Introduction
In 2002 the Global Fund to Fight AIDs, Tuberculosis and Malaria was implemented in order to tackle the catastrophe caused by the world three killer diseases that had their most adverse effect in developing countries, notably sub-Saharan Africa. Combined these three killer diseases are responsible for the deaths of more than 11,500 persons in a given day which translates to more than 42 million persons annually. In any given year for more than decades now 300 million cases of malaria are diagnosed worldwide majority of this cases occurring in developing countries; 1 million of the persons infected with malaria eventually dies, 90% of the time happening in Africa mainly among children aged below ten years.
On 25th April, 2010 the Africa Malaria Day celebrated its 10th anniversary since the Abuja declaration was brought into force which aimed to reduce the number of malaria mortality rates by half by the end of this year.
Globally the epidemiological distribution of Malaria and Tuberculosis disease worldwide is greatly skewed with majority of the cases occurring in Africa; 90% of all malaria related deaths for instance take place in Africa which is the home to a third of all tuberculosis diagnosed cases. Tuberculosis is the number one cause of death for persons infected with HIV AIDs; in Sub-Saharan Africa, tuberculosis related complications are the cause for 30% deaths among the 25 million peoples infected with HIV. In 2008, tuberculosis related deaths were responsible for approximately 1.8 million deaths worldwide which translates to 5,000 persons in a day; another 2 billion people are estimated to be infected by the WHO, making it by far the worst public health crisis that had ever affected humanity.
However, this high prevalence rate for persons affected by tuberculosis emanates from the nature of the vaccine that is given to children at an early age which is usually injected when it is live attenuated. Both malaria and tuberculosis prevalence are strongly linked to the HIV AIDs disease since they are the most common opportunistic infections that eventually cause mortality to HIV infected persons. The purpose of this paper is to discuss the disparity of malaria and tuberculosis infections, risk factors as well as intervention strategies in two different regions; Africa and Middle East.
Malaria Prevalence, Risk Factors and Disparity: Africa & Middle East
Malaria is a disease caused by plasmodium; a protozoa that is categorized into four species; p.falcipurum, p. ovale, p.malarae and p. vivax. Among all these four species, p. falcipurum is the most deadly of all and accounts for the highest proportional of the deaths. The disease is transmitted by the female mosquitoes, anopheles which acts as the vector that incubates the plasmodium. Typical symptoms of malaria among infected cases include fever, anemia and organ dysfunctional among others.
Disparity in Risk factors
The major risk factor for contracting malaria is travelling or living in regions that are considered endemic to malaria or even regions that are not necessarily endemic especially for persons who have low immunity to the disease. Besides the area of residence, the probability of contracting malaria will largely depend with the strength of the immune system of a person as far as malaria is concerned.
The WHO classifies into five categories the groups of persons that are most likely to be infected with malaria based on research studies as well as mortality and morbidity rates of the disease in the general population. These groups of persons include; young children, pregnant women, HIV infected persons, immigrants returning to endemic regions and persons emigrating in endemic regions; almost always these groups of persons are the ones who are mostly affected by the epidemic.
In sub-Saharan Africa the risk factors for malaria disease are notably more than is the case in Middle East; One of the major disparity of malaria risk factors is caused by the climatic conditions of the tropical and subtropical region where the highest prevalence of malaria infections are found in Africa. This is because these regions experience high humidity levels, high temperatures and rainfall patterns that are equally distributed throughout the year which creates the optimal breeding sites for malaria and the favorable conditions for the reproduction of the plasmodium protozoa.
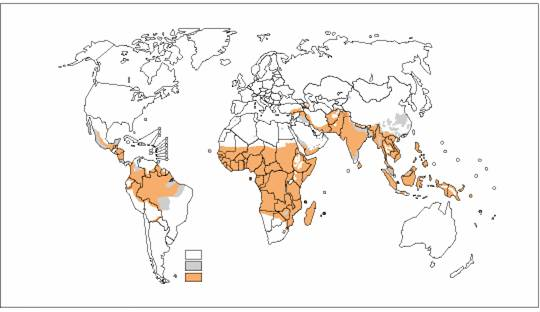
The combinations of these interrelated climatic factors are clearly not found in most countries of Middle East which are largely found in semi-desert and desert regions. Besides there is evidence of correlation between high malaria prevalence and poverty; in a research study by Gallup and Sachs on the interrelation of malaria and low income level a positive correlation was found.
The conclusion of the study was that “malaria and poverty are intimately connected”, this was based on the fact that malaria was both a cause and an effect of poverty in sub-Saharan Africa when all other conditions were kept constant. The study also found that high poverty levels in the region aggravated the malaria prevalence which was then worsened by the economic sabotage that the epidemic caused in the continent by affecting a significant number of the most productive persons in the community.
Comparing these trends to the per capita income found in many countries of Middle East there is huge disproportion in terms of income levels that explains why there is low malaria prevalence in this region. The correlation between income and high malaria prevalence has to do with the high economic costs of fighting malaria; this year alone, the Global Fund has allocated $5.33 billion to fight Malaria disease alone much of which will be used in Africa.
According to WHO high prevalence rate of malaria in Africa is responsible for reduced Gross Domestic Product (GDP) by up to 1.3% while it account for 40% for all health related expenditures, this is a significant amount of scarce resources that could be used elsewhere. Finally, Africa has very high HIV AIDs burden than is the case in Middle East; because HIV is a major determinant for the prevalence of malaria, this factor becomes very significant.
To quantify this comparison consider that Africa has 60% of all HIV related cases while it only comprise 10% of the world population with a rate of 3.1 million infections per year.
Disparity in Prevalence
For more than five decades now malaria is still the leading cause of deaths in both children under five years of age as well as pregnant mothers in Africa; 20% of all child related deaths that occur among children aged less than five years are directly as a result of malaria epidemic. The highest proportion of hospital admissions and clinical consultations that take place in Africa are largely as a result of malaria infection; as high as 30% cases are diagnosed with the disease while more than 25% of admissions are malaria related in endemic countries of Sub-Saharan Africa. Overall even the least affected countries in Africa which are not located in tropical or subtropical regions where malaria prevalence is at its highest indicates ever increasing prevalence rate for malaria.
On the other hand Middle East has very low prevalence of malaria overall due to the climatic conditions that are unfavorable to mosquitoes breeding in the larger part of the region. Save for Saudi Arabia, Bhutan, Iran, Iraq, Afghanistan and Yemen, most other countries in the region has very low prevalence of the disease which officially makes them free of malaria. Malaria free countries in Middle East include Israel, United Arabs Emirates, Qatar, Oman, Brunei and Bahrain. The reason for the low prevalence of the disease in some countries in the region lies in the climatic and topographic characteristic of the regions.
But Middle East countries that are susceptible to malaria such as Yemen and Afghanistan tend to register high prevalence rates of the disease especially during the peak periods which are associated with high rainfalls. A recent study conducted on Yemen school going children between the months of July and September and February to March when malaria infections were at their highest found the prevalence rate to be as high as 40% in hospitalized children similar to malaria prevalence rates for malaria endemic countries in Africa. However, only 1% of the cases who were hospitalized eventually died which is a far cry from Africa where up to 20% of children who are infected with malaria eventually dies.
This is perhaps the first indication which shows evidence of the effectiveness of resources in malaria management interventions, notably in areas of curative and prevention. Many experts think it is probably for the same reasons that Afghanistan has high prevalence rate of malaria and related deaths than any other country in the region because of its low per capita income that is way below many countries in the region. Indeed many research studies have for some years now linked the high mortality rates from malaria related complications to poverty; a factor of disparity on malaria prevalence between the two regions that we shall more comprehensively investigate later on this paper.
In recent years the trend in malaria prevalence has led experts to believe that the disease is reemerging especially in Sub-Saharan Africa. This is due to increased incidence rates of the disease that significantly kills more people in Africa than it has previously been the case and despite the numerous intervention strategies that are already in place.
More specifically the reemergence of malaria incidence worldwide is being attributed to several factors key of which include resistance to chloroquine and quinolines which have traditionally been the first line of treatment of malaria cases. Other factors that have been linked to increase of malaria prevalence include human migrations, armed conflicts that lead to displacement of large populations in endemic areas, climate change, adaptation of the vector and inadequate health systems in the most affected countries.
Disparity in Malaria Intervention Strategy
Malaria intervention strategies involve multispectral approach that must be undertaken at various different levels for effective impact based on the unique circumstances of the community. More importantly, efficient malaria control strategy cannot be achieved without the committed support of the community and the individuals themselves. There are five levels at which malaria intervention strategies can be designed which are all focused on the person since previous research efforts have been unable to target mosquitoes as a factor in malaria prevention.
They are early diagnosis and treatment, personal protection such as prophylaxis, complete treatment, environment control through destruction of breeding sites and compliance with treatment to prevent disease resistance. The figure below show a cycle that highlights the various points of intervention that could be implemented.
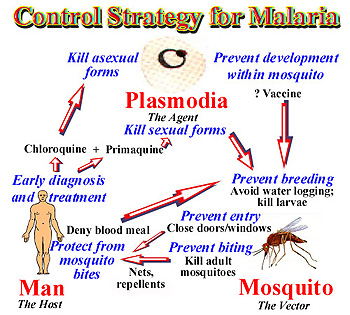
Because resource is a key component to the design of effective reliable intervention strategies as we have so far determined, African countries are disadvantaged in this area than the oil rich countries of Middle East. Consequently, countries in Africa have high burdens from the disease than in Middle East and most interventions strategies for malaria that are being undertaken in Africa are largely focused on treatment rather than prevention due to scarcity of this resources.
Overall the cost of prevention strategies for malaria disease will therefore be far less in Middle East than in Africa because of it topography for instance such as the semi-desert and desert terrain of most countries in Middle East which pose less challenge in elimination of mosquitoes breeding sites. In addition the rainfall experienced in this region is intermittent which means prevention strategies need not be sustained throughout the year.
Tuberculosis Prevalence, Risk Factors and Disparity: Africa & Middle East
25% of the world tuberculosis infections are found in Sub-Saharan Africa that totals approximately 2.4 million cases ; in 2005 the WHO in their annual declaration officially pronounced Tuberculosis to be an emergency disease across Africa. Tuberculosis is an invasive disease that most affects the lung tissue which is highly contagious because it’s transmitted through the air. A huge proportion of the world population, 30% are infected with tuberculosis but are not infectious and therefore cannot be capable of transmitting the disease nor exhibit symptoms of the disease.
50 years since the cure of tuberculosis was found, current epidemiology of the disease has now given rise to another strain of the disease that is largely untreatable or very expensive and challenging to treat; what is referred as the multi-drug-resistant TB. This strain of TB which is proportionally found in countries that have high HIV AIDs prevalence due to their causal association such as in Africa further complicates the prevention and management of the disease. The table below shows the tuberculosis prevalence rate for the disease in 2008 worldwide.
Figure 3: Estimated TB Incidence, Prevalence and Mortality, 2008.
Comparing the tuberculosis infections data as highlighted between the two regions, Africa and Middle East shows the prevalence rate to be more than four times in Africa than in Middle East. The associated mortality from the disease is also found to be approximately three times higher in Africa than is the case in Middle East countries while the rate of new infections in a year is about four times the rate in Middle East. Besides America and Europe, Middle East countries have the third least tuberculosis disease burden while Africa is the leading with almost ten times the burden found in America with 25% of the world share.
Risk Factors
Ironically the major risk factor for tuberculosis is the BCG vaccine that is injected during the early years of life; this is because the tuberculosis vaccine has to be live attenuated in order to excite the body to produce the required level of immunity of the disease. Since the TB bacilli that is introduced in the body during vaccination is just dormant but not completely destroyed, weakened immunity usually results to rejuvenation of this bacteria. For this reason HIV infection is one of the most significant risk factor for tuberculosis disease due to its ability to comprise the immune system thereby giving TB the opportunity to resurge; and the major factor that that is responsible for the unprecedented reemergence of the epidemic worldwide.
TB is therefore the leading cause of death in all persons that are infected with HIV AIDS disease; other risk factors for Tb are poor aerated environments, humidity, living with a person who is infectious as well as other conditions that causes reduced immunity. The disparity of tuberculosis prevalence in the two regions of Africa and Middle East is therefore largely determined by the prevalence of HIV infections. For this reason Middle East has relatively low prevalence of tuberculosis than Africa.
Disparity in Tuberculosis Intervention strategies
The tuberculosis intervention framework implemented by various countries is usually a modification of the WHO Stop TB Strategy that is customized for the case specific challenges that are faced by each country. In general tuberculosis intervention strategy designed by the WHO attempts to manage and prevent TB from six levels; expansion and enhancement of DOTS, focus on reduction of HIV which is the key risk factor to the disease, strengthening of health systems, community empowerment, consolidation of healthcare providers and research initiatives.
Most countries in Sub-Saharan Africa have so far implemented frameworks for addressing TB in all this areas but they are limited in three fronts; research on tuberculosis, strengthening of the health care system and expansion of DOTS. Due to scarce resources available to fight the epidemic most intervention strategies are channeled towards treatment initiatives rather than research, and even then there are countries that are yet to provide free treatment of TB due to limited capacity.
The fact that the health care system is already over burdened by other equally devastating disease such as malaria and HIV AIDs means that the quality of care that is available is greatly limited in terms of drug quality and quality of treatment given to cases. On the same level, comparison of intervention strategies implemented in most Middle East countries would indicate a great disparity largely because of the availability of resources and reduced prevalence of the disease in the region.
This means that the health care systems in many of these countries are not stretched by the burden of the disease given that HIV prevalence is also relatively low. The reduced population levels in most Middle East countries coupled with the high GDP levels makes it possible for the governments to put in place health intervention strategies that offer quality care. Except in Yemen and Iraq where tuberculosis prevalence rate are significantly high, other countries in the region have relatively low tuberculosis prevalence; in Yemen tuberculosis is the number four cause of mortality which has been declining over the recent past. The WHO recommended treatment protocol for the disease is as summarized in the following table.
Figure 4: WHO Treatment Protocol for TB.
Conclusion
From the analysis of malaria and tuberculosis prevalence rates between the two regions Africa and Middle East, it is clear that huge disparity exists as far as mortality, morbidity, incidence and prevalence are concerned. Even the risk factors of the two diseases appear to differ at times between the two regions for the same disease making the distribution and progression of the two diseases vary. Indeed, as we have seen poverty is a significant cause of both diseases which means it is a risk factor.
The epidemiology of the diseases and other socio-demographic factors such as income levels and culture that differs across these regions is also the other factors of the disparity of the diseases between the two regions. When all these factors are considered, the causes and effect of malaria and tuberculosis between Africa and Middle East is as different as the culture between the two countries; which is all the more reasons why the intervention strategies cannot be designed the same way for both regions.
References
- UNAIDS. Middle East and North Africa: AIDS epidemic update Regional summary. 2007. Web.
- WHO. Tuberculosis. 2010. Web.
- Unicef. The Africa malaria report. 2003. Web.
- Kent, J. Statistics: HIV AIDS, malaria and tuberculosis. 2005. Web.
- UNESCAP. Combat HIV/AIDS, malaria and other diseases. 2007. Web.
- Nchida, T. Malaria: A remerging disease in Africa. Emerging Infectious Diseases. 1998; 4(3): 179-191.
- Savigny D, Mayombana C, Mwangeni E, Minhaj A, Reid G. Care-seeking patterns of fatal malaria in Tanzania. Malaria Journal. 2004; 3(27): 254-262.
- Gallup, L, Sachs J. The Economic burden of malaria. 2001. Web.
- Kowalski, S. The cost of fighting AIDS, TB and malaria. 2010. Web.
- Aidspan. Global fund overview. 2002. Web.
- Malhotra M, Srivastra A. case Studies from the south. 2001. Web.
- Kakkilaya B. Control of malaria. 2002. Web.
- Nooritajer M. Review of tuberculosis. Middle East Journal of Nursing 2008; 2(2): 542-563.
- Pagnoni F, Convelbo N, Tiendrebeago H, Cousens S, Esposito F. A community-based programme to provide prompt and adequate treatment of presumptive malaria in children. Trans R Soc Trop Med Hyg 1997; 91(2):512-527.
- Conrad,K. HIV AIDS and other infectious diseases. 2009. Web.
- Mons B, Klasen E, van Kessel R, Nchinda T. Partnerships between South and North crystallizes around malaria. Science 1998;279 (1):498-509.
- Lynn, J. Malaria AIDS, TB in Retreat-Global Fund. 2010. Web.