Introduction
We rarely think of the risks and consequences of acute disease, until we face it. Our bodies often warn us of an upcoming challenge, but we ignore these signs. Hypothermia is an acute health diagnosis that does not happen at once but can have devastating impacts on all human organs and systems. I could not imagine that I would ever be admitted to a hospital with hypothermia. Now I keep suffering from the damaging consequences of my mistakes because it is always better to prevent a disease than to deal with its complications.
Living before contracting the disease
I am a 79-year-old man. My wife died two years ago. Since then, I have been trying to find my way in life. Before Eleanor died, she had always cared for me. I never thought I had to cook, clean, or use the laundry machine. Everything in my life was organized. Eleanor knew that I had to care for my health. She made regular appointments with my physician and knew how I felt. She monitored how I took medicines and made sure I never missed a visit to the hospital. After her death two years ago, I could hardly understand how I would survive. Drinking became a daily routine for me. I forgot about proper nutrition and ate, whatever I could find in the nearest store. Within months, I lost nearly 20 pounds, but my emotional grief left little room for physical suffering. I simply did not notice that the tragedy was coming. Last winter, I nearly froze myself to death, as I could not find my way home. I was drunk. By the time I reached home, my hands and legs were pale, and I started to feel sleepy. This winter, the situation has been much worse: on my way to the food store, I got lost in a snowstorm. I was hungry and drunk, and it is alcohol and hunger that favored the rapid onset of hypothermia.
I must say that, as an elderly person, I face higher risks of hypothermia than my younger counterparts. According to Cire, “older people are at risk for hypothermia because their body’s response to cold can be diminished by certain illnesses such as diabetes and some medicines, including over-the-counter cold remedies.” Moreover, elderly people’s bodies do not generate enough heat to withstand extreme colds (Cire). I ignored all precautions and did not think about hypothermia. I had a few clothes on me at the time of the snowstorm. I did not wear any gloves or hats. On the same day, I was admitted to the hospital. Estimating the exact number of such patients does not seem possible, mainly because emergency departments register only the severest cases (Edelstein & Adler). Still, the rates of mortality in hypothermic patients are quite high: between 12% and 40% of patients with moderate and severe hypothermia are likely to die (Edelstein & Adler). These rates are similar for men and women, but the youngest and the oldest ones are particularly susceptible to these risks (Edelstein & Adler).
I should say, that my age was not the only risk factor for hypothermia. Certainly, age matters, because older people may not be able to communicate or move when they are cold (Mayo Clinic). However, I was also drunk, and alcohol is one of the most prevalent factors of hypothermia and poor metabolism (Mayo Clinic). Alcohol leads to the dilation of blood vessels; as a result, the body loses heat faster (Mayo Clinic). Being drunk, I was mostly indifferent as to what I was wearing, where I was going, and what could happen to me. Poor nutrition further contributed to the development of hypothermia: before the snowstorm, I had not eaten for several days, and this is actually why I left home and went to the food store.
As I said earlier, hypothermia does not happen at once. Now I can remember how I was getting cold on my way to the food store. At first, I felt how my hands, feet, and head were getting cold. My face was swelling and I could feel my skin going pale. I cannot remember whether I was shivering, but I started to feel sleepy. I did not care, because I attributed my state to alcohol and hunger. In a couple of hours, I was not able to move. I was not able to speak. I sat down in the snow because I could not walk any longer. For some reason, I decided I had to wait until the snowstorm was over. My heart was getting slower. Then, I could not remember anything, until I opened my eyes in the emergency department.
Establishing the diagnosis
I was admitted to the nearest emergency department with the following symptoms: shivering, clumsy speech, poor movements, poor decision-making and confusion, slow breathing, and weak pulse (Mayo Clinic). I was also half-conscious. I felt as if my energy had left me (Mayo Clinic). I was not quite aware of what was happening to me. Mayo Clinic suggests that individuals with hypothermia may not realize the severity of their condition, because the symptoms emerge gradually, leaving individuals in confusion. This is, probably, what happened to me, because even now I cannot remember the details of my being admitted to the hospital.
What I know is that I had to undergo all possible tests and diagnostic procedures to confirm the diagnosis. Although the circumstances of my admission made the diagnosis absolutely evident, my body temperature was measured. The nurse used a rectal thermometer, which showed 28oC (82.4oF) – a boundary condition between moderate and severe hypothermia (McCullough & Arora 2327). I should say that, in a normal condition, my temperature would have to range between 36.0 and 36.6oC (97.8oF). The ECG showed a decreased heart rate. Ventricular arrhythmias were also noted. A blood test for alcohol was made, and the blood alcohol concentration (BAC) was estimated at 0.10. Normally, such tests would show no alcohol. I do not think they measured any potassium or electrolyte levels, because the symptoms of hypothermia were too obvious. At times, patients with hypothermia may display the signs of coagulopathy, but I am not sure I had it (McCullough & Arora 2328). What they said was that I had a metabolic disorder, which made me extremely vulnerable to the risks of hypothermia. They told me I had a decreased basal metabolic rate, which could have its roots in thyroid dysfunction (McCullough & Arora 2327).
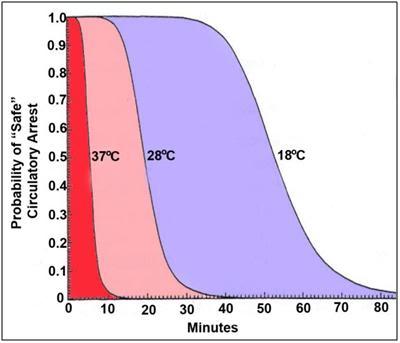
The pathophysiology of hypothermia is quite straightforward. Hypothermia is a state that affects all organs and systems: the flow of blood becomes slow, and cells no longer have enough energy to maintain their normal function. Because hemoglobin binds more oxygen at lower temperatures, all organs and systems may suffer from hypoxia. I lost most heat through radiation, convection, and conduction, coupled with respiration and active evaporation. Due to the loss of heat and low temperature, my hypothalamus could not maintain adequate levels of heat production and conservation (Edelstein & Adler). The CNS and cardiovascular system suffered the most: the cardiac output and arterial pressure kept decreasing and could lead to myocardial ischemia or sepsis (Edelstein & Adler). Low temperatures led to decreased CNS metabolism, further reducing brain activity. Every time body temperature falls by 1oC, cerebral metabolism decreases up to 10% (Polderman S187). Oxygen consumption by tissues also continued to decrease (Edelstein & Adler). Not surprisingly, I could not manage my actions and thoughts any longer. The level of consciousness was abnormally low. I was simply dying.
Treatment and prognosis
At first, the nurse removed my clothes, and I was placed under warm blankets. I was given thiamine because it has minimal adverse effects on patients with a history of alcohol abuse (McCullough & Arora 2329). Active external rewarming was used to speed up and increase body temperature. My skin was normal, and they used heating pads and hot water bottles to help me recover from the cold. A warm IV saline solution was used to warm my blood (Mayo Clinic). The intravenous solution was continuously warmed with a fluid heater to raise my body temperature through induction (Tsuei & Kearney 10). Induction is the best way to transfer heat (Tsuei & Kearney 10). Now I know that warm saline fluid is an essential element of hypothermia treatment.
As a result of hypothermia, I also developed pancreatitis and aspiration pneumonia. However, pancreatitis can also be attributed to the nutrition problems I had been facing before hospitalization. I had to spend almost one month in the hospital. Luckily, I was not admitted to intensive care. I was also lucky to avoid the most common sequelae usually left after hypothermia treatment, including renal failure and aftershock. Today, I have to monitor my nutrition and heart rate, while keeping warm and avoiding any alcohol. I have to test the levels of electrolytes regularly to prevent the risks of delayed renal failure. I believe that, due to my age and health status, the long-term consequences of hypothermia will continue to persist. I do not think I can fully recover from what happened to me, but I am happy to be alive and conscious.
Conclusion
Hypothermia is a serious health condition, which affects all organs and systems. The consequences of hypothermia can vary considerably, from milder complications to death. Hypothermia is easy to prevent, but the sequel of hypothermia treatment is likely to persist with age. An individual who once suffered from hypothermia will have to constantly monitor changes in his (her) physical health.
Works Cited
Cire, Barbara. “Hypothermia: A Cold Weather Risk for Older People.” NIH News, 2009. Web.
Edelstein, Jamie and Jonathan Adler. “Hypothermia.” Medscape, 2011. Web.
Mayo Clinic. “Hypothermia.” Mayo Clinic, 2011. Web.
McCullough, Lynne and Sanjay Arora. “Diagnosis and Treatment of Hypothermia.” American Family Physician, 70.12 (2004): 2325-2332. Print.
Polderman, Kees H. “Mechanisms of Action, Physiological Effects, and Complications of Hypothermia.” Critical Care Medicine, 37.7 (2009): S186- S202. Print.
Tsuei, Betty J. And Paul A. Kearney. “Hypothermia in the Trauma Patient.” Injury, 35.1 (2004): 7-15. Print.
Walpoth, B.H., T. Locher, F. Leupi, P. Schupbach, W. Muhlemann & U. Althaus.
“Accidental Deep Hypothermia with Cardiopulmonary ArrestL Extracorporeal Blood Rewarming in 11 Patients.” European Journal of Cardio-Thoracic Surgery, 4.7 (1990): 390-393. Print.