Across the world, and notably in the developed nations, the number of older persons is increasing, a trend that is largely attributed to the technological innovations in the medical field. The increase in the number of the aged, however, raises many other pressing issues such as health implications and other financial and ethical questions (Elwan, 1999). Changes, especially among the working class, leave many older people vulnerable, consequently affecting their sense of belonging in society.
Despite the welfare programs instituted in many areas, the real needs for the elderly such as relief from pain, feeling involved and being part of a community are rarely taken into consideration (Elwan, 1999). This makes such experiences as pain, marginalization, physical suffering and loneliness become part of their everyday life. Thus as noted by Ferraro (2003), most deaths in the developed and emerging economies occur at 65 years. However, life expectancy rates are increasing in many countries. Increase in expectancy has increased the number of people who live to old age, i.e. past 65 years. More people are consequently dying from chronic illnesses rather than the past acute illness (Ferraro, 2003). People will, therefore, need other kinds of help with problems associated with the old and the care projected to the people.
In the past, quality care was only given to cancer patients who were hospitalized. However, currently, the care needs to be projected to other illnesses that crop up with age, for instance, Alzheimer’s disease (Lakatta, 2002). This then means that older people will need multiple care packages with the kind of care being provided by professionals in partnership with other groups. Professionals will additionally need to be supportive of the older people’s families, and the state, in general, will need to generate other mechanisms that could handle the aged (Lakatta, 2002). Countries will additionally need to develop health care services that will assist them in meeting the medical and social needs of the elderly.
Wenger (1999) adds that effective care will need to reach hospitals, people’s residential places and other nursing and residential homes in the community. As populations age, the pattern of diseases people is suffering from also change. As noted, many people die because of chronic diseases such as heart diseases, célèbre vascular disease, respiratory diseases and cancer (Marshall et al., 2009). It, therefore, becomes difficult to diagnose one particular disease with certainty as to the real cause of death as the old suffer from multiple diseases. For instance, it is very difficult to diagnose dementia, and it is not very clear to many people on whether the increased age is accompanied by longer periods of disability (Wenger, 1999).
It is without a doubt that the increased number of old people will challenge the health care systems and make it impossible to provide effective and compassionate care. In most countries, old people live in their homes, and various countries have advanced various mechanisms for offering care to the aged (Harwood et al., 2004). In Australia, for instance, 1 out of every 15 people live in institutions in comparison to 1 out of 20 in the United Kingdom (Harwood et al., 2004). Many aged people spend their time in nursing homes in the United States, and the service is maintained by federal Medicare benefits.
Modernization and urbanization, in addition to the shifting values as regards family care for older people, has led to a marked breakdown in the community and intergenerational support mechanisms (Wells, 2005). Thus the current support and care models have taken various forms such as community-based care and health maintenance approaches; however, there is a need to integrate strategies that the old can call upon in times of emergencies. Health is not merely the absence of disease but includes among other factors the capacity of one to cope effectively with emerging life challenges and to maintain physical, mental and social well being (Wells, 2005).
Family members must thus ensure that old people have access to basic health services during emergencies. Additionally, their capacity to maintain their health will reflect the ability to re-establish the relationship networks and most importantly, self-sufficiency (Sandhu, 2009). Therefore, other than health, caregivers need to recognize other broader factors such as the socio-economic conditions that affect the older ones’ ability to survive and recover.
In Australia, only about 40% of Australian Aged Care Providers are able to make a profit (De Looper & Bhatia, 2001). The rest of the population lives mainly on borrowed supplements or depend wholly on their family members. Aged recipients in Australia are dependent on assistance from the Australian Federal Government. However, this process requires an assessment by an Aged Care Assessor (ACAT). The care is then divided into several other categories depending on the situation and can fall into three main levels: low care, high care and the veteran’s home care (De Looper & Bhatia, 2001).
In caring for the aged, most care is listed as non-medical, which is covered by insurance or other public funds. In the US, for instance, almost 86% of the residents live in facilities pay for care from their own funds. The rest of the population gets their help from family and friends and other state agencies. Medicare does not include pay unless the unskilled medical care is needed and later given in skilled nursing facilities (De Looper & Bhatia, 2001).
As aforementioned, older people are prone to many diseases and cardiovascular diseases are among them. In the US, for instance, this category of diseases is responsible for almost 40% of total deaths in those aged above 65 years (Help Age International, 2000). Age is thus an identifying characteristic of the disease. Clinical manifestations and diagnosis of the various cardiovascular diseases differ with age as interactions occur between age-associated cardiovascular changes. Cardiovascular diseases in Australia are on the rise among ageing persons. And as recorded by the Australian Bureau of Statistics, in 2005- 2005, 13% of the age groups 35-44 had the disease, the ratio increased to 23% amongst the 45-54 years and 63% amongst the 75 years and above (Help Age International, 2000). The number of females with the disease was higher than that of males. 20% of all females had the disease in comparison to 16% of the males (De Looper & Bhatia, 2001). The report is shown on the table below for more detailed coverage.
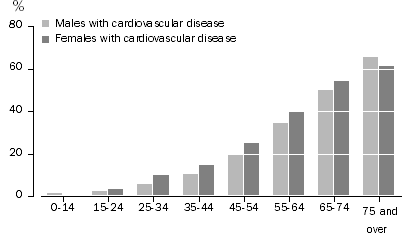
In terms of care, the prevalence amongst women in relation to men presents a problem in that few men are able to cope with the single life. Most men are used to being assisted in various activities and thus are unable to cope in the absence of their partners. The situation gets worse if the man is older. As noted, some cardiovascular diseases such as stroke and oedema are more likely to be found in women in comparison to men. Thus many, women with an increase in age, indicate a higher susceptibility to many cardiovascular diseases such as heart attacks. Women are more exposed to triggers in comparison to men and tend to demise earlier than men. However, as noted, due to the weakness of the body and the failure to conquer life challenges alone, men do not live long either after the spouse’s demise.
However, major differences can only be attributed to race. As noted from the table, men’s prevalence of cardiovascular disease only shoots up after 75 years of age, indicating their difficulties in coping either after the death of a spouse and the depreciating health due to unhealthy eating.
Many old people disregard their symptoms and rarely speak about them. Thus the caregivers need to give them enough attention and take notice of simple complains such as dull days and the presence of undue sweating. These, in most cases, are symptoms of silent heart attacks. Painless heart attacks are mostly identified with the old mostly among the diabetics. Additionally, sudden environmental changes, for instance, severe colds, could have a fatal effect on cardiovascular function in older people. Thus the caregivers have to safeguard against such as their frequent occurrence could aggregate conditions such as heart attacks, tachyarrhythmias or the rapid and irregular beating of the heart in addition to congestive heart failure.
Diseases of loved ones, for instance, a spouse, also lead to serious disturbances and imbalances in emotional behaviour. This could worsen some cardiac malfunctions among the elderly and death of an old person following the demise of a spouse is very common.
The old adage, old is gold, this can only make sense in a society if the old are well cared for. The state should not leave the responsibility to the family members alone as most of them are mobile, leaving the old helpless and vulnerable. Thus mechanisms should be put in place to enable the old enjoy the last phases of their life.
References
De Looper, M. and Bhatia, K. (2001). Australian Institute of Health and Welfare: Australian Health Trends. AIHW Cat. No. PHE 24. Canberra: AIHW. Web.
Elwan, A. (1999). Poverty and disability: a survey of the literature. New York: Routledge. Web.
Ferraro, R. (2003). Psychological resilience in older adults. Clinical Gerontologist, 26 (3-4):139-143. Web.
Harwood, R., Sayer, A. A. and Hirschfeld, M. (2004). Current and future worldwide prevalence of dependency, its relationship to total population, and dependency rations. Bulletin of the World Health Organization, 82 (4): 251-258. Web.
Help Age International (2000). Older people in disasters and humanitarian crises: Guidelines for best practice. London: HelpAge International. Web.
Lakatta, E. G. (2002). Age-associated cardiovascular changes in health: impact on cardiovascular disease in older persons. Heart Fail Reviews, 7(1):29-49. Web.
Marshall, C. A., Kendall, E., Banks, M. E. and Gover, R. M. (eds). (2009). Disabilities: insights from across fields and around the world, Volume 1. Westport, CT: Greenwood Publishing Group. Web.
Sandhu, H. S. et al. (2009). “Hyponatremia associated with large-bone fracture in elderly patients.” International Medical Journal 41, 733-737. Web.
Wells, J. (2005). “Protecting and assisting older people in emergencies.” Humanitarian Practice Network. London: Overseas Development Institute. Web.
Wenger, K. (1999) Cardiovascular disease in the elderly. The Cardiologists Journal, 17(10):609-90. Web.