Introduction
The organisation under analysis is a Hospital located in Abu Dhabi, United Arab Emirates. It has a diverse range of healthcare businesses under its wing, such as, pharmaceutical services, scientific services and general health treatment. The focus of this paper will be on the Electra Street branch of Lifeline Hospital. The company has a reputation of high quality healthcare provision as seen through the Joint Commission International accreditation and the Sheikh Khalifa Excellence award. The assessment will look at the effectiveness of the company’s Lean strategy.
Institutional and quality program background
The program that was implemented at Lifeline Hospital was Lean production; it is also known as the Toyota System. Prior to implementation of the program, the company received moderate responses about patient satisfaction levels. Furthermore, patient waiting times were equal to local industry standards, but the firm wanted to meet international specifications. The high number of foreign nationals in the country put pressure on the organisation to look beyond the region for standard setting. Besides patient waiting times, the hospital also intended on reducing readmission rates. Therefore, this analysis will centre on those three objectives: increasing patient satisfaction, reducing patient waiting times and reducing hospital readmission rates
Lean systems started in the automobile industry from Toyota Motor Corporation. The management philosophy emphasises the elimination of inconsistencies and waste through eradication of unnecessary processes. Although this process is quite suited to the manufacturing industry, several hospitals and healthcare facilities have adopted and customised it for themselves (Manos et al., 2006). In healthcare provision, institutions tend to dwell on the customer as the main indicator of quality.
In lean thinking, organisations need to think about the methods and processes that cause them to meet customer needs. In this course, companies need to identify activities that lead to delays. The organisation can carry out a process flow analysis in order to identify value adding work and non value adding work. The main point of emphasis is the reduction of waste. Waste may lead to cost increases, unfavourable customer experiences, low quality services, time wastage as well as availability of fewer resources for improvement.
At Lifeline Hospital, the company started with a root cause analysis. It followed the five whys of lean systems. Here, the company identified the root causes of the problems it was facing. It looked at the processes, people and tangibles that led to its current predicaments. The company also worked on analysing all the potential sources of waste and they included: material flow, patient motions, excess inventory, overcorrection, overcapacity, and waiting. After carrying out this analysis, the company found that most of the problems centred on patient waiting times. It was also found that readmission rates were too high. This was the reason why Lifeline settled on the above as areas of improvement. The organisation also realised that if it boosted these aspects, then it would increase patient satisfaction levels. Therefore, the latter aspect was also included in the quality improvement method.
Data collection method
This research will involve an analysis of patient satisfaction levels from the lean improvement system at Lifeline Hospital. Patient satisfaction levels are an important indicator of whether a hospital is meeting its quality improvement goals. Since these institutions are set up in order to meet patient needs, then an assessment of their opinion about the services should be the main focus. A number of analysts have asserted that patient satisfaction ratings are not to be relied upon in quality assessments because patients are too easily pleased by even the slightest changes.
However, other critics also note that when patient satisfaction analyses are used in combination with other data collection techniques, then they can provide crucial insights about a hospital’s ability to meet their needs. High patient satisfaction indicates that the company is committed to its clients and it has a firm grasp of what they need. The research will also look at patient waiting times. Long waiting times are symptomatic of poor quality. When patients wait for too long, they may get dissatisfied with the hospital and even their patronage may decline. The hospital may loose them to other competitors (Backer, 2002).
Alternatively when waiting periods are too long, some patients may fail to comply with certain directions given by medical professionals, thus undermining their safety and health. Lastly, the research will assess the readmission rates. Patient readmissions are deemed as depictions of system failures or inadequacies in the quality provided by an institution. When readmissions occur due to obvious or preventable errors, then quality in service provisions is likely to go down. A vigilant and quality-centred institution should not have high readmission rates. Since the three objectives are quite distinctive, then they will necessitate the use of various data collection methods. In other words, this study will employ mixed methods. All of them will be quantitative analyses.
An observational method will be used for patient waiting times. Here the time it takes for patients to enter the hospital and see physicians will be recorded (Manos et al., 2006). A patient will be asked to participate in the study. If the patient accepts, then a stop clock will be used to measure the time it takes him or her to see a physician from the time he or she enters the hospital. It should be noted that patients in the hospital always go to the reception first. Since the latter is located at the entrance, then it can be assumed that it is the entry point. However, if there is a queue at the reception, then waiting will start from the door.
Some patients may not necessarily need to pass through the reception if they are coming for scheduled speciality services such as EEGs or laboratory tests. Such individuals will not be included in the study. Patient waiting times may be measured through a myriad of ways. One may opt to measure the time it takes patients to complete their treatment cycle; that is, their entrance into the institution to their exit. Others may focus on speciality services, such as, the time it takes a patient to give a pharmacist a prescription and receive his medication, or the time it takes to enter the X ray department and get X-ray results. These aspects will not be the focus of the paper. Only door-to-physician waiting times will be considered as these are the most common and general aspects of healthcare provision.
The second data collection method will be statistical analysis. This will apply to the assessment of patient readmission rates. Since the Lean program aimed at reducing patient readmission rates, then it will be critical to assess whether this objective was reached by the Hospital. The analysis will involve an examination of patient records within the company. The time it takes an individual to get admitted will be noted and the time it takes to discharge him or her will also be noted. Thereafter, previous readmission rates will be noted. An analysis of all the readmissions that have occurred within three months will be noted. This analysis will cover the past year; that is, from June 2011 to 1 June 2012. Thereafter, a percentage calculation of the readmissions rates per admission will be done in order to assess the success of the lean method after its implementation.
The third data collection method will entail the use of structured questionnaires. This will be an analysis of patient satisfaction. The questions in the questionnaire will mostly be closed. However, there will be two open ended questions. The latter will be included in order to provide some insights about the questions asked or in order to capture some oversights that may not have been included in the multiple choice questions. The participants who will be targeted for this data collection method will be randomly collected in the Hospital. Each individual will be approached and asked whether he or she would like to participate in a short survey. They will be expected to choose responses from multiple choices and give short answers to the open needed segment of the questionnaire (White, 1999)
Development of data collection tools
The door-to-physician waiting times in the hospital can be divided into five major categories. The first one is getting to the reception; the second is registration, if a patient is new, or verification of a patient’s hospital card if the patient is an old one. Patients will be requested for participation as soon as they complete the first step. However, if there is a queue at the reception, then timing will start as soon as they sit down. For those patients who walk straight to the reception, the stop clock will commence after the patients start registration and the time they take to do that will be noted. Some of them may have to fill out forms.
Alternatively, some of them may take a minute or two if they have a card. The third category will involve the amount of time it takes patient to finish with payment processing at the payments section. A number of them may use insurance while others may prefer cash. Thereafter, nurses or other attendants will measure their vitals. The time it takes patients to complete this process will also be noted. Finally, patients will need to wait for physicians after this measurement before they can get examined. The total amount of time it takes for an individual to complete this entire process will be noted (Manos et al., 2006).. Shown below is summary of the tables that will be filled by participants.
Table on total waiting times per participant
Table illustrating patient waiting categories (Backer, 2002)
The target population involves all those individuals who use the Hospital’s healthcare services. The sample size will be 15. In order to reach such a level, then approximately 50 people will need to be approached as a number of them may refuse to participate.
The assessment of readmission rates will follow this sequence. First, all the admitted patient records will be analysed. Their previous readmissions will be noted and the reason for admissionwill also be noted. An aggregate of the total readmissions will be done. Since this will be a statistical analysis, then all the patients ever admitted in the hospital in the past one year will be considered. Therefore, the sample size will be equal to the target population. Shown is a summary of the data categories that will be collected.
(AHIP, 2012)
The last section will involve an analysis of patient satisfaction levels. In order to increase response rates, 100 questionnaires will be administered. Studies often indicate that response rates for questionnaires are around 35%. The questionnaires will be distributed by handing the survey forms to the patients directly. It will be too costly and inefficient to mail the forms to patients when they can be approached directly. All the questions except the last two will be closed ended. They will have multiple choices with five categories. Researchers are often advised to use consistent scales in order to facilitate result comparisons. All the questions will have five options on ratings: strongly agree, agree, neither agree or disagree, disagree, and strongly disagree (White, 1999).
The categories will have a score of 5, 4,3,2,1 respectively. However since patients may choose not to answer a particular question, then “no response” will be noted in the paper. Shown is a summary of the questions that respondents will answer in the paper:
Please rate this hospital on the basis of the following: Strongly Agree-5, Agree-4, Neither agree or disagree -3, Disagree-2, Strongly disagree-1.
Circle the number that captures your sentiments
Discretion
The Hospital keeps my information private 5 4 3 2 1
I would refer my acquaintances to Lifeline Hospital 5 4 3 2 1
Facility
The building is clean and well kept 5 4 3 2 1
It is easy to find where I am going in this building 5 4 3 2 1
I feel safe and comfortable in the hospital building 5 4 3 2 1
Payment
The hospital collects payment easily 5 4 3 2 1
Workers explain the hospital charges to me 5 4 3 2 1
I required to pay for necessary services 5 4 3 2 1
Workers (dentist, lab technician, nurse, radiologist, physician, physician assistant)
Workers listen to me 5 4 3 2 1
They take ample time with me 5 4 3 2 1
Employees explain to me what I ask 5 4 3 2 1
They give me proper treatment 5 4 3 2 1
Other non technical staff are helpful to me 5 4 3 2 1
Waiting
The time it takes to wait before seeing a physician is acceptable 5 4 3 2 1
The time it takes while waiting at the examination room is acceptable 5 4 3 2 1
The time it takes to perform tests is acceptable 5 4 3 2 1
The time it takes to get test results is acceptable 5 4 3 2 1
Access to care
The Hospital returns my calls promptly 5 4 3 2 1
The Hospital is conveniently located 5 4 3 2 1
The hours that the Hospital opens are convenient 5 4 3 2 1
What is the least desirable thing for you in service quality?
What do you find satisfactory about the Hospital?
Data presentation
The following were the results found on patient waiting times
The following were the results found on readmission rates for the past one year
The following were the results found on patient satisfaction
In response to the two open ended questions, the respondents stated the following about the things they liked in the facility: it is well known, the doctors are competent, it is clean, and has modern technologies. In response to the least desirable features, most of the patients felt that the hospital needed to synchronise its speciality services, doctors did not follow through on details during shift changes, and the hospital was hidden.
Interpretation and analysis of data
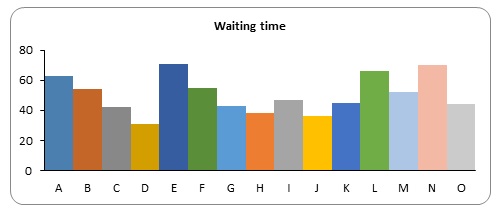
The highest waiting time was 71 minutes while the least waiting time was 31minutes. The average waiting times for all the participants was 50.47 minutes. Before implementation of the lean program, average door to physician waiting times were 60.4 minutes. Consequently, the institution has reduced its waiting times by 16.44%.
The following were the results on readmissions
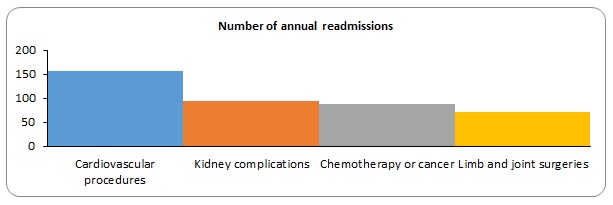
The percentage readmissions for the entire year represented 23.4% of all the admissions. This was a decrease of 4% from the previous year. (AHIP, 2012)
Lastly, the following is an illustration of the patient satisfaction levels.
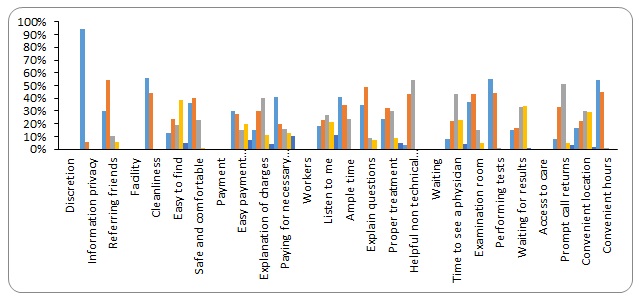
Most patients agreed with the level of discretion in the hospital. Under facilities, most patients agreed although they disagreed with the convenience of the building. Under the category of workers most agreed with their service except for non technical staff. In the ‘waiting’ category, participants were unsure about their responses except for the time it takes to test them. Lastly, most patients disagreed with access to care in the hospital.
Conclusion and Recommendations
The organisation has clearly achieved two major objectives of reducing readmission rates as well as patient waiting times. However, it has not achieved the goal of improving patient satisfaction as most participants’ responses fall in the middle category. The organisation can improve this by increasing access to the facility. It can achieve this by increasing the number of transporters around the facility. The Hospital should also market the location of the building in order to increase an understanding of the same. It should also consider some of the suggestions made by patients in the open-ended section of the questionnaire. Here, the hospital can reorganise the shift process so as to facilitate smooth transitions. It should also work on the speciality services such that patients do not have to waste time.
Although the institution recorded decreases in patient readmission rates, it can still work on improving these numbers by identifying the conditions that cause the most number of readmissions and creating programs for them. Alternatively, it can eliminate possible errors in these programs.
References
AHIP (2012). Working paper: simple methods of measuring hospital readmission rates. Centre for Policy and Research report, 1-15.
Backer, L. (2002). Strategies for better patient flow and cycle time. Family Practice Management, 9(6), 45-50/
Manos, A., Sattler, M., Alukal, G. (2006). Make healthcare lean. Quality Progress 39(7), 156-160.
White, B. (1999). Measuring patient satisfaction: How to do it and why to bother. Family Practice Management, 6(1), 40-44..