The collected data analysis and the results of the conducted research are presented in the fourth chapter. The findings obtained in the course of the qualitative descriptive study are presented through research questions introduction, data collection procedure, demographics, and data analysis description. The study involves understanding the experience of surgical personnel in ambulatory surgical centers in the northeastern part of the United States who learn new, advanced medical-surgical technology through in-services and on-the-job training. The findings are presented in tabular and charts.
Research Questions
The research questions of the present study are as follows:
- RQ 1: How do surgical personnel describe their experience of learning new, advanced medical-surgical technology through in-services at ambulatory surgical centers in the northeastern United States?
- RQ 2: How do surgical personnel at selected ambulatory surgical centers experience in-services as a means to learn to use new, advanced medical-surgical technology?
- RQ 3: How do surgical personnel describe the effect of learning new, advanced medical-surgical technology through in-services with respect to their self-described confidence in their skill?
Data Collection
The data collection began as soon as the proposal was approved by the University of Phoenix Institutional Research Board. Announcements regarding the study were posted on social media and spread through word-of-mouth. The flyers included descriptions of the purpose and procedures for accessing and completing the questionnaire. As part of the recruitment process, each participant who met the inclusion criteria was able to log into the URL to access the questionnaire hosted by SurveyMonkey.
Each participant acknowledged and affirmed informed consent by checking the appropriate box on the first page of the study website to receive access to the questionnaire. Those who did not provide consent did not receive access. Participants in the study voluntarily continued through the questionnaire to receive the thank you note at the end of the questionnaire. Broad and open-ended questions helped the participants to concentrate on the topic.
Demographic
Participants in this study (a) had experience working in the surgical center and (b) attended in-services on new technologies by at least two different modalities. The training occurred (c) within the last two to three years. The researcher attempted to ensure, if possible, that (d) participants had experience with in-person/team-based training as well as technologically mediated training. In that way, (e) the participants could speak meaningfully about the advantages and disadvantages of either an on-the-job or in-service or technology-based method of learning, using a relevant basis for comparison. The working experience and the level of expertise in the surgical field, as well as the characteristics of training experience, were critical to the study. Such demographic characteristics as age, race, gender or marital status were not collected since they were of no relevance to the research purpose and intended outcomes. Only profession-related information, such as the position at the facility, the type of organization-based training the participants attended, and their reflection on the experience they obtained during the training were collected during the questionnaire.
Data Analysis
Upon the completion of data collection, the researcher initiated the process of data analysis. The research data obtained from the participants in the course of conducting the questionnaire was analyzed by studying each questionnaire’s answers upon completion. The researcher attended each questionnaire and systematized the answers separating them according to the question number and the similarities in responses. Since the questionnaire contained broad and open-ended questions, the answers to them required the researcher’s thoughtful and determined attention. The analysis of the responses based on the characteristics and perceived attitudes of the participants was carried out to identify the core themes in the population’s attitudes.
Open-ended question answers were grouped by theme and presented in the form of bar charts to demonstrate and interpret the percentage of each theme in the responses of the participants. The answers to the closed-ended questions were presented in the form of pie charts to demonstrate the percentage of particular answers among the entire studied population sample. Such a systematic and thorough approach allowed for laying a solid background with vividly illustrated data for the following step of results representation. Overall, the methods of analysis and synthesis were applied to conduct data analysis. In particular, Braun and Clarke’s (2012) thematic analysis was applied to address each research question and describe the themes of surgical competence, operating room efficiency, and patient safety and satisfaction.
Participants’ Role Identification
The primary data that was chosen for analysis was the roles of the participants within their respective organizational departments. This information was collected from the questionnaire answers manually by the researcher to identify what percentage of the respondents were surgeons, surgical technologists, operating room nurses, anesthesiologists, occupational therapists, and certified registered nurse anesthetists. The answers were manually analyzed and grouped into categories. This data was used as a starting point to determine the interrelations between the position specifications and the perception of training programs.
The Analysis of Data to Answer the First Research Question
The first research question of the study sought to determine how surgical personnel describe their experience of learning new, advanced medical-surgical technology through in-services at ambulatory surgical centers in the northeastern United States? Based on the themes of the questions formulated for the questionnaire, the researcher manually reviewed all relevant questions that provided information pertaining to the first research questions. Firstly, answers to the multiple-choice questions obtained from all participants were reviewed, analyzed, and grouped by the selection of a particular type of training. Secondly, the answers to the open-ended questions were read, analyzed, and grouped based on the characteristics of the described experience each participant provided. Thirdly, the answers to both types of questions from the questionnaire were combined and synthesized to formulate a response to the first research question. All the answers were separately recorded in tables to visualize the outcomes. Since the question was aimed at identifying the ways participants describe their experience, the researcher paid particular attention to the ideas and descriptive utterances the participants used in their texts. The nature of the study and the subjective features of inquiry necessitated a manual analysis of the data without the application of statistical methods.
The Analysis of Data to Answer the Second Research Question
Similarly to the procedure undertaken in the analysis of data pertaining to the first research question, the participants’ answers to the second research question, which aimed at defining how surgical personnel at selected ambulatory surgical centers experience in-services as a means to learn to use new, advanced medical-surgical technology, were manually analyzed. Judging from the perspective of their experience, the participants were asked to identify the most common drawbacks in in-service and on-the-job training for surgical technology use. This question was a multiple-choice type and was grouped into two categories, including on-the-job and in-service training. Consequently, following the procedure of data collection, the answers were analyzed gradually by retrieving all participants’ choices of drawbacks for both types of training. The selected drawbacks were categorized into two categories and grouped according to the particular drawbacks. The selected drawbacks were listed in the order from most frequently reported to the list frequently reported ones. All answers were recorded in a table depicting the participants and their selection.
After that, the answers to the open-ended questions pertaining to the participants’ experience of in-service and on-the-job training and their vision of possible improvements to eliminate the identified drawbacks were read, analyzed, and grouped based on the characteristics of the answers. All similarities in the answers were identified and used as a basis for categorizing. The answers to the open-ended questions related to the second research question were tied with the identified drawbacks to maintain clarity and consistency in the interconnection between the problem and its proposed solution. Thus, the table containing drawbacks selection was expended with the relevant proposed improvements. All the analytical processes were conducted manually by the researcher to ensure adequate and thorough interpretation of the participants’ answers, suggestions, and examples. The information that was not related to the themes investigated by the study was eliminated and disregarded.
The Analysis of Data to Answer the Third Research Question
To analyze the participants’ answers pertaining to the third research question, which asked how surgical personnel describe the effect of learning new, advanced medical-surgical technology through in-services with respect to their self-described confidence in their skill. The answers to the specific open-ended questions were read and grouped depending on the themes raised in the descriptions and perceptions provided by the participants. In total, four questions from the questionnaire were devoted to the investigation of the problem raised in the third research question. The answers of all participants were grouped accordingly with the identification of similarities in the perceived opportunities for improvement and the influence of the training on surgical competency and confidence. The information and participants’ comments that did not contain any implications relevant to the themes investigated by the study were disregarded.
The thematic analysis approach was used to identify key themes in the participants’ answers and comments. Such an approach allowed for distinctive interpretation of multifaceted phenomena of training, learning, and professional growth, which necessitated deliberate and thoughtful analysis of the researcher rather than mere quantitative representation of statistical data. Thus, the applied data analysis procedures matched the nature and purpose of the qualitative descriptive study. The categorized answers and descriptions retrieved from the participants and analyzed separately with regards to each research question were then combined to determine commonalities pertaining to the themes. At the stage of results interpretation, the researcher extensively utilized the data analysis procedure outcomes to develop the narrative for the findings depending on their contribution to each theme.
Results
At the initial stage, the questionnaire sought to understand respondents’ current role/position by asking them to “describe your role in your current organization and department.” Out of the 13 participants, three were surgeons, two were Surgical Technologist, two were Operating Room Nurses, two were Anesthesiologists, one was Occupational Therapist, one was Certified Registered Nurse Anesthetist (CRNA), and two did not indicate their current positions. Figure 1 below shows participants’ distribution per current role/position.
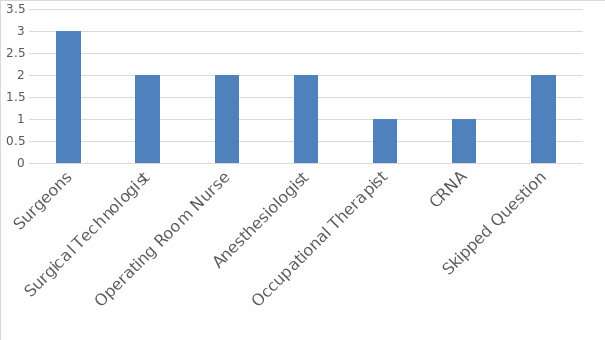
To understand participants’ education and training regarding new medical-surgical technologies, they were asked to choose the education and training they had received or continue to receive as a surgeon, anesthesiologist, CRNA, surgical technologist, operating room nurse, or “other.” The choices given to the respondents included In-services, On-the-job-training, or All of the above. Out of the 13 respondents, 2 (15%) did not respond to the question while 10 (77%) indicated that they had used both In-services and On-the-job-training. Lastly, only one (8%) respondent said that s/he had used in-services (see Figure 2 below).
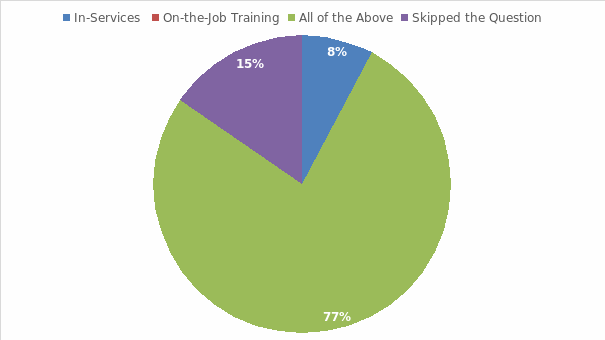
Experience of Learning New, Advanced Medical-Surgical Technology Through In- Services at Ambulatory Surgical Centers in Northeastern United States
Shortcomings and Drawbacks of In-Service Training Strategies
One of the goals of data collection by means of questionnaire was to explore the perceived reasons for drawbacks and imperfections of the training sessions the participants attended. To understand the shortcomings and drawbacks of in-service training strategies, the participants were asked to describe their experience by answering the following question: “From experience, what are the shortcomings and drawbacks of in-service training strategies?” Analysis of their responses led to the emergence of the following themes: inappropriate methodology and curriculum and lack of follow-up and motivation. Thus, a closer explanation of each of these two themes is relevant.
Inappropriate methodology and curriculum
Some of the participants emphasized that the methodology and curriculum utilized in in-service training were inappropriate. For example, Participant 10 complained of the inappropriate curriculum. Participants 1, 7, and 13 noted that in-service training was characterized by “lack of motivation, inappropriate curriculum, inappropriate methods, and lack of follow-up.” Lastly, Respondent 12 complained of “Lack of motivation, Inappropriate methods, and Lack of follow-up.”
Lack of follow-up and motivation
Participants 3, 6, 8, 9, and 11 indicated “lack of follow-up” was a major impendent to in-service training. On the other hand, Participant 5 complained of “lack of motivation.” Overall, majority of the respondents (38%) perceive “lack of follow-up” as the key hindrance to in-service training (see Figure 3). Next, 23% of them described “Lack of motivation, Inappropriate curriculum, Inappropriate methods, and Lack of follow-up” as drawbacks of in-service training. On the other hand, 8% of the participants noted that “lack of motivation” hindered their participation in in-service training. Similarly, 8% of respondents attributed the training to “inappropriate curriculum” while another 8% complained of “Lack of motivation, Inappropriate methods, and Lack of follow-up.” Lastly, 15% of the respondents did not describe the drawbacks associated with in-service training.
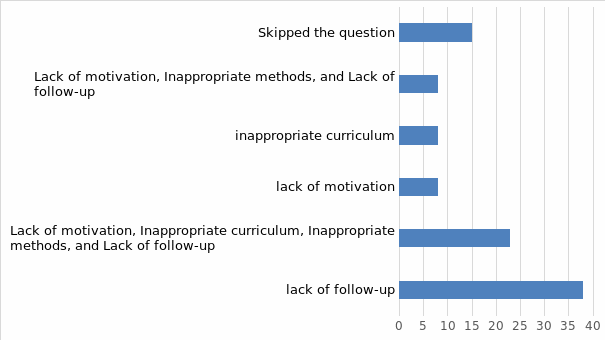
Ways of Addressing Shortcomings and Drawbacks of In-Service Training Strategies
To understand ways of addressing shortcomings and drawbacks of in-service training strategies, participants were asked to describe “How can the shortcomings and drawbacks of in-service training be improved to increase the quality of performance of future/novice operating room staff members?” Analysis of their responses led to the emergence of four themes— manufacturers’ representatives as trainers, follow-ups, the adequacy of trainers, and motivation and interactive instruction.
Manufacturers’ representatives as trainers
The participants suggested various ways of addressing the shortcomings and drawbacks of in-service training strategies. Participant 1 indicated that “training should include appropriate and strict curriculum” while the second respondent skipped the question. The third respondent noted that “there should be scheduled dates for the representative of the manufacturers to come in for follow-ups and possible retraining.” This implies that the respondent perceives the representative of the manufacturers as being the best trainers— possibly because they have experts who are well-versed with how the instruments and the equipment work. The fourth respondent did not provide ways of addressing in-service training challenges.
Follow-ups
The sixth respondent suggested that “follow-up should be encouraged.” Similarly, Participant 8 said that “the manufacturer should always schedule follow up training to ensure the efficiency of the staff in handling the equipment.” Respondent 9 agrees that “by making follow-ups available,” the quality of performance of future/novice operating room staff members could be improved. Participant 11 emphasized that “follow up will help increase competence. The company or manufacturer can schedule follow up after each training as continuing education for a better outcome.” These responses denote respondents’ inadequate skills and knowledge regarding the use of instruments or equipment was attributed to the failure of the trainers to try to understand whether participants understood the curriculum or not. The response further implies that the participants believe that they can master the essential skills if the trainers did a follow-up.
Adequacy of trainers
Participant 7 noted that “The reps from the companies may have difficulty with the dynamics of the operating room. They should be educated on how OR works. Follow up should be scheduled after the training.” This implies that although experts sent by manufacturers to train hospital personnel are well-versed in how the instruments and equipment work in the factory setting, they are not well-versed in using them in the operating room since they are not healthcare professionals. Participant tenth stated that inadequate quality of performance of operating room staff members is because “sometimes the equipment is not discussed in the training session.” This means that part of the training is more focused on the theoretical aspects of the instruments and equipment rather than the practical component.
Motivation and interactive instruction
The fifth participated suggested that in-service training should “create creative, insightful, and interactive in-service training.” This indicates that the previous curriculum provided to the participants was inappropriate and did not motivate them to learn the skills needed to operate the instruments and equipment. Participant 12 noted that the quality of performance of future/novice operating room staff members could be improved if “Before each in-service, the company provided light refreshments and always use a media that will have clear visual and audio.” In agreement, Participant 13 emphasized that “Motivate people by serving some refreshments. Go to the point, talk about the focus instrument or the equipment only. Teach with the right media. and try to follow up to encourage others to participate.” Participants’ responses highlight the importance of motivating trainees to help them stay on track and use of interactive instruction to keep trainees focused.
Shortcomings and Drawbacks of On-The-Job-Training Strategies
The participants further described shortcomings and drawbacks of on-the-job-training strategies. According to Participant 1, the short-comings include “ineffective trainer, team disturbances, rushed training, low productivity.” Participant 2 and 4 skipped the question while the third respondent complained of “team disturbances, rushed training, and low productivity.” The fifth and thirteenth respondent described on-the-job-training as characterized by “Rushed training” while Participant 6, 7, and 11 described the drawbacks as “Team disturbances and Rushed training.” Participant 8 and 9 complained of “Team disturbances.” Participant 10 described on-the-job-training strategies as having “Ineffective trainer.” The twelfth respondent complained of “Ineffective trainer, Team disturbances, Rushed training.”
Overall, majority of the respondents (23%) attributed on-the-job-training strategies to “team disturbances and Rushed training.” Next, 15% linked this methodology to “Rushed training” while a similar percentage (15%) complained of “team disturbances” while 15% did not answer the question. Additionally, 8% of the respondents “ineffective trainer, team disturbances, rushed training, low productivity.” Similarly, 8% of them described the strategy as having “ineffective trainer” and one of them (8%) complained of “team disturbances, rushed training, and low productivity.” Lastly, one respondent (8%) saw on-the-job training as characterized by “ineffective trainer, team disturbances, rushed training.” These results are displayed in Figure 4 below.

Ways of Addressing Shortcomings and Drawbacks of On-The-Job-Training Strategies
To understand ways of addressing shortcomings and drawbacks of in-service training strategies, participants were asked to describe “How the shortcomings and drawbacks of on-the-job-training are improved to increase the quality of performance of future/novice operating room staff members.” From an analysis of their responses, the following themes emerged: timely training by qualified staff and minimizing distractions.
Timely Training by Qualified Staff
Participant 1 stated that “All training should be scheduled ahead of time to accommodate most employees. The team should be given strict rules to adhere to instructions from the trainer.” This means that the respondent felt that majority of the employees were not told in advance that the training was taking place and, thus, a lower turnout. In support, the third respondent emphasized that “The training should be conducted by the most experienced staff member. Enough time should be allocated for the training, and the schedule must be made to accommodate most staff members or all.” Therefore, apart from timely informing employees about upcoming training, the respondent agrees that adequate time should be allocated for effective learning of the skills.
The need for competent trainers was further highlighted by Participant 5, who said that “personal providing on the job training should be well-versed and show complete competence.” This implies that a trainer who is well-versed with knowledge and skills regarding the use of instruments and equipment in the operating rooms can effectively teach the health workers. The seventh respondent further noted that “All staffers must take the training seriously. They should give more time for training” while Participant 8 emphasized on the need for “Strict handling of training time and participants.”
Timely Training by Qualified Staff is a recurrent theme as highlighted by Participant 10 who emphasized that “Experienced person should be the one teaching” and the eleventh respondent who noted that “They should allocate more time and enforce time and location.” Additionally, Participant 12 emphasized that “The on the job training team must deliver the training using a well-experienced employee and give enough time for the training. All employees participating in the training must be cautioned about cell phone use.” Lastly, Participant 13 agreed that “Allowing enough time for training will encourage others.”
Minimizing Distractions
The second theme that arose from the participants’ response is the need to minimize distractions. The sixth respondent noted that “All team members must be discouraged from socializing during training.” In support, Participant 9 stated that “All staff members must take training seriously and not try to socialize during training.” The minimal distraction allows the trainees to be mentally focused on what is being taught.
Effect of Learning Advanced Medical-Surgical Technology on Participants’ Confidence
Participants’ Experience In-Service
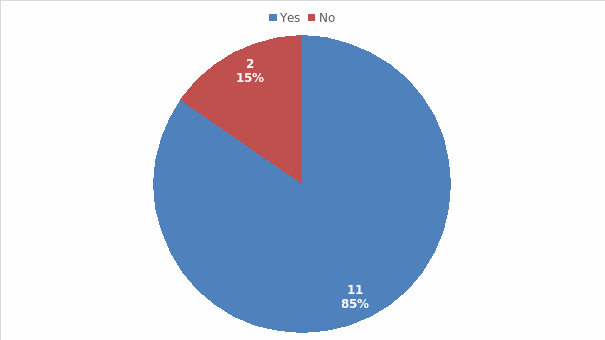
To understand whether personnel experience in-service as a means to learn to use new, advanced medical-surgical technology, they were asked to state whether the “in-services training available to the staff members are sufficient to prepare you for your role/s, especially as you often encounter crucial circumstances and manage complicated medical equipment in your daily tasks.” Out of the 13 respondents, 11 (85%) of them agreed that in-service training is essential in learning to use new, advanced medical-surgical technology while 2 (15%) skipped the question (see Figure 4). Similarly, 85% of them agreed that on-the-job-training available to the staff members are effective in helping them learn to use new, advanced medical-surgical technology while 15% did not respond to the question (see Figure 5).
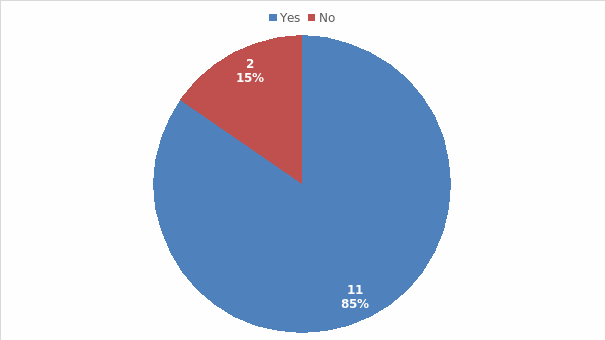
Participants’ Confidence
Participants were asked to describe “How do the in-services and on-the-job-training and education strategies help the staff members perform their duties and contribute to staff competence and efficiency inside the operating room.” Research participants shared a range of experiences and beliefs regarding the impact of learning new, advanced medical-surgical technology on their confidence, competence, and efficiency. For example, Participant 1 stated that “It helps shed more lights to how to use the instruments and or equipment. More education, the better experience.” This implies that the first respondent saw the learning experience as being important in improving their skills regarding the use of instruments and equipment. Therefore, the participant felt more confident in the use of the instruments and equipment following the in-service training.
Participant 2 did not respond to the question while Participant 3 described the in-service training as helpful “in refreshing old skills and applying new ones.” Like Participant 1, it can be seen that Participant 3 understands in-services and on-the-job-training as useful in improving their confidence in the use of instruments and equipment. This is attributable to the idea that the respondent sees the in-services and training as helpful in reminding them of things they might have forgotten and help them learn new skills.
Participant 4 skipped the question, while Participant 5 explained that the in-service “increases confidence and competency.” Therefore, like Participants 1 and 3, the respondent believes that through in-services, they will be capable of using the instruments and equipment successfully and efficiently. That is, by updating their knowledge and skills, they can use the instruments and equipment confidently.
Both Participants 6 and 13 stated that in-services and training lead to “increased productivity.” Improved productivity means that the respondents agree that by equipping them with new skills, thus preventing them from making mistakes. Increased productivity can also imply that the respondents believe that the acquired skills enable them to efficiently carry out their tasks.
Participants 7 and 12 stated that following the in-services and training, they have witnessed “better performance” or “improved performance.” As highlighted by Participant 5, improved performance could be attributed to “retained skills” which make them more effective in carrying out assigned tasks and using the instruments and equipment. In agreement, Participant 8 stated that training helped them achieve “better outcome and quality service.” The better outcome implies that the training equipped the responded with knowledge, skills, and confidence required to make well-informed diagnoses.
Participant 9 described learning new, advanced medical-surgical technology through in-services as “the best way to learn as you are handling human lives. It helps increase comfortably.” This means that the respondent perceives the in-services as the most effective platform for improving confidence in handling patients. Enhanced confidence is attributed to the participant’s comfort in addressing patients’ needs. Participant 10 just stated that training “helps a lot.” Lastly, Participant 11 emphasized that on-the-job training “is more like a residency. Working hard both with on-the-job training and in-services makes one a competent physician.” Improved competence means that the respondent perceives on-the-job training as crucial in boosting their confidence at work.
To further assess participants’ self-described confidence, they were asked to describe what they believed “would be most effective training process in developing the competency of surgical staff members or in terms of utilizing the new equipment and navigating the technologies inside the operating room.” Participant 1 explained that competency would be best built through “job training.” Specifically, the respondent emphasized that “the most effective training in my experience is on the job training.” Participant 2 did not answer the question. The third respondent agreed with Participant 1 that the most appropriate training is “Hands-on-training, which is mostly acquired with all types of training modes as long as staff members are allowed to work on the instruments and or equipment at the time of training.” Participant 4 skipped the question.
Participant 5 explained that “Most effective training process would be interactive training which simulates realistic scenarios.” Next, Participant 6 emphasized that “Both in-services and on-the-job training” are useful. In agreement, Respondent 7 maintained that “hands-on training” is the best while Participant 8 also agreed that “Hands-on training during either on-the-job or in-services” work the best. Another respondent who agreed that on-the-job training makes them competent were Participants 9 and 10 who described it as “On the job daily training” and “on the job training” respectively. Similarly, Participant 11 and 12 associated competencies with “on the job training is very effective as it is taught by experienced staffer” and “On-the-job training by well-experienced team member” respectively. Lastly, Participant 13 attributed competency to the assumption that “On the job training is better.”
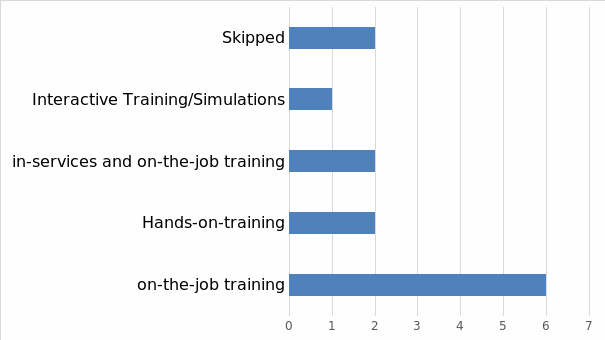
Overall, participants’ responses showed that the most preferred training method is “on-the-job” training (see Figure 5). This may be attributed to the presence of “well-experienced team member” and being “taught by an experienced staffer.” Out of the thirteen participants, six preferred “on-the-job” training. Hands-on-trainings was the second most preferred training method with two respondents supporting it. Similarly, two participants liked “in-services and on-the-job training.” Only one participant preferred “interactive Training/Simulations,” implying that it was not a preferred training method.
To further understand effective approaches needed to improve staff confidence inside the operating room, the participants were asked to describe “other methods and strategies can be implemented to improve the staff competence and efficiency inside the operating room.” Participant 1 stated that competence and efficiency could be improved through “Pre-recorded video is always useful for playbacks.” In agreement, Participant 3 emphasized that “Prerecorded training” is preferred.
Participant 5 linked improved competence and efficiency to “Teamwork and trust-building activities.” Similarly, Participant 6 seemed to like the idea of teamwork seen through a preference for “Peer training.” According to the seventh respondent, “Daily reminder training before procedures” improves staff confidence in the use of instruments and equipment. Participants 8, 9, and 13 preferred “online training.” Participant 10 wanted “Daily training and in service.” Similarly, the eleventh respondent emphasized on the need for “Daily in-service prior to procedures.” Participant 12 wished for “Daily refresher course before and after each procedure.”
Summary
Conclusively, this chapter presents the findings received as the result of the qualitative descriptive design data analysis. The overall research is aimed at investigating how operating room staff in the northeastern part of the United States learns medical-surgical technology by participating in on-the-job training or in-service training. The analysis of the current research’s findings allowed for answering the stated research questions by means of the questionnaires conducted among surgical room staff. The responses of the sampled population were analyzed, synthesized, and interpreted in accordance with the aims of the research.
In total, thirteen participants participated in this questionnaire, including surgeons, nurses, anesthesiologists, occupational therapists, surgical technologists, and certified registered nurse anesthesiologist. Two participants out of thirteen did not state their current position. Ten participants indicated that they had both on the job training and in-service training, which accounts for 77% of the respondents, while one participant stated that he/she did not participate in any activity, and two skipped this question.
Next, this research aimed to investigate the shortcomings and drawbacks of the technology-related surgical training. Their responses indicate that inadequate curriculum and methodology, as well as having no follow-ups and motivation, are the critical reasons for avoiding professional surgical training. When asked about ways to address these shortcomings, the participants indicated that they would want to have manufacturer’s representatives as instructors, follow up to ensure that the equipment is used appropriately, motivation, and adequate comprehension of the operating room and its dynamics. On the other hand, 23% indicate that rushed training and team disturbance is a major issue during training, while 15% referred to “rushed training” as the main problem.
In the open-ended questions part of the questionnaire, participants were asked to reflect on the ways of improving the current training practices. A participant stated that training sessions should be scheduled in advance to ensure a better turnout. Moreover, this participant complained of having insufficient time to learning new skills. Another participant noted that the trainer should be highly qualified and show competence. Three other participants supported this by arguing that better training for the instructors should be provided prior to the on-the-job training. Finally, distractions, such as socialization between team members, should be minimized as cited by two of the participants.
To reiterate the results, this research found that although the majority of staff members in the operating rooms undergo technology training, there are some significant issues with the way this training is conducted. Despite the shortcomings, 85% agreed that on-the-job training is an effective way of learning new skills required to use advanced surgical technologies. Most participants agreed that such training improves their performance and allows them to have more confidence when working with equipment or instruments in the operating room. On-the-job training was cited by most as the most effective training method. This chapter presents the complete responses of the individuals who participated in the current qualitative descriptive study on education and the use of medical technology.
Conclusions and Recommendations
The current study is designed to investigate the intersection between education and the use of medical technology in the surgical setting. The purpose of the study is to explore the experience of surgical personnel in ambulatory surgical centers in the northeastern part of the United States who learn new, advanced medical-surgical technology through in-services and the acquired level of skill competency. The objective of the current research is to understand how the medical personnel involved in the performance in the operating room perceives the level of their skills in terms of technology usage, as well as their perception of educational forms, techniques, and outcomes as they are used in the modern health care facilities. This final chapter will reiterate research questions to discuss how they were answered. Also, the findings obtained as the result of the conducted qualitative descriptive study will be presented and followed by the discussion of the study’s limitations. Finally, recommendations for leaders and practitioners and implications for future research will be addressed.
Reiterating Research Questions
For the purposes of qualitative research, the research questions pertinent to the identified topic of education and medical technology use were designed to investigate the ways the studied personnel perceives their experience related to training in technological use. Three research questions were formulated as follows:
- RQ 1: How do surgical personnel describe their experience of learning new, advanced medical-surgical technology through in-services at ambulatory surgical centers in northeastern United States?
- RQ 2: How do surgical personnel at a selected ambulatory surgical centers experience in-services as a means to learn to use new, advanced medical-surgical technology?
- RQ 3: How do surgical personnel describe the effect of learning new, advanced medical-surgical technology through in-services with respect to their self-described confidence in their skill
Discussion of Findings
Overall, 13 participants who represented the members of surgical team responded to the questionnaire investigating their experience in training, perception of the outcomes and the reasons for drawbacks. The findings of the study might be grouped in several sections.
Shortcomings and Drawbacks of In-Service Training Strategies
The study identified that the major reasons for drawbacks in the effectiveness of in-service training they attended were of internal and external nature. Firstly, the key factor in the diminished effectiveness of in-service training strategies is the inappropriate methodology and curriculum. Another reason, as perceived by the participants, is the lack of follow-up activities and insufficient motivation. These findings are consistent with those obtained by Bahler and Sundaram (2014) who found well-structured curriculum one of the core elements in achieving positive results in robotic surgery training. As perceived by the personnel, the best ways to address the identified shortcomings include manufacturers’ representatives as trainers, motivation and interactive instruction, follow-ups, and adequacy of trainers.
Shortcomings and Drawbacks of On-the-Job Training Strategies
The findings demonstrated that the frequently observed drawbacks and shortcomings in the implementation of on-the-job training for surgeons were determined by ineffective trainers, team disturbances, rushed training, and low productivity. These findings match the previous studies results but contribute to the scope of literature by identifying more reasons of possible inadequacy of training techniques. For example, the importance of effective trainers especially in the surgical setting expands the findings of Bamford and Coulston (2016). As the ways of addressing these shortcomings, the participants identified timely training by qualified staff and minimizing distractions as the most important ones.
Participants’ Experience and Confidence
Despite the identified difficulties with the effectiveness and feasibility of training interventions, the majority of participants admitted the usefulness and overall positive effect of training on their level of skills of technological use. It implies that once addressed from the perspective of the proposed improvements, the training strategies applicable to surgical team’s utilization of technologies will deliver better practical outcomes. The increased level of knowledge and competence in using advanced technologies in the operating room has amplified the personnel’s confidence and contributed to the safety of patients. These findings agree with and contribute to those of Cavalini (2014) and Cervantes-Sanchez (2015).
Limitations
The limitations of the study are those related to the population and the chosen study design. Firstly, the sampled participants’s diversity is not perfectly distributed across the team roles. The number of CRNAs and occupational therapists was less than that of other team representatives. Also, the subjective nature of the study that is limited to the interpretation of the data by the participants might be considered a limitation. Since the perceived attitudes dominated in responses, the findings of the research are influenced by the subjective views of the personnel.
Recommendations to Leaders and Practitioners
Since the problem addressed in this study is the lack of understanding the experience of medical personnel engaged in training for technology use, the study findings might be helpful in filling this gap and solving this problem. The leaders of health care facilities might construct better training sessions, employ more qualified experts and trainers who would lead the learning process effectively. Since one of the reported problems was the lack of motivation, leaders should implement benefits for personnel who attend training and demonstrate positive results. As for the practitioners, it is recommended to expand their knowledge and skills within the realm of technological advancement by means of systematic attending of training sessions, stimulating inner motivation for professional development, and allocation of sufficient time and resources for continuous learning.
Recommendations for Future Research
The conducted research might serve as a solid ground for future research. Since the field of technology use training in the surgical domain is relatively scarce, extensive investigation of the issues related to the topic are encouraged. The current qualitative descriptive study has presented an observational data concerning the most frequently observed problems in effectiveness of training strategies. Future research should concentrate on specific problems and reasons. Also, it is encouraged to utilize experimental and quantitative methodologies to diversify the scope of findings and improve the quality of training in the medical setting.
Concluding Remarks
In summation, the study investigated how the education and medical technology intersect in the surgical setting as perceived by the members of operating room team. The questions that were aimed to be answered in the course of the study included How do surgical personnel describe their experience of learning new, advanced medical-surgical technology through in-services at ambulatory surgical centers in northeastern United States? How do surgical personnel at a selected ambulatory surgical centers experience in-services as a means to learn to use new, advanced medical-surgical technology ? How do surgical personnel describe the effect of learning new, advanced medical-surgical technology through in-services with respect to their self-described confidence in their skill?
The findings demonstrate that despite the overall perceived effectiveness of in-service and on-the-job training, the participants reported significant problems that caused drawbacks and shortcomings in learning. They include inappropriate methodology and curriculum, the lack of follow-up activities and insufficient motivation, ineffective trainers, team disturbances, rushed training, and low productivity. However, the proposed ways to address these problematic areas are feasible and should be implemented in practical settings. The findings optimistically contribute to the scope of current literature and provide a solid background for future research. The description of the drawbacks and their elimination will be valuable information for leaders and practitioners working in surgical settings using advanced technology.