Abstract
Nursing is a discipline that requires comprehensive care and mutual interaction between nurses and patients in the event of service delivery. The partnership should encompass both physical and emotional (interpersonal) relations to ensure a conjoint understanding between the two parties. This essay elaborates on the orientation and assessment phases that are experienced during the nursing process. These segments are interrelated due to the existence of a relationship between the nurse and the patient. At the first meeting, the nurse and patient are strangers from different entities. The patient who shares a pressing need with the nurse initiates the interaction. After the understanding of the need, the two individuals start working together towards the desired solution. The interpersonal relationship established leads to a concept of care that is aimed at solving the patient’s health issue.
Introduction
Most nursing objectives are accomplished using various care models. An interpersonal relationship that is established between a healthcare provider and the patient forms a framework for developing feasible treatment interventions that encompass both physical, emotional, and psychological needs. A clear understanding of the interpersonal relationship theory ensures efficient diagnosis and treatment of the patient’s health issues in the hospital setup. This essay provides a conceptual analysis of comprehensive care in the health setting by providing an insight into Hildegard E. Peplau’s Interpersonal Relations Model (IRM).
Interpersonal Relations Theory in Nursing Practice
Hildegard E. Peplau developed the model of interpersonal relationships in 1952. This model is guided by various theories of needs that were advanced by philosophers such as Abraham Maslow and Percival Symonds among others. It is classified under the interaction theories because it elaborates on the relations between nurses and patients (Peplau, 1997). According to Peplau (1997), the theory describes nursing as an interpersonal relationship with the patient and caregiver. It is seen as a process that involves a mutual interaction between the patient and nurse based on therapy. However, the healthcare provider has to be willing to help the patients to meet their desired needs. Therefore, the two individuals must have a common goal to achieve (Peplau, 1997). They are bound to show respect towards each other besides being ready to learn and educate one another during their interactions. There is a matureness nurturing technique that is acquired through education, therapy, and the interpersonal processes that occur during the interactions between the nurse and patient (Peplau, 1997).
Framework for Interpersonal Relation
In the context of the nurse-patient relationship, the framework for the human relations concept focuses on the need, feeling, and ideas of both the patient and nurse. Through interaction, a common goal is set that details the process of seeking realistic health solutions (Peplau, 1997).
Explanation of the Framework
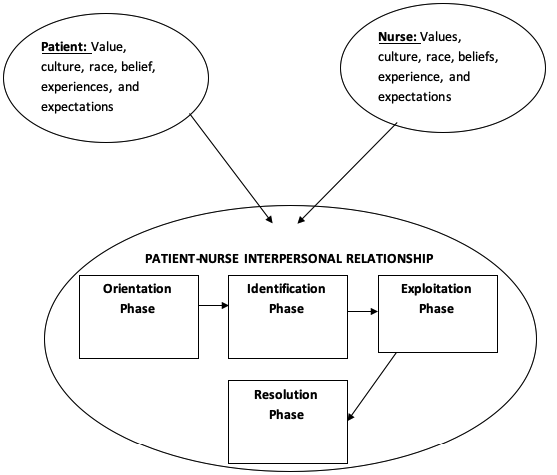
Before the interpersonal relationship between the patient and nurse is initiated, both parties have differences concerning values, experiences, and cultures among others. However, when the relationship is established, it undergoes a series of phases. The first phase is known as the orientation phase. In this state, there is a need that is felt by the patient. This need develops an urge for seeking assistance from the nurse. In this case, nurses start by ensuring that the patients recognize their problems in detail. Next, they determine various techniques that will be used to solve health problems (Peplau, 1997). The second phase involves identification of the values, beliefs, and healthcare atmosphere among other factors that promote the interactive process. The patients form relationships with nurses who are charged with the responsibility to help them achieve their health needs. The caregivers have to create an atmosphere that strengthens the beliefs of the patients. As a result, the patient should feel a sense of belonging by being involved in the goal-setting process actively (Peplau, 1997). The third phase is the exploitation of information. In this stage, the patient must seek knowledge about the relevant nurses who can lead the healing process. It also involves the formulation of new goals by either the nurse or patient. Lastly, there is a resolution phase whereby patients form new goals after the other goals have been achieved. The stage sets the termination of the relationship between the patient and the nurse (Peplau, 1997).
Importance of the Interpersonal Relations Theory concerning Knowledge Advancement
Many nurses have implemented the interpersonal theory due to the concepts concerning the healing of patients that it lays (Arnold & Boggs, 2015). The following are ways through which the theory has contributed to the nursing profession. This theory views the nurse as a stranger who possesses the mandate to welcome any ill individuals. According to Arnold and Boggs (2005), the nurse must noteworthy attributes such as excellent communication skills, etiquette, and courtesy among others. The theory further portrays nurses as resource persons who should be relied upon to provide solutions to underlying problems that affect patients and colleagues.
In the context of the model of interpersonal relations, nurses also play the role of teachers. A consistent learning process takes place between the nurse and patient during mutual interaction. The patients seek more information from the nurses who educate them on their predicaments. Therefore, the patients learn both formally and informally. Nurses are also surrogate caretakers. In most cases, nurses take care of the patients with a motherly love (Arnold & Boggs, 2015). As a result, they are viewed as substitute parents of the patients. Another knowledge that is gathered through this theory is the technical ability of nurses to handle equipment seamlessly and give physical care to patients among others (Arnold & Boggs, 2015). Also, nurses are leaders in healthcare facilities. Therefore, knowledge about the model of interpersonal relations equips them with some leadership skills that are essential for performing their caregiving responsibilities. Lastly, the interpersonal relations theory implies that nurses are counselors. Due to the adverse experiences of the patients, the nurses are in a better position to heal them emotionally through proper counseling. Other duties that are carried out by the nurses include management, administration, record keeping, researching, mediation, and health advocacy among others.
The Concept of Nursing (Primary Care) concerning the Interpersonal Relations Theory
The interpersonal relations theory elaborates that the nurse must ensure that the patients identify their problems. Through set principles, the nurses should apply the appropriate techniques to solve the problems that the patients experience (Orem, 2001). The concept of primary care concerning the interpersonal theory of nursing helps the nurses to make the relationship productive. It brings on board four distinct features that entail the patients, the curing environment, health, and the nurses (Orem, 2001). In the context of such characteristics, the patient refers to the person who needs a solution to a pending health problem. Health implies the normality of a person. The environment is viewed in the context of culture and routines that must be followed by the patient. Nursing is a therapeutic service that is offered to patients with a view of realizing their recovery. The nurse carries out the implementation of interpersonal relations and technical procedures (Orem, 2001).
Model Case
A model case is an example based on real-life concepts that are implemented to show all the attributes. The following scenario shows the actual scene that includes all attributes that are in the nursing concept (Tilley, 2008).
Mary is currently a registered nurse who graduated from a nursing school six years ago. However, she joined a private hospital immediately as a gynecologist with a ratio of 1:4 patients. The anonymous healthcare setting prioritizes comprehensive care based assessment and counseling. Mary enjoys her work life due to the rapport that she has developed with the patients. The affirmative feedback that she receives from both her patients and the hospital about comprehensive care compliments her responsibilities as a nurse. Nurse Mary’s action to take care of the patients at all times by paying attention to their culture, ideas, and the environment for improvement demonstrated a comprehensive care concept.
A Related Case
A related case represents a nursing concept that has similar attributes in a different set up (Tilley, 2008). In this scenario, Paul is a registered practitioner who is employed as a surgeon in a separate hospital. His experience with patients for seven years in a long-term care setting has earned him adequate skills to counsel patients, perform a comprehensive assessment, and care delivery. Paul loves the nursing environment where he continuously interacts with the patients. This situation demonstrated a highly regarded patient care responsibility (Tilley, 2008).
Illegitimate case
A case is illegitimate when an action that is done by a health practitioner is contrary to the required nursing interventions. Other nurses can testify that the executed action using facts to disapprove the inappropriate care activities (Tilley, 2008). A case scenario is seen where Nurse Philip is supposed to attend to a new patient in a surgical ward. The qualifications of a practitioner require a vast experience of at least five years in practice. However, Philip’s credentials clearly show that he is a fresh graduate who needs more experience to conduct counseling and interpersonal relationship practices. Against the protocols of the healthcare institution, the nurse goes ahead to handle the patient. However, several nurses confirm that his experience is below the required standards to handle the patient and the action is stopped.
Measurement of the Concept
The concept of comprehensive care can be measured using various assessment tools that include nurse-client, facility, providers, and/or health system surveys among others. The information obtained from such surveys can be used to evaluate the quality of delivery of the core concept of the health system (Punch, 2013).
Nominal Measurement
Various variables that include gender, race, religion, and marital status have features that only meet the minimal criteria that are required. Upon thorough examination, such variables lead to logical grouping. As a result, they can have mutually exclusive attributes (Punch, 2013). Ranking these variables cannot be achieved mathematically. For example, assume the examination of a questionnaire with a question about the marital status of a patient using the Likert scale where 1 represents ‘never married’, 2 ‘widowed’, 3 ‘divorced or not married’, 4 ‘married but separated’, and 5 ‘currently married’ is to be marked. When the response is 1, it does not indicate that it is three times higher or lower than 2, which represents that the patient is widowed. The numbers on the Likert scale only indicate categories (Punch, 2013).
Ratio Measurement
Variables that contain information about weight, level of income and temperature among others can be measured using ratios. For example, the number of patients in a hospital can be related to the number of nurses in the facility to determine the nurse-patient ratio. This situation has a mathematical meaning that can be used by the management to solve issues that pertain to staffing, bed capacity, and/or reduction of expenses (Babbie, 2015).
Application of Comprehensive Care
Victoria is a nurse works in both hospital and home-based care settings. The nurse knows that comprehensive care is mandatory for patients constantly. She encounters many patients at home and the hospital among other places. However, most of the patients are afraid of their conditions due to the surrounding healthcare settings that do not give weight to primary care. The patients rely on Nurse Victoria who delivers comprehensive care to promote their wellness (Adashi, Geiger, & Fine, 2010).
Victoria has a plethora of skills in nursing. As a result, she ensures that the patients are healed both spiritually and emotionally by engaging them in counseling sessions in the course of care delivery. She realizes that her relationship with the patients is interpersonal and each one of them needs her around the facility (Adashi, Geiger, & Fine, 2010). The nurse also observes care as an activity that is centered on love, dignity, and humanity in the event to alleviate the poor condition of the patient. This kind of care should be holistic and must cover issues that pertain to support, protection, correction and/or healing of the mental, physical, social, and spiritual aspects that surround the patient. To ensure that she delivers comprehensive care efficiently, Victoria handles the patients with compassion, tenderness, gentleness, and love among others attributes apart from giving therapeutic medications (Adashi, Geiger, & Fine, 2010).
Interventions: Evidence-Based
In most cases, many people only perceive care as a part of clinical services that are accorded to patients rather than an activity that is hooked on evidence-based interventions. To ensure that thorough comprehensive care intervention is offered to patients, a state of art activity must be integrated into evidence-based clinical interventions. Clinical solutions must be proven through scientific backing (Friedman, 2001; McEwen & Will, 2014). Although many practitioners perceive evidence-based interpositions as alternative ways, they should only complement comprehensive care concepts with a view of boosting the quality of treatment because they serve as resources for advanced knowledge (Friedman, 2001). Policymakers should also ensure that health regulations address the inclusion of complementary evidence-based techniques to comprehensive care delivery (McEwen & Will, 2014). If the comprehensive care that is offered to the patient does not need evidence-based interventions, then common sense and experience must be used together with clinical interventions (Friedman, 2001).
Conclusion
The essay has elaborated on the concept analysis of comprehensive care nursing concerning Peplau’s theory of interpersonal relations. It has been noted that this theory underpins the idea of comprehensive care due to the rapport that is developed between the patient and nurse. Interpersonal relationships result in the delivery of efficient therapeutic interventions to patients since nurses execute talents that are interrelated, professional, and dynamic as leaders and counselors who are responsible for the health of others. However, a comprehensive care plan should be complemented with evidence-based techniques to ensure an all-encompassing healing environment.
References
Adashi, E., Geiger, H., & Fine, M. (2010). Health care reform and primary care: the growing importance of the community health center. New England Journal of Medicine, 362(22), 2047-50.
Arnold, E., & Boggs, K. (2015). Interpersonal relationships: Professional communication skills for nurses. Elsevier, BV: Elsevier Health Sciences.
Babbie, E. (2015). The practice of social research. Boston, MA: Cengage Learning.
Friedman, R. (2001). The practice of psychology with children, adolescents, and their families: A look to the future. New York, NY: Oxford Press.
McEwen, M., & Will, E. (2014). Theoretical Basis for Nursing. New York, NY: Lippincott Williams & Wilkins.
Orem, D. (2001). Nursing: Concepts of practice. Elsevier, BV: Elsevier Health Sciences.
Peplau, H. E. (1997). Peplau’s theory of interpersonal relations. Nursing Science Quarterly, 10(4), 162-7.
Punch, K. F. (2013). Introduction to social research: Quantitative and qualitative approaches. Newcastle: Sage.
Tilley, D. (2008). Competency in nursing: A concept analysis. Journal of continuing education in nursing, 39(2), 58.