriate clinical course of action.
The role of an advanced registered nurse is to leverage health care data by applying clinical knowledge from experience and specialization in a particular field of medicine. In this case, the nurse will apply critical care procedures based on a well-thought-out, idealized perspective on ICU patient management from past, literary, and sustainable encounters (Blitz, 2021). The advanced practice nurse will develop knowledge and share it with other clinicians regarding the required skills for caring for patients with specific clinical conditions.
Strategies for Implementing New EHR Proposal
The first strategy is to set a clear roadmap for EHR execution. In this strategy, the health informatics workforce will communicate to other staff involved in health records the need to integrate new systems to improve clinical duties (Blitz, 2021). Communication builds the team’s readiness, which is a key factor since the group is the primary personnel behind successful electronic health records implementation. Communicating changes to the IT infrastructure, current systems, and processes will be key to helping the team recognize the need to improve ICU services by integrating LOS data.
The other strategy is to create a multi-faceted team that shall play an integral part in the execution of new systems. In this case, it manages human resources, including three key players. First, a superuser is put in place, followed by a lead physician, and, lastly, a project manager to link the EHR service provision to the tasks undertaken by these human resources (DeNisco, 2021). The second strategy involves creating a budget that assembles fiscal resources to ensure sufficient funds for the purchase of new clinical practice equipment. The reason system changes may be costly is the acquisition of new, modern machinery that can support improved ICU care.
Professional, Ethical, and Regulatory Standards to Incorporate
The care facility must incorporate professionalism, ethics, and regulatory requirements into its EHR system. Professional standards include having a team specializing in medical technology as a course and having gained competent training to maintain and access the systems efficiently (DeNisco, 2021). The other professionalism is through the appropriate use of systems to determine specific medical courses of action without trial-and-error methods. Ethical standards include work autonomy, responsibility in the work environment, and privacy and confidentiality.
A person working with the new systems should aim to care for ICU patients without negligence in data entry and should not share information on diagnosis, prescriptions, or conditions with third parties. The regulatory standards include compliance with federal laws such as the Health Insurance Portability and Accountability Act of 1996 (Zangmo & Khwannimit, 2022). HIPAA requires individuals who handle sensitive patient data to protect it in the patient’s best interest.
Evaluating the Success of EHR Implementation from Staff, Setting, and Patient Perspectives
Staff competency in using the new system shall be a key measure of whether or not the success rate has been achieved. It requires verifying whether nurses and doctors can perform clinical practice tasks using the systems without limitations. In terms of setting, it is essential to assess whether the new EHR is helping solve problems that existed before its implementation (Abd-Elrazek et al., 2021). For instance, a new ICU machine will be evaluated to determine whether it can reduce LOS and lower costs in a care facility. Patient-centric measures include measuring patient satisfaction through reduced hospitalizations, shorter recovery periods, and an exemplary patient experience in medical practice.
Leadership Skills Required
It is important to have a specific leadership skill that enables collaboration and leads to evidence-based care through theoretical supplementation. The required skills include partnership teamwork, promptness, confidence, and communication (Weberg et al., 2019). It means a leader in transforming patient care through new EHR implementation must involve other members to offer solutions to underlying problems and do so promptly.
Additionally, the leader must be confident in preventing uncertainties and vulnerabilities in the news system from being handled by other members. Lastly, they should communicate the steps that have improved, the key goals, what needs to be changed to improve, and how the team is performing. The collaborative learning theory (CLT) is useful in this context, as groups will work together to complete a task by combining knowledge and expertise and leveraging evidence from experience (Weberg et al., 2019). The theory advocates cooperation between medical and IT professionals, with ideas combined to address challenges through problem-based learning.
Conclusion
Nursing informatics is an important initiative that helps a clinical facility implement effective IoT in healthcare. Opportunities that may involve the application of informatics include determining LOS for ICU patients. A hospital can assess the trajectories of patient admissions, thereby leveraging care in terms of quality, cost, and liabilities. The role of informatics is to provide evidence-based knowledge through strategies and methodologies that improve care. These perspectives require professional, ethical, and regulatory standards to evaluate success. CPT is a recommended theory for interprofessional reasoning in solving medical problems.
References
Abd-Elrazek, M. A., Eltahawi, A. A., Abd Elaziz, M. H., & Abd-Elwhab, M. N. (2021). Predicting length of stay in hospital intensive care unit using general admission features. Ain Shams Engineering Journal, 12(4), 3691–3702.
Blitz Rogério Marcus. (2021). Conceptual design, implementation, and evaluation of generic and standard-compliant data transfer into electronic health records. Routledge.
DeNisco, S. M. (Ed.). (2021). Advanced practice nursing: Essential knowledge for the profession (4th ed.). Jones & Bartlett Learning.
Hu, Y., Zheng, L., & Wang, J. (2022). Predicting ICU length of stay for patients with diabetes using machine learning techniques. 2022 International Conference on Cyber-Physical Social Intelligence (ICCSI), 4(7), 2–9.
Jain, R., Singh, M., Rao, A. R., & Garg, R. (2022). Machine learning models to predict the length of stay in hospitals. 2022 IEEE 10th International Conference on Healthcare Informatics (ICHI), 4(6), 34–44.
McGonigle, D., & Mastrian, K. G. (Eds). (2018). Nursing informatics and the foundation of knowledge (3rd ed.). Jones & Bartlett Learning.
Trivedi, N., Moser, R. P., Breslau, E. S., & Chou, W.-Y. S. (2021). Predictors of patient-centered communication among U.S. adults: Analysis of the 2017-2018 Health Information National Trends Survey (HINTS). Journal of Health Communication, 26(1), 57–64.
Weberg, D. R., Mangold, K., Porter-O’Grady, T., & Malloch, K. (2019). Leadership in nursing practice: Changing the landscape of health care (3rd ed.). Jones & Bartlett Learning.
Zangmo, K., & Khwannimit, B. (2022). Validating the ApacheⅣ score in predicting length of stay in the intensive care unit among patients with sepsis, 9(6), 39–62.