Introduction
The human body highly depends on food for survival because various nutrients play different roles in maintaining one’s wellbeing. Metabolism is the process by which the food ingested is processed into energy. An element everyone needs to engage in various activities. Meals mainly comprise fats, carbohydrates, and proteins, which are broken down in the digestive system with the aid of enzymes into acids and sugars that act as fuel to the body. Additionally, the body can make use of the produced energy immediately or store it in the body tissues. However, individuals with metabolic disorders can neither convert food into energy correctly nor store it for later use.
Carbohydrate is the main source of body energy and are therefore responsible for the majority of metabolism disorders. Ordinarily, the body enzymes are supposed to break down carbohydrates into sugars. However, people with metabolism-related illnesses often lack the amount of enzymes required to successfully disintegrate carbohydrates, which can lead to other health complications, including death. Most carbohydrate metabolism disorders are hereditary, and it is always appropriate that are screened through blood tests.
Parents with a history of the conditions are also encouraged to conduct genetic tests to ascertain whether they have the genes. When identified in good time, patients can receive treatments in the form of supplements, special diets, and prescribed medicines. It is also important to note that there is no cure for some of these disorders, but therapies are crucial in managing the symptoms. Understanding the various carbohydrate metabolism disorders and their features is necessary for medical researchers and also educating the public about the same.
Research Objectives
One of the most neglected areas in the subject of carbohydrate metabolism is the study of related diseases. Consequently, the research aims at investigating all pathways involved in carbohydrate metabolism and chances of illnesses from involved reactions. Secondly the paper will evaluate all the possible disorders associated with carbohydrate metabolism throughout the digestion process. Additionally, the paper attempts to identify the damages these illnesses cause to the general body function. However, the research will be restricted to disorders that relate to digestion, absorption, synthesis, and breakdown of carbohydrates. The main research question is, what are the metabolic disorders associated with carbohydrate metabolism?
Methodology
Since this is a scientific research, the selected methodologies are systematic review and meta-analysis. The former technique will help in the identification, selection, evaluation, and synthesis of all relevant studies that answer the research question. Consequently, the paper will use the search phrase “carbohydrate metabolism disorders”, and the identified materials will be limited to articles published within the past five years. Meta-analysis will be instrumental in the statistical evaluation of the pooled data. The collected data information regarding carbohydrate information will be summarized and scrutinized in the results and analysis section.
Results and Discussion
The study used a total of seven scholarly and peer-reviewed articles that all researched carbohydrate metabolism and related disorders. The collected data, as is narrated in this section, entails information relating to the process of carbohydrate metabolism, digestion, and synthesis disorders. Before obtaining materials on the disorders, it is important to gather data on the steps involved in carbohydrate metabolism (Malicka, 2016). The components of carbohydrates include starch, fructose, galactose, and glucose. Once these elements are synthesized, they are passed into the bloodstream through the metabolism process, which comprises anabolism and catabolism, as represented below.
Anabolism (Synthesis) + Catabolism (Degradation) = Metabolism
Glycolysis
The process through which glucose is oxidized to pyruvate is termed glycolysis, and this occurs in all tissues. During digestion, polysaccharides are broken down into monosaccharides including glucose which are then transferred across the small intestine’s walls into the body’s circulatory system. Blood then transports these sugars to the liver, which can then be released immediately as a source of energy or stored as glycogen (Vijaya, 2016). Body cells obtain the glucose in the circulatory system through glycolysis, and some of the energy is transferred to adenosine diphosphate (ADP) to form adenosine triphosphate (ATP). Glycolysis is the most important process in carbohydrate metabolism and can be summarized in a chemical equation.
G![]() lucose + 2ADP + 2Pi 2L (+) – Lactate +2ATP + 2H2O
lucose + 2ADP + 2Pi 2L (+) – Lactate +2ATP + 2H2O
Consequently, carbohydrate metabolism disorders can occur when the reactions in a glycolytic pathway are interrupted. Glycolysis involves a 10 step reaction with every phase of the process crucial in metabolism. In summary, nicotinamide adenine dinucleotide (NAD+) is converted into nicotinamide adenine dinucleotide hydrogen NADH. Additionally, the glyceraldehyde 3-phosphate undergoes oxidation to form 1, 3-biphosphoglycerate within the same duration. Nonetheless, NADH is oxidized again to ensure the coenzyme NAD+ is not used, and this is all done during the conversion of pyruvic acid into lactic acid and in the presence of anaerobic conditions (Vijaya, 2016). Any slight interference with the ten stages involved in glycolysis can induce different metabolic disorders. The pathway is represented diagrammatically in the figure below.
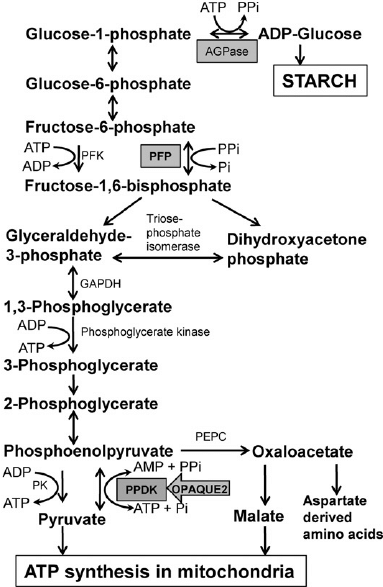
Anaerobic Phase
Oxygen is important in carbohydrate metabolism because its absence hinders the conservation of NAD+ since the NADH cannot be oxidized in the glyceraldehyde 3-phosphate phase. However, since the cells still have little coenzymes, the re-oxidation of NADH can be achieved by allowing pyruvate to lactate without manufacturing ATP (Lutsenko, 2018). It is important to note that it is the presence of glyceraldehyde 3-phosphate as a catalyst that hinders the production of ATP. Without oxygen, it is impossible to produce energy in the entire metabolism process. The anaerobic phase is represented in the figure below.
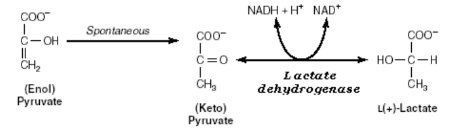
Tricarboxylic Acid (TCA) Cycle
The other process, as realized in the analyzed literature, which can be a source of carbohydrate-related disorders is the tricarboxylic acid (TCA) cycle. This stage is referred to as the aerobic phase, which imitates the anaerobic pathway in the pyruvate stage and is also known as the citric acid cycle. In this phase, pyruvate is converted into Acetyl coenzyme A through oxidation and decarboxylation before proceeding into the citric acid cycle. The process occurs in the mitochondrion organelle and results in a connection between the TCA cycle and glycolysis (Mendrick et al., 2017). All the processes of carbohydrate metabolism are interconnected, and it is important to note that disorders can occur at any phase and in any body part or cell, including mitochondria. Additionally, the pyruvate dehydrogenase complex is the enzyme responsible for the reaction in the TCA cycle. The chemical reaction can be represented in the form of a summary equation and a schematic diagram.
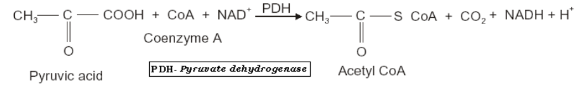
Citric Acid Cycle
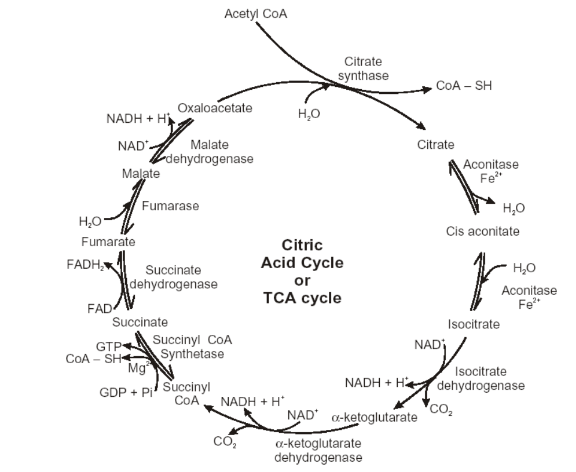
There are eight steps involved in the citric acid cycle, as demonstrated in the diagram, and they are all aimed at producing energy to the body through metabolism. When a single molecule of the TCA cycle’s substrate is oxidized in the presence of NADH, three ATP molecules will be produced. An addition of two other ATP molecules will be formed through flavin adenine dinucleotide (FADH2) (Pankiv, 2017). Consequently, when two molecules of pyruvate are generated from a single glucose molecule through glycolysis, the same process also results in the production of two other molecules in the TCA cycle.
Hexose Monophosphate (HMP) Shunt Pathway
The main metabolic pathways, as deduced in the findings, are the citric acid cycle and glycolysis since they provide the right enzymes and environment for glucose oxidation in animal tissues to produce ATP energy and CO2 and H2O. However, the research results also indicate alternative pathways which are equally effective in carbohydrate metabolism. One that has been proven to be essential is the Hexose monophosphate (HMP) shunt pathway that takes place in the additional mitochondrial soluble components of the cells. In this pathway, nicotinamide adenine dinucleotide phosphate (NADPH) in preparation for steroids and fatty acids synthesis (Rochlani et al., 2017). The process is also instrumental in the fusion of ribose to produce nucleic acid and nucleotide. Since glucose is among the primary hexoses obtained from the digestive system, the HMP shunt pathway facilitates the conversion of fructose and galactose into glucose, and this occurs in the liver. Any damages in the liver and mitochondria hinder the successful transformation of the two sugars into glucose, over ally interfering with the metabolism process. The hexose monophosphate (HMP) shunt pathway can be represented in a chemical equation below.

Gluconeogenesis
Gluconeogenesis is the other carbohydrate metabolism process that can be a source of disorders in case of any alterations in the involved reactions. It is defined as the production of glucose with the help of non-carbohydrate chemicals and processes. The reaction which normally occurs in the liver is often triggered by insufficient carbohydrate in the diet which fails to meet the body’s need of the nutrient (MedlinePlus, n.d.). Consequently, the protein tissues in the body are broken down during starvation into amino acids used to produce glucose. However, for gluconeogenesis to take place, reactions in glycolysis and the citric acid cycle must have taken place to give the molecules that will act as substrates. These precursors include lactate, glycerol, and amino acids, which are crucial in the synthesis of glucose in the liver.
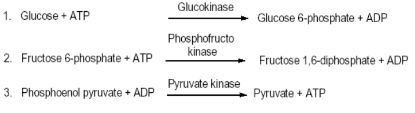
However, the results of the study indicate that gluconeogenesis and glycolysis are contradicting metabolic pathways but use similar enzymes in their reactions. For instance, glucose is transformed into pyruvate during glycolysis, and on the other hand, pyruvate is converted back to glucose in gluconeogenesis. Nonetheless, it is important to note that neither of the pathways is a reverse of the other (Vijaya, 2016). Consequently, there are three irreversible stages in glycolysis represented in the form of chemical equations below that have to be bypassed or replaced for gluconeogenesis to occur. Gluconeogenesis has to occur on the three precursors for the body to have energy in the absence of carbohydrates.
A diagrammatical representation of Gluconeogenesis
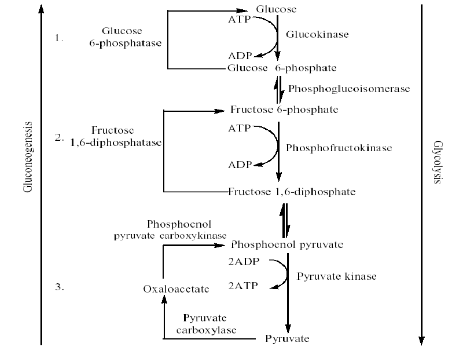
Galactose and Fructose Disorders
Galactosemia: Galactose disorder is also known as galactosemia, which results from issues in the second phase of metabolism when breaking down galactose. When this type of sugar is taken into the body, mainly in the form of milk, an accumulation of galactose-1-phosphate takes place. Consequently, the signs and symptoms of galactosemia begin to manifest as soon as milk feeding is initiated. When realized, it is advised that the feeding is stopped immediately. Otherwise, the child will develop kidney-related complications, jaundice, weight loss, and lethargy (Malicka et al., 2016). Moreover, infants with the disorder are also prone to numerous bacterial infections. Delayed and lack of treatment leads to intellectual disability and the development of cataracts in the patients. Removal of galactose from the infant’s diet is one of the major therapy approaches which helps in reversing the symptoms.
Hereditary Fructose Intolerance (HFI): Fructose 1-phosphate is crucial in the general metabolism, and its absence, which is often due to problems in the liver, leads to hereditary fructose intolerance (HFI). The symptoms of this disorder are visible after taking in fructose and therefore can only be discovered at a later age compared to galactosemia. The common sources of fructose are fruits, infant meals that mainly contain sucrose, and table sugar. Some signs and symptoms of HFI include defects in the kidney, deficiencies in the liver, weight loss, hypoglycemia, and vomiting (Malicka et al., 2016). Furthermore, children with this condition prefer not to use extremely sugary foods such as candy with minimal caries in their teeth. The best intervention for hereditary fructose intolerance is avoiding meals with sucrose and fructose sugars.
Fructose 1, 6-Diphosphatase Disorder: The disorder is caused by the lack of the enzyme fructose 1, 6-diphosphatase disorder, crucial in gluconeogenesis, a process that converts glucose into other substrates crucial in metabolism. Symptoms of the condition include liver enlargement, inability to fast, and extreme hypoglycemia. The treatment of the disorder includes the use of intravenous fluids with the right glucose content, and patients are advised to avoid fasting in all its forms (MedlinePlus, n.d.). In severe fructose 1, 6-diphosphatase disorder cases, affected individuals are given bedtime doses and continuous drips throughout the night to help minimize the development of hypoglycemia.
Glycogen Storage Disorders (GSD)
Aside from galactose and fructose-related metabolism conditions, some result from the body’s inability to store glycogen in the body tissues. Glucose is very important to the body because it is necessary for the metabolic processes that take place in the brain, adrenal medulla, and red blood cells (Rochlani et al., 2017). The availability and distribution of glucose commence at the small intestine, where transport proteins facilitate the movement of glucose into the cells. The glucose is then transported via the blood to the liver and then stored in the form of glycogen which is later broken down again to give out energy to the body, particularly during fasting and starvation. Furthermore, glycogen can also be stored in body tissues and used during rigorous body activities such as exercises.
Consequently, when enzymes meant to aid in the breaking down the glycogen in the body tissues and liver into energy fail to do so, glycogen storage disorders (GSD) emerge. These conditions can either affect the liver and muscles, depending on the affected enzyme. GSD type 1 is an example of the disorders which takes place due to a faulty liver and often leads to hypoglycemia. Treatments in infants include a constant supply of glucose using drips into the digestive system. The continuous process helps the child do away with some of the symptoms as they grow older (Rochlani et al., 2017). The other effective GSD therapy is a liver transplant, but this step is reserved for extreme cases where the patients are unable to respond to the ordinary treatment process or are victims of liver cancer. Individuals who have muscle-related GSDs are to avoid different forms of demanding exercises to manage their conditions.
Glycosylation Congenital Disorders
Metabolism disorders not only affect the liver and muscles, as in the case of GSD but other vital body organs such as the brain. Congenital disorders of glycosylation (CDG) is a condition that damages various parts of the body, and its manifestation is in the endoplasmic reticulum and cytoplasm, crucial to the fusion of lipids and proteins. CDG type 1 is a common type of this illness, which is brought about by a defective phosphomannomutase 2, one of the enzymes responsible for glycosylation (Mendrick et al., 2017). Some of the symptoms of the disorder include abnormalities in the brain, poor muscle development during infancy, and extreme developmental delay. Additionally, children with CDG type 1 may have seizures, retinal damage, hypoglycemia, vomiting, and diarrhea. Unfortunately, there are no effective treatment approaches to this group of disorders. Affected patients can only find means of managing the symptoms as curing the condition is not possible at the moment.
Mitochondrial Disorders
As noted in previous carbohydrate metabolism disorders, the mitochondrion is crucial in the oxidation process. Therefore any defects in this element can lead to more metabolism issues within the human body. In a mitochondrial respiratory chain, there are five protein networks responsible for producing the energy required to complete chemical reactions in the cells (Malicka et al., 2016). Consequently, any abnormality affecting the respiratory chain triggers toxic oxygen reactive substances due to low energy production. Moreover, defects in the mitochondria lead to the production of apoptotic elements, which prompt cell death.
The signs and symptoms of the disorders are linked to deficiencies in the mitochondrion by the level of mutation, considering they can be inherited, the energy required by the affected tissues, and the segments of the mitochondria that have been damaged. Patients with the disorder experience defects in the muscular and nervous systems because the tissues of these two cannot function without mitochondrial metabolism. Furthermore, there is a connection between the disorder and neurodegenerative conditions such as amyotrophic lateral sclerosis (ALS), Parkinson’s disease, and Alzheimer’s disease (Malicka et al., 2016). It is important to note that there is no proven cure for mitochondrial disorders. However, there are existing supplements prescribed by medical professionals and other experiments meant to aid in gene therapy.
Lysosomal Storage Disorders
Lysosome is another group of organelles with multiple enzymes with the capability of breaking down carbohydrates. This means that it is an integral component metabolic processes in the body. Each lysosome has a corresponding lysosomal enzyme with specific nuclear DNA markers (Lutsenko, 2018). Consequently, when a lysosomal enzyme goes missing, becomes insufficient, or mismatches a lysosome, the broken down macromolecules accumulate and lead to irregular storage of compounds, including glycogen. Most lysosomal storage defects are considered autosomal recessive, other than the Hunter syndrome and Fabry disease, which are X-linked.
The signs and symptoms of lysosomal storage disorders are determined by the storage location of the degraded molecules. For instance, the gauche disease causes anomalies in the peripheral tissues such as bones, spleen, and the liver. On the other hand, Tay-Sachs disease affects the nervous system, while Niemann-Pick disease damages both systemic organs including the brain. Consequently, the symptoms of the lysosomal storage related conditions include enlarged spleen and liver, eye deformities, bone diseases, and coarse facial features (Lutsenko, 2018). Generally, this group of diseases often cause acute neurological damages as early as infancy. There are no scientific interventions to lysosomal storage disorders other than supportive care. Previously, there have been attempts of bone marrow transplant but the few cases have not been successful.
Conclusion
Carbohydrate metabolism is one of the most significant activities in the body because it is necessary for the production of the energy required to perform even the simplest of human tasks. Whenever people eat, the food can be broken down immediately through glycolysis to provide energy to the body, or excess of the energy can be stored in the form of glycogen in tissues which can be used later. However, the interference of these chemical processes leads to carbohydrate metabolism disorders. The bodies of people with these conditions struggle to disintegrate the ingested carbohydrates into sugar because they lack enough enzymes required to do so. Additionally, during starvation, the body is forced to obtain glucose of cell proteins through gluconeogenesis. Consequently, in studying carbohydrate metabolism disorders, it was imperative to understand glycogen-related disorders and those that affect different enzymes and organelles that participate in energy production and storage. Since a majority of these disorders are genetic, few therapies can be used to treat the illnesses effectively. However, their symptoms can be managed by simple adjustments in the diets of the affected individuals.
References
Agana, M., Frueh, J., Kamboj, M., Patel, D., & Kanungo, S. (2018). Common metabolic disorder (inborn errors of metabolism) concerns in primary care practice. Annals of Translational Medicine, 6(24), 469-469. Web.
Carbohydrate metabolism disorders. MedlinePlus. Web.
Lutsenko, L. (2018). Glycemic screening and recurrent carbohydrate metabolism disorders with endocrine pathology. International Journal of Endocrinology, 14(2), 205-210. Web.
Malicka, J., Kurowska, M., Dudzińska, M., Smoleń, A., Oszywa-Chabros, A., & Tarach, J. (2016). Disorders of carbohydrate metabolism and their relationship with the prevalence of cancer in patients with acromegaly – authors’ own observations. Family Medicine & Primary Care Review, 3, 291-293. Web.
Mendrick, D., Diehl, A., Topor, L., Dietert, R., Will, Y., & La Merrill, M. et al. (2017). Metabolic syndrome and associated diseases: From the bench to the clinic. Toxicological Sciences, 162(1), 36-42. Web.
Pankiv, V. (2017). Disorders of carbohydrate metabolism in clinical practice. International Journal of Endocrinology, 13(1), 39-44. Web.
Rochlani, Y., Pothineni, N., Kovelamudi, S., & Mehta, J. (2017). Metabolic syndrome: pathophysiology, management, and modulation by natural compounds. Therapeutic Advances in Cardiovascular Disease, 11(8), 215-225. Web.
Vijaya, J. (2016). Salacia Chinensis Extract (SCE) Modulates Carbohydrates and Lipid Metabolism: in vitro and in vivo Models. Endocrinology & Metabolism International Journal, 3(6), 45-69. Web.