Introduction
In the event that food is not handled properly during preparation or is poorly stored, there is likelihood of food borne illness. For many years, food safety has been a growing threat to the public health in many regions of the world. Basically, food borne diseases can be grouped as either infections or intoxications and are caused by microorganisms that are ingested in the body and have the capability of multiplying.
According to Unnevehr and Hirschhom (2008), some factors that can inhibit the safety of food products are microbial pathogens, zoonotic diseases, parasites, adulterants, mycotoxins, antibiotic drug residues, pesticides, heavy metals, and genetically modified foods (p.8).
According to Unnevehr and Hirschhom (2008), Gram-negative pathogens are “bacteria that do not retain crystal violet dye in the Gram staining protocol”; however, they usually hold a “pink or reddish dye once a counterstain chemical is used.” These bacteria produce toxic substances when they enter the blood stream and cause destruction to tissue, hence leading to inflammation of tissues.
However, recent studies show that these bacteria are evolving and becoming immune to the available antibiotics. Most of the Gram-negative pathogens are considered harmful to their host, and are known to cause severe pneumonia, infections of the urinary tract, and the blood stream.
On the other hand, some threats to food safety are environmental and industrial pollution, agricultural practices, and food production practices and cultural practices i.e. consumption of raw food. Some of foods borne diseases are salmonellosis, Campylobacter, diarrhea, cholera, and Shigella. Shigella is a rod shaped bacteria that mostly affect the digestive tract.
According to Curtis, et al (2003, p.69), Salmonella are gram-negative bacteria, non-sporing, growing in both anaerobic and non-anaerobic conditions and that cause salmonellosis disease. The salmonella bacteria are capable of growing and living in areas with limited amount of oxygen. Some types of salmonella bacteria affect only animals and not human.
On the other hand, Shigellas are bacteria than cause shigellas infections symbolized with diarrhea and dysentery. Shigella bacteria can cope in area of very low temperatures. Campylobacter is bacteria that cause diseases in animals and human being, and the most common bacteria that causes disease is known as campylobacter jejuni, which is a zoonotic organism and has sixteen species and six sub species (Curtis, et al., 2003, p.23).
This paper will therefore discuss food borne diseases in the sense that, food borne diseases are a widespread and growing public health problem, both in developed and developing countries. Every person is at risk of a food borne illness.
Salmonella
Salmonella is a food borne disease caused by salmonella bacteria, which enters the stomach, and can move to other organs through the blood stream if not treated promptly (Brands & Alcamo, 2005, p.81). Salmonella accounts for one of the biggest causes of food borne diseases (Beier, Pillai, Ziprin, 2004, p.8).
This bacterium is commonly found in the intestines of mammals, birds, and reptiles. In addition, Salmonella poisoning causes, gastroenteritis, vomiting, and fever mainly attack the stomach and intestines causing diarrhea (Curtis, et al., 2003, p.70); and if not treated in good time, it can result to chronic arthritis, which is a painful and expensive disease to treat.
Salmonella poisoning can also cause severe illness in elderly persons, infants and persons with low immunity. A very small amount of salmonella has the capability to cause infections to human beings, hence making the diseases very common. Unfortunately, there is no vaccine for the disease and some strains have developed resistance to the available drugs.
However, Salmonella is not a contagious disease but contact with surfaces that are contaminated may result to infections. Moreover, incubation duration of salmonella is eight to seventy two hours and does not cause many fatality cases; however, in immune compromised persons, it leads to death.
Food sources
Animal and non-animal food sources can transmit salmonella bacteria. Poultry is a reservoir of salmonella in human being due to the ability of salmonella to proliferate in the intestines of poultry (WHO and FAO, 2002, p.56). Primarily, cattle and chicken products are the most common type of food that transmits this bacterium.
Eggs shells can collect these bacteria and some species have the ability to penetrate through the shell. In addition, the bacteria can affect fish products from oceans and lakes; shellfish, oysters, clams and mussels. Oysters have the greatest risk since they are often eaten raw. (Brands & Alcamo, 2005, p.29)
Other non-animal products that spread this bacterium are fruits and vegetables such as cantaloupes, melons, tomatoes, lettuce, peanut butter, and alfalfa sprouts. Additionally, Curtis, et al (2003, p.71) asserts, “Fermented meat products have been implicated to contain salmonella.”
Generally, agricultural products are contaminated through either irrigation with water that is contaminated with animal waste, use of animal manure as fertilizer and farm workers who could be contaminated with salmonella. Marijuana plant leaves also contain salmonella bacteria transferable by only touching of the leaves.
Outbreaks of salmonella
In 1997, CDC recorded 401 cases of salmonella in 41 states that was linked with uncooked potpies. In 1985, there was al large outbreak of salmonella resulting from contaminated milk, with 16, 000 cases reported; while in the same year in the UK, there was also an outbreak linked to milk products. In another case, contamination of ice cream in 1994 resulted to one of the largest number of cases; 224,000 (Curtis, et al., 2003, p.71).
Prevention
According to Beier, Pillai and Ziprin (2004, p.4), lowering of contamination from fecal matter of surfaces and food reduces the spread of salmonella. One method of preventing contamination is by cleaning all fruits and vegetables before eating or cooking.
In this case, most of bacteria are destroyed if food is cooked at the right temperature and required duration. In addition, raw eggs and poultry products should be avoided, while proper storage of food in refrigeration, meat products should be separate from vegetables, and defrosting of frozen food should be done in water or microwave and not in room temperature.
Cleaning of hands after handling pets or other animals waste must be emphasized, since the waste could be contaminated. In developing countries where human beings share water points with animals, the watering points should be monitored to ensure that the water is not contaminated. Other measures that can be applied to prevent an outbreak of salmonella are vaccination of poultry, and culling of infected poultry. Movement of animals during an outbreak should also be restricted to avoid further spread of the disease.
Shigella
Shigella bacteria cause an infection known as shigellosis, which results from ingestion of less than a hundred bacteria. The bacteria thrive in the intestines of human beings. Shigella is highly infections as it require very few organisms to cause an infection; and the incubation period of shigella ranges between 12 hours to seven days (Curtis, et al., 2003, p.124).
The symptoms of shigella infection include diarrhea that is blood stained with mucus, stomach cramping, headache, and fever. There is increased resistance to antibiotics due to mutating of these bacteria; hence, vaccination is seen as an option of countering the infections. However, Shigella is believed to confer immunity if a person was exposed repeatedly to shigella in the first five years of life (Dworkin, Falkow, 2006, 114).
Path of infection
According to (Dworkin and Falkow (2006), the path of infection of shigella is through fecal-oral route (p.115), and one mode of transmission is through contact of person-to-person. It can also be transmitted through certain sexual activities if proper hygiene is not taken into account. For instance, men who have sex with other men are likely to pass shigella bacteria, while young children are more likely to get the disease since they are not toilet trained.
In addition, insects like flies that are bred in fecal material that is contaminated can transmit and contaminate food products. Other modes include recreation activities or drinking contaminated water and vegetables grown with water or manure from animals that is contaminated. However, antiboitherapy can be used to control the spread of shigella as it shortens the duration of shigella excretion.
Outbreak
According to CDC database, in 2009, the number cases reported to be infected were children of four years and below, while the cases of fatality occurred in persons with fifty years and over.
However, the number of reported cases was lower compared to the previous surveillance period – 1996 to1998. On the other hand, the number of laboratory incidences reported in 2009 was 17,468. Moreover, in 1994, there was an outbreak of food borne disease caused by shigella in Europe traced from iceberg lettuces imported from Spain (Curtis, et al., 2003, p.124).
Prevention
Proper washing of hands with soaps for all persons and especially young children is one technique that can be used to prevent shigella. The water points and distribution system should also be secured to avoid contamination from sewage system. In addition, disposal of feces should be done in a proper manner so as children do not reach surfaces contaminated with feces (Dworkin, Falkow, 2006, p.115).
It is always important to ensure that water should is treated or boiled before being declared safe for consumption. Food should also be prepared in hygiene area and properly cooked, and stored in places where it cannot be contaminated by flies and other insects. Lastly, waters in recreational facilities like swimming pools should be treated using chlorine to destroy bacteria, and if there is an outbreak in a region, the government should control or ban all public recreations facilities from use, as well as the public eateries.
Campylobacter
Campylobacter infections are likely to be more prevalent during the warm seasons than during the cold seasons. Normally, the incubation period of campylobacter ranges between one and eleven days (Curtis, et al., 2003, p.24).
In most cases, the young children and young adults are at higher risk of attack compared to the older age group while men are frequently attacked compared to women. Moreover, it is estimated that 13 cases are diagnosed in every 10,000 persons in a population, though there are many cases that are never reported (Center for disease and control, 2010).
Path of infection
Humans are infected with campylobacter bacteria through food from animals, close contact with pets and recreation activities in contaminated waters (Nachamkin, Szymanski and Blaser, 2008, p.627). Transmission from animals occurs due to contact with feces from an infected animal; however, poultry and their products have the highest potential of containing campylobacter.
In addition, raw milk, pork, beef, lamb, and seafood are also linked with this bacterium. Moreover, bird pecked milk is associated with transmission of campylobacter (Curtis, et al., 2003, p.26). Generally, birds can transmit campylobacter to other birds through watering systems; these bacteria are mostly found in the intestines or the liver of poultry.
Milk is contaminated if the udder of cows contains the bacteria or the milk is polluted with animal waste from infected herds, while water sources and bodies are contaminated through feces from infected birds and animals. In addition, human beings working in farms can act as vectors of the campylobacter and transfer the bacteria in their bodies (Curtis, et al., 2003, p.29). In most case, Campylobacter jejuni can be transmitted by flies bred in feces that are infected with campylobacter. In addition, campylobacter has been identified to exist in sewers and mud.
Outbreaks
The outbreaks of campylobacter are sporadic. Data from CDC indicated that the number of campylobacter outbreaks have reduced by 30% in 1996-2005. The graph below indicates the number of outbreaks recorded in United States. The black bars indicate outbreaks caused by other food products whereas the white shows outbreak from milk food sources, grey waterborne. (Blaser, 2000, P.128)
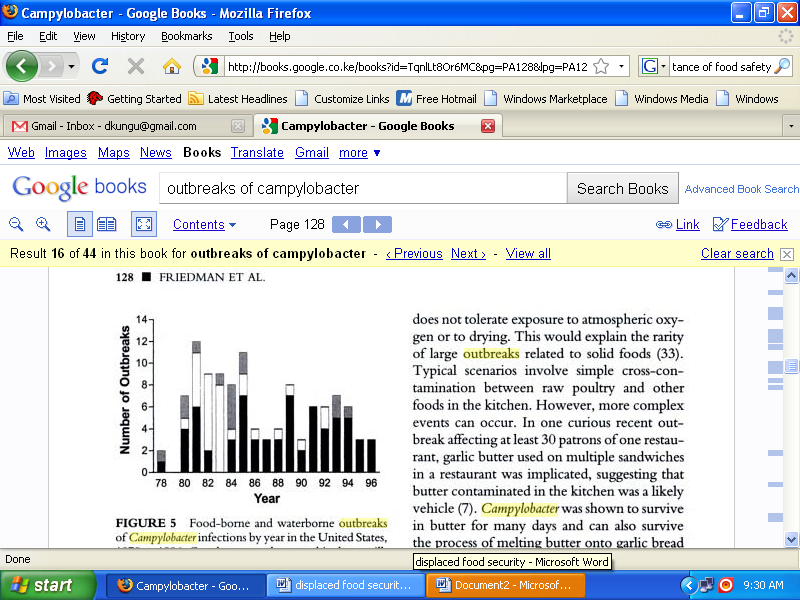
Prevention
Since poultry products account for the largest spread of the campylobacter bacteria, reducing the contamination to these products would prevent most of the spread (Curtis, et al., 2003, p.29). This can be achieved through proper hygiene practices during production in the farms and good preparation techniques by the consumers. Prevention of contamination of poultry products during processing is very crucial; thus, slaughterhouses and refrigeration systems should be kept hygienic.
Refrigeration of food also destroys campylobacter since the bacteria cannot survive in cold environment – they flourish in room temperature and multiply in contaminated foods. Since the bacteria are sensitive to heat, cooking of foods at the right temperatures can kill them. Moreover, disinfecting of rearing areas and processing plants i.e. slaughterhouses using chlorine and pasteurization of milk destroy campylobacter, mainly due to the fact that Campylobacter is sensitive to drying agents or conditions.
Importance of food safety
Food poisoning can bring serious ailments and damage of body organs or lead to fatality. The economic loss associated with food poisoning is large and can result to lack of food for the population. In addition, the annual cost of treating food borne diseases is high putting a strain on a national budget and the individuals (Gibney, 2009, p.326).
Food safety can also result to loss of income to persons who became too ill to work while companies incur loses due low productivity or absenteeism by ill worker. Food borne diseases can cause a company to collapse or suffer huge losses due to recalls of products or legal action for selling unfit products.
Some members of the population are vulnerable namely infants, elderly persons, and expectant mothers due to low immunity in their bodies. If these groups of people with low immunity are attacked with food poisoning, they are at higher risk of getting the diseases. Economically, outbreaks in a region may result to banning of food products from that region, hence affecting the economy of the region.
Food security of is very low in many countries especially developing ones, and food borne disease outbreak can result to lack of food for the bloated population putting stress to the little available food. Monitoring and surveillance of food borne diseases in regions where food is produced or imported from is therefore a sure way of preventing spread of the diseases. Moreover, the nutrition requirements of diets can be affected especially in developing countries where there is food shortage (Gibney, 2009, p.324).
Conclusion
According to Veenema (2007, p.189), “food borne illnesses are defined as diseases, which are usually either infectious or toxic in nature, caused by agents that enter the body through the ingestion of food.” The occurrence of food borne diseases is mainly caused by either contaminated water or food.
Water can be contaminated by pathogens that cause food borne diseases if it is exposed to contaminated fecal matter from animals. However, the epidemiology of some pathogens that cause food borne diseases is still unknown; hence, it is difficult to treat, thus leading to a huge threat to public health (Beier, Pillai, Ziprin, 2004, p.8).
In addition, food borne illness and food safety concerns may result to risks of malnutrition especially in developing countries, leading to high mortality (Gibney, 2009, p.324). Outbreaks of food borne diseases have the capacity of causing catastrophic effects on the economy of agriculture and food distribution industries. However, food safety can be prevented and controlled through proper surveillance of production, processing, and distribution of food products.
Germ-negative pathogens are bacteria that turn pinkish in the Gram stain test; most of these pathogens are harmful to the host. They are commonly found in animal guts and are transmitted to human beings through contact infected with fecal matter. They have the ability to mutate and hence get resistant to the available antibiotics. Most of these bacteria are capable of living and growing in aerobic and anaerobic conditions.
Early detection of an outbreak can reduce the spread of the disease by putting up measure that will prevent further spread. Educating people on ways of handling, storing and preparing foodstuff can counter the outbreaks of food borne diseases. This is because the increases of incidences of food borne diseases is due to change in the food supply chain; food production, methods of processing, length of duration of distribution, food preparation and storage methods.
Therefore, given that the diseases can cause long-term effects on the health of population, regular inspections of meat products should carried out by qualified vets to establish if the product is fit for consumption before it goes to the market, while the governments should control and monitor GM foods as they can cause food borne diseases.
Some factors that may cause an outbreak of food borne disease are; disasters i.e. floods and earthquakes, globalization of trade and travel, changes in food production system and consumer demographic. (Veenema, 2007, p.189) Both people living in developed and developing countries are exposed to food borne diseases. It is very difficult to contain outbreaks of food borne diseases in some settings like in refugee or displaced people’s camps.
References
Beier, R., Pillai, S. & Ziprin, R. (2004). Preharvest, and postharvest food safety: contemporary issues and future direction. NY: Wiley-Blackwell.
Blaser, M. (2000). Campylobacter/. NY: ASM Press.
Brands, D. & Alcamo, I. (2005). Salmonella. CA: Infobase Publishing.
Center for disease and control. (2010). Preliminary FoodNet Data on the Incidence of Infection with Pathogens Transmitted Commonly Through Food. Morbidity and Mortality Weekly Report, Vol. 59, No. 14, pp. 418-422. Retrieved from https://www.cdc.gov/mmwr/preview/mmwrhtml/mm5914a2.htm
Curtis, L. et al. (2003). Micro- Facts. London: Britain Royal Society of Chemistry.
Dwokin, M. & Falkow, S. (2006). The Prokaryotes: A handbook on the biology of Bacteria: proteobacteria: Gamma subclass. Singapore: Springer.
Gibney, M. (2009). Introduction to Human nutrition. Singapore: Wiley-Blackwell.
Nachamkin, I., Szymanski, C. and Blaser, M. (2008). Campylobacter. NY: ASM Press.
Unnevehr, L. and Hirschhom, N. (2000). Food safety in developing countries. NY: World Bank publication.
Veenema, T. (2007). Disaster nursing and emergency preparedness: for chemical, biological, and radiological terrorism and other hazards. NY: Springer Publishing Company.
WHO & FAO. (2002). Risk assessment of Salmonella in eggs and broiler chickens. Geneva: FAO publishers.