Asthma is a chronic condition that is similar to other obstructive lung diseases, but its main symptoms affect a person’s bronchi, and they can be reverted. Asthma can be intermittent and persistent, its severity depending on a variety of genetic, environmental, and individual characteristics (Bonsignore et al., 2015). However, acute asthma exacerbations, commonly known as asthma attacks, can occur in all patients. The pathophysiology of this disorder involves one’s response to an antigen and a subsequent reaction of the body in the form of inflammation, bronchospasm, and airway obstruction (Huether & McCance, 2017). This process, as well as treatment options, can be affected by a person’s genetic predisposition and family history of asthma.
Pathophysiology
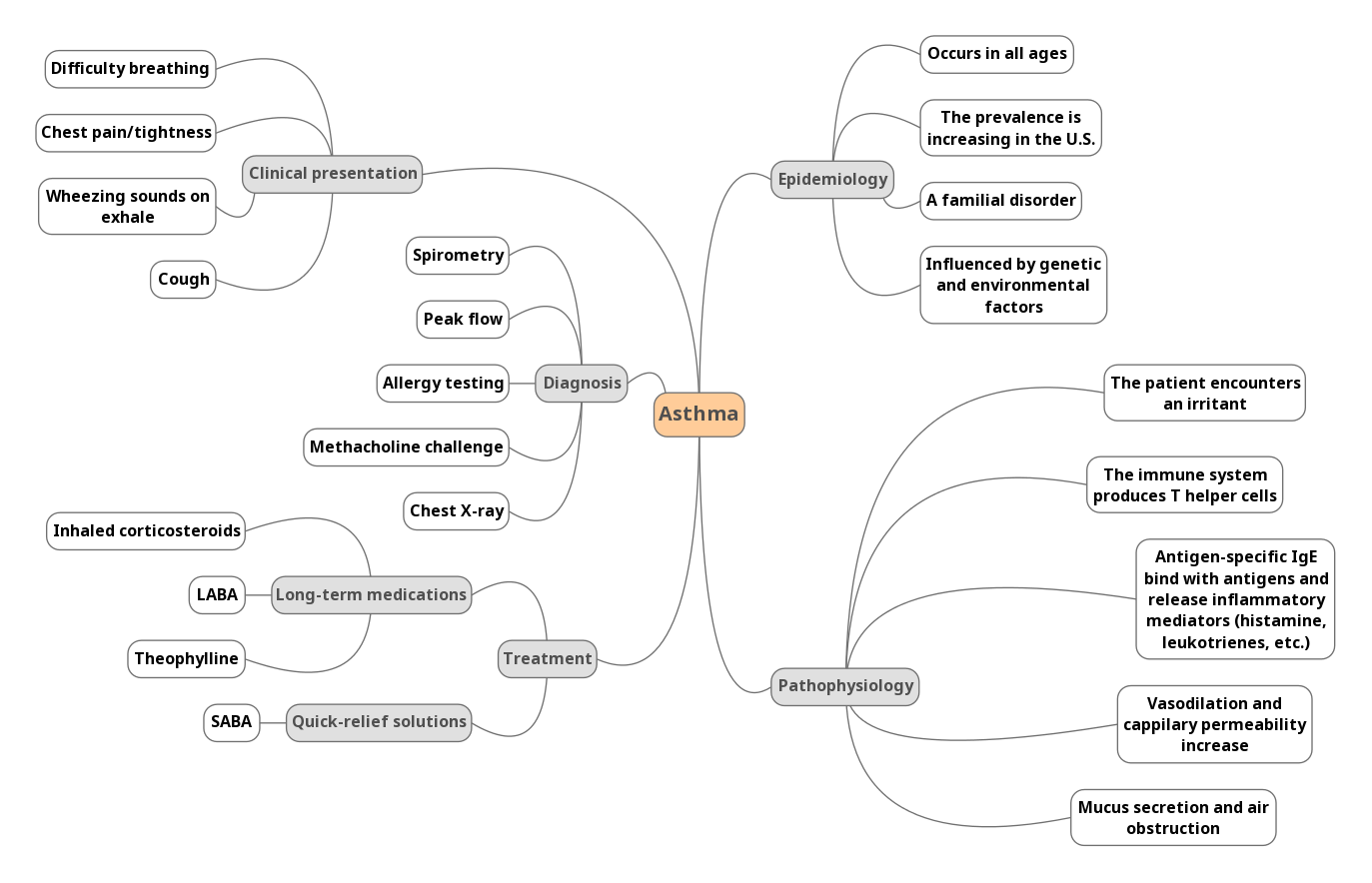
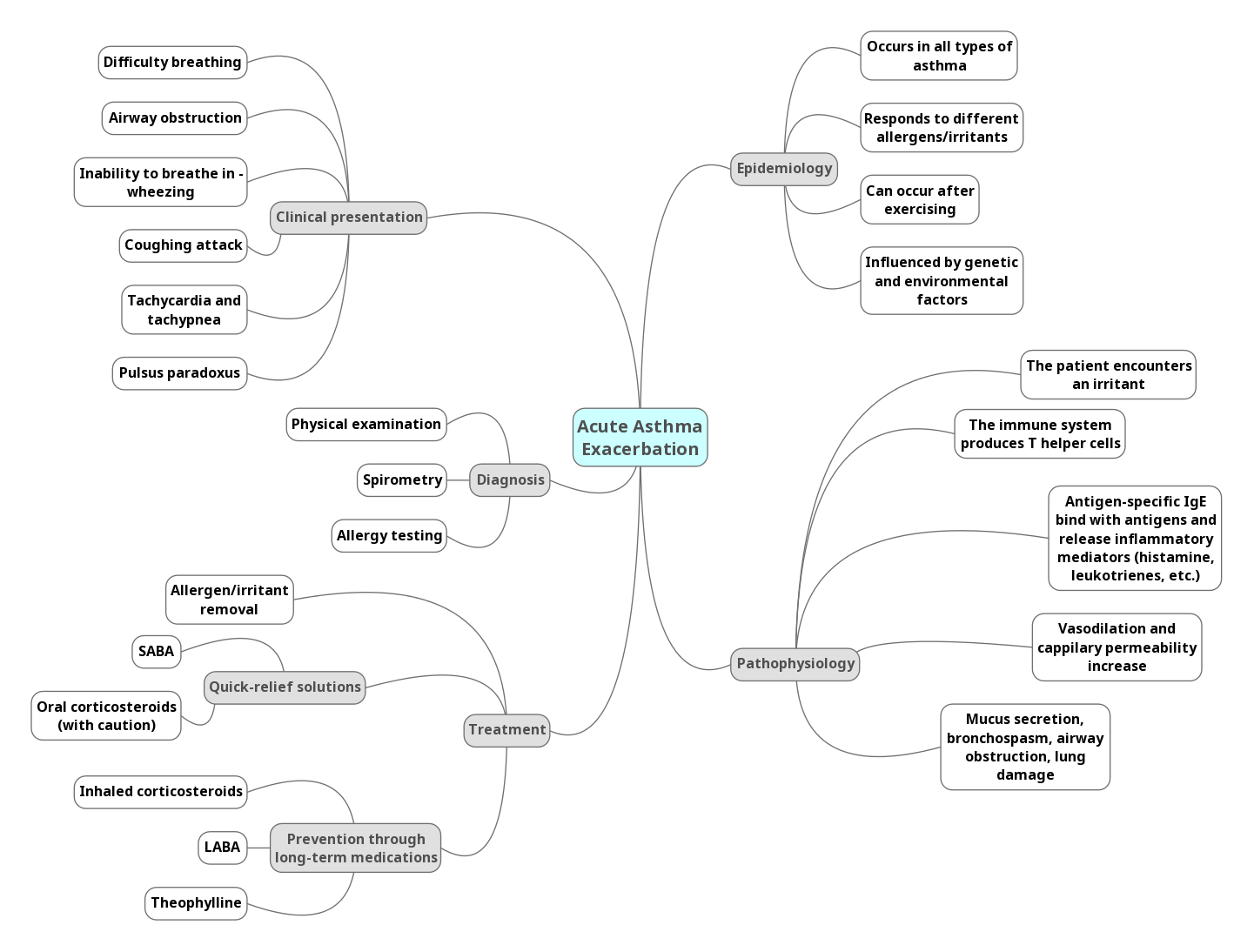
Chronic asthma can differ in its severity from one patient to another. The symptoms in patients with mild asthma, for example, may not appear daily or even weekly, while individuals with the severe form can continuously struggle to breathe properly (Hammer & McPhee, 2014). However, the pathophysiology of this condition is similar for all types. First, the individual with a sensitized immune system encounters an allergen or an irritant. Then, the body reacts in two ways, producing a fast and slow response.
In the early stage of asthma, the immune system activates T-helper cells (T-helper 2 lymphocytes) which start the process of inflammation. In turn, plasma cells (B lymphocytes) are stimulated during the inflammatory onset release IgE that are specific to the type of allergen for the body. A reaction between these IgE molecules and the antigen leads to the rising levels of histamine and other vasoactive mediators. They cause an increase in capillary permeability and vasodilation. As a result, the lungs suffer from bronchospasms (smooth muscle contractions), mucus secretion, and congestion (Huether & McCance, 2017).
The late response is characterized by another release of mediators that repeat the same processes causing edema, bronchospasm, and mucus production. However, in this case, this reaction can cause severe damage to the lungs if left untreated. The trapped air creates different areas of pressure in the organ and changes the lungs’ resistance to the airflow. As an outcome, alveolar gas pressure increases, while perfusion decreases, and hyperventilation may lead to respiratory failure (Huether & McCance, 2017). This is a long-term manifestation of chronic asthma that should be treated as well.
Patient Factor
Genetics plays a vital role in a person’s history of asthma. According to Ferreira et al. (2014), multiple variants identified in people’s genomes can exacerbate the probability of having asthma. Moreover, they can also increase one’s resistance to usual treatments. For example, Ferreira et al. (2014) find that some phenotypes lead to patients having both hay fever and asthma, and these variations are more common than those which cause only one of the two conditions. Meyers, Bleecker, Holloway, and Holgate (2014) argue that the factor of genetics also influences patients’ severity of asthma, susceptibility to medication, and their response to various drugs. The authors propose creating an individual plan for each patient based on their genotype. For example, the use of short-acting beta2-adrenoceptor agonists (SABA) as relief for bronchoconstriction may produce varying results for patients with different phenotypes (Meyers et al., 2014).
A simple therapy plan that does not include one’s phenotype diagnostics can consider the effectiveness of medications based on family history and physical examinations. Treatment includes long- and short-term solutions focused on symptom management. Long-term medications are used to control asthma and lower the potential for future attacks. They include inhaled corticosteroids, long-acting beta2-adrenoceptor agonists (LABA), and theophylline. Short-term drugs such as SABA provide quick relief and should not be used for long periods.
Conclusion
Chronic asthma affects one’s bronchi and leads to airway constriction. Severe asthma exacerbations and failure to treat persistent symptoms can result in the infliction of substantial damage to one’s lungs and future respiratory failure. Genetics affects the development of asthma significantly, which family history being one of the risk factors for this condition. A healthcare provider should consider the patient’s family members and their health to develop an individual plan that will recognize genetic predispositions.
Mind Maps
References
Bonsignore, M. R., Profita, M., Gagliardo, R., Riccobono, L., Chiappara, G., Pace, E., & Gjomarkaj, M. (2015). Advances in asthma pathophysiology: Stepping forward from the Maurizio Vignola experience. European Respiratory Review, 24(135), 30-39.
Ferreira, M. A., Matheson, M. C., Tang, C. S., Granell, R., Ang, W., Hui, J.,… Hopper, J. L. (2014). Genome-wide association analysis identifies 11 risk variants associated with the asthma with hay fever phenotype. Journal of Allergy and Clinical Immunology, 133(6), 1564-1571.
Hammer, G. G., & McPhee, S. (2014). Pathophysiology of disease: An introduction to clinical medicine (7th ed.) New York, NY: McGraw-Hill Education.
Huether, S. E., & McCance, K. L. (2017). Understanding pathophysiology (6th ed.). St. Louis, MO: Mosby.
Meyers, D. A., Bleecker, E. R., Holloway, J. W., & Holgate, S. T. (2014). Asthma genetics and personalised medicine. The Lancet Respiratory Medicine, 2(5), 405-415.