- Project Description: Palliative Care for Adult Cancer Patients
- Determining the Type of the Statistical Analysis: Paired T-test
- Project Timeline: Setting the Deadline and Crucial Milestones
- Considering the Expenses: Financial Aspects of the Study
- Outcomes and How They Will Be Analyzed
- Statistical Analysis Related to the Data Collection Tools
- Type of Demographic Data to Be Considered
- Expected Outcomes: PM Team as the Solution
- References
Project Description: Palliative Care for Adult Cancer Patients
Cancer patients have to face a variety of health-related challenges regularly, pain being one of the key issues (Fonseca, Ramos, Lopes, Mendes, & Parreira, 2017). Therefore, efficient palliative care, particularly, the design of strategies aimed at reducing the painful experiences, is essential (Koller, Hasemann, Jaroslawski, Geest, & Becker, 2014). However, the current approach toward meeting the patients’ needs lacks efficacy due to the absence of focus on patient education and promotion of agency among the members of the target population (Shah & Abdi, 2017). Therefore, introducing the palliative care team that will provide patients with detailed guidelines about self-management and offer support is bound to have a powerful effect on the success of the palliative care (Hucker, Winter, & Chou, 2015).
Determining the Type of the Statistical Analysis: Paired T-test
Choosing the right framework for statistical analysis is crucial to the success of the overall research. Therefore, it is imperative to focus on the essential characteristics of the study to determine the appropriate statistical tools. Therefore, the fact that the key variables of the study will have to be compared needs to be brought up.
Particularly, one must mention that the means of the research variables will need to be compared. Therefore, a paired t-test will have to be used to compare the outcomes of the application of the appropriate tools. As a result, the efficacy of the PM team’s work combined with the traditional approach to managing pain can be compared to the standard types of alleviating pain among cancer patients (Main & Ogaz, 2016).
Project Timeline: Setting the Deadline and Crucial Milestones
The timeline for the project will include the following essential stages: arranging the available resources and allocating expected costs; recruiting the participants; introducing the team of pain management experts to the study participants; gathering the data retrieved from the target group and the control group; conducting the analysis, and interpreting the results. Seeing that the project is going to be rather lengthy due to the need to help the target audience develop the required skills and manage pain successfully, it can be assumed that the project will require at least six months. The chart below shows the timeline for the study.
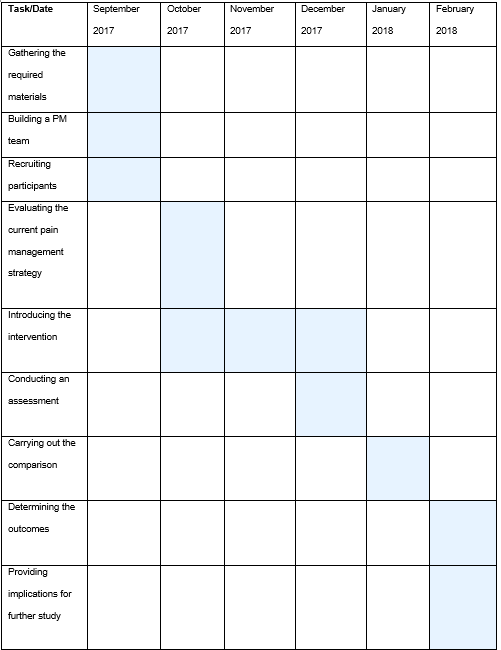
Considering the Expenses: Financial Aspects of the Study
Seeing that the project will require the services of expert nurses, one will have to expect a significant number of expenses. At present, the budget of the study estimates approximately $50,000. As the table below shows, it will be crucial to spend a large amount of money on communication since the connection between the participants, the nurses, and the authors of the study will have to be maintained and remain consistent.
Table 2. Budget.
Grant-related opportunities will be viewed as the primary source of research funding.
Outcomes and How They Will Be Analyzed
The results of the study will be analyzed with the help of the IBM statistical tools. Particularly, SPSS software will be used to conduct the study. To answer the research question, one will have to compare the patient data before and after the intervention. Particularly, the information gathered with the help of the pain measurement scales will have to be used to carry out the study.
Statistical Analysis Related to the Data Collection Tools
As stressed above, the Student’s t-test will be used as the main analysis tool. Thus, the data will be compared successfully. Furthermore, the tendencies observed among the patients will be identified.
Type of Demographic Data to Be Considered
To make sure that the analysis should return objective results and that the study should lead to an accurate representation of the target population and its needs, one will have to include the demographics-related information in the analysis. Age and gender will be viewed as the key demographic variables to be incorporated into the research.
Expected Outcomes: PM Team as the Solution
It is believed that the study will prove the superiority of the PM team combined with the traditional approach to the use of the standard tools solely. Moreover, it is assumed that the research will point to the importance of giving the patients a certain amount of agency. Finally, the importance of patient education is likely to become evident after the study is completed.
References
Fonseca, C., Ramos, A., Lopes, M., Mendes, F., & Parreira, P. (2017). Control of pain and dyspnea in non-pharmacological interventions: Patients with oncologic disease in acute care. Journal of Cancer Science and Therapy, 9(1), 319-320. Web.
Hucker, T., Winter, N., & Chou, J. (2015). Challenges and advances in pain management for the cancer patient. Current Anesthesiology Reports, 5(1), 346-353. Web.
Koller, A., Hasemann, M., Jaroslawski, K., Geest, S. D., & Becker, G. (2014). Testing the feasibility and effects of a self-management support intervention for patients with cancer and their family caregivers to reduce pain and related symptoms (ANtiPain): Study protocol of a pilot study. Open Journal of Nursing, 4(1), 85-94. Web.
Main, M. E., & Ogaz, V. L. (2016). Common statistical tests and interpretation in nursing research. International Journal of Faith Community Nursing, 2(3), 5-9. Web.
Shah, K. B., & Abdi, S. (2017). Acute perioperative pain management in chronic pain oncology patients. Pain Research and Management, 2017(6120395), 1-6. Web.